Abstract
Acute lung injury is marked by damage to alveolar-capillary barrier. High pulmonary levels of matrix-degrading serine proteinase trypsin and matrix metalloproteinases (MMP)-2, -8, and -9 have been shown in preterm infants with respiratory distress syndrome (RDS). We studied expression of trypsin and MMP-2, -8, and -9 in rats exposed to >95% oxygen for 24, 48, or 60 h. As demonstrated by zymography and Western immunoblotting, levels of trypsin and MMP-2, -8, and -9 in bronchoalveolar lavage fluid (BALF) sharply increased after 48 h of hyperoxia relative to normoxia controls. This coincided with increase in alveolar-capillary permeability, as indicated by increased protein concentration in BALF. Both neutrophil-derived 80-kD and mesenchymal cell–derived 60-kD MMP-8 isoforms were detected in BALF. Of them, mesenchymal-type MMP-8 predominated. In immunohistochemistry, alveolar epithelium showed strong trypsin expression at 48 and 60 h of hyperoxia, whereas it was predominantly negative in controls. MMP-8 was mostly expressed in macrophages. Marked up-regulation of trypsin and MMP-8 early during hyperoxic lung injury suggests that these enzymes play a role in the pathogenesis of acute lung injury and may therefore be potential targets for therapy of lung injury.
Similar content being viewed by others
Main
The extracellular matrix (ECM) between epithelial and capillary endothelial layers and in particular the basement membranes (BM) of the cell layers are essential in the maintenance of the structural and functional integrity of the alveolar wall (1). Trypsin is a serine proteinase that can efficiently degrade various ECM proteins; at very low concentrations, it is capable of activating proforms of several MMPs, thus having potential to initiate a broad-spectrum proteinase cascade eventually leading to tissue destruction (2,3). Multiple isoforms of trypsin have been demonstrated in human pancreas and in most animal species (4,5). Trypsinogen-1 and -2 were detected for the first time outside the gastrointestinal tract in cyst fluid of human ovarian tumors (6). Later, trypsinogens have been identified in a variety of human extrapancreatic tissues including normal human epithelial cells of the lung, vascular endothelial cells, and various cancers (4,7,8). Recently, ectopic trypsin was identified in rat lung (9).
In the lung, trypsin may induce tissue injury not only through initiating matrix-degrading proteolytic cascade, but also through proinflammatory actions. Trypsin is a potent activator of proteinase-activated receptor 2 (PAR2), a G protein–coupled receptor that is believed to play an important role in airway inflammation (10,11). In preterm infants, high pulmonary trypsinogen-2 early postnatally is associated with the severity of acute lung injury and with the development of bronchopulmonary dysplasia (BPD) (8). Furthermore, in autopsy specimens from preterm infants who died of respiratory distress syndrome (RDS) or BPD, trypsin-2 colocalizes with PAR2 in alveolar and bronchial epithelium (12).
MMPs are a family of zinc-dependent, genetically distinct but structurally related endopeptidases collectively capable of degrading almost all components of ECM. MMP-2 and MMP-9 are type IV collagenases that can disrupt alveolar BM (13). MMP-8 belongs to the collagenase subfamily of MMPs and cleaves collagen types I–III, of which I and III are the major structural components of the pulmonary interstitial ECM. Furthermore, MMP-8 can act on various nonmatrix proteins such as serine proteinase inhibitors (serpins) and chemokines and thus may modulate inflammatory processes in different ways (14,15). Increased levels of MMP-2, MMP-8, and MMP-9 are associated with inflammatory lung diseases such as RDS, BPD, and asthma (13,16–18).
Hyperoxia-induced lung injury (exposure to >95% oxygen), a well-established model of acute lung injury, is characterized by damage to the alveolar-capillary barrier with subsequent increased pulmonary vascular permeability, progressive inflammation, and pulmonary edema (19). In rats exposed to 100% oxygen, the first signs of increased alveolar-capillary permeability are detected at 48 h (20). Severe interstitial and alveolar edema is present at 60 h, leading to death usually within 72 h of exposure (19,20).
Association of high pulmonary levels of trypsin, MMP-2, -8, and -9 with tissue-destructive lung diseases suggests that these proteinases may play an important role in the pathogenesis of lung injury. By use of an experimental animal model, we wanted to determine the cellular localization and chronological increase of these proteinases during development of acute lung injury. Therefore, we characterized trypsin, MMP-2, -8, and -9 in lungs of rats exposed to >95% oxygen for 24, 48, and 60 h.
METHODS
Experimental model.
The study protocol was approved by the Institutional Review Board for Animal Studies of Helsinki University Central Hospital, Helsinki, Finland. Female Wistar rats (Harlan Nederland, Horst, The Netherlands) aged 8 wk were housed for 1 wk before use. The animals were placed in a sealed Plexiglas chamber (85 × 60 × 40 cm) and exposed to >95% O2 for 24 h (n = 6), 48 h (n = 6), and 60 h (n = 6) by administration of pure oxygen at 5 L/min. O2 concentration was monitored with an oximeter (Datex, Helsinki, Finland). Food and water were allowed ad libitum and a 12-/12-h light/dark cycle was maintained. Control animals (n = 6) were kept in room air. At different exposure times, animals were anesthetized by intraperitoneal injections of ketamine (50 mg/kg) and xylazine (10 mg/kg) and killed by cervical dislocation. Immediately after decapitation, the right lung was removed and cut into two pieces. The pieces were soaked in isotonic saline, snap frozen in liquid nitrogen, and stored at −80°C until determination of myeloperoxidase (MPO) activity. The left lung was removed, fixed in 10% paraformaldehyde for 24 h, embedded in paraffin, and stored at room temperature for subsequent immunohistochemistry.
Bronchoalveolar lavage (BAL).
In a parallel experiment, BAL was performed for normoxia controls (n = 8) and rats exposed to >95% O2 for 24 h (n = 8), 48 h (n = 8), and 60 h (n = 8). Immediately after killing the rat, the trachea was cannulated, and the lungs were lavaged by flushing with sterile isotonic saline (10 mL) as 10 aliquots of 1 mL each. BALF samples were kept on ice until centrifuged at 500 × g for 10 min at 4°C, and the supernatant was stored at −20°C for subsequent analyses. Protein concentration in BALF was measured (21) and used as an indicator of increased vascular permeability and loss of capillary endothelial membrane integrity.
Gelatin zymography.
For analysis of gelatinolytic activity by zymography, BALF samples were run on 1.5-mm thick 8%–10% sodium dodecylsulfate (SDS)–polyacrylamide gels impregnated with 1 mg/mL gelatin labeled fluorescently with 2-methoxy-2,4-diphenyl-3(2H)-furanone (Fluka, Sigma Chemical Co.–Aldrich, Buchs SG, Switzerland) as described previously (8). The intensities of gelatinolytic bands were evaluated with Bio-Rad Model GS-700 Imaging Densitometer using Quantity Program, new version of the Molecular Analyst/PC program (Bio-Rad Laboratories, Hercules, CA) (16). Results were expressed as arbitrary units (AU).
ECL Western blotting.
In BALF, molecular weight forms of trypsin and MMP-2, -8, and -9 were analyzed by ECL Western immunoblot method using specific antisera as described previously (16). Briefly, the BALF samples were separated on 10% SDS-polyacrylamide gels and transferred onto nitrocellulose membranes (Schleider & Schuell, Dassel, Germany). Nonspecific binding was blocked with 5% milk powder (Valio, Helsinki, Finland). The membranes were incubated with a 1:500 solution of polyclonal antibodies against human MMP-2 (2), MMP-8 (16), MMP-9 (2), and trypsin (1:500, Chemicon International, Temecula, CA) for 12 h at room temperature, and then with horseradish peroxidase–linked anti–rabbit antibody for 1 h. The proteins were detected by the ECL detection system according to the manufacturer's instructions (Amersham Pharmacia Biotech). The intensities of immunoreacted forms of MMP-8 were evaluated and expressed as arbitrary units as described above (16).
MPO activity.
MPO activity was measured as a marker of pulmonary neutrophil accumulation, as previously described (22). Briefly, lung samples were thawed and homogenized in phosphate-buffered saline (PBS). After centrifugation, the pellet was resuspended in 1 mL of 50 mmol/L potassium phosphate containing 0.5 g/100 mL centrimonium bromide. Resuspended pellets were frozen at −70°C until the MPO assay was performed. Frozen samples were thawed, sonicated for 90 s, incubated in a 60°C water bath for 2 h. After centrifugation, 33 μL of supernatant was combined with 957 μL of 50 mmol/L potassium phosphate buffer, pH 6.0, containing 0.167 mg/mL o-dianisidine dihydrochloride and 5 × 10−4 M hydrogen peroxide. Change in absorbance was measured in a Lambda Bio UV/VIS Spectrometer (Perkin Elmer, Boston, MA) at 460 nm absorbance. MPO activity was expressed as mU/mg protein. Protein concentration was quantified by the method of Bradford (21).
Immunohistochemistry.
In lung tissue, trypsin immunoreactivity was visualized with monoclonal anti–trypsin antibody, MAB 1482 (Chemicon International), and MMP-8 immunoreactivity with rabbit polyclonal antibody against human MMP-8 (23). Four-micrometer sections were deparaffinized and rehydrated. To enhance antigen retrieval, sections were pretreated with microwave heat. The sections were then treated with 0.5% hydrogen peroxide in methanol for 30 min and blocked with either normal horse serum (trypsin) or normal goat serum (MMP-8) (both 1:20) for 15 min. Primary antibody to trypsin (diluted 1:1000) or to MMP-8 (diluted 1:250) was added, and the sections were incubated overnight at room temperature. Bound antibody was visualized by the avidin-biotin complex immunoperoxidase technique (ABC) (Elite ABC Kit, Vectastain, Vector Laboratories, Burlingame, CA) following the manufacturer's instructions. The sections were incubated with the biotinylated second layer antibody and the peroxidase-labeled avidin-biotin complex for 30 min each. Peroxidase activity was developed with 3-amino-9-ethyl-carbazole (A-5754, Sigma Chemical Co.), and finally the sections were stained with hematoxylin. Sections that were treated with PBS served as negative controls. Rat pancreatic and skin specimens were used as positive controls for trypsin and MMP-8 immunohistochemistry (24).
The immunoreactivities of trypsin and MMP-8 were analyzed independently by two investigators (K.S. and K.C.) in a blinded fashion. In each case, the entire section of lung tissue (approximately 1 cm2) was evaluated. The level of trypsin immunoreactivity was scored in a semiquantitative manner according to the following method: absent = 0, low = 1, moderate = 2, or strong = 3. Separate scores were given for bronchial and bronchiolar epithelium, alveolar epithelium, and vascular smooth muscle.
Statistical analysis.
Data are expressed as box and whisker plots, representing median, interquartile range, and 10th and 90th percentiles. Comparisons between controls and hyperoxia groups were performed with the nonparametric multiple comparison Kruskal-Wallis test (StatView 5.0.1, Abacus Concepts Inc., Berkeley, CA). The Dunn's test was used for the post hoc comparisons. p Values <0.05 were considered statistically significant.
RESULTS
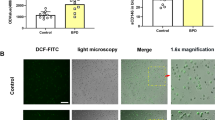
No evident signs of respiratory distress or macroanatomic changes could be detected up to 48 h of exposure to >95% O2. At 60 h, pleural effusions were found on opening the thoracic cavity and the lungs looked hemorrhagic and consolidated. Protein concentration in BALF was stable until 48 h, when it was significantly increased, and after 60 h of exposure a 10-fold increase was detected as compared with controls (Fig. 1A). Increased MPO activity in lung tissue was first observed at 48 h, and the MPO activity further increased by 60 h (Fig. 1B).
Protein concentration in BALF samples (n = 8 per group) (A) and MPO activity in lung homogenates (n = 6 per group) (B) from controls and rats exposed to >95% oxygen for 24, 48, and 60 h. Data shown as box and whisker plots, representing median, interquartile range, and 10th and 90th percentiles. *p < 0.05; **p < 0.0005 vs controls.
Characterization of trypsin and MMPs in BALF.
In gelatin zymograms, three gelatinolytic proteinases of molecular weights 28, 68, and 90 kD were clearly detected at 48 h of exposure, and the gelatinolytic activity was further increased at 60 h (Fig. 2A). In contrast, very faint gelatinolytic activity was detected in BALF samples from controls or rats exposed to 24 h of hyperoxia (Fig. 2A). By ECL Western blotting, the 28-kD species was identified as trypsin (Fig. 2B), and the 68- and 90-kD species as proenzyme forms of MMP-2 and -9, respectively (data not shown). At 48 and 60 h of exposure, Western blot analysis of BALF samples with anti-MMP-8 revealed the presence of both neutrophil-derived 80-kD MMP-8 and 60-kD mesenchymal cell–derived MMP-8 species, of which the 60-kD mesenchymal cell–derived MMP-8 species predominated. No MMP-8 immunoreactivity could be demonstrated in controls or in rats exposed to 24 h of hyperoxia (Fig. 2C). Densitometric analysis demonstrated that BALF levels of trypsin and MMP-2 were significantly increased by 48 h of hyperoxia (Fig. 3A,B). At 60 h, the levels of these enzymes were further increased, and a significant increase was also detected in levels of MMP-9 (Fig. 3), as well as in levels of both neutrophil-derived and mesenchymal cell–derived MMP-8 (Fig. 4).
BALF samples from controls and rats exposed to >95% oxygen for 24, 48, and 60 h. Gelatin zymogram (A); ECL Western immunoblotting for trypsin (B). Lane 1: BALF sample from rat exposed to hyperoxia for 60 h, lane 2: rat pancreatic trypsin, lane 3: human tumor-associated trypsin-2. Arrowheads indicate 28 kD trypsin. ECL Western immunoblotting for MMP-8 (C). Both neutrophil-derived (PMN) and mesenchymal cell-derived (mes) isoforms of MMP-8 are detected. Positions of molecular weight standards indicated by kD.
Levels of trypsin (A), MMP-2 (B), and MMP-9 (C) in BALF from controls and rats exposed to >95% oxygen for 24, 48, and 60 h as evaluated by densitometric analysis of gelatinolytic bands. Data shown as in Fig. 1. AU, arbitrary unit; *p < 0.01; **p < 0.0005 vs controls.
Levels of neutrophil-derived latent MMP-8 (A) and mesenchymal cell–derived latent MMP-8 (B) in BALF from controls and rats exposed to >95% oxygen for 24, 48, and 60 h. Evaluated by densitometric analysis of immunoreactive bands in Western immunoblots. Data shown as in Fig. 1. AU, arbitrary unit; *p < 0.0005 vs controls.
Trypsin immunohistochemistry.
In normoxia controls, low trypsin immunoreactivity was detected in bronchial and bronchiolar epithelial cells, whereas alveolar epithelium was predominantly negative (Fig. 5A). After 24 h of hyperoxia, there was a tendency for increased trypsin immunoreactivity in bronchial and bronchiolar epithelium when compared with controls (Figs. 5B and 6B). At 48 and 60 h, immunohistochemistry revealed moderate to strong expression of trypsin in alveolar epithelium, whereas in bronchial and bronchiolar epithelium, the trypsin level remained low (Fig. 5C and D). When compared with controls, semiquantitative scoring showed a significant increase in the level of trypsin immunoreactivity in alveolar epithelium of rats exposed to 48 and 60 h of hyperoxia (p < 0.05 and p < 0.005, respectively) (Fig. 6A). In four of the six rats exposed to 48 or 60 h of hyperoxia, moderate or strong trypsin immunoreactivity could be detected in vascular smooth muscle of large arteries, whereas smooth muscle of smaller arteries was negative. In addition, trypsin immunoreactivity was detected in hyaline membranes and occasionally in intra-alveolar macrophages.
Immunohistochemical localization of trypsin in hyperoxia-injured and control rat lung. In controls (A) and rats exposed to >95% oxygen for 24 h (B), low trypsin immunoreactivity is observed in bronchial epithelium, whereas alveolar epithelium is predominantly negative. After exposure to >95% oxygen for 48 h (C) and 60 h (D), strong trypsin immunoreactivity is detected in alveolar epithelium, whereas immunoreactivity in bronchial epithelium remains low. br, bronchiole; v, blood vessel. Scale bars = 100 μm.
Box plot of semiquantitative analysis of trypsin immunoreactivity in alveolar (A) and bronchial (B) epithelium in normoxia controls and rats exposed to >95% oxygen for 24, 48, and 60 h (n = 6 per group). Semiquantitative scoring of trypsin immunoreactivity was assessed as follows: absent = 0, low = 1, moderate = 2, or strong = 3. Data shown as in Fig. 1. *p < 0.05; **p < 0.005 vs controls.
MMP-8 immunohistochemistry.
Almost no immunoreactivity for MMP-8 could be demonstrated until 48 h of hyperoxia, when positive cells with a large cytoplasm obviously representing recruited macrophages could be detected in edematic perivascular space (Fig. 7A–C). At 60 h, a large number of macrophages strongly positive for MMP-8 were detected in alveoli as well as in interstitium (Fig. 7D and E). Although MMP-8 was predominantly localized in macrophages, at 48 h, positive immunostaining was also found in intravascular and perivascular neutrophils and, in addition, at 60 h in neutrophils located in the interstitium and intra-alveolar space (Fig. 7F).
Immunohistochemical localization of MMP-8 in hyperoxia-injured and control rat lung. Lung samples from control (A) and rat exposed to >95% oxygen for 24 h (B) show no MMP-8 immunoreactivity. In rats exposed to >95% oxygen for 48 h(C) and 60 h (D), marked MMP-8 immunoreactivity is detected in recruited macrophages (arrows) and neutrophils (arrowheads). (E) Positive intra-alveolar macrophage; (F) positive intravascular neutrophils. br, bronchiole; v, blood vessel. Scale bars: A–D = 100 μm; E and F = 10 μm.
DISCUSSION
Acute lung injury is marked by destruction of the alveolar-capillary barrier. We show a striking increase in the pulmonary expression of the potent matrix-degrading serine proteinase trypsin during the development of hyperoxic lung injury in rat. After 48 h of exposure to >95% oxygen, immunohistochemical analysis demonstrated strong expression of trypsin in alveolar epithelium, which, in contrast, showed almost no immunoreactivity for trypsin under normoxic conditions.
Trypsin can directly attack various important structural components of the pulmonary ECM such as native collagen types I and IV (3,25), of which collagen IV is the major component of the alveolar-capillary BM. In addition to trypsin, zymography of BALF samples from rats exposed to 48 and 60 h of hyperoxia demonstrated the up-regulation of two other gelatinolytic enzymes that were identified as MMP-2 and -9. Similarly to trypsin, MMP-2, and MMP-9 can efficiently degrade BM structures (2,13). The marked up-regulation of trypsin, MMP-2, and MMP-9 in BALF coincided with an increase in the alveolar-capillary permeability, as indicated by increased protein concentration in BALF, suggesting that they may play a role in the degradation of alveolar-capillary BM associated with the development of hyperoxic lung injury. In accordance with our results, an earlier study showed increased expression of pulmonary MMP-2 and -9 in rats exposed to 100% oxygen for 60 h (26). The expression of MMP-2 was localized in interstitial cells and MMP-9 in intra-alveolar macrophages (26). In our study, the markedly increased expression of trypsin in alveolar epithelium corroborates an important role for alveolar epithelium in the pathogenesis of oxidant injury leading to increased permeability and subsequent pulmonary edema (19,20).
Trypsin efficiently activates various pro-MMPs, including MMP-8 and -9, at very low concentrations by cleaving off the activation propeptide, which concomitantly results in diminished molecular weight of the target MMP (2,3). In this study, most of the MMP-2, -8, and -9 detected in BALF samples were in nonconverted proforms as demonstrated by Western immunoblotting. This is in line with the findings of our previous study, in which we characterized the presence and the molecular weight forms of MMP-2, -8, and -9 in tracheal aspirate fluid samples from preterm infants with RDS (16). It is noteworthy that some of the nonconverted forms may represent oxidatively activated forms of these MMPs in vivo since oxidative activation of MMP-8 or -9 does not necessarily involve changes in their molecular sizes (27,28).
Besides its capacity to degrade ECM and BM structures, trypsin can cause tissue damage by inducing inflammation (11,29,30). In a rat model of pancreatitis-associated lung injury, infusion of trypsin or trypsinogen causes an acute dose-dependent pulmonary injury characterized by perivascular edema and hemorrhage (29). This lung injury is neutrophil dependent and possibly mediated by the ability of trypsin to up-regulate pulmonary intercellular adhesion molecule-1, a key vascular endothelial adhesion molecule necessary for transport of leukocytes from intravascular space into inflamed tissues (30). The proinflammatory effects of trypsin may also be mediated through activation of PAR2, a G protein–coupled receptor that is believed to play an important role in inflammation (10,11). PAR2 is markedly up-regulated by inflammatory agents and widely expressed in lungs (11). Activation of PAR2 increases lung vascular and epithelial permeability to protein and causes pulmonary edema in a dose-dependent manner (10). In preterm infants with RDS, trypsin-2 colocalizes with PAR2 in airway epithelium (12).
However, increased trypsin in alveolar epithelium may also play a protective role in the development of lung injury. In the injured lung, active transepithelial transport of Na+ limits alveolar edema (31). Trypsin increases ion transport across rat alveolar type II cells and paracellular resistance, indicating that it may play an important role in the clearance of alveolar fluid (32). In fluid-filled lungs in a rat model, inhibition of trypsin by intratracheal soyabean trypsin inhibitor or α1-antitrypsin decreases amiloride-sensitive lung fluid clearance, and the effect is partially restored by instillation of trypsin (32).
In control rats, we detected low trypsin expression in bronchial epithelium. This is in accordance with earlier studies showing expression of trypsin in bronchial epithelium of human adults and of term newborn infants without pulmonary pathology and supports the hypothesis that trypsin also participates in normal cellular functions in the lung (7,8).
We observed a marked up-regulation of MMP-8 after 48 of exposure to hyperoxia. MMP-8 (collagenase-2) was previously regarded solely as a neutrophil-specific MMP that is stored in granules and released on degranulation (33). However, certain activated mesenchymal cells and macrophages also express MMP-8 (18,23). In our study, immunoblotting of BALF samples demonstrated the presence of both neutrophil-derived 80-kD MMP-8 and 60-kD mesenchymal cell–derived MMP-8 species, of which the mesenchymal cell–derived MMP-8 species clearly predominated. Immunohistochemical analysis confirmed that in the hyperoxic lung, MMP-8 was mostly expressed in recruited macrophages, which at 48 h were detected in perivascular space and at 60 h in alveoli and interstitium. In inflammation, MMP-8 is believed to have a pivotal role in the degradation of collagen Type I. Recently, an unexpected anti-inflammatory role was evidenced for MMP-8 in the lung (15,34). One possible mechanism is the regulation of inflammatory cell apoptosis, as demonstrated by reduced neutrophil apoptosis in MMP-8−/− mice during allergen-induced lung inflammation (34). During the development of hyperoxic lung injury, a large number of infiltrating inflammatory cells is found in the rat lung (35). Whether the role of MMP-8 in hyperoxic lung injury is anti-inflammatory possibly by regulating inflammatory cell apoptosis remains a subject for future research.
In summary, in a rat model of hyperoxic lung injury, we have demonstrated a striking increase in pulmonary expression of the potent matrix-degrading serine proteinase trypsin after 48 h of hyperoxia. Trypsin was localized in alveolar epithelium, which in controls was predominantly negative. In line with trypsin, the expression of especially mesenchymal cell–derived MMP-8 was clearly increased during the course of hyperoxic lung injury and was localized in intra-alveolar and interstitial macrophages. Although we cannot directly draw a parallel from our results in the hyperoxic lung injury model to earlier findings in preterm infants with RDS, these results support the hypothesis that high pulmonary levels of trypsin and MMP-8 are injurious in the lung. Further exploration of the roles of trypsin and MMP-8 in acute lung injury may offer new targets for therapeutic intervention.
Abbreviations
- BALF:
-
bronchoalveolar lavage fluid
- BM:
-
basement membrane
- BPD:
-
bronchopulmonary dysplasia
- ECM:
-
extracellular matrix
- MMP:
-
matrix metalloproteinase
- MPO:
-
myeloperoxidase
- PAR2:
-
proteinase-activated receptor 2
- RDS:
-
respiratory distress syndrome
References
Maina JN, West JB 2005 Thin and strong¡ The bioengineering dilemma in the structural and functional design of the blood-gas barrier. Physiol Rev 85: 811–844
Sorsa T, Salo T, Koivunen E, Tyynelä J, Konttinen YT, Bergmann U, Tuuttila A, Niemi E, Teronen O, Heikkilä P, Tschesche H, Leinonen J, Osman S, Stenman UH 1997 Activation of type IV procollagenases by human tumor-associated trypsin-2. J Biol Chem 272: 21067–21074
Moilanen M, Sorsa T, Stenman M, Nyberg P, Lindy O, Vesterinen J, Paju A, Konttinen YT, Stenman UH, Salo T 2003 Tumor-associated trypsinogen-2 (trypsinogen-2) activates procollagenases (MMP-1, -8, -13) and stromelysin-1 (MMP-3) and degrades type I collagen. Biochemistry 42: 5414–5420
Paju A, Stenman UH 2006 Biochemistry and clinical role of trypsinogens and pancreatic secretory trypsin inhibitor. Crit Rev Clin Lab Sci 43: 103–142
Lutcke H, Rausch U, Vasiloudes P, Scheele GA, Kern HF 1989 A fourth trypsinogen (P23) in the rat pancreas induced by CCK. Nucleic Acids Res 17: 6736
Stenman UH, Koivunen E, Vuento M 1988 Characterization of a tumor-associated serine protease. Biol Chem Hoppe Seyler 369: 9–14
Cocks TM, Fong B, Chow JM, Anderson GP, Frauman AG, Goldie RG, Henry PJ, Carr MJ, Hamilton JR, Moffatt JD 1999 A protective role for protease-activated receptors in the airways. Nature 398: 156–160
Cederqvist K, Haglund C, Heikkilä P, Sorsa T, Tervahartiala T, Stenman UH, Andersson S 2003 Pulmonary trypsin-2 in the development of bronchopulmonary dysplasia in preterm infants. Pediatrics 112: 570–577
Towatari T, Ide M, Ohba K, Chiba Y, Murakami M, Shiota M, Kawachi M, Yamada H, Kido H 2002 Identification of ectopic anionic trypsin I in rat lungs potentiating pneumotropic virus infectivity and increased enzyme level after virus infection. Eur J Biochem 269: 2613–2621
Su X, Camerer E, Hamilton JR, Coughlin SR, Matthay MA 2005 Protease-activated receptor-2 activation induces acute lung inflammation by neuropeptide-dependent mechanisms. J Immunol 175: 2598–2605
Steinhoff M, Buddenkotte J, Shpacovitch V, Rattenholl A, Moormann C, Vergnolle N, Luger TA, Hollenberg MD 2005 Proteinase-activated receptors: transducers of proteinase-mediated signaling in inflammation and immune response. Endocr Rev 26: 1–43
Cederqvist K, Haglund C, Heikkilä P, Hollenberg MD, Karikoski R, Andersson S 2005 High expression of pulmonary proteinase-activated receptor 2 in acute and chronic lung injury in preterm infants. Pediatr Res 57: 831–836
Chakrabarti S, Patel KD 2005 Matrix metalloproteinase-2 (MMP-2) and MMP-9 in pulmonary pathology. Exp Lung Res 31: 599–621
Balbin M, Fueyo A, Tester AM, Pendas AM, Pitiot AS, Astudillo A, Overall CM, Shapiro SD, Lopez-Otin C 2003 Loss of collagenase-2 confers increased skin tumor susceptibility to male mice. Nat Genet 35: 252–257
Owen CA, Hu Z, Lopez-Otin C, Shapiro SD 2004 Membrane-bound matrix metalloproteinase-8 on activated polymorphonuclear cells is a potent, tissue inhibitor of metalloproteinase-resistant collagenase and serpinase. J Immunol 172: 7791–7803
Cederqvist K, Sorsa T, Tervahartiala T, Maisi P, Reunanen K, Lassus P, Andersson S 2001 Matrix metalloproteinases-2, -8, and -9 and TIMP-2 in tracheal aspirates from preterm infants with respiratory distress. Pediatrics 108: 686–692
Schock BC, Sweet DG, Ennis M, Warner JA, Young IS, Halliday HL 2001 Oxidative stress and increased type-IV collagenase levels in bronchoalveolar lavage fluid from newborn babies. Pediatr Res 50: 29–33
Prikk K, Maisi P, Pirilä E, Reintam MA, Salo T, Sorsa T, Sepper R 2002 Airway obstruction correlates with collagenase-2 (MMP-8) expression and activation in bronchial asthma. Lab Invest 82: 1535–1545
Crapo JD, Barry BE, Foscue HA, Shelburne J 1980 Structural and biochemical changes in rat lungs occurring during exposures to lethal and adaptive doses of oxygen. Am Rev Respir Dis 122: 123–143
Royston BD, Webster NR, Nunn JF 1990 Time course of changes in lung permeability and edema in the rat exposed to 100% oxygen. J Appl Physiol 69: 1532–1537
Bradford MM 1976 A rapid and sensitive method for the quantitation of microgram quantities of protein utilizing the principle of protein-dye binding. Anal Biochem 72: 248–254
Kinsella JP, Parker TA, Galan H, Sheridan BC, Halbower AC, Abman SH 1997 Effects of inhaled nitric oxide on pulmonary edema and lung neutrophil accumulation in severe experimental hyaline membrane disease. Pediatr Res 41: 457–463
Hanemaaijer R, Sorsa T, Konttinen YT, Ding Y, Sutinen M, Visser H, van Hinsbergh VW, Helaakoski T, Kainulainen T, Ronka H, Tschesche H, Salo T 1997 Matrix metalloproteinase-8 is expressed in rheumatoid synovial fibroblasts and endothelial cells. Regulation by tumor necrosis factor-alpha and doxycycline. J Biol Chem 272: 31504–31509
Pirilä E, Ramamurthy N, Maisi P, McClain S, Kucine A, Wahlgren J, Golub L, Salo T, Sorsa T 2001 Wound healing in ovariectomized rats: effects of chemically modified tetracycline (CMT-8) and estrogen on matrix metalloproteinases -8, -13 and type I collagen expression. Curr Med Chem 8: 281–294
Koshikawa N, Yasumitsu H, Umeda M, Miyazaki K 1992 Multiple secretion of matrix serine proteinases by human gastric carcinoma cell lines. Cancer Res 52: 5046–5053
Pardo A, Selman M, Ridge K, Barrios R, Sznajder JI 1996 Increased expression of gelatinases and collagenase in rat lungs exposed to 100% oxygen. Am J Respir Crit Care Med 154: 1067–1075
Saari H, Suomalainen K, Lindy O, Konttinen YT, Sorsa T 1990 Activation of latent human neutrophil collagenase by reactive oxygen species and serine proteases. Biochem Biophys Res Commun 171: 979–987
Westerlund U, Ingman T, Lukinmaa PL, Salo T, Kjeldsen L, Borregaard N, Tjaderhane L, Konttinen YT, Sorsa T 1996 Human neutrophil gelatinase and associated lipocalin in adult and localized juvenile periodontitis. J Dent Res 75: 1553–1563
Hartwig W, Werner J, Jimenez RE, Z'graggen K, Weimann J, Lewandrowski KB, Warshaw AL, Fernandez-del Castillo C 1999 Trypsin and activation of circulating trypsinogen contribute to pancreatitis-associated lung injury. Am J Physiol 277: G1008–G1016
Hartwig W, Werner J, Warshaw AL, Antoniu B, Castillo CF, Gebhard MM, Uhl W, Buchler MW 2004 Membrane-bound ICAM-1 is upregulated by trypsin and contributes to leukocyte migration in acute pancreatitis. Am J Physiol Gastrointest Liver Physiol 287: G1194–G1199
Yue G, Matalon S 1997 Mechanisms and sequelae of increased alveolar fluid clearance in hyperoxic rats. Am J Physiol 272: L407–L412
Swystun V, Chen L, Factor P, Siroky B, Bell PD, Matalon S 2005 Apical trypsin increases ion transport and resistance by a phospholipase C-dependent rise of Ca2+. Am J Physiol Lung Cell Mol Physiol 288: L820–L830
Weiss SJ 1989 Tissue destruction by neutrophils. N Engl J Med 320: 365–376
Gueders MM, Balbin M, Rocks N, Foidart JM, Gosset P, Louis R, Shapiro S, Lopez-Otin C, Noel A, Cataldo DD 2005 Matrix metalloproteinase-8 deficiency promotes granulocytic allergen-induced airway inflammation. J Immunol 175: 2589–2597
Barry BE, Crapo JD 1985 Patterns of accumulation of platelets and neutrophils in rat lungs during exposure to 100% and 85% oxygen. Am Rev Respir Dis 132: 548–555
Acknowledgements
We thank Marjatta Vallas, Päivi Peltokangas, and Elina Laitinen for excellent technical assistance.
Author information
Authors and Affiliations
Corresponding author
Additional information
This research was supported by grants from the Foundation for the Pediatric Research, Finska Läkeresällskapet, The Sigrid Jusélius Foundation, the Academy of Finland, and the Helsinki University Central Hospital Research Fund.
Rights and permissions
About this article
Cite this article
Cederqvist, K., Janer, J., Tervahartiala, T. et al. Up-Regulation of Trypsin and Mesenchymal MMP-8 During Development of Hyperoxic Lung Injury in the Rat. Pediatr Res 60, 395–400 (2006). https://doi.org/10.1203/01.pdr.0000238342.16081.f9
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1203/01.pdr.0000238342.16081.f9
This article is cited by
-
IL-1β is a key cytokine that induces trypsin upregulation in the influenza virus–cytokine–trypsin cycle
Archives of Virology (2017)
-
Gene expression profile in newborn rat lungs after two days of recovery of mechanical ventilation
Pediatric Research (2015)