Abstract
Background: Management of endoscopic retrograde cholangiopancreatography (ERCP)–associated duodenal perforation remains controversial. Some recommend surgery, while others recommend conservative treatment.
Methods: A retrospective chart review was conducted to identify patients treated at our institution for ERCP-related duodenal perforations. Study variables included indication for ERCP, clinical presentation, diagnostic procedures, time to diagnosis and treatment, location of injury, management, length of stay in hospital and survival.
Results: Between January 2000 and October 2009, 12 232 ERCP procedures were performed at our centre, and perforation occured in 11 patients (0.08%; 5 men, 6 women, mean age 71 yr). Six of the perforations were discovered during ERCP; 5 required radiologic imaging for diagnosis. Three perforations were diagnosed incidentally by follow-up ERCP. In 1 patient, perforation occurred 3 years after the procedure owing to a dislocated stent. Four of 11 perforations were stent-related; in 2 patients ERCP was performed in a nonanatomic situation (Billroth II gastroenterostomy). Free peritoneal perforation occurred in 4 patients; 1 was successfully managed conservatively. Four patients (36%) were treated surgically and none died. Five patients were managed conservatively with a successful outcome, and 2 patients died after conservative treatment (18%). Operative treatment included hepaticojejunostomy and duodenostomy (1 patient), suture of the perforation with T-drain (1 patient) and suture only (2 patients). The mean length of stay in hospital for all patients was 20 days.
Conclusion: Post-ERCP duodenal perforations are associated with significant morbidity and mortality. Immediate surgical evaluation and close monitoring is needed. Management should be individually tailored based on clinical findings only.
Endoscopic retrograde cholangiopancreatography (ERCP) is widely regarded as a safe procedure, but the associated rate of major adverse events approaches 6%–7%. Although the incidence of duodenal perforations after ERCP has decreased since its introduction in 1968 from more than 2% to less than 0.5%,1–6 most likely because of improvement in experience and skill of the endoscopists, severe and fatal cases continue to occur.7 Several studies have suggested surgical, endoscopic, radiologic or conservative management, but consensus is lacking since these injuries are rare and reported patient populations are not comparable.8–10 In this study, we report a retrospective analysis of a series from a single European tertiary referral centre and define a management algorithm for ERCP-related duodenal perforations based on clinical and radiographic findings at presentation.
Methods
We retrospectively collected data on patients treated at our centre for ERCP-related duodenal perforations between January 2001 and December 2009. We searched our database for all patients with small bowel perforations. From this population, patients who had received ERCP were chosen. Computer records and charts were reviewed to exclude patients with peptic ulcer, traumatic or other perforations of any cause. We collected data on the following variables: ERCP findings, clinical and radiological presentation of the perforation, diagnostic methods, time to diagnosis and surgery, location of the duodenal leak, methods of management, surgical procedures, complications, length of stay in hospital and patient outcomes. All patients consenting to eventual surgical treatment were transferred to the surgical department. Generally, patients were conservatively managed if diffuse peritoneal signs were not present. Conservative therapy included a nasogastric tube, nil-by-mouth diet, total parenteral nutrition, broad-spectrum intravenous antibiotics, close surgical monitoring of abdominal status and daily laboratory tests. Abdominal computed tomography (CT) was performed in patients with elevated inflammatory parameters or fever. Oral nutrition was resumed at normalization of laboratory parameters and bowel movements. Patients were discharged when asymptomatic at oral food intake. Surgery was performed in patients with diffuse abdominal tenderness and guarding regardless of mechanism and place of injury. One patient underwent CT-guided drainage of a retroperitoneal abscess.
Results
Study population
During the study period, 12 232 ERCPs were performed at our centre. Our study population of 11 patients represents all cases of duodenal perforations following ERCP treated in our department; 10 patients underwent ERCP in our gastroenterology department, and 1 had the procedure at an affiliated hospital and was transferred to our centre for further treatment after the diagnosis of duodenal perforation. The team treating these patients included 7 gastroenterologists performing ERCPs with 17 dedicated nurses and technical assistants, 9 senior surgeons and 31 junior surgeons and residents.
The mean age of our study population was 75 years. There were 5 men and 6 women. The indication for ERCPs were hilar cholangiocarcinoma (n = 3), choledocholithiasis (n = 2), suspected pancreatic cancer (n = 1), chronic pancreatitis (n = 1), adenoma of Ampulla of Vater (n = 1) and jaundice of unknown origin (n = 3). In 2 patients, ERCP was performed after previous gastric resection with Billroth II reconstruction.
ERCP data
During the study period 8291 purely diagnostic ERCPs and 3941 ERCPs with sphincterotomy were performed in our medical centre. The duodenal perforation rate was 0.02% (2 of 8291) for purely diagnostic investigations and 0.2% (8 of 3941) for procedures with papillotomy. Four of 11 (36%) perforations were caused by a dislocated biliary stent. The site of perforation was periampullar in 4 patients, at the second part of the duodenum in 4 patients, at the afferent limb of gastroenterostomy after Billroth II reconstruction in 2 patients and in the postpyloric duodenum in 1 patient. One patient had combined iatrogenic injury of the papilla of Vater and the common bile duct.
Clinical features and diagnosis
In 5 patients, duodenal perforation was immediately noticed during the ERCP procedure, and in 1 patient the diagnosis was made after routine post-ERCP abdominal radiography. The abdominal radiographs of 4 patients (36%) showed intra-abdominal free air. Two perforations were incidentally diagnosed in an asymptomatic patient in a follow-up ERCP 1 and 6 days, respectively, after the initial procedure. In 1 patient, a stent-related perforation was diagnosed 3 years after the initial procedure when the patient presented with acute onset abdominal pain. In 1 patient, the iatrogenic injury was incidentally diagnosed by subsequent upper gastrointestinal endoscopy 3 days after ERCP. In 1 patient with fever and elevated leukocyte count 4 days after ERCP, the diagnosis of retroperitoneal perforation was made from an abdominal CT scan. Two patients experienced pancreatitis, defined as abdominal pain and a serum concentration of pancreatic enzymes (amylase or lipase) 3 or more times the upper limit of normal.1 In 3 patients, generalized peritonitis developed on the first day after the initial procedure. Ten of 11 patients had elevated leukocyte counts during their stay in hospital. Two patients underwent surgery without having had a post-ERCP blood test after the perforation was diagnosed during the procedure. Three patients had leukocyte counts greater than 20.0 × 109/L (reference range 4.5–11.0 × 109/L) during their course; 2 were managed conservatively.
Management and outcomes
Conservative management
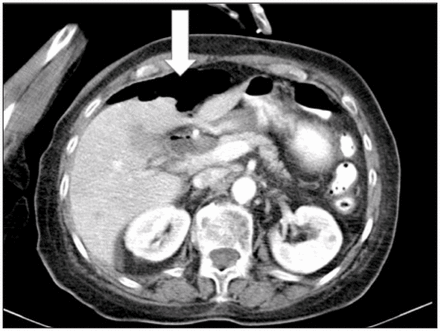
Conservative management was defined as nonoperative management after the diagnosis was made. Seven of 11 (64%) patients were managed conservatively. Among them, 3 patients refused surgery, 5 were successfully managed with standard conservative therapy, and 2 of the patients who refused surgery died after 17 and 19 days, respectively. Both patients had end-stage malignant periampullar disease. One patient with free abdominal air had no clinical signs of diffuse peritonitis and was managed conservatively with a successful outcome (Fig. 1). The mean length of stay in hospital among surviving patients was 19 (13–30) days. These patients were either initially completely asymptomatic or experienced minimal abdominal tenderness during their stay in hospital. The mortality associated with conservative management was 2 of 7 (28%) patients; both refused surgical evaluation and eventually declined any further treatment.
Intraperitoneal air visible on a computed tomography scan of a patient with duodenal perforation after endoscopic retrograde cholangiopancreatography. The patient was successfully managed conservatively. The arrow denotes the typical diagnostic finding.
Operative management
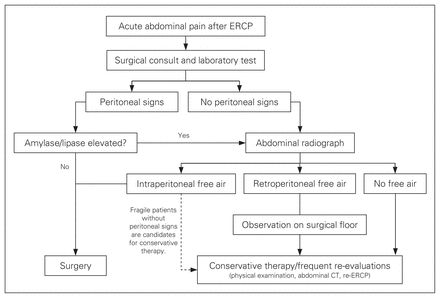
Surgery was indicated in the presence of diagnosed or suspected perforation and diffuse abdominal tenderness (Fig. 2). In 4 patients (36%), operative treatment was necessary. Three of them had free intra-abdominal air visible on abdominal radiograph and/or CT scan. The fourth patient had diffuse peritonitis with extraluminal air in the retroperitoneal space. Three patients had their operation less than 24 hours after ERCP; for 1 patient, treatment was delayed by 4 days owing to late diagnosis. One patient who had previous Billroth II reconstruction was treated with a simple suture of the perforated afferent jejunal limb. In the other patient (#4 in Table 1) who had a Billroth II reconstruction after gastric resection, we found no jejunojejunostomy at exploration, therefore, the perforation site was resected and a jejunojejunostomy was performed. An additional hepaticojejunostomy was performed for a fibrotic stenosis of the distal part of the common bile duct. One patient with injuries both to the periampullar duodenum and the common bile duct was treated by suture and T-drain placement. One of the 4 patients (25%) treated surgically required reoperation owing to an early fascial dehiscence. The mean length of stay in hospital in the operative group was 23 (9–41) days. None of the surgically treated patients died in hospital.
Algorithm of the management of endoscopic retrograde cholangiopancreatography (ERCP)-related duodenal perforations. CT = computed tomography.
Demographic and clinical characteristics of the study population
Discussion
Our retrospective review of our hospital data identified 11 patients with duodenal perforations related to endoscopic periampullar procedures. The major findings of this study are a perforation rate lower than that reported recently in the literature,4,11 the recent sight decrease in the use of ERCP and the pivotal role of surgical assessment and tailored treatment of patients with duodenal perforation after ERCP.
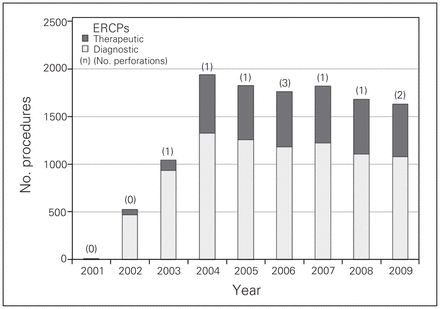
Contrary to previous reports,11 the number of procedures did not decline dramatically in our study (Fig. 3), probably owing to the relatively extensive expertise in ERCP in our hospital. The annual perforation rate is extremely low and shows no trend. As expected, most perforations occurred in procedures with papillotomy. Only 2 of 8941 patients had an iatrogenic injury to the duodenum during a procedure without sphincterotomy. Both patients had a previous Billroth II reconstruction after gastrectomy, which shows that in these patients particular caution is required with the use of a side-viewing endoscope. Therapeutic ERCP carries a greater inherent risk owing to its invasive nature and the foreign bodies (stents) used during the procedure.
The number of duodenal perforations and endoscopic retrograde cholangio-pancreatographies with and without papillotomy per year in our hospital.
Our data show that patients with ERCP-related duodenal injuries are of advanced age and have multiple comorbidities, making them particularly susceptible to post-procedural complications. Nevertheless, the 2 fatalities in our series occurred in patients who refused surgical therapy. Interestingly, 5 of 11 patients in our series underwent ERCP for suspected premalignant disease.
Interestingly, a periampullar duodenal diverticula (PAD) was diagnosed in 2 of 11 patients during ERCP. Although the prevalence of PAD reported in the literature is 1%–25%,12,13 surgical series of ERCP-related perforations show that this diagnosis often cannot be confirmed at the subsequent operation.10 In our series, all the patients who received a diagnosis of PAD were managed conservatively.
One perforation in our series was stent-related and was included in this analysis because, in our opinion, during the treatment of these patients, the surgeon faces the same questions as in other cases: Should we operate or not? Does the abdominal status warrant a conservative approach, or does abdominal sepsis develop?
Based on our experience, previously published classifications of ERCP-related small bowel injuries are of small value in the everyday clinical setting. These studies are always based on retrospective findings on small patient populations and their findings cannot be generalized. In Table 2, we summarize the most cited classifications and treatment suggestions and compare them to our data. Stapfer and colleagues10 published their classification based on a retrospective analysis of 14 patients, 3 of whom died. Based on this classification, 2 of 4 patients in our study would not have received surgical treatment, and 1 patient would have undergone an unnecessary operation. Furthermore, contrary to the suggestions by Stapfer and colleagues,10 large abdominal fluid collections are not obligatory indications for surgery, as these are almost always well managed by CT-guided drainage. The classification and proposed therapy of ERCP-related perforations by Howard and colleagues9 differed from our experience even more. First, the authors classified the injuries based on their mechanisms. In our study, perforations were diagnosed immediately during ERCP in only half of the patients, making treatment decisions based on the injury mechanism difficult, if not impossible. Second, the only guide wire–related injury (Howard type I) was managed surgically, contrary to the suggestions of Howard and colleagues,9 and 2 of 5 patients with injuries remote from the papilla were successfully treated without an operative intervention.
Comparison of our data with previously published classifications of endoscopic retrograde cholangiopancreatography (ERCP)-related perforations
The presence or absence of abdominal signs of diffuse peritonitis diagnosed by an experienced surgeon should play a central role in indication for surgery. In our series, 1 patient with free intraperitoneal air (Stapfer type I/Howard type III) but without diffuse tenderness was managed successfully without an operation. This is in concordance with the literature on the successful conservative management of peptic ulcer perforations.14,15 Additionally, not all patients with retroperitoneal perforations could be managed conservatively. In our study, 1 of the 4 patients treated surgically had retroperitoneal duodenal perforation (Stapfer type IV/Howard type I), which was managed successfully by a simple closure of the defect and drainage of the retroperitonum. An additional patient had a duodenal perforation complicated by an injury to the common bile duct (Stapfer type II–III/Howard type II) diagnosed with both retro- and intraperitoneal air on the CT scan. Both of these patients had diffuse abdominal tenderness indicating peritonitis, but were candidates for conservative therapy based on both Stapfer and Howard classifications.
If surgical treatment is indicated, we advocate the simplest damage control therapy possible, since the patients are usually fragile and possibly in a catabolic state due to malignancy and peritonitis. The operation should include an extensive lavage of the abdominal cavity and drainage of possible sites of abscess formation. The decision whether to explore and drain the retroduodenal space should be based on the intraoperative findings and the injury mechanism. Naturally, the indication of the ERCP could have an effect on the surgical strategy. Perforating stents and occluding bile stones can be removed during the operation, but contrary to the management guidelines suggested by Stapfer and colleagues,10 these do not represent a uniform indication to perform surgery. Stent perforations can be managed conservatively, and biliary occlusion can be treated by a percutaneous drainage as a bridging procedure and followed by a repeat ERCP. Contrary to the surgical therapy tailored to the intraoperative findings and possibly to the indication of ERCP, conservative therapy was uniform in our study population. All patients in this study, regardless of therapy, received broad-spectrum intravenous antibiotics, parenteral nutrition, a nasogastric tube and a nil-by-mouth diet. Unspecific misleading elevated inflammatory laboratory parameters due to cholangitis, pneumonia or cystitis should trigger radiological evaluation, not immediate surgery. In our study, 91% of patients had elevated leukocyte counts at one point during their stay in hospital. New onset leukocytosis without peritonitis prompted further work-up, including chest radiography and abdominal CT. The most important laboratory parameter in the decision-making regarding the management strategy were the levels of pancreatic enzymes. Patients with post-ERCP pancreatis could present with diffuse tenderness, although this is usually mild and resolves on conservative therapy. Previous studies have criticized unnecessary radiologic investigations,16 which could delay treatment and have a deteriorating effect on the outcome and provide no additional information regarding the indication for surgery. In one study published by Genzlinger and colleagues,17 immediate routine CT scans after ERCP revealed extraluminal free air in 29% of asymptomatic patients. Furthermore, several articles in the literature reported unacceptably low sensitivities for oral contrast studies in detecting duodenal perforations.18 Our series included 4 patients who had operative treatment; 3 of these patients underwent surgery within 24 hours of the initial ERCP. Interestingly, contrary to previous reports,10,11 there were no patients in our series with failed conservative therapy. One patient received prompt surgical treatment after delayed diagnosis: after careful retrospective review of medical charts it was concluded that the alarming signs developed only 4 days after the initial procedure, and the patient was promptly transferred to our department and underwent subsequent exploration.
Limitations
The limitation of our study is its retrospective nature and the relatively small number of patients treated with duodenal perforations after ERCP in our institution, but this complication is rare, and, to our knowledge, there are no prospective randomized trials in the literature.
Conclusion
Based on our study findings, we can conclude that ERCP is safe, but perforations occur also in the most experienced centres. Perforations have a high morbidity but could be managed with relatively low mortality. Patient selection is paramount; all patients suspected to have ERCP-related duodenal perforations should be transferred to the surgical department for further therapy. Initial treatment should include broad-spectrum intravenous antibiotics, parenteral nutrition, nasogastric tube and a nil-by-mouth diet. Previously published classifications have little value in the clinical setting. Treatment decisions should be based on frequent assessment of abdominal tenderness by an experienced surgeon and should be performed with the cooperation of the interventional radiology department and the gastrointestinal unit.
Footnotes
Competing interests: None declared.
Contributors: A. Dubecz, J. Ottmann, M. Schweigert, R.J. Stadlhuber, M. Feith and H.J. Stein designed the study. A. Dubecz, J. Ottmann, M. Schweigert, R.J. Stadlhuber, V. Wiessner and H. Muschweck acquired the data, which A. Dubecz, J. Ottmann and R.J. Stadlhuber analyzed. A. Dubecz and J. Ottmann wrote the article. All authors reviewed the article and approved its publication.
- Accepted December 23, 2010.