Abstract
Background: Clinical evaluation alone is still considered adequate by many clinicians who treat patients with appendicitis. The impact of computed tomography (CT) on clinical outcomes remains unclear, and there is no consensus regarding the appropriate use of CT in these patients. We sought to evaluate the impact of abdominal CT on the clinical outcomes of patients presenting with suspected appendicitis.
Methods: We conducted a systematic review of the literature to identify studies that examined clinical outcomes related to the use of abdominal CT in the diagnosis of acute appendicitis. Inclusion criteria were studies of adult patients with suspected appendicitis that evaluated the impact of abdominal CT on negative appendectomy rates, perforation rates or time to surgery. Two independent investigators reviewed all titles and abstracts and extracted data from 28 full-text articles. Statistical analysis was conducted using Review Manager 5.0.10 software.
Results: The negative appendectomy rate was 8.7% when using CT compared with 16.7% when using clinical evaluation alone (p < 0.001). There was also a significantly lower negative appendectomy rate during the CT era compared with the pre-CT era (10.0% v. 21.5%, p < 0.001). Time to surgery was evaluated in 10 of the 28 studies, 5 of which demonstrated a significant increase in the time to surgery with the use of CT. Appendiceal perforation rates were unchanged by the use of CT (23.4% in the CT group v. 16.7% in the clinical evaluation group, p = 0.15). Similarly, the perforation rate during the CT era was not significantly different than that during the pre-CT era (20.0% v. 19.6%, p = 0.74).
Conclusion: This meta-analysis supports the hypothesis that the use of preoperative abdominal CT is associated with lower negative appendectomy rates. The use of CT in the absence of an expedited imaging protocol may delay surgery, but this delay is not associated with increased appendiceal perforation rates. Routine CT in all patients presenting with suspected appendicitis could reduce the rate of unnecessary surgery without increasing morbidity.
Appendicitis is the most common emergency surgical condition, with more than 250 000 appendectomies performed yearly in the United States.1 Historically, negative appendectomy rates of 10%–20% have been accepted to avoid the consequences of missing a true case of appendicitis.2 Negative appendectomy rates of up to 40% have been reported in women of child-bearing age.3
In 1998, Rao and colleagues4 published their landmark study demonstrating the utility of using computed tomography (CT) in patients with suspected acute appendicitis. Over the past 10 years, numerous studies have been performed to evaluate the sensitivity and specificity of CT in the diagnosis of acute appendicitis.5 A recent systematic review showed that CT is a very accurate diagnostic tool in appendicitis, with an overall sensitivity and specificity of 94% and 95%, respectively.6
Whereas CT is an accurate diagnostic tool in patients with suspected appendicitis, the appropriate use of CT remains controversial. Clinical evaluation alone is still considered adequate by many clinicians who treat patients with appendicitis. The impact of CT on clinical outcomes remains unclear, and there is no consensus regarding the appropriate use of CT in these patients. Our objective was to perform a meta-analysis of the current literature evaluating the clinical impact of CT in the diagnosis of patients with suspected appendicitis. We sought to determine whether the use of CT, compared with clinical examination alone, in the diagnosis of acute appendicitis reduces negative appendectomy rates, time to the operating room and perforation rates.
Methods
Search strategy
We performed a systematic review of the literature to identify studies that examined clinical outcomes related to the use of abdominal CT in the diagnosis of acute appendicitis. We searched the MEDLINE, EMBASE and Cochrane databases for the period January 1980 to May 2007 using the following MeSH terms: [“appendicitis” OR “appendectomy” OR “appendix”] AND [“tomography, x-ray computed tomography” OR “tomography scanners”]. The above terms and their combinations were also searched as text words, and we used the “related articles” function to broaden the search. Two independent investigators (S.K., C.J.B.) scanned the titles, abstracts and keywords of every record to identify potentially relevant articles. Discrepancies between selected articles were resolved by consensus between the 2 reviewers. We reviewed the full texts of all articles selected to ensure eligibility for inclusion, and reference lists from articles selected by electronic searching were searched manually to identify further relevant trials. We contacted authors directly to obtain additional data that were not published but were felt to be relevant to our study.
Study criteria
To be included in this meta-analysis, the following criteria needed to be met.1 The studies must have included adult patients presenting with acute right lower quadrant (RLQ) pain,2 compared patients who underwent preoperative CT with those who underwent clinical examination alone3 and included at least 1 of the following clinical outcomes: negative appendectomy rate (as determined by the formal pathology report), perforation rate (as determined by the formal pathology report) or time from presentation in the emergency department (ED) to the operating room. We excluded studies that were composed of mostly pediatric populations (< 18 yr), case–control studies, case reports and case series.
Data extraction
Data were extracted from each included study using standardized data extraction forms developed a priori. Two independent reviewers (S.K., C.J.B.) extracted relevant data, and conflicts were resolved by consensus. Reviewers were not blinded to the authors or journal titles of the included studies. Data related to demographics, intervention, study design and outcomes were extracted. Data from all included studies were pooled to calculate pooled odds ratios (ORs) for negative appendectomy rates and perforation rates. Data on time to the operating room were collected but not statistically combined, as most of the studies did not provide the standard deviation needed to calculate the weighted mean difference.
Statistical analysis
We performed statistical analyses using Review Manager 5.0.10 software (The Cochrane Collaboration), and we calculated pooled ORs with 95% confidence intervals (CIs) for each outcome. Heterogeneity between studies was assessed using the Q test (significant at p < 0.05) and the I2 statistic using the 95% CI of I2 to test significance. Because heterogeneity was noticeable, we produced pooled estimates of the ORs using a random-effects model. Studies were stratified so that studies examining time from admission to the operating room and time from ED presentation to the operating room could be analyzed independently. We performed a sensitivity analysis to examine the influence of individual studies by omitting 1 study at a time and observing the effect on the OR.
Results
Included studies
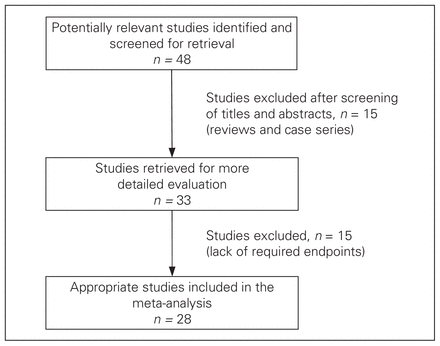
Our search of the MEDLINE, EMBASE and Cochrane databases yielded 1510 entries. Review of the titles and abstracts identified 48 studies where preoperative CT was the main predictor of clinical outcome in patients with suspected acute appendicitis. On review of the full text, 28 articles met the inclusion criteria: 2 randomized controlled trials (RCTs) and 26 cohort studies (Fig. 1, Table 1). The included studies comprised a total of 9330 patients. Eleven studies compared outcomes before the widespread use of CT for the diagnosis of appendicitis (pre-CT era) with outcomes after the use of CT became more frequent in patients with suspected appendicitis. This distinction was determined in each study based on when that institution showed a substantially increased rate of CT scanning. The remaining 17 studies compared outcomes between patients who underwent CT and those who underwent clinical evaluation alone.
Flow chart for selection of studies for the meta-analysis.
Studies included in a meta-analysis on the impact of abdominal computed tomography in patients with acute lower quadrant pain
In studies that recorded the type of contrast used for CT scanning, 1156 patients (38%) received a combination of intravenous and oral contrast, 826 (27%) underwent noncontrast studies, 527 (17%) had focused appendiceal studies using a limited number of axial slices through the RLQ and only rectal contrast, 134 (4%) received intravenous contrast alone, 32 (1%) received oral contrast alone and the remaining 368 patients (12%) had some combination of the above modalities. In 15 of the studies, patients underwent CT of the abdomen/pelvis, whereas 5 other studies evaluated clinical outcomes in patients receiving a focused appendiceal scan. In 8 studies, the extent of the CT scan performed was not specified. The median sensitivity for CT across all studies was found to be 95% (range 84%–99%), whereas the median specificity was 97% (range 85%–100%).
Excluded studies
Of the 48 studies where preoperative CT was the main predictor of clinical outcome in patients with suspected acute appendicitis, we excluded 20. Twelve studies were case series without a control group.30,34–44 Three articles were reviews without any primary clinical data.2,45,46 One article evaluated the clinical outcomes before and after the implementation of an ED protocol, but both arms of the study had identical rates of CT investigation.47 Another did not include the rate of CT for the post-CT era.48 One RCT randomly assigned patients to mandatory CT or standard management with optional CT if the surgeon felt that scanning was clinically indicated.49 The number of patients in the standard management group who underwent CT was not available, and an attempt to contact the authors did not yield a response. In 1 article, the rate of CT during the CT era was only 3%.50 The final excluded article used data from the California Inpatient File and thus generated a very large sample size (n = 75 452).3 The researchers used International Classification of Diseases (ICD)–9 billing codes instead of pathology reports to identify negative appendectomy and perforated appendicitis. Perforation rates were found to be substantially higher than what has previously been reported in the literature (43.6% and 27.6% for the CT and no-CT groups, respectively). Owing to the large number of patients in this study and the inherent uncertainty related to secondary nonclinical data sources, we performed our analyses with and without this paper included. The Q test for statistical heterogeneity was significant for both perforation rates and negative appendectomy rates with the study included, which was consistent with our concerns regarding the congruence between this study using administrative data and the other studies that used more reliable clinical data. Thus, we excluded this study from the main analysis.
Negative appendectomy rates
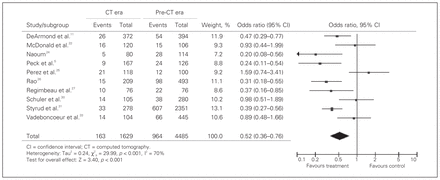
Ten studies compared negative appendectomy rates between the pre-CT and CT eras.5,11,22,24–27,30,31,33 The mean CT rate during the pre-CT era was 7.6% (range 0%–31.6%) and increased to 53.6% (range 33.6%–83.8%) during the CT era. Including all studies, 4485 patients were evaluated during the pre-CT era, and 1629 patients were evaluated during the CT era. With negative appendectomy as the outcome of interest and the pre-CT era as the reference, we found a pooled OR of 0.52 (95% CI 0.36–0.76) for the CT era (Fig. 2). The negative appendectomy rate was 21.5% during the pre-CT era, and it decreased to 10.0% during the CT era (p < 0.001). There was increased heterogeneity (χ2 = 29.99, p < 0.001, I2 = 70.0%). The article that most affected heterogeneity was by Perez and colleagues,25 which, when removed, resulted in an OR of 0.45 (95% CI 0.37–0.55), but significant heterogeneity (χ2 = 0.71, p = 0.008, I2 = 61.4%) remained.
Cumulative pooled estimates of odds ratios of negative appendectomy rates for the computed tomography (CT) era versus the pre-CT era.
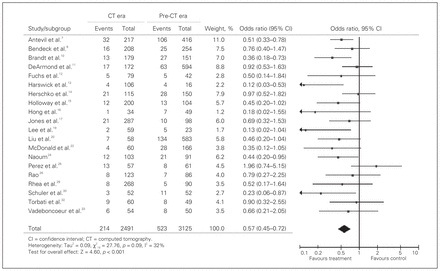
Twenty studies compared the negative appendectomy rates between patients who underwent preoperative CT and those who underwent clinical evaluation alone.7,8,10–17,19,20,22,24–26,28,30,32,33 There were 2491 patients in the CT group and 3125 patients in the clinical evaluation group, with a pooled OR of 0.57 (95% CI 0.45–0.72) in favour of patients who underwent CT (Fig. 3). The negative appendectomy rate was 8.6% for patients in the CT group and 16.7% in the clinical evaluation group (p < 0.001). Heterogeneity was not significant (χ2 = 27.76, p = 0.09, I2 = 31.6%).
Cumulative pooled estimates of odds ratios of negative appendectomy rates for computed tomography versus clinical assessment.
Time to the operating room
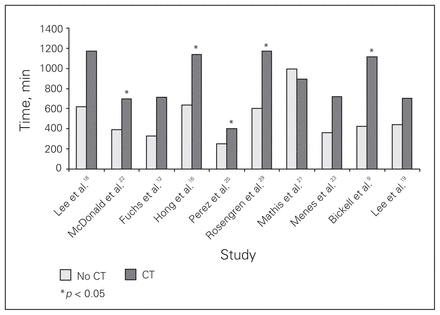
Ten studies (n = 1887) examined the time from the ED to the operating room, comparing patients who underwent preoperative CT with those who had not.9,12,16,18,19,21–23,25,29 Five studies reported statistically longer time in the CT group (Fig. 4). The mean waiting time was 468 minutes (7.8 h) for the clinical evaluation group and 800 minutes (13.3 h) for the CT group. More recent studies showed no difference in times in the CT group. No further statistical analysis was performed on this data set because standard deviations were not available to calculate a standardized mean difference.
Time to the operating room: computed tomography (CT) versus no CT.
Perforation rates
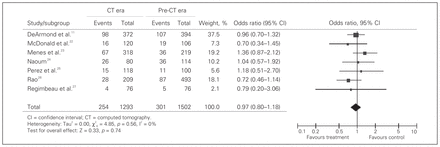
Seven studies compared perforation rates during the pre-CT era with those during the CT era.11,22–27 There were 1502 patients in the pre-CT era and 1293 patients in the CT era with a pooled OR of 0.97 (95% CI 0.80–1.18; Fig. 5). The perforation rate was 20.0% during the pre-CT era and 19.6% during the CT era, showing no statistical significance (p = 0.74). Heterogeneity was not significant (χ2 = 4.85, p = 0.56, I2 = 0%).
Cumulative pooled estimates of odds ratios of appendiceal perforation rates for the computed tomography (CT) era versus the pre-CT era.
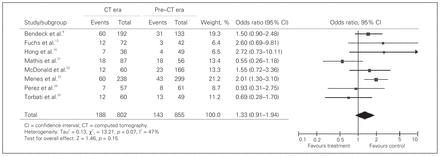
Eight studies compared the perforation rates in patients in the CT group with those in the clinical evaluation group.8,10,12,16,21–23,25,32 There were 802 patients in the CT group and 855 patients in the clinical evaluation group with a pooled OR of 1.33 (95% CI 0.91–1.94; Fig. 6). The perforation rate was 23.4% in the CT group and 16.7% in the clinical evaluation group (p = 0.15). Heterogeneity was not significant (χ2 = 13.21, p = 0.07, I2 = 47.0%).
Cumulative pooled estimates of odds ratios of appendiceal perforation rates for computed tomography versus clinical evaluation.
Sex subset analysis
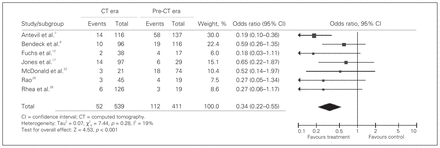
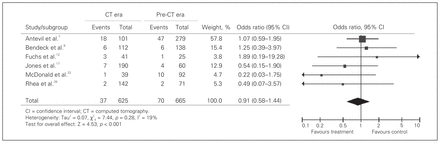
Seven articles reported sex-specific negative appendectomy rates, comparing patients who underwent preoperative CT with those who had not.7,8,12,17,22,26,28 Analysis of the 7 studies with a total of 950 female patients resulted in a pooled OR of 0.34 (95% CI 0.22–0.55; Fig. 7). The negative appendectomy rate for female patients was significantly lower in the CT group than in the clinical evaluation group (9.6% v. 27.3%, p < 0.001). Six studies with a total of 1290 male patients resulted in a pooled OR of 0.91 (95% CI 0.58–1.54). The negative appendectomy rate for male patients was 5.9% in the CT group and 10.5% in the clinical evaluation group and was not significant (p = 0.49; Fig. 8). Heterogeneity was not significant in either sex cohort (χ2 = 7.44, p = 0.28, I2 = 19.0%).
Cumulative pooled estimates of odds ratios of the negative appendectomy rate in female patients who underwent computed tomography versus those who underwent clinical assessment alone.
Cumulative pooled estimates of odds ratios of the negative appendectomy rate in male patients who underwent computed tomography versus those who underwent clinical assessment alone.
There were only 2 studies that examined perforation rates based on sex and, therefore, these data were not analyzed.
Discussion
The use of CT in the diagnosis of appendicitis began in the 1990s, but its popularity increased with the landmark study by Rao and colleagues in 1998.4 Since that time, there have been 28 studies examining the influence of CT on clinical outcomes. During the late 1990s and early 2000s, the CT scaning rate in patients with suspected appendicitis increased from less than 10% to over 50% at many institutions.5,25,51 Comparative studies published in the past 10 years have demonstrated a mean uniform decrease in the negative appendectomy rate after the widespread implementation of CT. Our review demonstrated a significant decrease in the negative appendectomy rate from 21.5% during the pre-CT era to 10.0% during the CT era (p < 0.001), and there was significant heterogeneity for this outcome in this analysis. The article that most affected heterogeneity was that of Perez and colleagues,25 which, when removed, decreased but did not eliminate heterogeneity. This article’s contribution to heterogeneity may have resulted from the fact that the diagnostic accuracy of CT in this study did not improve over time (81.8% in 1994 and 80.7% in 2000) as it did in other institutions, resulting in a negative appendectomy rate that was actually higher during the CT era than the pre-CT era.
To better delineate the role of CT in patients with suspected appendicitis, our meta-analysis combined data from 20 studies that compared the negative appendectomy rate among patients who underwent preoperative CT with those who underwent clinical assessment alone. Again, we found a statistically significant decrease in the negative appendectomy rate from 16.7% in the clinical evaluation group to 8.6% in the CT group (p < 0.001). Most of the studies analyzed were retrospective cohort studies, which may have introduced an important selection bias. However, it is more likely that those patients presenting with the “classic” signs of appendicitis would go straight to the operating room. In contrast, those with more atypical presentations would more likely undergo preoperative imaging. These biases should have led to fewer negative appendectomies in the patients with appendicitis diagnosed on clinical grounds; instead, there was a higher negative appendectomy rate in this group despite the bias. However, a physician’s practising habits may also influence their use of CT, irrespective of the degree of diagnostic uncertainty. Regardless, the significantly lower negative appendectomy rate in the CT group suggests that CT in all patients may decrease the negative appendectomy rate even further.
To date, there have been no RCTs comparing preoperative CT with clinical evaluation alone in patients with suspected appendicitis. A recent RCT performed by Lee and colleagues19 compared mandatory and selective CT for adult patients presenting with acute RLQ pain of less than 72 hours’ duration and suspected appendicitis. There were 80 patients randomly assigned to the selective CT imaging group, and 72 were randomly assigned to the mandatory imaging group. The authors found a trend toward decreased negative appendectomy rates in the mandatory CT group with a reduction in the negative appendectomy rate (13.9% v. 2.6%, p = 0.07). Interestingly, there was no significant difference in the mean time to the operating room, and the perforation rate was 18.4% in the selective group compared with 10.3% in the mandatory CT group (p = 0.24). Walker and colleagues49 performed a similar study comparing a mandatory CT group (n = 65) with a standard management group (n = 63) where a CT scan could be obtained if it was felt to be clinically warranted. The negative appendectomy rate was found to be 19% in the standard management group and 5% in the mandatory CT group (p = 0.08). Both of these studies show a strong trend toward decreased negative appendectomy rates with mandatory CT, and the lack of significance found in these studies could be owing to type-II error resulting from the relatively small sample sizes.
From our meta-analysis, we estimated that 13 CT scans are needed to avoid 1 unnecessary surgery. Although negative explorations carry a low mortality (0.14%), the morbidity associated with these procedures may be greater than is generally appreciated by surgeons. Negative explorations result in substantial expense and lost time at work, and they create adhesions, which have been shown to cause intestinal obstruction in up to 1.25% of postappendectomy patients.12
One of the major concerns about the widespread use of CT in diagnosing appendicitis is the risk of radiation, especially in women of child-bearing age. Computed tomography involves larger radiation doses than the more common conventional radiologic imaging procedures. It is estimated that more than 62 million CT scans are currently obtained each year in the United States, compared with about 3 million in 1980.52 No large-scale epidemiologic study of the long-term risk of cancer associated with CT scans has been published to date. Potential cancer risks associated with the radiation exposure from CT have been estimated and extrapolated from studies of atomic-bomb survivors. The estimated lifetime attributable risk of death from cancer that results from abdominal CT is less than 0.06% in a 25-year-old and less than 0.02% in people over 40 years of age.52 The risks are minimal and they are outweighed by the risks of performing negative surgeries. However, it is imperative that radiation exposure be minimized by using alternative imaging methods when feasible, especially in children and women of child-bearing age. This could include focused appendiceal CT, abdominal/pelvic ultrasonography or magnetic resonance imaging, which result in less radiation and have been shown to be reasonably accurate for the diagnosis of appendicitis.6,26
There is some evidence that the increased use of CT may delay surgical intervention in some patients. Our meta-analysis shows that those patients who undergo CT have surgery, on average, 5 hours later than those who are assessed by clinical acumen alone. This delay may be related to the time to obtain a CT scan as well as diagnostic delay owing to a more complicated patient group presenting with atypical symptoms. In patients with an unclear diagnosis, extensive investigations such as gynecologic consultations and increased ancillary testing (radiography, pelvic ultrasonography) may also contribute to delays to surgery.
Menes and colleagues23 evaluated clinical outcomes during the earlier years (1996–1998) of CT scanning and compared them with those in more recent years (2001–2002). During that time, the rate of CT scanning increased 3-fold, and the time to the operating room in patients who underwent CT decreased from 18 hours to 12 hours (p = 0.040). In the RCT by Lee and colleagues,19 there was no significant delay to surgery in patients who underwent CT. This could be because this is a more recent study and CT scans are now more easily obtained. It could also be related to the increased ease and accessibility of obtaining a CT scan within the framework of an RCT protocol.
A concerning potential consequence of delayed surgery is appendiceal perforation. A recent retrospective study by Ditillo and colleagues53 examined the pathologic severity and postoperative complications of appendicitis with increased time from diagnosis to definitive treatment. They concluded that the severity of pathology and the complication rate in patients with acute appendicitis are both time-dependent. However, the authors identified that patient delay in presenting to the ED was more profoundly related to worsening pathology than were in-hospital delays. Similarly, Earley and colleagues54 evaluated the implementation of an acute care surgery model and its effects on outcomes of appendectomy. They found that the presence of an in-house surgeon resulted in a significant decrease in time from the ED to the operating room. Furthermore, reduced waiting times led to a significant decrease in perforation rate and rate of postoperative complications. Bickell and colleagues9 evaluated the association between time and the risk of appendiceal rupture. Patients whose appendices ruptured had a significantly longer time to presentation and an increased in-hospital time; CT was found to significantly increase time to the operating room. The above studies support the argument that time spent waiting in hospital does adversely affect perforation and complication rates.
Whereas these studies suggest that delays to surgery may lead to perforation, our meta-analysis demonstrated similar rates of perforation between patients in the CT group and those in the clinical evaluation group (23.4% v. 16.3%, p = 0.15). Again, most of the studies included in our analysis were retrospective and were subject to selection bias. Patients with an atypical presentation or a longer history of abdominal pain would be more likely to undergo CT to aid in the diagnosis. These same patients may be more likely to have perforated appendices, possibly having an abscess, before presentation.
Several studies have evaluated the effect of CT on negative appendectomy rates based on sex. Previous reports in the literature have suggested that CT may have more of an impact in decreasing the negative appendectomy rate in women. Fuchs and colleagues12 showed that CT reduced the negative appendectomy rate in women from 23.5% to 5.3%. Bendeck and colleagues8 noted a significantly lower rate of negative appendectomy in women undergoing CT for appendicitis, but they found that CT had no effect on the negative appendectomy rate for men. Rao and colleagues51 also found that the most notable improvement in decreasing negative explorations occurred in women, with the negative appendectomy rate decreasing from 35% to 11%. Our meta-analysis showed no significant reduction in the negative appendectomy rates in male patients undergoing CT. The negative appendectomy rate was 10.5% in male patients who underwent clinical evaluation alone and 5.9% in those who underwent CT (p = 0.69). However, the negative appendectomy rate was significantly affected in female patients, with a rate of 27.3% in those who underwent clinical evaluation alone versus 9.6% in those who underwent CT (p < 0.001). Most studies in this review did not present outcomes stratified by sex, so the observed difference in negative appendectomy rates in men may be significant, but masked by type-II error.
Limitations
To our knowledge, this study is the first meta-analysis to evaluate the clinical impact of CT in the diagnosis of acute appendicitis. The analysis of 28 studies involving over 9000 patients provides important insight into the role of CT in patients with suspected appendicitis. However, there are several limitations to this study. Most of the included studies were retrospective in nature. The resulting selection bias affected many of the results in the comparisons of the CT and clinical evaluation groups. As previously stated, this bias would make our study less likely to show a difference in negative appendectomy rates in patients who underwent CT. Another weakness of the analysis is that patients who underwent appendectomy were the only participants who were identified in most of the retrospective studies. This method of patient selection fails to identify patients who presented with suspected appendicitis but had negative CT scans. A negative CT scan has the potential to avoid a nontherapeutic laparotomy, diagnose alternative conditions that may account for patient’s presentation and allow expedient discharge from hospital.
Conclusion
In summary, the results of this meta-analysis show that CT in patients with suspected appendicitis leads to lower negative appendectomy rates. Limited subgroup analysis suggests increased diagnostic benefit in using CT in women compared with men; however, the utility of CT in men has not been well studied. Whereas patients with appendicitis who underwent CT experienced an increase in time from assessment to surgery, this did not seem to adversely affect the perforation rates. Based on the results of this meta-analysis, routine CT in all adult patients presenting with acute lower abdominal pain suspicious for appendicitis can be justified. However, the poorly defined risks of CT–related radiation must be considered and integrated into this clinical decision. Further directions of study include the development and prospective evaluation of an expedited imaging protocol with interdepartmental cooperation among the departments of surgery, radiology and emergency medicine.
Footnotes
Competing interests: None declared.
Contributors: All authors helped design the study, analyze the data, critically review the article and approved its publication. Drs. Krajewski and C. Brown acquired the data and wrote the article.
- Accepted November 3, 2009.