Abstract
Background: The use of prophylactic mesh in end colostomy procedures has been shown to reduce the rate of parastomal hernia. However, the degree to which the practice has been adopted clinically remains unknown. We conducted a study to evaluate the current opinions and practice patterns of Canadian and US colorectal surgeons with regard to the use of prophylactic mesh in end colostomy.
Methods: Between May and July 2017, we conducted an internet-based survey of colorectal surgeons in Canada and the United States (selected at random). Using a questionnaire designed and tested for this study, we assessed the rate of mesh use, types of mesh and placement techniques, and perceived barriers and facilitators associated with the practice.
Results: Forty-eight (51.6%) of 93 invited Canadian surgeons and 253 (16.6%) of 1521 invited US surgeons responded (overall response rate 18.6%). Of the 301 respondents, 32 (10.6%) were currently using mesh, 32 (10.6%) had previously used mesh, and 237 (78.7%) had never used mesh. Of 29 respondents currently using mesh, 12 (41.4%) used it only in selected patients; the majority used a sublay technique (20 [69.0%]) and biologic mesh (17 [58.6%]). Most respondents agreed that parastomal hernias are common and negatively affect quality of life; however, there remained concerns about evidence quality and the perceived risk associated with mesh among those who had never or had previously used mesh.
Conclusion: Prophylactic mesh placement remains relatively uncommon; when used, biologic mesh was the most common type. Many surgeons were not convinced of the safety or efficacy of prophylactic mesh placement.
Parastomal hernias are a predictable consequence of the fascial defect created for an ostomy and represent a major source of morbidity for patients with stomas. 1,2 The incidence of parastomal hernia appears to be highest following end colostomy creation, and although reported rates vary, rates up to 57% are cited for clinically detectable hernias and up to 78% for radiologically detectable hernias.1,3,4 Parastomal hernias can cause pain and reduced quality of life, affect body image and result in difficulties with application of the stoma appliance, which, in turn, results in leakage, skin excoriation and increased cost.1,5 Parastomal hernia repair can be a difficult operation with a high rate of failure, even with newer mesh-based techniques. 6–9 Surgical repair of these hernias is often delayed until symptoms become debilitating or the patient presents with an acute indication such as obstruction, incarceration or strangulation necessitating urgent surgical intervention.
We identified 10 randomized controlled trials (RCTs) conducted between 2009 and 2015 investigating the efficacy of prophylactic mesh insertion at the time of the index stoma creation for prevention of parastomal hernias.10–20 In the most comprehensive current meta-analysis (2017), Cross and colleagues21 synthesized data from 649 patients across all 10 RCTs and found that prophylactic mesh insertion reduced the rate of parastomal hernia formation from 36.6% to 16.4% (odds ratio 0.24, 95% confidence interval 0.12–0.50). Since this meta-analysis, the STOMAMESH trial was published and did not show the previously seen efficacy of mesh prophylaxis.22 High rates of parastomal hernia, detected both clinically and on computed tomography, were noted in both the intervention group and the control group, with 1-year rates of radiologically detected parastomal hernia of 34% without mesh placement and 32% with mesh placement. An analysis of follow-up data at 36 months is planned.
A small online study of 70 surgeons in Switzerland in 2012 cited fear of mesh-related infection as the most common reason that surgeons did not use mesh.23 However, none of the RCTs showed an increased risk of complications with mesh insertion.10–22 Rates of stoma-related complications were low across all RCTs, and there was no difference in rates of stoma-related complications, such as parastomal infection, stoma necrosis or stenosis, between mesh and control groups on meta-analysis.21
The present study aimed to evaluate the current opinions and practice patterns of Canadian and US colorectal surgeons with regard to the use of prophylactic mesh in end colostomy and to identify areas of clinical concerns with the current evidence base.
Methods
Study population
Between May and July 2017, we conducted a cross-sectional survey of North American colorectal surgeons. We identified Canadian colorectal surgeons through membership in the Canadian Society of Colon and Rectal Surgeons and the American Society of Colon and Rectal Surgeons, and a manual search of the faculty pages of all Canadian academic medical institutions. We excluded those without valid email addresses and those who were not practising surgery (non-surgeons, retired/deceased surgeons). For US colorectal surgeons, we surveyed a random selection of surgeons identified through membership in the American Society of Colon and Rectal Surgeons. We calculated our sample size based on the suggested sample size for a 5-point Likert scale, specifically with a coefficient of variation of population, C, of 0.5 and a pairwise correlation coefficient, p, of 0.5, and assumed a 40% response rate.24 Surgeons with an invalid email address and those not actively practising were excluded after the individualized invitation was sent and were replaced with additional randomly selected American Society of Colon and Rectal Surgeons members. Because both the response rate and the use of prophylactic mesh were lower than expected, we conducted a second round of surveys with a further random selection of US surgeons to increase our sample size of completed responses.
Questionnaire development
Questionnaire development followed standard methods for survey-based research.25–27 Two frameworks for barriers assessment and a previous survey guided initial item generation. 23,27–31 Items were generated within the domains of knowledge, attitudes, behaviours, patient characteristics, innovation characteristics, context characteristics and current evidence. We added items until sampling redundancy was achieved within each domain, and then reduced them to the smallest number possible without important omissions. Response formats included a 5-point Likert scale and an open-ended format. Pilot testing of the survey was conducted by the investigators and a small sample of physician reviewers (colorectal surgeons, senior residents interested in colorectal surgery and colorectal fellows at the University of Toronto) to assess clarity and comprehensibility. Limited sensibility testing was conducted by an expert in the colorectal field and an expert in knowledge translation to ensure the accuracy and pertinence of the questionnaire. The final questionnaire is presented in Appendix 1 (available at canjsurg.ca/019018-a1).
Survey administration
We administered the questionnaire using SurveyMonkey, a secure internet-based commercial service. An invitation to participate preceded the survey and was distributed by email with an individualized link. If there was no response, this was followed by 2 further requests for participation, sent a week apart. Entry into a prize draw was offered to all participants as an incentive.
Data analysis
Responses were anonymized through SurveyMonkey. We calculated the response rate as the number of completed questionnaires divided by the number of invited participants in each respondent group, including incomplete questionnaires. We categorized respondents into 3 groups based on self-reported use of mesh: 1) those who had never used mesh, 2) those who were currently using mesh and 3) those who had previously used mesh but no longer did so. We compared the response distribution of the Likert score for each item between the 3 groups using the Kruskal–Wallis test adjusted by the Benjamini–Hochberg method for multiple comparisons. We used the Dunn test to determine which of the groups were significantly different. We compacted Dunn analysis results into letter display format (a, b and c); groups sharing the same letter were not significantly different. We analyzed the quantitative data using R, version 3.3.3 (R Foundation for Statistical Computing). We collapsed the Likert responses into 3 categories; strongly agree/agree, neutral and disagree/strongly disagree. Answers to open-ended questions were reviewed and recurring factors identified. These factors were grouped and are presented in 4 domains: evidence, risk–benefit ratio, technical factors and professional factors. Respondents were also asked to identify any tools or information that have helped or would be helpful in deciding whether to use mesh.
Results
Of the 93 Canadian surgeons contacted, 79 could be verified to have received and opened the email, of whom 48 (60.8%) responded. A total of 1521 US surgeons were contacted, 585 in the first round and 936 in the second round. Of the 1521, 760 could be verified to have opened the email, of whom 253 (33.3%) responded. The overall response rate for all North American surgeons was 18.6% (301/1614). The overall response rate was higher for Canadian surgeons (48/93 [51.6%]) than for US surgeons (253/1521 [16.6%]).
Current surgical practices
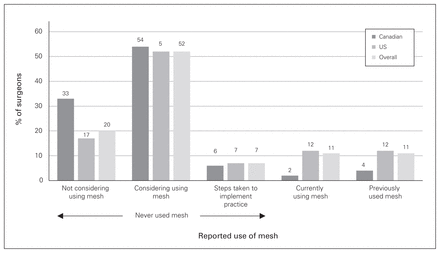
Of the 301 respondents, 32 (10.6%) reported that they currently used prophylactic mesh, 237 (78.7%) had never used mesh, and 32 (10.6%) had used mesh in the past but no longer did so (Fig. 1). Of the respondents who had never used mesh, 178 (75.1%) were considering its use; 21 (8.9%) had actively taken steps to implement the practice in the previous year. Among Canadian respondents, only 1 surgeon (2.1%) was using prophylactic mesh, and 2 surgeons (4.2%) had used it in the past. The practice was more common among US respondents: 31 (12.2%) reported they were currently using mesh, and 30 (11.9%) reported that they had used it in the past. Similar proportions of Canadian (26 [54.2%]) and US (131 [51.8%]) surgeons were considering the use of mesh.
Use of prophylactic mesh in end colostomy by North American surgeons.
The clinical practice characteristics of the 301 respondents by mesh use are presented in Table 1. The respondents performed a median of 13 (interquartile range 9–20) colostomy procedures a year. More than half (169 [56.1%]) estimated that parastomal hernias will develop in 40% or more of patients undergoing end colostomy within 5 years of surgery. Most surgeons who reported currently using mesh (24 [75.0%]) indicated that they knew at least 1 other surgeon who also did so, whereas few surgeons who had never used mesh (22 [9.3%]) did. Most surgeons currently using mesh (22/29 [75.9%]) did not use it in all patients (Table 2). More than half (17/29 [58.6%]) used a biologic product, and most (20/29 [69.0%]) used a sublay technique, with the remaining 9 (31.0%) using an underlay or intraperitoneal approach (Table 2).
General characteristics of respondents’ clinical practice
Clinical practice patterns regarding the use of prophylactic mesh
Surgeons who had previously used prophylactic mesh in end colostomy but no longer did so were asked to comment on why they had stopped. The most common factors identified were insufficient benefit (12 [37.5%]) and lack of appropriate resources (7 [21.9%]). Four respondents (12.5%) had personal experience with bad outcomes.
Factors affecting adoption of prophylactic mesh into clinical practice
Table 3 displays the results of Likert scale questions and Table 4 the results of open-ended questions regarding factors affecting the adoption of prophylactic mesh into practice. Regarding the evidence base for prophylactic mesh, most surgeons reported awareness of current literature on the use of prophylactic mesh; however, opinions differed with respect to the quality of the evidence. Most (20/29 [69.0%]) of those currently using mesh agreed there was high-quality evidence to support the efficacy of prophylactic mesh, compared to 101/223 (45.3%) of those who had never used mesh and 5/28 (17.8%) of those who previously had used mesh (p < 0.01) (Table 3). On open-ended questioning, surgeons not currently using mesh (both those who had never used mesh and those who had previously used it) cited concern with the quality and nature of the current evidence as a major barrier to the use of prophylactic mesh in end colostomy. Further evidence was the factor most commonly identified by both groups as potentially helpful in implementing the use of prophylactic mesh during end colostomy creation in the future (Table 4). Almost half (117/251 [46.6%]) of surgeons not currently using prophylactic mesh had reservations about the available research as it may have been unduly influenced by industry factors (Table 3).
Factors identified by respondents as affecting the adoption of prophylactic mesh into practice, by mesh use
Factors identified by respondents on open-ended questions as affecting the adoption of prophylactic mesh into practice
When considering the risk–benefit ratio of prophylactic mesh, most respondents agreed that parastomal hernias have a negative effect on a patient’s quality of life, and almost all believed that they are problematic enough to justify a prophylactic measure. However, there was disagreement on the risk associated with prophylactic mesh: more surgeons not currently using mesh than those currently using mesh agreed that prophylactic mesh increases the risk of short-term (96/251 [38.2%] v. 4/29 [13.8%]) and long-term (84/251 [33.5%] v. 1/29 [3.4%]) complications (p < 0.01 for both) (Table 3). On open-ended questioning, concern regarding the risk of mesh placement was the most common barrier to the use of mesh in end colostomy identified by surgeons who had never used mesh (57/164 [34.8%]) and those who had previously used mesh (5/25 [20.0%]).
Technical factors were not identified as a major barrier in most respondents’ decision-making (Table 3). Some respondents who had previously used prophylactic mesh (4/25 [16.0%]) noted that lack of appropriate resources, specifically difficulty obtaining an appropriate mesh or discontinuation of previously used mesh product, was a factor in their decision to stop using mesh (Table 4). Some surgeons who had never used mesh reported that educational tools (16/109 [14.7%]) and technical experience (15/109 [13.8%]) in how to place the mesh would be helpful in implementing the practice (Table 4).
Most respondents disagreed that professional factors played a major role in their decision-making. Most disagreed that there were substantial institutional barriers, and only a minority were concerned with professional consequences if there was a complication. The perceived need for clinical guidelines varied. Surgeons who had never used mesh were most strongly in favour of guidelines as a prerequisite to implementation (131/223 [58.7%]), while those currently using mesh disagreed that guidelines are necessary (24/29 [82.8%]) (p < 0.01) (Table 3). The lack of clinical guidelines supporting the use of prophylactic mesh was the second most commonly cited barrier on open-ended questioning among surgeons who had never used mesh (35/164 [21.3%]) (Table 4).
Discussion
The use of prophylactic mesh to prevent parastomal hernia was uncommon among the North American colorectal surgeons surveyed, and in Canada only a single surgeon was using prophylactic mesh. However, there was a high level of interest among those surveyed, with the majority considering adopting the practice in the future. This high level of interest and low level of adoption, along with a marked difference in interpretation of the current evidence, suggest that the reluctance of clinicians to adopt the practice may reflect not a failure of dissemination of current research but, rather, ongoing concern among clinicians regarding the safety, efficacy and technical details of the practice. Of the surgeons currently using mesh, just over half reported using biologic mesh. Notably, neither of the 2 RCTs in which biologic mesh was used showed a statistically significant reduction in parastomal hernia rates with mesh use.10,17 Our results do not identify any general characteristic of a current clinical practice that appears to be related to a surgeon’s decision to use prophylactic mesh, apart from potential use by colleagues at his or her institution.
Although most of our respondents agreed that parastomal hernias have a negative impact on a patient’s quality of life, there was disagreement as to whether that impact justified the theoretical risk of mesh. Surgeons who were not currently using mesh or who previously used mesh remained concerned with the risk of mesh placement, both in the short and the long term, despite a lack of evidence of increased risk in current clinical studies. Among surgeons not using mesh and those who had used it previously, the risk of mesh use was the most common factor cited when asked about the major barrier to prophylactic mesh use. Given that these surgeons were also less likely to strongly agree with the negative impact of parastomal hernias on patients’ quality of life and more likely to disagree with the efficacy of mesh placement, their risk–benefit analysis would likely be weighted away from mesh.
To our knowledge, there have been 11 RCTs investigating the efficacy of prophylactic mesh for parastomal hernia prevention,10–20,22 representing a larger body of evidence than is available for most surgical practices. Yet, surgeons may have a higher threshold for the adoption of this practice given the perception of risk owing to first- or second-hand experiences with mesh complications. Furthermore, surgeons not using mesh remained concerned with the influence of industry on the current evidence. Although cost was not commonly identified as a barrier, the cost of a polypropylene mesh, used in the majority of studies, would be much less substantial than that of the biologic counterparts. The applicability of current data to a North American population may also be a point of contention given that the majority of the RCTs were conducted in European populations. A review of the current evidence by a national organization, along with guidelines, would address the concerns of a minority of surgeons not currently using mesh; however, this was not a major barrier for the majority of our respondents.
Limitations
Our low response rate represents a potential source of bias common to many studies that rely on voluntary response to surveys. Survey respondents were more likely to have stronger opinions with regard to the use of prophylactic mesh than the general colorectal surgeon population. As a result, surgeons using prophylactic mesh and those who had used it previously may be overrepresented. Colorectal surgeons less familiar with the current evidence may have been less likely to respond. Because of this, it is unlikely that our findings underestimate the use of prophylactic mesh for parastomal hernia prevention in North America, although we may have overestimated the use of mesh by US surgeons.
Conclusion
The use of prophylactic mesh to prevent parastomal hernias remains a relatively uncommon practice among North American surgeons despite interest in the practice. Persistent concerns about the efficacy and long-term safety of prophylactic mesh will need to be addressed before this practice gains more widespread acceptance.
Footnotes
This abstract was presented at the American Society of Colon and Rectal Surgeons annual scientific meeting, May 19–23, 2018, Nashville, Tenn.
Funding: This research was funded through a General Surgery Resident Research Initiation Grant (GSSRIG-035) and a Medical Student Research Initiation Grant (MSRIG-020) from the American Society of Colon and Rectal Surgeons, as well as a Knowledge to Action Grant from the Canadian Cancer Society (grant 705597) and the Canadian Institutes of Health Research Institute for Cancer Research (grant 155428).
Competing interests: None declared.
Contributors: J. Holland, T. Chesney, F. Dossa, S. Acuna and N. Baxter designed the study. J. Holland acquired the data, which all authors analyzed. J. Holland wrote the article, which all authors reviewed and approved for publication.
- Accepted March 5, 2019.