Abstract
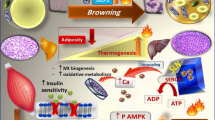
It has been documented that exogenously administered irisin (1010 fibronectin-type III domain-containing 5 [FNDC5]), which is a new polypeptide hormone, induces the browning of subcutaneous fat and thermogenesis. In this study, effects of physical activity and exogenous administration of irisin were investigated on parameters related with reproduction and metabolism in the high-fat diet-induced obesity model of the female C57BL/6J mice. Sixty mice were gathered at age approximately 5 to 6weeks and were divided into 3 groups. Control group remained sedentary. Irisin group remained also sedentary but intravenously received 1010 FNDC5-expressing adenovirus after 20 weeks. Exercise group performed treadmill after 6 weeks. All mice were sacrificed 22 to 23 weeks after the start of the study. There was a significantly greater A weight in the controls compared with the irisin and exercise groups (P <.05). Glucose and insulin levels were significantly higher in the controls (P <.05). The serum irisin level was significantly higher in the exercise group (P <.05). Serum luteinizing hormone levels were significantly increased in the irisin group (P <.05). Serum anti-Miillerian hormone levels were significantly higher in irisin and exercise groups (P <.05). There were significant negative correlations between serum irisin levels and A weight and homeostatic model assessment of insulin resistance (r = -0.327, r = -0.297, respectively; P <.05 for both). The numbers of primordial follicles per ovary were similar (P >.05), whereas primary and secondary follicles per ovary were higher in the irisin and exercise groups compared with controls (P <.05). Pharmacologic introduction of irisin may improve metabolic factors such as insulin sensitivity and obesity by promoting weight loss and consequently improving the reproductive potential.
Similar content being viewed by others
References
Speakman JR, Selman C. Physical activity and resting metabolic rate. Proc Nutr Soc. 2003;62(3):621–634.
Bostrom P, Wu J, Jedrychowski MP, et al. A PGCl-alpha-dependent myokine that drives brown-fat-like development of white fat and thermogenesis. Nature. 2012;481(7382):463–468.
Kelly DP. Medicine. Irisin, light my fire. Science. 2012;336(6077):42–43.
Hassan MA, Killick SR. Negative lifestyle is associated with a significant reduction in fecundity. Fertil Steril. 2004;81(2):384–392.
Rogers J, Mitchell GW Jr. The relation of obesity to menstrual disturbances. N Engl J med. 1952;247(2):53–55.
Hartz AJ, Barboriak PN, Wong A, Katayama KP, Rimm AA. The association of obesity with infertility and related menstural abnormalities in women. Int J Obes. 1979;3(1):57–73.
Norman RJ, Clark AM. Obesity and reproductive disorders: a review. Reprod Fertil Dev. 1998;10(1):55–63.
Rich-Edwards JW, Goldman MB, Willett WC, et al. Adolescent body mass index and infertility caused by ovulatory disorder. Am J Obstet Gynecol. 1994;171(1):171–177.
Linne Y. Effects of obesity on women’s reproduction and complications during pregnancy. Obes Rev. 2004;5(3):137–143.
Chinsomboon J, Ruas J, Gupta RK, et al. The transcriptional coactivator PGC-1alpha mediates exercise-induced angiogenesis in skeletal muscle. Proc Natl Acad Sci U S A. 2009;106(50):21401–21406.
Caligioni CS. Assessing reproductive status/stages in mice. Curr Protoc Neurosci. 2009; Appendix 4Appendix 41.
Myers M, Britt KL, Wreford NG, Ebling FJ, Kerr JB. Methods for quantifying follicular numbers within the mouse ovary. Reproduction. 2004;127(5):569–580.
Taskin EI, Akgun-Dar K, Kapucu A, et al. Apoptosis-inducing effects of Morinda citrifolia L. and doxorubicin on the Ehrlich ascites tumor in Balb-c mice. Cell Biochem Funct. 2009;27(8):542–546.
Senturk LM, Seli E, Gutierrez LS, Mor G, Zeyneloglu HB, Arici A. Monocyte chemotactic protein-1 expression in human corpus luteum. Mol Hum Reprod. 1999;5(8):697–702.
Folch J, Lees M, Sloane Stanley GH. A simple method for the isolation and purification of total lipides from animal tissues. J Biol Chem. 1957;226(1):497–509.
Pedersen BK, Febbraio MA. Muscles, exercise and obesity: skeletal muscle as a secretory organ. Nat Rev Endocrinol. 2012;8(8):457–465.
Moreno-Navarrete JM, Ortega F, Serrano M, et al. Irisin is expressed and produced by human muscle and adipose tissue in association with obesity and insulin resistance. J Clin Endocrinol Metab. 2013;98(4):E769–E778.
Pardo M, Crujeiras AB, Amil M, et al. Association of irisin with fat mass, resting energy expenditure, and daily activity in conditions of extreme body mass index. Int J Endocrinol. 2014;2014:857270.
Huh JY, Panagiotou G, Mougios V, et al. FNDC5 and irisin in humans: I. predictors of circulating concentrations in serum and plasma and II. mRNA expression and circulating concentrations in response to weight loss and exercise. Metabolism. 2012;61(12):1725–1738.
Staiger H, Bohm A, Scheler M, et al. Common genetic variation in the human FNDC5 locus, encoding the novel muscle-derived ’browning’ factor irisin, determines insulin sensitivity. PloS One. 2013;8(4):e61903.
Laven JS, Mulders AG, Visser JA, Themmen AP. De Jong FH, Fauser BC. Anti-mullerian hormone serum concentrations in nor-moovulatory and anovulatory women of reproductive age. J Clin Endocrinol Metab. 2004;89(1):318–323.
Freeman EW, Gracia CR, Sammel MD, Lin H, Lim LC. Strauss JF III. Association of anti-mullerian hormone levels with obesity in late reproductive-age women. Fertil Steril. 2007;87(1):101–106.
Su HI, Sammel MD, Freeman EW, Lin H, DeBlasis T, Gracia CR. Body size affects measures of ovarian reserve in late reproductive age women. Menopause. 2008;15(5):857–861.
Moy V, Jindal S, Lieman H, Buyuk E. Obesity adversely affects serum anti-mullerian hormone (AMH) levels in Caucasian women. J Assist Reprod Genet. 2015;32(9):1305–1311.
Ogden CL, Carroll MD, Curtin LR, Lamb MM, Flegal KM. Prevalence of high body mass index in US children and adolescents, 2007-2008. JAMA. 2010;303(3):242–249.
Robker RL, Wu LL, Yang X. Inflammatory pathways linking obesity and ovarian dysfunction. J Reprod Immunol. 2011;88(2):142–148.
Wittemer C, Ohl J, Bailly M, Bettahar-Lebugle K, Nisand I. Does body mass index of infertile women have an impact on IVF procedure and outcome? J Assist Reprod Genet. 2000;17(10):547–552.
Dokras A, Baredziak L, Blaine J, Syrop C, VanVoorhis BJ, Sparks A. Obstetric outcomes after in vitro fertilization in obese and morbidly obese women. Obstet Gynecol. 2006;108(1):61–69.
Esinler I, Bozdag G, Yarali H. Impact of isolated obesity on ICSI outcome. Reprod Biomed Online. 2008;17(4):583–587.
Xie F, Anderson CL, Timme KR, Kurz SG, Fernando SC, Wood JR. Obesity-dependent increases in oocyte mRNAs are associated with increases in proinflammatory signaling and gut microbial abundance of Lachnospiraceae in female mice. Endocrinology. 2016;157(4):1630–1643.
Jungheim ES, Schoeller EL, Marquard KL, Louden ED, Schaffer JE, Moley KH. Diet-induced obesity model: abnormal oocytes and persistent growth abnormalities in the offspring. Endocrinology. 2010;151(8):4039–4046.
Wu LL, Dunning KR, Yang X, et al. High-fat diet causes lipo-toxicity responses in cumulus-oocyte complexes and decreased fertilization rates. Endocrinology. 2010;151(11):5438–5445.
Caillon H, Freour T, Bach-Ngohou K, et al. Effects of female increased body mass index on in vitro fertilization cycles outcome. Obes Res Clin Pract. 2015;9(4):382–388.
Minge CE, Bennett BD, Norman RJ, Robker RL. Peroxisome proliferator-activated receptor-gamma agonist rosiglitazone reverses the adverse effects of diet-induced obesity on oocyte quality. Endocrinology. 2008;149(5):2646–2656.
Igosheva N, Abramov AY, Poston L, et al. Maternal diet-induced obesity alters mitochondrial activity and redox status in mouse oocytes and zygotes. PloS One. 2010;5(4):e10074.
Bermejo-Alvarez P, Rosenfeld CS, Roberts RM. Effect of maternal obesity on estrous cyclicity, embryo development and blastocyst gene expression in a mouse model. Hum Reprod. 2012;27(12):3513–3522.
Bazzano MV, Torelli C, Pustovrh MC, Paz DA, Elia EM. Obesity induced by cafeteria diet disrupts fertility in the rat by affecting multiple ovarian targets. Reprod Biomed Online. 2015;31(5):655–667.
Richards JS, Sharma SC, Falender AE, Lo YH. Expression of FKHR, FKHRL1, and AFX genes in the rodent ovary: evidence for regulation by IGF-I, estrogen, and the gonadotropins. Mol Endocrinol. 2002;16(3):580–599.
Cunningham MA, Zhu Q, Unterman TG, Hammond JM. Follicle-stimulating hormone promotes nuclear exclusion of the forkhead transcription factor FoxOla via phosphatidylinositol 3-kinase in porcine granulosa cells. Endocrinology. 2003;144(12):5585–5594.
Shi F, LaPolt PS. Relationship between FoxOl protein levels and follicular development, atresia, and luteinization in the rat ovary. J Endocrinol. 2003;179(2):195–203.
Kajihara T, Uchino S, Suzuki M, Itakura A, Brosens JJ, Ishihara O. Increased ovarian follicle atresia in obese Zucker rats is associated with enhanced expression of the forkhead transcription factor FOXO1. Med Mol Morphol. 2009;42(4):216–221.
Liu Z, Castrillon DH, Zhou W, Richards JS. FOXO1/3 depletion in granulosa cells alters follicle growth, death and regulation of pituitary FSH. Mol Endocrinol. 2013;27(2):238–252.
Cunningham MA, Zhu Q, Hammond JM. FoxOla can alter cell cycle progression by regulating the nuclear localization of p27kip in granulosa cells. Mol Endocrinol. 2004;18(7):1756–1767.
John GB, Shirley LJ, Gallardo TD, Castrillon DH. Specificity of the requirement for Foxo3 in primordial follicle activation. Reproduction. 2007;133(5):855–863.
Brenkman AB, Burgering BM. Fox03a eggs on fertility and aging. Trends Mol Med. 2003;9(11):464–467.
John GB, Gallardo TD, Shirley LJ, Castrillon DH. Foxo3 is a PI3K-dependent molecular switch controlling the initiation of oocyte growth. Dev Biol. 2008;321(1):197–204.
Hosaka T, Biggs WH III, Tieu D, et al. Disruption of forkhead transcription factor (FOXO) family members in mice reveals their functional diversification. Proc Natl Acad Sci U S A. 2004;101(9):2975–2980.
Geva E, Jaffe RB. Role of vascular endothelial growth factor in ovarian physiology and pathology. Fertil Steril. 2000;74(3):429–438.
Jablonka-Shariff A, Olson LM. The role of nitric oxide in oocyte meiotic maturation and ovulation: meiotic abnormalities of endothelial nitric oxide synthase knock-out mouse oocytes. Endocrinology. 1998;139(6):2944–2954.
Ellman C, Corbett JA, Misko TP, McDaniel M, Beckerman KP. Nitric oxide mediates interleukin-1-induced cellular cytotoxicity in the rat ovary. A potential role for nitric oxide in the ovulatory process. J Clin Invest. 1993;92(6):3053–3056.
Shukovski L, Tsafriri A. The involvement of nitric oxide in the ovulatory process in the rat. Endocrinology. 1994;135(5):2287–2290.
Sengoku K, Takuma N, Horikawa M, et al. Requirement of nitric oxide for murine oocyte maturation, embryo development, and trophoblast outgrowth in vitro. Mol Reprod Dev. 2001;58(3):262–268.
Chun SY, Eisenhauer KM, Kubo M, Hsueh AJ. Interleukin-1 beta suppresses apoptosis in rat ovarian follicles by increasing nitric oxide production. Endocrinology. 1995;136(7):3120–3127.
Sugino N, Takiguchi S, Ono M, et al. Nitric oxide concentrations in the follicular fluid and apoptosis of granulosa cells in human follicles. Hum Reprod. 1996;11(11):2484–2487.
Mitchell LM, Kennedy CR, Hartshorne GM. Expression of nitric oxide synthase and effect of substrate manipulation of the nitric oxide pathway in mouse ovarian follicles. Hum Reprod. 2004;19(1):30–40.
Basini G, Grasselli F. Nitric oxide in follicle development and oocyte competence. Reproduction. 2015;150(1):R1–R9.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Bastu, E., Zeybek, U., Gurevin, E.G. et al. Effects of Irisin and Exercise on Metabolic Parameters and Reproductive Hormone Levels in High-Fat Diet-Induced Obese Female Mice. Reprod. Sci. 25, 281–291 (2018). https://doi.org/10.1177/1933719117711264
Published:
Issue Date:
DOI: https://doi.org/10.1177/1933719117711264