The principles that guide optimal prescribing for older patients1,2 (Box 1) include deprescribing medications that are no longer indicated, appropriate or aligned with evolving goals of care. Deprescribing is a relatively new term that focuses attention on the sometimes overlooked step in medication review of stopping medications to improve outcomes and decrease risks associated with polypharmacy in older people.3–5 These risks include nonadherence,6 adverse drug reactions,7 functional and cognitive decline,8 and falls.9,10 In Canada, more than 50% of older people living in long-term care facilities and 27% of those living in the community take more than five medications a day.11 Although frailty12 should be a catalyst for deprescribing, the principles and practice of deprescribing apply to all older patients and, if integrated early into care, may play a role in preventing frailty.
Principles to guide prescribing and deprescribing medications in older patients1,2
Pharmacokinetics: what the body does to the drug; what factors determine the concentration of the drug at the target receptor or organ
Absorption: little change due to aging alone, but it can be affected by medications and conditions common in older people
Distribution: increased fat:water ratio with aging; protein binding may be affected by malnutrition or medical conditions
Metabolism/excretion: decrease in some liver metabolism with aging may affect different drugs differently; decrease in renal excretion with aging may affect drugs dependent on kidneys for excretion
Pharmacodynamics: what the drug does to the body; what factors affect whether medication will have a greater or lesser affect with same serum concentration
Prescribing tips
Remember that medications may cause illness
Know the patient and his or her current medications (and how they are taken)
Consider nonpharmacologic therapy
Know the pharmacology of the prescribed drugs
Keep drug regimens simple
Establish treatment goals at the time of prescription
Strive for a diagnosis before prescribing; if a therapeutic trial is done, stop medications if treatment goals are not reached
Encourage the patient to be a responsible medication user and to participate in his or her medication management
Consider the patient’s current medications and medical conditions before adding or changing new medications
Start low, go slow (but get there!)
Monitor closely for adverse effects when starting or stopping medications
Manage the whole of the patient’s treatment regimen
In this article, we describe an approach to deprescribing based on principles, practice and available evidence. We reviewed evidence from systematic reviews and randomized controlled trials on the impact of deprescribing (Box 2). Most of the studies failed to measure clinical outcomes relevant to the care of older patients, such as improved functioning. The quality of the evidence was limited by small samples, short study durations and heterogeneous study designs.13–15 Nonetheless, we found evidence16 that a substantial proportion of older patients can tolerate careful dosage reduction or withdrawal of certain classes of medications without harmful consequences and with possible improvement in quality of life, especially if the goals of care shift from disease-specific targets to improvements in symptom management and function.
Evidence for this review
We included published systematic reviews that were known to us. We then searched the databases Embase and MEDLINE using the terms “deprescribing” and “drug withdrawal” to identify additional systematic reviews as well as reports of randomized controlled trials of deprescribing published from January 2010 to March 2014. We restricted our review to articles published in English that had a study population aged 65 years or more.
When and for whom is deprescribing appropriate?
Although all older people taking prescribed drugs may benefit from a medication review with a deprescribing lens, those who are frail12 are the main target of this approach. Frail patients tend to take more medications and have more adverse outcomes related to medications than other older patients. They are also more likely to have limited life expectancy than well older people of similar age.17 Medication lists tend to lengthen as patients age, and there are few guidelines to inform medication management in the context of polypharmacy, multiple morbidities and age-related changes to pharmacokinetics and pharmacodynamics (Box 1). All prescribers contributing to the medication list need to be alert to “prescribing inertia”18 (the tendency to automatically renew a medication even when the original indication is no longer present) and should view polypharmacy as an impetus to deprescribe when appropriate.
Any patient interaction can be an opportunity for critical medication review. Certain transitional events in the care of older patients provide identifiable opportunities. For example, medication errors tend to occur during transfers between care settings.19,20 To reduce this risk, facilities routinely undertake systematic reconciliations of medication lists between sites; this is an opportunity for deprescribing. Similarly, changes in the overall health of a patient that affect life expectancy, such as the diagnosis of a terminal cancer or progression of dementia or clinical frailty,17 signal the need for medication review to identify drugs that are unlikely to provide meaningful benefit to the individual in their remaining time.21
Can deprescribing medications improve clinical outcomes?
It is well recognized that medications can cause harm in older patients, and there is growing recognition that careful adherence to disease-specific guidelines in frail patients can result in increased risks of drug interactions and adverse reactions.22
Despite this context, the evidence to support deprescribing as a broad strategy to improve clinical outcomes in older patients is weak. According to three recent reviews,13–15 most of the trials studying deprescribing failed to measure clinical outcomes relevant to the care of older patients, such as improved functioning, and were limited by small samples and short study durations. Although many of the interventions involved pharmacists, the engagement between the pharmacist and prescriber was not adequately described,14 and few studies incorporated patient perspectives. Heterogeneity in study design, sample selection, choice of outcome measure and intervention made it difficult to synthesize results and draw conclusions.
Nonetheless, when the evidence about deprescribing is organized by the intentions to stop drugs that are no longer indicated, that are no longer appropriate or that no longer align with goals of care, deprescribing appears to be potentially helpful without causing substantial harm, if done well.
Drugs that are no longer indicated
A systematic review of 31 trials involving older adults, published in 2007, examined the benefits and harms of withdrawing medications felt to be no longer indicated.16 The studies focused on the complete withdrawal of one of four classes (benzodiazepines, antihypertensives, diuretics for indications other than heart failure and antipsychotics). Although the included studies were limited by small samples and short durations, the results showed that a substantial proportion of participants could tolerate withdrawal of one of these classes and experienced benefits of reduced risk of falling (e.g., psychotropic medication withdrawal, hazard ratio 0.34, 95% confidence interval 0.16–0.74)23 and improvement in total memory test scores (e.g., benzodiazepine withdrawal, p< 0.004).24
These results are borne out in current clinical practice. It is almost conventional wisdom that tapering benzodiazepines25 can improve cognition and reduce the risk of falls. The recent changes in clinical practice guidelines to relax targets for blood pressure (e.g., 150/90 mm Hg)26,27 and blood glucose (hemoglobin A1C concentration < 7.5%)28 in older patients is informed by the trade-off between the risk of vascular events with the risk of falling because of orthostatic hypotension29 or hypoglycemia. Likewise, there is evidence that a systematic approach to reduce the prescribing of antipsychotics for behavioural symptoms of dementia when stable allows many people to be off medications for sustained periods of time or indefinitely.30
Drugs that are no longer appropriate
A recent Cochrane review31 concluded that systematic medication reviews involving a pharmacist working closely with the physician and the patient or caregiver results in a substantial reduction in inappropriate prescribing, either through medication substitution or discontinuation. The results from these studies do not clarify whether improving appropriateness of prescribing improves clinical outcomes; however, this association may be inferred from the evidence about risk of adverse outcomes used to construct tools to identify inappropriate medications in older patients, such as the Beer criteria.32
Drugs that no longer align with goals
Frail patients or their substitute decision-makers may shift treatment goals away from prolonging life to controlling symptoms or maximizing function. Eliciting preferences and perspectives on outcomes and goals of therapy is important to guide decisions to reduce or stop medications. In their work on universal health outcomes, Tinetti and colleagues33 found that the proportion of older patients who identified reducing the risk of falls as their priority equalled the proportion who prioritized stroke prevention with use of antihypertensives. Decreasing the dose or stopping an antihypertensive medication may be an acceptable choice for someone who has had frequent falls or has limited function, a poor prognosis or recent hip fracture, even at the cost of increased stroke risk. More studies are needed to assist with these difficult discussions and decisions about preferences and trade-offs.
What are some of the guiding principles and steps involved in deprescribing?
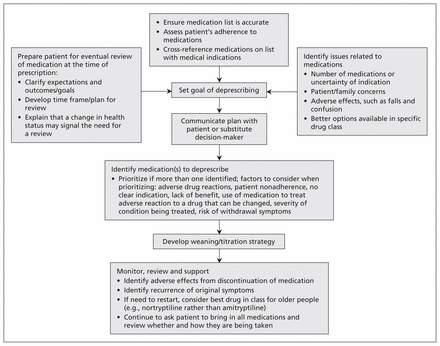
In the absence of clear evidence about the best approach to deprescribing, a structured stepwise approach is recommended (Figure 1, Table 1).3,4 Either a specific clinical concern or a routine medical review may prompt deprescribing. The first step is to ask the patient to bring in all prescribed and over-the-counter medications for a visual “brown bag review” by the physician, nurse or pharmacist. This exercise provides a lot of information about the patient’s understanding of and attitudes toward his or her medications and pill-taking habits. The resulting list of current medications should be cross-referenced with the chart and the pharmacy list when possible. Each medication should be classified according to indication. Medications without a current, credible indication and medications duplicated for the same indication are candidates for deprescribing. In addition, the appropriateness of drug choice and dose within each class of medications may be evaluated at this point and modified if required. A number of tools (Table 2) are available to assist with identifying inappropriate medications32,34–40 and, occasionally, relevant medications that need to be started.36
Practical approach to deprescribing.
Examples of tools to assist with medication review and deprescribing35
Often patients will have stopped taking a prescribed medication on their own volition. It is necessary to understand why and to evaluate the justification for continuing with the prescription or not. Medications not being taken regularly are candidates for discontinuation if there are no evident health consequences resulting from the nonadherence.
Current medications should align with current goals of care. With older patients, discussions about goals of care need to be framed in terms of the patient’s functional ability, clinical frailty and life expectancy. Predicting life expectancy remains as much the art of medicine as science. According to a recent systematic review of 16 potential prognostic indicators, 10 predicted greater than 50% mortality, but only 3 predicted greater than 80% risk in the highest risk group.41 Tools focusing on severity of frailty, such as the Clinical Frailty Scale,12,42 provide general prognostic information that may help to identify patients with limited life expectancy.
As part of the discussion about goals of care, it is important to clarify the patient’s preferences for trade-offs between risk reduction (e.g., “I want to avoid a stroke at all costs”) and symptom management (e.g., “I want help with my pain”) or between disease-specific targeted goals (e.g., “Please lower my blood pressure”) and universal goals (“Please keep me as independent as possible”). As goals of care evolve from disease-specific to more universal ones, understanding the relative contribution of chronic conditions to universal outcomes such as self-rated health, functioning, symptom burden and mortality can help to elicit priorities and guide clinical decisions.43
Once a decision to deprescribe a drug is made, engaging the patient or caregiver in the plan is important. A number of medications require tapering. Health care providers, patients and care-givers need to monitor for withdrawal-related adverse events (Table 3).44,45 In some instances, it may be necessary to restart the medication.
What are some of the challenges and barriers to deprescribing?
Establishing a successful deprescribing plan takes time and open discussion between the physician and the patient, which does not always occur. Studies on the topic identify several barriers in attitude and practice to be overcome by both physician and patient.
Schuling and colleagues46 conducted focus groups with Dutch general practitioners to explore their feelings about and experiences with deprescribing for very old patients with multiple morbidities. They found that the physicians tended to dichotomize medications into symptomatic and preventive types. Physicians expressed more difficulty about withdrawing preventive medications because of the lack of evidence to inform patients about the specifics of risks and benefits with discontinuation and because of the challenge of discussions about life expectancy and quality of life. The general practitioners also expressed concern about stopping medications prescribed by medical specialists. They identified training in shared decision-making to elicit patient preferences and explicit rules for collaborating with medical specialists as potential ways to help them with deprescribing.
Reeve and colleagues47 published a systematic review of 21 studies related to medication cessation and patients’ beliefs. Three themes emerged: beliefs about the appropriateness of the medication being deprescribed, concerns about the process for cessation, and attitudes of family and physicians about the deprescribing process. Not surprisingly, patients’ beliefs that the prescribed medication was doing something or was “better than doing nothing” presented barriers to stopping the medication, whereas beliefs that the medication was no longer appropriate enabled cessation. Patients reported that ensuring the process for deprescribing was monitored, supported and suitably paced assisted discontinuation, as did good relationships with the physicians and support of family over the process.
Recognition of terminal illness is an important reason to review goals of care and medications. However, even when faced with a terminal illness, some patients will be concerned about stopping medications they have been taking for years, especially when a physician in the past has stressed its importance. One example may be stopping a medication for the primary prevention of cardiovascular disease, even though there is little evidence to support its use in individuals aged over 80 years and even less evidence in those aged over 90. A randomized controlled trial is currently under way to determine whether there is a difference in survival time and quality of life between patients with advanced life-limiting illness whose statins are discontinued and those whose statins are continued (ClinicalTrials.gov trial no. NCT01415934).
Medications commonly used in palliative and end-of-life care can have adverse effects such as confusion, drowsiness, constipation and fatigue. To optimize the use of these medications, it may be prudent to minimize the use of other medications that could potentially worsen these effects. For example, ferrous gluconate may no longer provide achievable benefit for anemia but may exacerbate constipation caused by opiates.
Paradoxically, stopping a medication with a previously unrecognized adverse effect can sometimes improve overall function and change the short-term outlook at end of life. Although not well described in the literature, many physicians caring for patients with end-stage heart failure have had the experience of patients rallying with short-term improvement when high doses of cardiac medications are stopped or decreased because of apparently imminent death.
These practical lessons reinforce the importance of understanding the current indication for each medication prescribed to an older patient and a readiness to review and deprescribe as appropriate.
Unanswered questions
Which approach to deprescribing is most effective in improving clinical outcomes? Most approaches seem to involve a pharmacist and prescriber. Available study interventions are too heterogenous or poorly described to permit comparisons between approaches.
How effective are medication reviews in improving patient-centred results such as quality of life? Most existing trials fail to measure outcomes such as improved functioning and are of too short a duration or too small a size to show significant clinical improvements with deprescribing.
Does primary prevention of cardiovascular disease at end of life improve quality of life? Studies looking at the role of statins in end-of-life care are underway.
Key PointsThe same principles that guide prescribing for older patients guide deprescribing for this patient group.
Identify drugs that are no longer indicated, appropriate or align with goals of care.
Engage the patient, family and other health care providers in the process.
Develop a tapering/discontinuation plan and monitor adverse outcomes and benefits.
Acknowledgement
Karen Gagnon contributed to the design and conduct of the original literature search and assisted with acquiring abstracts and articles.
Footnotes
See related editorial at www.cmaj.ca/lookup/doi:10.1503/cmaj.122099 and articles at www.cmaj.ca/lookup/doi:10.1503/cmaj.122012 and www.cmaj.ca/lookup/doi:10.1503/cmaj.130523
Competing interests: None declared.
This article has been peer reviewed.
Contributors: Both authors contributed to the original concept of the work and acquired, analyzed and interpreted data and references. They drafted and revised the manuscript, approved the final submission and agreed to be guarantors of the work.