Abstract
Background: Dislocation may complicate revision total hip arthroplasty (THA). We examined the correlation between the components revised during hip arthroplasty (femur only, acetabulum only and both components) to the rates of dislocation in the first and multiple revision THA.
Methods: We obtained data from consecutive revision THAs performed between January 1982 and December 2005. Patients were grouped into femur-only revision, acetabulum-only revision and revision THA for both components.
Results: A total of 749 revision THAs performed during the study period met our inclusion criteria: 369 first-time revisions and 380 repeated revisions. Dislocation rates in patients undergoing first-time revisions (5.69%) were significantly lower than in those undergoing repeated revisions (10.47%; p = 0.022). Within the group of first-time revisions, dislocation rates for acetabulum-only revisions (10.28%) were significantly higher than those for both components (4.61%) and femur-only (0%) reconstructions (p = 0.025).
Conclusion: Although patients undergoing first-time revisions had lower rates of dislocations than those undergoing repeated revisions, acetabulum-only reconstructions performed at first-time revision arthroplasty entailed an increased risk for instability.
Dislocation is a common cause of failure after primary and revision total hip arthroplasty (THA),1,2 exceeded only by aseptic loosening.2 Dislocation is disabling for the patient and compromises the long-term function of the joint and ultimate patient satisfaction.3
Dislocation rates after primary THA range from 0.5% to 5%,1,2 while their frequency increases to 0.95%–27% after revision THA.4–8 Impingement and poor abductor muscle function are often the underlying cause of instability. Thus, surgical technique as well as component design and alignment have a substantial impact on the risk for post-THA dislocation.9
Previous reports have shown that larger femoral head size directly influences the primary arc of motion and subsequent stability.5,6,10 In addition, use of an elevated acetabular liner rim in revision THAs decreases the rates of dislocations.5,11 In contrast, displaced trochanteric nonunion precludes proper abductor function and has been associated with increased rates of dislocations.8
Revision THA is often associated with bone loss either due to osteolysis, infection or iatrogenesis as a result of the removal of well-fixed components. Acetabular bone loss in particular may bias the surgeon to less favourable component alignment and subsequent instability since the combined acetabular and femoral components’ anteversion may not be fully restored.1,5,6,9,10 The present study addressed the following clinical questions. What are the rates of dislocation for acetabulum-only, femur-only or both component revision THA? Are the rates of dislocations in each group different between first revision and repeated revisions?
Methods
We obtained data for all revision THAs performed between January 1982 and December 2005 performed by the senior author (A.E.G.). After each revision, data were recorded in a prospective database. We excluded revisions that consisted of liner exchange only or that were specifically performed for infection or instability from our analysis.
We examined the rates of dislocation in patients undergoing first revision and those undergoing repeat revisions according to the revised components: femur only, acetabulum only and both components.
In all cases the surgical procedure was a lateral approach with a trochanteric osteotomy. Patients followed hip precautions that included no active abduction, hip flexion under 90° and no cross-leg adduction for 3 months.
Statistical analysis
We used a nonparametric χ2 test to compare the incidence of dislocation in each of the groups. We considered results to be significant at p < 0.05.
Results
Between January 1982 and December 2005, 887 revision THAs were performed in 761 patients. We excluded 106 revisions (11.9%): 54 that consisted of liner exchange only, 28 that were performed for infection and 24 that were performed for instability. In addition, 32 (3.6%) revisions were in patients who were lost to follow-up, leaving 749 revision THAs in 632 patients available for analysis.
The mean age of patients at the time of surgery was 64 ± 14.3 (range 30–93, median 67) years. Five hundred (66.7%) revisions were performed in women and 249 (33.3%) were performed in men. Average follow-up was 13.2 ± 6.9 (range 2–23) years. The database included 369 first revisions and 380 repeat revisions. The indication for revision arthroplasty was aseptic loosening in 659 hips, periprosthetic fractures of the femur in 80, fractures of the implant in 3 and fractures of a femoral allograft in 7 hips. In all, 418 (55.8%) arthoplasties involved revision of both the acetabulum and the femur, 202 (26.9%) involved the acetabulum only and 129 (17.3%) involved the femur only.
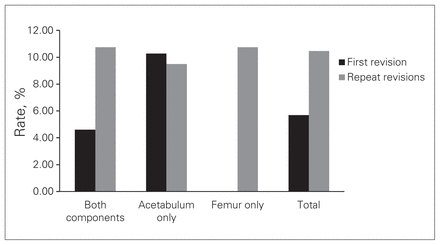
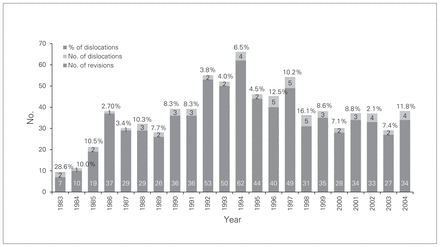
There were 61 (8.17%) dislocations in the entire series. Rates of dislocation were similar in men and women. Forty-one (8.2%) dislocations occurred in women and 20 (8.03%) in men (p = 0.47). The overall dislocation rate was significantly lower in the first-time revision group (5.69%) than in the repeat revision group (10.47%, p = 0.022; Fig. 1). In the first-revision group, the dislocation rate was significantly higher for the acetabulum-only reconstruction (10.28%) than for both components (4.61%) and femur-only reconstructions (0%, p = 0.025). In the multiple revision group there was no significant difference between the dislocation rate in the acetabulum-only (9.49%), femur-only (10.75%) and both component reconstructions (11.02%, p = 0.92; Fig. 1). Twenty-nine (47.5%) dislocations were managed by closed reduction and 5 were treated with open reduction. Twenty-seven (44.3%) dislocations required revision arthroplasty. The rates of dislocation were 9.2% per year (range 2.7%–28.6%; Fig. 2).
The rates of dislocation in first-revision and repeat/revision total hip arthroplasty.
Distribution in absolute numbers and rate of dislocations per year.
Discussion
Dislocations are one of the most disabling complications of hip arthroplasty and may necessitate a prolonged hospital stay or further surgical intervention.1,12 Although numerous studies have documented the rates of dislocation after primary THA, to the best of our knowledge there are no reports examining the incidence of both of these complications in a single surgeon’s revision practice over a period of 23 years.
The possible weaknesses of retrospective studies derived from the influence of multifactorial variables (surgical technique, implant designs, operating room environment, perioperative antibiotics protocol and postoperative hip precautions) associated with these complications can be substantially reduced when evaluating a single surgeon’s practice. We acknowledge that the early revisions in the 1980s and early 1990s were performed via a classical Charnley trochanteric osteotomy, whereas all subsequent revisions were performed via a modified trochanteric sliding osteotomy.11,13 However, since this is a retrospective study relying on a database, the exact data regarding the type of osteotomy from the early years are missing. Yet, this advancement in the surgical technique was put to all types of revisions and influenced them similarly.
Revision THA is a technically demanding procedure that often requires an extensile exposure for a controlled removal of previously implanted components and management of accompanying bone loss. The main objective of this study was to examine the correlation between the components revised during the revision arthroplasty and the rates of postoperative dislocation and infection. The overall dislocation rate was 8.14% in this series, which is well within the range reported in other studies, thus validating our data.7,8,14–16
The first-time revision group had essentially half the rate of dislocation occurring in the repeat revision group (5.69% v. 10.47%, p = 0.022; Fig. 1). First-time revisions consisting of acetabulum-only reconstructions had significantly higher dislocation rates (10.28%) than reconstructions of both components (4.61%) and the femur-only reconstructions (0%, p = 0.025; Fig. 1).
These differences can be attributed to the fact that the acetabular bone loss encountered and the perilous position of a well-fixed femoral stem precluding adequate exposure may bias the surgeon to place the cup in a less favourable orientation. Conversely, in femoral revisions adequate femoral anteversion can be maintained even at the presence of severe bone loss, especially with the availability of modular femoral stems. In revisions of both components, a satisfactory combined anteversion can be more readily established, although the required surgical exposure and soft tissue compromise can be more extensive.
Dislocation rates within the multiple revisions group were similar, regardless of the revision type (p = 0.93; Fig. 1). This finding can be derived from a repeated insult that was inflicted on the soft tissue envelope, specifically the abductor muscles, resulting in at least a temporary compromise in their function and potentially exposing the patient to instability.16,17 Since the extent of soft tissue compromise was not consistent in this group of patients, it may have been a confounder that obscured the effect of revising each type of reconstruction leading to these results.
Based on this data, we contend that when performing acetabulum-only revisions the threshold to use ancillary precautions for prevention of postoperative instability should be lowered. These measures should include an abductor-sparing surgical exposure, such as a trochanteric slide osteotomy and use of larger size femoral heads or a hooded liner. The fixation of the femoral stem as well as its alignment should be carefully examined. The combined acetabular and femoral anteversion must be appropriately established and impingement systematically ruled out.5,10
Conclusion
Both the surgeon and patient should be aware of the increasing risk of instability after acetabulum-only revisions. Since the first revision arthroplasty has the lowest complication rates, every reasonable effort should be made to provide the patient with a stable and durable joint at the time of the index revision arthroplasty.
Footnotes
The first 2 authors contributed equally to this work.
Competing interests: None declared.
Contributors: Y. Kosashvili, M. Drexler, D. Backstein and O. Safir designed the study. Y. Kosashvili, M. Drexler, D. Lakstein, A. Safir and R. Chakravertty acquired and analyzed the data, which T. Dwyer and A. Gross also analyzed. Y. Kosasvhili and M. Drexler wrote the article, which all authors reviewed and approved for publication.
- Accepted April 14, 2013.