Abstract
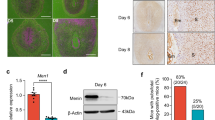
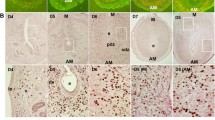
Decidual stromal cells differentiate from endometrial stromal fibroblasts (ESFs) under the influence of progesterone and cyclic adenosine monophosphate (cAMP) and are essential for implantation and the maintenance of pregnancy. They evolved in the stem lineage of placental (eutherian) mammals coincidental with the evolution of implantation. Here we use the well-established in vitro decidualization protocol to compare early (3 days) and late (8 days) gene transcription patterns in immortalized human ESF. We document extensive, dynamic changes in the early and late decidual cell transcriptomes. The data suggest the existence of an early signal transducer and activator of transcription (STAT) pathway dominated state and a later nuclear factor κB (NFKB) pathway regulated state. Transcription factor expression in both phases is characterized by putative or known progesterone receptor (PGR) target genes, suggesting that both phases are under progesterone control. Decidualization leads to proliferative quiescence, which is reversible by progesterone withdrawal after 3 days but to a lesser extent after 8 days of decidualization. In contrast, progesterone withdrawal induces cell death at comparable levels after short or long exposure to progestins and cAMP. We conclude that decidualization is characterized by a biphasic gene expression dynamic that likely corresponds to different phases in the establishment of the fetal—maternal interface.
Similar content being viewed by others
References
Gellersen B, Brosens JJ. Cyclic decidualization of the human endometrium in reproductive health and failure. Endocr Rev. 2014; er20141045. doi:https://doi.org/10.1210/er.2014-1045
Evans J, Salamonsen LA, Winship A, et al. Fertile ground: human endometrial programming and lessons in health and disease. Nat Rev Endocrinol. 2016;12(11):654–667. doi:https://doi.org/10.1038/nrendo.2016.116
Pavličev M, Wagner GP, Chavan AR, et al. Single-cell transcriptomics of the human placenta: inferring the cell communication network of the maternal—fetal interface. Genome Res. 2017;27(3):349–361. doi:https://doi.org/10.1101/gr.207597.116
Wu S-P, Li R, DeMayo FJ. Progesterone receptor regulation of uterine adaptation for pregnancy. Trends Endocrinol Metab. 2018; doi:https://doi.org/10.1016/j.tem.2018.04.001
Vinketova K, Mourdjeva M, Oreshkova T. Human decidual stromal cells as a component of the implantation niche and a modulator of maternal immunity. J Pregnancy. 2016;2016. doi:https://doi.org/10.1155/2016/8689436
Popovici RM, Kao LC, Giudice LC. Discovery of new inducible genes in in vitro decidualized human endometrial stromal cells using microarray technology. Endocrinology. 2000;141(9):3510–3513. doi:https://doi.org/10.1210/endo.141.9.7789
Tierney EP, Tulac S, Huang S-TJ, Giudice LC. Activation of the protein kinase A pathway in human endometrial stromal cells reveals sequential categorical gene regulation. Physiol Genomics. 2003;16(1):47–66. doi:https://doi.org/10.1152/physiolgenomics.00066.2003
Takano M, Lu Z, Goto T, et al. Transcriptional cross talk between the forkhead transcription factor forkhead box O1A and the progesterone receptor coordinates cell cycle regulation and differentiation in human endometrial stromal cells. Mol Endocrinol. 2007;21(10):2334–2349. doi:https://doi.org/10.1210/me.2007-0058
Mazur EC, Vasquez YM, Li X, et al. Progesterone receptor transcriptome and cistrome in decidualized human endometrial stromal cells. Endocrinology. 2015;156(6):2239–2253. doi:https://doi.org/10.1210/en.2014-1566
Salker MS, Nautiyal J, Steel JH, et al. Disordered IL-33/ST2 activation in decidualizing stromal cells prolongs uterine receptivity in women with recurrent pregnancy loss. Fritz JH, ed. PLoS One. 2012;7(12):e52252. doi:https://doi.org/10.1371/journal.pone.0052252
Peter Durairaj RR, Aberkane A, Polanski L, et al. Deregulation of the endometrial stromal cell secretome precedes embryo implantation failure. MHR Basic Sci Reprod Med. 2017;23(7):478–487. doi:https://doi.org/10.1093/molehr/gax023
Godbole G, Suman P, Malik A, et al. Decrease in expression of HOXA10 in the decidua after embryo implantation promotes trophoblast invasion. Endocrinology. 2017 May 17;158(8):2618–2633. doi:https://doi.org/10.1210/en.2017-00032
Yu J, Berga SL, Johnston-MacAnanny EB, et al. Endometrial stromal decidualization responds reversibly to hormone stimulation and withdrawal. Endocrinology. 2016;157(6):2432–2446. doi:https://doi.org/10.1210/en.2015-1942
Trapnell C, Pachter L, Salzberg SL. TopHat: discovering splice junctions with RNA-seq. Bioinformatics. 2009;25(9):1105–1111. doi:https://doi.org/10.1093/bioinformatics/btp120
Anders S, Pyl PT, Huber W. HTSeq — a Python framework to work with high-throughput sequencing data. Bioinformatics. 2015;31(2):166–169. doi:https://doi.org/10.1093/bioinformatics/btu638
Wagner GP, Kin K, Lynch VJ. A model based criterion for gene expression calls using RNA-seq data. Theory Biosci. 2013;132(3):159–164. doi:https://doi.org/10.1007/s12064-013-0178-3
Robinson MD, McCarthy DJ, Smyth GK. edgeR: a Bioconductor package for differential expression analysis of digital gene expression data. Bioinformatics. 2010;26(1):139–140. doi:https://doi.org/10.1093/bioinformatics/btp616
Vasquez YM, Mazur EC, Li X, et al. FOXO1 is required for binding of PR on IRF4, novel transcriptional regulator of endometrial stromal decidualization. Mol Endocrinol. 2015;29(3):421–433. doi:https://doi.org/10.1210/me.2014-1292
Erkenbrack EM, Maziarz JD, Griffith OW, et al. The mammalian decidual cell evolved from a cellular stress response. PLoS Biol. 2018;16(8):e2005594. doi:https://doi.org/10.1371/journal.pbio.2005594
Xu B, Geerts D, Qian K, Zhang H, Zhu G. Myeloid ecotropic viral integration site 1 (MEIS) 1 involvement in embryonic implantation. Hum Reprod. 2008;23(6):1394–1406. doi:https://doi.org/10.1093/humrep/den082
Kommagani R, Szwarc MM, Vasquez YM, et al. The promyelocytic leukemia zinc finger transcription factor is critical for human endometrial stromal cell decidualization. In Spencer TE, ed. PLoS Genet. 2016;12(4):e1005937. doi:https://doi.org/10.1371/journal.pgen.1005937
Li Q, Kannan A, DeMayo FJ, et al. The antiproliferative action of progesterone in uterine epithelium is mediated by hand2. Science (80-). 2011;331(6019):912–916. doi:https://doi.org/10.1126/science.1197454
Ray S, Pollard JW. KLF15 negatively regulates estrogen-induced epithelial cell proliferation by inhibition of DNA replication licensing. Proc Natl Acad Sci U S A. 2012;109(21):E1334–E1343. doi:https://doi.org/10.1073/pnas.1118515109
Pabona JMP, Simmen FA, Nikiforov MA, et al. Krüppel-like factor 9 and progesterone receptor coregulation of decidualizing endometrial stromal cells: implications for the pathogenesis of endometriosis. J Clin Endocrinol Metab. 2012;97(3):E376–E392. doi:https://doi.org/10.1210/jc.2011-2562
Liu F, Guo J, Tian T, et al. Placental trophoblasts shifted Th1/Th2 balance toward Th2 and inhibited Th17 immunity at fetomaternal interface. APMIS. 2011;119(9):597–604. doi:https://doi.org/10.1111/j.1600-0463.2011.02774.x
Nagashima T, Maruyama T, Uchida H, et al. Activation of SRC kinase and phosphorylation of signal transducer and activator of transcription-5 are required for decidual transformation of human endometrial stromal cells. Endocrinology. 2008;149(3):1227–1234. doi:https://doi.org/10.1210/en.2007-1217
Vitorino Carvalho A, Eozenou C, Healey GD, et al. Analysis of STAT1 expression and biological activity reveals interferon-tau-dependent STAT1-regulated SOCS genes in the bovine endometrium. Reprod Fertil Dev. 2016;28(4):459–474. doi:https://doi.org/10.1071/RD14034
Christian M, Marangos P, Mak I, et al. Interferon-gamma modulates prolactin and tissue factor expression in differentiating human endometrial stromal cells. Endocrinology. 2001;142(7):3142–3151. doi:https://doi.org/10.1210/endo.142.7.8231
Ronchetti S, Migliorati G, Riccardi C. GILZ as a mediator of the anti-inflammatory effects of glucocorticoids. Front Endocrinol (Lausanne). 2015;6:170. doi:https://doi.org/10.3389/fendo.2015.00170
Brooks SA, Blackshear PJ. Tristetraprolin (TTP): interactions with mRNA and proteins, and current thoughts on mechanisms of action. Biochim Biophys Acta. 2013;1829(6–7):666–679. doi:https://doi.org/10.1016/j.bbagrm.2013.02.003
Stumpo DJ, Byrd NA, Phillips RS, et al. Chorioallantoic fusion defects and embryonic lethality resulting from disruption of Zfp36L1, a gene encoding a CCCH tandem zinc finger protein of the tristetraprolin family. Mol Cell Biol. 2004;24(14):6445–6455. doi:https://doi.org/10.1128/MCB.24.14.6445-6455.2004
Sun S-C. Non-canonical NF-κB signaling pathway. Cell Res. 2011;21(1):71–85. doi:https://doi.org/10.1038/cr.2010.177
Ogawa S, Satake M, Ikuta K. Physical and functional interactions between STAT5 and runx transcription factors. J Biochem. 2008;143(5):695–709. doi:https://doi.org/10.1093/jb/mvn022
Ziros PG, Georgakopoulos T, Habeos I, Basdra EK, Papavassiliou AG. Growth hormone attenuates the transcriptional activity of Runx2 by facilitating its physical association with Stat3beta. J Bone Miner Res. 2004;19(11):1892–1904. doi:https://doi.org/10.1359/JBMR.040701
Collins A, Littman DR, Taniuchi I. RUNX proteins in transcription factor networks that regulate T-cell lineage choice. Nat Rev Immunol. 2009;9(2):106–115. doi:https://doi.org/10.1038/nri2489
Voon DC-C, Hor YT, Ito Y. The RUNX complex: reaching beyond haematopoiesis into immunity. Immunology. 2015;146(4):523–536. doi:https://doi.org/10.1111/imm.12535
Lu BC, Cebrian C, Chi X, et al. Etv4 and Etv5 are required downstream of GDNF and Ret for kidney branching morphogenesis. Nat Genet. 2009;41(12):1295–1302. doi:https://doi.org/10.1038/ng.476
Herriges JC, Verheyden JM, Zhang Z, et al. FGF-regulated ETV transcription factors control FGF-SHH feedback loop in lung branching. Dev Cell. 2015;35(3):322–332. doi:https://doi.org/10.1016/j.devcel.2015.10.006
Boengler K, Pipp F, Fernandez B, Ziegelhoeffer T, Schaper W, Deindl E. Arteriogenesis is associated with an induction of the cardiac ankyrin repeat protein (CARP). Cardiovasc Res. 2003;59(3):573–581. http://www.ncbi.nlm.nih.gov/pubmed/14499858. Accessed May 28, 2018
Lee KH, Kim J-R. Hepatocyte growth factor induced up-regulations of VEGF through Egr-1 in hepatocellular carcinoma cells. Clin Exp Metastasis. 2009;26(7):685–692. doi:https://doi.org/10.1007/s10585-009-9266-7
Pillon NJ, Chan KL, Zhang S, et al. Saturated fatty acids activate caspase-4/5 in human monocytes, triggering IL-1β and IL-18 release. Am J Physiol Metab. 2016;311(5):E825–E835. doi:https://doi.org/10.1152/ajpendo.00296.2016
Osuga Y, Hirota Y, Yoshino O, Hirata T, Koga K, Taketani Y. Proteinase-activated receptors in the endometrium and endometriosis. Front Biosci (Schol Ed). 2012;4:1201–1212. http://www.ncbi.nlm.nih.gov/pubmed/22652866. Accessed May 28, 2018
Kunsch C, Lang RK, Rosen CA, Shannon MF. Synergistic transcriptional activation of the IL-8 gene by NF-kappa B p65 (RelA) and NF-IL-6. J Immunol. 1994;153(1):153–164. http://www.ncbi.nlm.nih.gov/pubmed/8207232. Accessed May 28, 2018
Bitko V, Velazquez A, Yang L, Yang YC, Barik S. Transcriptional induction of multiple cytokines by human respiratory syncytial virus requires activation of NF-kappa B and is inhibited by sodium salicylate and aspirin. Virology. 1997;232(2):369–378. doi:https://doi.org/10.1006/viro.1997.8582
Robb L, Li R, Hartley L, Nandurkar HH, Koentgen F, Begley CG. Infertility in female mice lacking the receptor for interleukin 11 is due to a defective uterine response to implantation. Nat Med. 1998;4(3):303–308. http://www.ncbi.nlm.nih.gov/pubmed/9500603. Accessed May 28, 2018
Gorrini C, Harris IS, Mak TW. Modulation of oxidative stress as an anticancer strategy. Nat Rev Drug Discov. 2013;12(12):931–947. doi:https://doi.org/10.1038/nrd4002
Kajihara T, Jones M, Fusi L, et al. Differential expression of FOXO1 and FOXO3a confers resistance to oxidative cell death upon endometrial decidualization. Mol Endocrinol. 2006;20(10):2444–2455. doi:https://doi.org/10.1210/me.2006-0118
Kania A, Klein R. Mechanisms of ephrin—Eph signalling in development, physiology and disease. Nat Rev Mol Cell Biol. 2016;17(4):240–256. doi:https://doi.org/10.1038/nrm.2015.16
Fujii H, Fujiwara H, Horie A, Sato Y, Konishi I. Ephrin A1 induces intercellular dissociation in Ishikawa cells: possible implication of the Eph-ephrin A system in human embryo implantation. Hum Reprod. 2011;26(2):299–306. doi:https://doi.org/10.1093/humrep/deq340
Luo Q, Liu X, Zheng Y, Zhao Y, Zhu J, Zou L. Ephrin-B2 mediates trophoblast-dependent maternal spiral artery remodeling in first trimester. Placenta. 2015;36(5):567–574. doi:https://doi.org/10.1016/j.placenta.2015.02.009
Dong H, Yu C, Mu J, Zhang J, Lin W. Role of EFNB2/EPHB4 signaling in spiral artery development during pregnancy: an appraisal. Mol Reprod Dev. 2016;83(1):12–18. doi:https://doi.org/10.1002/mrd.22593
Ruehl M, Somasundaram R, Schoenfelder I, et al. The epithelial mitogen keratinocyte growth factor binds to collagens via the consensus sequence glycine—proline—hydroxyproline. J Biol Chem. 2002;277(30):26872–26878. doi:https://doi.org/10.1074/jbc.M202335200
Kera H, Yuki S, Nogawa H. FGF7 signals are relayed to autocrine EGF family growth factors to induce branching morphogenesis of mouse salivary epithelium. Dev Dyn. 2014;243(4):552–559. doi:https://doi.org/10.1002/dvdy.24097
Zhou W-J, Hou X-X, Wang X-Q, Li D-J. Fibroblast growth factor 7 regulates proliferation and decidualization of human endometrial stromal cells via ERK and JNK pathway in an autocrine manner. Reprod Sci. 2017;24(12):1607–1619. doi:https://doi.org/10.1177/1933719117697122
Holland PM. Death receptor agonist therapies for cancer, which is the right TRAIL? Cytokine Growth Factor Rev. 2014;25(2):185–193. doi:https://doi.org/10.1016/j.cytogfr.2013.12.009
Lonergan M, Aponso D, Marvin KW, et al. Tumor Necrosis Factor-Related Apoptosis-Inducing Ligand (TRAIL), TRAIL receptors, and the soluble receptor osteoprotegerin in human gestational membranes and amniotic fluid during pregnancy and labor at term and preterm. J Clin Endocrinol Metab. 2003;88(8):3835–3844. doi:https://doi.org/10.1210/jc.2002-021905
Blanco O, Leno-Durán E, Morales JC, Olivares EG, Ruiz-Ruiz C. Human decidual stromal cells protect lymphocytes from apoptosis. Placenta. 2009;30(8):677–685. doi:https://doi.org/10.1016/j.placenta.2009.05.011
Siersbæk R, Nielsen R, Mandrup S. Transcriptional networks and chromatin remodeling controlling adipogenesis. Trends Endocrinol Metab. 2012;23(2):56–64. doi:https://doi.org/10.1016/j.tem.2011.10.001
Tripathi SK, Lahesmaa R. Transcriptional and epigenetic regulation of T-helper lineage specification. Immunol Rev. 2014;261(1):62–83. doi:https://doi.org/10.1111/imr.12204
Telley L, Govindan S, Prados J, et al. Sequential transcriptional waves direct the differentiation of newborn neurons in the mouse neocortex. Science. 2016;351(6280):1443–1446. doi:https://doi.org/10.1126/science.aad8361
Taylor HS, Igarashi P, Olive DL, Arici A. Sex steroids mediate HOXA11 expression in the human peri-implantation endometrium1. J Clin Endocrinol Metab. 1999;84(3):1129–1135. doi:https://doi.org/10.1210/jcem.84.3.5573
Mak IYH, Brosens JJ, Christian M, et al. Regulated expression of signal transducer and activator of transcription, Stat5, and its enhancement of PRL expression in human endometrial stromal cells in vitro. J Clin Endocrinol Metab. 2002;87(6):2581–2588. doi:https://doi.org/10.1210/jcem.87.6.8576
de Bruijn M, Dzierzak E. Runx transcription factors in the development and function of the definitive hematopoietic system. Blood. 2017;129(15):2061–2069. doi:https://doi.org/10.1182/blood-2016-12-689109
Komori T. Runx2, an inducer of osteoblast and chondrocyte differentiation. Histochem Cell Biol. 2018;149(4):313–323. doi:https://doi.org/10.1007/s00418-018-1640-6
Evans J, Salamonsen LA. Decidualized human endometrial stromal cells are sensors of hormone withdrawal in the menstrual inflammatory cascade1. Biol Reprod. 2014;90(1):14. doi:https://doi.org/10.1095/biolreprod.113.108175
King AE, Critchley HO, Kelly RW. The NF-kappaB pathway in human endometrium and first trimester decidua. Mol Hum Reprod. 2001;7(2):175–183. http://www.ncbi.nlm.nih.gov/pubmed/11160844. Accessed May 28, 2018
Kalkhoven E, Wissink S, van der Saag PT, van der Burg B. Negative interaction between the RelA(p65) subunit of NF-kappaB and the progesterone receptor. J Biol Chem. 1996;271(11):6217–6224. http://www.ncbi.nlm.nih.gov/pubmed/8626413. Accessed May 28, 2018
Zhang G, Cui L-J, Li A-Y, et al. Endometrial breakdown with sustained progesterone release involves NF-κB-mediated functional progesterone withdrawal in a mouse implant model. Mol Reprod Dev. 2016;83(9):780–791. doi:https://doi.org/10.1002/mrd.22686
Godbole G, Modi D. Regulation of decidualization, interleukin-11, and interleukin-15 by homeobox A 10 in endometrial stromal cells. J Reprod Immuno 2010;85(2):130–139. doi:https://doi.org/10.1016//j.jri.2010.03.003
Brighton PJ, Maruyama Y, Fishwick K, et al. Clearance of senescent decidual cells by uterine natural killer cells in cycling human endometrium. Elife. 2017;6:pii:e31274. doi:https://doi.org/10.7554/eLife.31274
Labied S, Kajihara T, Madureira PA, et al. Progestins regulate the expression and activity of the forkhead transcription factor FOXO1 in differentiating human endometrium. Mol Endocrinol. 2006;20(1):35–44. doi:https://doi.org/10.1210/me.2005-0275
Klotz L-O, Sánchez-Ramos C, Prieto-Arroyo I, Urbánek P, Steinbrenner H, Monsalve M. Redox regulation of FoxO transcription factors. Redox Biol. 2015;6:51–72. doi:https://doi.org/10.1016/j.redox.2015.06.019
Author information
Authors and Affiliations
Corresponding author
Additional information
Authors’ Note
Data described in this manuscript were acquired at Yale University.
Rights and permissions
About this article
Cite this article
Rytkönen, K.T., Erkenbrack, E.M., Poutanen, M. et al. Decidualization of Human Endometrial Stromal Fibroblasts is a Multiphasic Process Involving Distinct Transcriptional Programs. Reprod. Sci. 26, 323–336 (2019). https://doi.org/10.1177/1933719118802056
Published:
Issue Date:
DOI: https://doi.org/10.1177/1933719118802056