Abstract
Targeting cancer via ROS-based mechanism has been proposed as a radical therapeutic approach. Cancer cells exhibit higher endogenous oxidative stress than normal cells and pharmacological ROS insults via either enhancing ROS production or inhibiting ROS-scavenging activity can selectively kill cancer cells. In this study, we randomly chose 4 cancer cell lines and primary colon or rectal cancer cells from 4 patients to test the hypothesis and obtained following paradoxical results: while piperlongumin (PL) and β-phenylethyl isothiocyanate (PEITC), 2 well-defined ROS-based anticancer agents, induced an increase of cellular ROS and killed effectively the tested cells, lactic acidosis (LA), a common tumor environmental factor that plays multifaceted roles in promoting cancer progression, induced a much higher ROS level in the tested cancer cells than PL and PEITC, but spared them; L-buthionine sulfoximine (L-BSO, 20 μM) depleted cellular GSH more effectively and increased higher ROS level than PL or PEITC but permitted progressive growth of the tested cancer cells. No evident dose-response relationship between cellular ROS level and cytotoxicity was observed. If ROS is the effecter, it should obey the fundamental therapeutic principle – the dose-response relationship. This is a major concern.
Similar content being viewed by others
Introduction
Persistent high ROS level is a common biochemical feature of cancer cells1,2,3. Cancer cells rely on moderate increase of cellular ROS, which plays multiple vital roles in cancer cell survival and proliferation, tumor angiogenesis and growth, cancer invasion and metastasis and even resistance to therapy1,4,5,6,7,8. On the other hand, the higher level ROS in cancer cells than that in normal cells may render the former more vulnerable to further ROS insults. The pharmacological approach on this basis was proposed a decade ago9,10. The biological basis underlying this approach is straightforward: the higher endogenous ROS level in cancer cells than that in normal cells is the basis for therapeutic selectivity, pharmacologically active prooxidants, via either promoting ROS production or inhibiting ROS-scavenging systems, can increase ROS to lethal level preferentially in cancer cells, leading to irreversible oxidative damage and cell death. Trachootham et al.1 outlined the biological basis of the therapeutic approach, the current status of the research in this field and future perspectives. Piperlongumine (PL)11,12,13 and β-phenylethyl isothiocyanate (PEITC)14,15,16,17,18 are typical ROS-based anticancer agents with great potential in clinical application. So far, numerous agents targeting tumor ROS modulation have entered clinical trials1,19.
However, after reviewing the previous publications in the field, we found that the fundamental basis of the therapy – the causative role of ROS in cancer cell death - is unclear, because it is not known if pharmacologically-induced ROS level is truly excessive or fatal to cancer cells. The evidence we could find in the previous publications to support this claim are: anticancer prooxidants can induce an increase of ROS concurrently with a cell death and antioxidants such as N-acetylcysteine (NAC) can antagonize prooxidant-induced ROS and attenuate cell death. The evidence is important but not enough, because one can argue based on the following questions: is there any agent with potency to augment ROS stronger than anticancer prooxidants but permit cell survival? Is it possible that antioxidants can antagonize prooxidant-induced ROS but cannot block cell death or antioxidants can block prooxidant-induced cell death but cannot antagonize ROS? More importantly, if ROS is the effecter that kills or inhibit cancer cells, it should obey the therapeutic principle - dose-response relationship. Therefore, the anticancer efficacy of pharmacologically active prooxidants should correlate with their potency to disable GSH antioxidant system and/or to augment ROS and cell death rate should be proportional to cellular ROS level when it reaches toxic level or inversely proportional to cellular GSH level. These lines of evidence are essential but lacking.
We would address these issues as described below.
Results and discussion
Lactic acidosis induces a much higher cellular ROS level than PEITC or PL but permits a progressive growth of the tested cancer cells
4T1 cancer cells were treated with lactic acidosis (LA), PEITC, PL, doxorubicin (Dox), or arsenic trioxide (ATO). PEITC and PL increases ROS by depleting GSH11,14, Dox enhances ROS production via quinone one-electron redox cycling20 and ATO promotes ROS production via inhibiting mitochondrial respiratory chain21. LA, a common environmental factor of diverse cancers22, has been shown to induce a dramatic increase of ROS in endothelial cells23.
LA dramatically increased cellular ROS level and maintained it in 4T1 cancer cells in a time course of 60 hours (Fig. 1a & b). The LA condition used in this study was within the physiological range of pH and lactate levels in solid tumors22. LA increased ROS by ~30 folds, much higher than those induced by PEITC, PL, Dox and ATO (Fig. 1c). Paradoxically, LA only slowed down the proliferation rate of 4T1 cancer cells (Fig. 1d, note that cells still kept a progressive growth), while the others killed the cells (Fig. 1d). Similar results were obtained by using Bcap37, Hela and HepG2 cells (Supplementary Fig. S1–3). LA had no harmful effect on 4T1 cells and other cancer cells even in the long-term culture, instead, it conferred cancer cells (4T1, Bcap37, RKO, SGC7901) with resistance to metabolic stress, such as glucose deprivation24.
LA is a more potent ROS inducer than PEITC, PL, Dox, or ATO but does not kill 4T1 cells.
(a) 4T1 cells were incubated with LA (2.5–25 mM) for 4 hours and cellular ROS was probed by DCFH-DA. (b) 4T1 cells were incubated with LA (20 mM) and at the indicated time points, cellular ROS was probed by DCFH-DA. (c) Comparison of cellular ROS induced by LA, PEITC, PL, Dox and ATO. Cells were treated with LA (20 mM), PEITC (10 μM), PL (10 μM), Dox (10 μg/ml), or ATO (10 μM) for 4 hours and intracellular ROS was probed by DCFH-DA. (d) 4T1 cells were incubated with LA (20 mM), PEITC (10 μM), PL (10 μM), Dox (10 μg/ml) or ATO (10 μM), at the indicated time points, cell counts were performed. Experiments are repeated at least 3 times. Scale bar = 50 μm. *** p < 0.001.
L-BSO induces a severer oxidative stress than PEITC or PL but permits a progressive growth of the tested cancer cells
L-BSO is a classical γ-glutamylcysteine synthetase inhibitor25 and it is probably the most widely used agent for depleting cellular GSH26, the most important antioxidant in cells. L-BSO is also a ROS-based anticancer agent1. We used concentration and time dependent assays to define a concentration of L-BSO (20 μM) which depleted ~95% GSH (Fig. 2 a & b).
L-BSO, a more potent oxidative agent than PEITC and PL, allows a progressive growth of 4T1 cells.
(a) 4T1 cells were incubated with L-BSO (2.5–100 μM) for 48 hours and cellular GSH and GSSG were assayed as described in materials and methods. (b) 4T1 cells were incubated with L-BSO (20 μM), at the indicated time points, cells were collected and subjected for GSH and GSSG quantitation. (c) Cells were incubated with L-BSO, PEITC and PL at the indicated time points, cells were collected and cellular ROS was probed by DCFH-DA. (d & e) Cellular GSH and ROS change in cells treated with L-BSO, PEITC and PL. Cells were treated with PEITC (10 μM) or PL (10 μM) for 4 hours, or treated with L-BSO (20 μM) for 12 hours, followed by ROS, GSH and GSSG measurement, as described in Materials & Methods. (f) 4T1 cells were incubated with L-BSO (20 μM), PEITC (10 μM), or PL (10 μM), at the indicated time points, cell counts were performed. Experiments are repeated at least 3 times. Scale bar = 50 μm. ** p < 0.01, *** p < 0.001.
Then, we compared L-BSO (20 μM) with PL or PEITC with respect to their activity to deplete GSH (Fig. 2c). L-BSO was more potent in augmenting ROS and depleting GSH than PL or PEITC. L-BSO induced a sustained high ROS level and sustained depletion of GSH, whereas PL and PEITC induced a transient elevation of ROS followed by a decline. The decline of ROS in PEITC-treated cells was due to the loss of cell viability. Then we did an experiment to directly compare ROS and GSH levels in cells treated with L-BSO, PL, or PEITC. Cells were divided into 4 groups, control, L-BSO, PL and PEITC. L-BSO was added first. After 8-hour incubation, PL or PEITC was added. After another 4-hour incubation (because ROS peaks at the 4-hour point after PL and PEITC treatment [Fig. 2c], using this time point for comparison is appropriate.), cells were subjected for ROS and GSH measurement (Fig. 2d & e). L-BSO depleted GSH more efficiently than and induced a significantly higher ROS level than PL and PEITC. Unlike PEITC or PL, which killed 4T1 cells, L-BSO did not kill them (Fig. 2f). The results were reproduced by using Bcap37, HepG2 and Hela cells (Supplementary Fig. S1–3). Previously, Fath et al27 demonstrated that even 100 μM L-BSO does not kill A549 and H292 cancer cells. Miller et al showed that 20 μM BSO did not change the doubling time of PR4 cells, a ras-transformed NIH 3T3 subclones28.
The results pose a paradox. Although PEITC, PL and L-BSO all increase ROS via depleting GSH1,11,14, the fate of the cells are opposite. More confounding is that L-BSO, the more potent one to deplete cellular GSH than PL or PEITC does not kill the tested cancer cells.
H2O2 induces a higher oxidative stress than PEITC or PL but permits cell growth
Exogenous H2O2 is often used to study the effect of oxidative stress on cancer cells. We compared the oxidative stress induced by H2O2 (0.1 mM) with those induced by PETIC or PL. 0.1 mM H2O2 exerted a severer oxidative stress on 4T1 cells than PEITC, PL (Fig. 3a–c), note that hydroxyl free radical, the most toxic free radical and the decomposed product from H2O2, is ~2 folds higher than those induced by PEITC or PL. Unlike PL or PEITC, which killed 4T1 cells, 0.1 mM H2O2 allowed progressive growth of 4T1 cells (Fig. 3d). Similar results were obtained using Bcap37, Hela and HepG2 cells (Supplementary Fig. S1–3).
Hydrogen peroxide induces a severe oxidative stress which does not kill 4T1 cells.
(a) Time course of ROS in 4T1 cells treated with 0.1 mM hydrogen peroxide. (b & c) ROS levels (probed by DCFH-DA and HPF) in 4T1 cells treated with 0.1 mM hydrogen peroxide, 10 μM PEITC, or 10 μM PL. (d) 4T1 cell growth in the absence or presence of 0.1 mM hydrogen peroxide, 10 μM PEITC, or 10 μM PL. ** p < 0.01, *** p < 0.001. Data were repeated at least 3 times.
100 μM H2O2 is a very high concentration. It is not known if this concentration of H2O2 in vivo could be generated and maintained.
LA-induced ROS contains highly reactive species whose concentrations are significantly higher than those induced by anticancer prooxidants
ROS is composed of many species, some of which are more chemically reactive than hence more toxic than others, e.g., hydroxyl free radical is much more reactive than superoxide. Because the quantity of ROS induced by LA is far higher than that induced by PEITC or PL but does not kill cancer cells, we assumed that the composition of ROS induced by anticancer prooxidants might be different from and more deadly than that by LA. We determined several reactive species using available probes (Fig. 4a). DCFH-DA fluorescent signals largely reflected the concentrations of NO2· and CO3·−29, which were much higher in cells exposed to LA than to PEITC or PL. HPF signal (·OH or ONOO− level) was significantly higher in cells exposed to LA than those exposed to PL, PEITC, or ATO. LA induced an elevation of extra-mitochondria superoxide levels (probed by DHE), but PL increased intra-mitochondria superoxide (probed by MitoSOX Red) by ~3 folds higher than LA. This difference might account for toxicity of PL, but confounded to interpret the toxicity of PEITC or ATO, which showed similar toxicity as but much lower activity to augment intra-mitochondrial superoxide than PL. Nitric oxide levels (DAF-FM signal) were comparable with each other. We repeated the experiments using Bcap 37, Hela and HepG2 cells and obtained similar results (Supplementary Fig. S4–6).
ROS species and malonaldehyde in 4T1 cells treated by LA, L-BSO, H2O2, PEITC, PL, ATO, or Dox.
(a) The composition of ROS in 4T1 cells. (b) MDA content in 4T1 cells. ROS levels were measured by 5 probes and MDA were measured as described in Materials and Methods. Experiments are repeated 3 times. Scale bar = 50 μm. ** p < 0.01, ***, p < 0.001.
The results demonstrated that the levels of ·OH, ONOO− and CO3·− induced by LA were significantly higher than that by other treatments (Fig. 4a). It should be noted that ·OH is the most reactive free radical identified so far and ONOO− and CO3·− are highly reactive30. Therefore, LA induced-ROS is quantitatively higher and qualitatively more toxic than ROS-based anticancer drug -induced one in the tested cancer cells, but paradoxically, it does not kill the tested cancer cells.
ROS versus MDA
In order to confirm if ROS induced by LA, PEITC, PL, Dox, or ATO exert oxidative stress in 4T1 cancer cells, we measured malondialdehyde (MDA), a product generated from lipid peroxidation. Indeed, these treatments caused an increased MDA generation, LA caused a highest MDA production (Fig. 4b), followed by H2O2, L-BSO. MDA Levels in cells treated by PEITC, PL, ATO and Dox were comparable with each other and were marginally increased in comparison to control. The results further suggest that LA induced a higher oxidative stress than PL, PEITC, ATO and Dox in 4T1 cells.
The effect of LA and prooxidants on antioxidative enzymes
Apart from GSH, we measured the activities of superoxide dismutase (SOD), catalase (CAT), glutathione peroxidase (GPX) and glutathione reductase (GR) in the cell lysate derived from 4T1 cells treated with LA, L-BSO, H2O2, PETIC, PL, Dox, or ATO. The treatment, except PEITC, an inhibitor of GR31, did not significantly alter the activity of these antioxidant enzymes (Supplementary Fig. S7) in this cell line.
No evident dose-response relationship between cellular ROS level and cell growth inhibition or death
We would further discuss the rationale of ROS-based therapy. According to the prevailing hypothesis (Fig. 5a)32, there is a toxic threshold of ROS. In cancer cells, ROS production and scavenging system are both upregulated. The upregulated ROS scavenging capacity in cancer cells keeps ROS level below the toxic threshold. Kinetically, although ROS flux in cancer cells is high, ROS level or readout is below the toxic threshold. The redox balance is intricately maintained in cancer cells. On the other hand, because ROS flux in cancer cells is high, redox balance is vulnerable to pharmacological intervention either via inhibiting ROS scavenging or enhancing ROS production. When the redox balance is disturbed, ROS production overwhelms ROS scavenging, high ROS flux would result in ROS accumulation to toxic threshold. When ROS level reaches death threshold, it can not only cause irreversible oxidative damage but also trigger death signaling. Prooxidants such as PL and PEITC kill cancer cells via elevating ROS to toxic threshold11,14. Moreover, the higher basal ROS level in cancer cells than that in normal cells lays the basis for the therapeutic selectivity, i.e., cancer cells, but not normal cells, are sensitive to further ROS insults, such that exogenous ROS inducer can selectively eliminate cancer cells.
No evident dose-response relationship between cellular ROS level and cell growth inhibition or death.
(a) The current model of ROS-based therapy (copied from Ref. 1) – ROS modulation as the biological basis for therapeutic selectivity. Cancer cells show higher inherent ROS levels than normal cells. This difference is the basis for therapeutic selectivity. The exogenous ROS insults would kill cancer cells by increasing intracellular ROS to lethal concentration but spare normal cells. Note that it is on the premise that the basal ROS level in cancer cells is significant and near the lethal threshold. This is the basis for the feasibility of this therapy. (b) We show that the basal ROS level in cancer cells is negligible and even pharmacologically active prooxidant-induced ROS is far below that induced by LA, which does not kill 4T1 cells. (c & d) 4T1 cell death or cell growth inhibition is irrelevant with the potency of exogenous insults to augment ROS or to deplete GSH. (e) Cellular GSH level is not inversely proportional to ROS level. Except L-BSO treatment, in which cellular ROS and GSH levels were determined 12 hours after L-BSO exposure, ROS and GSH levels in cells exposed to other agents were measured 4 hours after treatment. Cell counts were performed 48 hours after treatment.
On the other hand, we came to a different point of view (Fig. 5b). First, if the endogenous ROS level in cancer cells is the biological basis for therapeutic selectivity, its concentration would be close to lethal threshold as depicted in Fig. 5a. However, we show that the endogenous ROS level is virtually negligible, as compared with LA-induced one. Second, although it is believed that pharmacologically-induced ROS level is greater than the toxic threshold11,14, we show that it is much lower than that induced by LA, which permit progressive growth. Thus, the toxic threshold of ROS is a key issue unresolved, at least in the tested cancer cells.
More importantly, according to the therapeutic principle, a therapeutic drug must show a dose-response relationship. If ROS is the effecter, cancer cells shall respond to ROS in a dose-dependent manner. Thus, cell growth inhibition or cell death should be inversely proportional to cellular ROS level when it reaches toxic level. If PEITC or PL-induced cellular ROS level is taken as the reference of toxic threshold, the higher ROS concentrations would be more toxic. We plotted the cell (4T1, Bcap37, Hela, HepG2) growth against ROS levels or GSH level and ROS levels against GSH level. The plots showed that growth inhibition or cell death was not associated with the potency of agents to augment ROS (Fig. 5c, Supplementary Fig. S8) or to deplete GSH (Fig. 5d, Supplementary Fig. S8), e.g., LA, the most potent ROS-inducer, allowed a rapid cell proliferation, in sharp contrast to much weak ROS-inducers PEITC, PL, ATO, or DOX, which killed ~71–94% of seeding cells. ROS level was not inversely proportional to GSH level (Fig. 5e, Supplementary Fig. S8). Taken together, there is no evident dose-response relationship between cellular ROS level and cell death or cell proliferation in the tested cells.
The effects of N-acetylcysteine on prooxidant-induced cell death and ROS are complicated
NAC, an antioxidant, is often used as a discriminator to verify if cell death is associated with ROS.
NAC exhibited a concentration-dependent inhibition on PEITC-induced ROS in 4T1 cells (Fig. 6a). Although NAC at 4 mM fully reversed PEITC-induced ROS to basal level, it only delayed but did not block PEITC-induced death, as the viable cell numbers with or without NAC ultimately were the same (Fig. 6a).
NAC effect on PEITC- or PL-induced 4T1 cell death.
(a) NAC fully reverses PEITC-induced ROS to basal level but does not rescue cell death. Left panel shows ROS levels (probed by DCFH-DA) in 4T1 cells treated with 10 μM PEITC in the presence or absence of NAC. Right panel shows 4T1 cell growth inhibition (lower growth rate) or death. (b) NAC fully rescues PL-induced 4T1 cell death but only partially reverses ROS basal. 4T1 Cells were treated with 10 μM PL in the presence or absence of NAC. Cell counts were done at the indicated time intervals. ** p < 0.01, *** p < 0.001. Experiments were performed for 3 times.
Similarly, 4 mM NAC could completely reverse Dox- or ATO-induced ROS to basal level but could not block cell death (Supplementary Fig. S9 & 10).
Unlike its effect on PEITC, NAC exhibited a weak inhibition on PL-induced ROS increase (Fig. 6b). There was no evident concentration-dependent effect of NAC on PL-induced ROS. Interestingly, NAC at 1 mM blocked PL-induced cell death, NAC at 4 mM abolished the hazardous effect of PL (Fig. 6b).
Thus, NAC completely reversed ROS induced by PEITC, Dox, or ATO to basal level but did block cell death; on the other hand, NAC only partially inhibited PL-induced ROS but completely blocked PL-induced cell death. We obtained consistent results by using Bcap 37, Hela and HepG2 cells (Supplementary Fig. S11–14). The results suggested that prooxidant-induced ROS was not tightly linked with the death of 4T1, Bcap37, Hela and HepG2.
Our results seem to be contradictory to but in fact are generally consistent with previous reports. Trachootham et al.14 showed that NAC (3 mM) fully reversed PEITC-induced ROS and significantly attenuated PEITC-induced death in a time course of 5 hours. As they did not show data of longer time points, it was not known if NAC delayed or blocked PEITC-induced cell death. We showed that NAC only delayed but did not block PEITC-induced cell death. Raj et al.11 showed that NAC (3 mM) fully reverse PL-induced ROS to basal level in EJ cells and completely blocked cell death. We also observed that 4 mM NAC completely blocked PL-induced cell death (Fig. 6b). The only discrepancy was the inhibitory effect of NAC on PL-induced ROS: while Raj et al. demonstrated that NAC fully inhibited PL-induced ROS, we showed that NAC only partially reversed PL-increased ROS (Fig. 6b). The results were consistent using 4 different cell lines, as described above. Therefore, the third party to perform the same experiments would be the proper way to resolve the discrepancy.
SOD and catalase mimetics reverse PL- or PEITC-induced ROS but do not rescue cell death
We further used SOD and catalase mimetics (EUK8 & EUK134) to intervene the action of PL or PETIC on cancer cells. Although EUK8 or EUK134 could fully reverse PL- or PEITC-induced ROS, they did not rescue cell death (Fig. 7). The results convey the same implication as NAC experiments.
SOD and catalase mimetics fully reverse PEITC- or PL-induced ROS to basal level but does not rescue 4T1 cell death.
4T1 cells were treated with 10 μM PEITC or PL in the presence or absence of EUK8 or EUK134. Cell counts were done at the indicated time intervals. *** p < 0.001. Experiments were performed for 3 times.
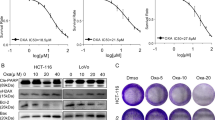
LA induces a much higher ROS in primary human colon or rectal cancer cells than anticancer prooxidants but does not kill them
Because primary cancer cells are different from cancer cell lines, it is necessary to test the effect of anticancer prooxidants and LA on primary cancer cells. The primary human colon cancer cells from a patient were resistant to hydrogen peroxide (Fig. 8). Although LA was obvious the most powerful ROS inducer in the tested compounds, it did not kill cancer cells (Fig. 8). The much weaker ROS-inducers PEITC, PL, ATO (Fig. 8) were highly cytotoxic. The effects of LA, PEITC, PL, hydrogen peroxide and ATO on primary colon or rectal cancer cells from 4 patients were consistent (Fig. 8 & Supplementary Fig. S15). Thus, the results of primary human colon and rectal cancer cells are virtually the same as those of cancer cell lines: while the much stronger ROS inducer LA does not kill the tested primary cancer cells, the much weaker ROS inducer PEITC, PL, or ATO effectively killed them.
LA induces a significantly higher ROS than PL, PEITC and ATO but does not kill primary human colon cancer cells.
(a) Comparison of cellular ROS induced by hydrogen peroxide, LA, PEITC, PL, or ATO. Cells were treated with hydrogen peroxide (100 μM), LA (20 mM), PEITC (10 μM), PL (10 μM), or ATO (10 μM) for 4 hours, followed by cellular ROS measurement, as reflected by DCFH-DA signals. (b) Cells were treated with hydrogen peroxide (100 μM), LA (20 mM), PEITC (10 μM), PL (10 μM), or ATO (10 μM) for 24 hours, subjected for cell counts and death rate calculation. (c) Representative photos of cells 24 hours after treatment. Scale bar = 50 μm. ** p < 0.01, *** p < 0.001.
Concluding remark
Using randomly chosen cancer cells cell lines and primary human colon and rectal cancer cells, we show that there is no evident dose-response relationship between ROS and cell killing or cell growth inhibition. Dose-response relationship is a basic therapeutic principle, which ROS therapeutics also should obey, if ROS is the effecter.
Another important point is the function of LA-induced ROS. In this study, we show that LA is a potent ROS inducer in all the tested cancer cell lines and primary human colon and rectal cancer cells. Previous studies from many laboratories have confirmed that LA is a common environmental factor22 in diverse solid tumors and played multifaceted roles in promoting cancer progression including cancer cell metabolism33,34 and survival24,35, cancer cell chromosomal instability36, tumor angiogenesis22,23 and cancer metastasis37,38. Clinical studies demonstrated that high level of lactate was a strong prognostic indicator of increased metastasis and poor overall survival22,39,40,41,42,43,44. We would ask if there is relationship between LA-induced ROS and the events listed above. Vegran et al suggested that LA-induced ROS may involve in tumor angiogenesis23.
These are the concerns in ROS-based cancer therapy that requires attention.
Methods
Cancer cell lines
Murine breast cancer 4T1 cells, human breast cancer Bcap37 cells, human cervical cancer Hela cells, human liver cancer HepG2 were maintained in complete RPMI-1640 (Life Technologies) with 10% FBS, 100 U/ml penicillin/streptomycin and 2 mM L-glutamine.
Treatment of cancer cells with LA, hydrogen peroxide, L-BSO, PL, PEITC, Dox, or ATO
For cells treated with LA, cells were cultured in medium with LA, which was generated by adding pure lactic acid (Sigma-Aldrich, L1750) to the culture media to final lactate concentrations (2.5–20 mM) as described24. For cells treated with hydrogen peroxide (Sigma-Aldrich, 323381), cells were cultured in the presence of 0.1 mM hydrogen peroxide. For cells treated with Dox and ATO, cells were cultured in medium containing Dox (10 μg/ml), or ATO (10 μM). For cells treated with PL and PEITC, cells were cultured in medium containing 10 μM of PL or PEITC, as described11,14. For cells treated with L-BSO (Sigma-Aldrich, B2515), cells were cultured in medium containing 2.5–100 μM L-BSO.
Cell count
After treatment, cells were observed under microscope every day. After cells were cultured for 24, 48 and 72 hours, we observed that many cells were lysed in the groups treated with PEITC, PL, ATO, or Dox. The viable cells were trypsinized and collected for cell counts using trypan blue exclusion assay.
Primary cancer cells
Human colon or rectal cancer biopsies were obtained from 4 colorectal cancer donors from the oncology department of the Second Affiliated Hospital of Zhejiang University School of Medicine, with patients' consent and approval of the hospital's Ethics Committee. All samples were anonymously coded in accordance with local ethical guidelines (as stipulated by the Declaration of Helsinki). Cancer epithelial cells from surgical specimens were obtained according to the methods as described45,46,47. Briefly, tissue sample was rinsed with PBS for three times. Fat, blood clots and connective tissues were removed from tumor tissues. Tissue sample was cut into small pieces (1-mm3) with scalpels, rinsed with complete DMEM medium twice. 3–5 pieces of tumor tissues were placed into one well of 12-well plate followed by addition of 500 μL complete DMEM medium and incubated in a humidified CO2 incubator at 37°C. When the cells reached 70% confluency, cells were treated with LA (20 mM), PEITC (10 μM), PL (10 μM), ATO (10 μM), or hydrogen peroxide (100 μM). After 4-hour treatment, ROS levels in cells were probed with DCFH-DA. After 24-hour treatment, cell death rate was counted by trypan blue exclusion assay.
ROS measurement
ROS measurement is assayed by dichloro-dihydro-fluorescein diacetate (DCFH-DA, Sigma, D6883), dihydroethidium (DHE, Sigma, D7008), MitoSOX™ Red mitochondrial superoxide indicator (Invitrogen, M36008), 4-amino-5-methylamino-2′,7′-difluorofluorescein (DAF-FM, Sigma, D2321), or hydroxyl radical and peroxynitrite sensor (HPF, Invitrogen, H36004), according to manufactures' instruction. Briefly, cells were loaded with DCFH-DA (final concentration of 10 μM for 30 minutes), DHE (final concentration of 5 μM for 30 minutes), MitoSOX™ Red (final concentration of 2.5 μM for 10 minutes), DAF-FM (final concentration of 10 μM for 30 minutes), or HPF (final concentration of 10 μM for 30 minutes), washed with ice cold HBSS (Hank's Balanced Salt Solution, pH 7.2), then observed under a Zeiss LSM710 laser confocal microscope (Carl Zeiss, Germany) equipped with Zen software to process the image.
Cellular MDA measurement
Cells were incubated with LA (20 mM), L-BSO(20 μM), hydrogen peroxide (100 μM), PEITC (10 μM), PL (10 μM), Dox (10 μg/ml), or ATO (10 μM) for 8 hrs. Cellular MDA were measured according to the previously described method using a kit (Nanjing Jiancheng Bioengineering Institute, Nanjing, China), which is based on the principles in the previous report48. Briefly, MDA reacts with thiobarbituric acid (TBA) at 90–100°C and acidic condition. The reaction yields a pink MDA-TBA conjugate, which was measured at 532 nm using a Multi-Mode Microplate Readers (SpectramMax M5). The cellular MDA was expressed nmole/mg cellular protein.
Measurement of the activities of antioxidant enzymes
Cells were incubated with LA (20 mM), PEITC (10 μM), PL (10 μM), ATO (10 μM), Dox (10 μg/ml), or hydrogen peroxide (100 μM) for 4 hrs and L-BSO(20 μM) for 12 hrs. Cellular extracts were prepared for the detection of total SOD, catalase, GR and GPX, by corresponding kits (Beyotime Institute of Biotechnology, Shanghai, China), which are based on the principles in the previous reports. Briefly, SOD activity was measured according to its ability to inhibit the production of water-soluble formazan dye, as previously described by Sun, Y. et.al.49. The activity of catalase was determined by converting hydrogen peroxide into H2O and O2, as previously described by Goth.50. The activity glutathione peroxidase (GPX) was determined by measuring the rate of oxidation of GSH to GSSG by the dismutation of cumene hydroperoxide (Cum-OOH), which is catalysed by GPX, as described by Flohe, L. et.al.51. Activity of gluathione reductase is measured by rate of the NADPH-dependent reduction of GSSG to GSH, as previously described by Carlberg, I.et.al.52.
Cellular GSH and GSSG measurement
Cells were cultured in the 6-well plate. When the culture reaches 70–80% confluency, cells were treated with L-BSO (20 μM) for 12 hours, or treated with LA (20 mM), hydrogen peroxide (100 μM), PEITC (10 μM), PL (10 μM), Dox (10 μg/ml), or ATO (10 μM) for 4 hours respectively. Cells were rinsed twice with 2 ml ice-cold Ca2+-/Mg2+-free PBS. Cells were collected by tripsinization and lysed in 0.2 ml of ice-cold extraction buffer (0.1% Triton-X and 0.6% sulfosalicylic acid in KPE) followed by 4 cycles of freezing and thawing (1 minute in liquid nitrogen and 2 min in water bath at 37°C). Cell lysate was centrifuged and supernatant was collected for GSH and GSSG measurement according to the method described by Rahman et al.53. The GSH assay is based on the chemical conjugation of GSH with 5,5′-Dithiobis(2-nitrobenzoic acid)[DTNB] (Sigma, D-8130). Total glutathione was measured by firstly reducing oxidized glutathione using glutathione reductase (Sigma, G-3664) and β-NADPH (Sigma, N-7505) followed by conjugation with DTNB. To measure GSSG, GSH was firstly covalently reacted with 2-vinylpyridine (Aldrich, 132292), then GSSG was measured as described above. Pierce® BCA protein assay kit was used for protein determination. All samples were run in triplicates. GSH and GSSG levels were expressed in nmol/mg protein.
Statistics
All data were analyzed using the InStat software (GraphPad, CA, USA) and displayed as mean ± SEM. Two-tailed Student's t-test was used for statistical analysis and significance was defined at ***P < 0.001, **P < 0.01, *P < 0.05.
References
Trachootham, D., Alexandre, J. & Huang, P. Targeting cancer cells by ROS-mediated mechanisms: a radical therapeutic approach? Nat Rev Drug Discov 8, 579–591 (2009).
Cabello, C. M., Bair, W. B., 3rd & Wondrak, G. T. Experimental therapeutics: targeting the redox Achilles heel of cancer. Curr Opin Investig Drugs 8, 1022–1037 (2007).
Engel, R. H. & Evens, A. M. Oxidative stress and apoptosis: a new treatment paradigm in cancer. Front Biosci 11, 300–312 (2006).
Patel, B. P. et al. Lipid peroxidation, total antioxidant status and total thiol levels predict overall survival in patients with oral squamous cell carcinoma. Integr Cancer Ther 6, 365–372 (2007).
Kumar, B., Koul, S., Khandrika, L., Meacham, R. B. & Koul, H. K. Oxidative stress is inherent in prostate cancer cells and is required for aggressive phenotype. Cancer Res 68, 1777–1785 (2008).
Pervaiz, S. & Clement, M. V. Tumor intracellular redox status and drug resistance--serendipity or a causal relationship? Curr Pharm Des 10, 1969–1977 (2004).
Tiligada, E. Chemotherapy: induction of stress responses. Endocr Relat Cancer 13 Suppl 1, S115–124 (2006).
Sullivan, R. & Graham, C. H. Chemosensitization of cancer by nitric oxide. Curr Pharm Des 14, 1113–1123 (2008).
Kong, Q. & Lillehei, K. O. Antioxidant inhibitors for cancer therapy. Med Hypotheses 51, 405–409 (1998).
Kong, Q., Beel, J. A. & Lillehei, K. O. A threshold concept for cancer therapy. in Med Hypotheses. 55, 29–35 (2000).
Raj, L. et al. Selective killing of cancer cells by a small molecule targeting the stress response to ROS. Nature 475, 231–234 (2011).
Adams, D. J. et al. Synthesis, cellular evaluation and mechanism of action of piperlongumine analogs. Proc Natl Acad Sci U S A 109, 15115–15120 (2012).
Adams, D. J. et al. Discovery of small-molecule enhancers of reactive oxygen species that are nontoxic or cause genotype-selective cell death. ACS Chem Biol 8, 923–929 (2013).
Trachootham, D. et al. Selective killing of oncogenically transformed cells through a ROS-mediated mechanism by beta-phenylethyl isothiocyanate. Cancer Cell 10, 241–252 (2006).
Schumacker, P. T. Reactive oxygen species in cancer cells: live by the sword, die by the sword. Cancer Cell 10, 175–176 (2006).
Trachootham, D. et al. Effective elimination of fludarabine-resistant CLL cells by PEITC through a redox-mediated mechanism. Blood 112, 1912–1922 (2008).
Zhang, H. et al. Effective killing of Gleevec-resistant CML cells with T315I mutation by a natural compound PEITC through redox-mediated mechanism. Leukemia 22, 1191–1199 (2008).
Hu, Y. et al. Overcoming resistance to histone deacetylase inhibitors in human leukemia with the redox modulating compound beta-phenylethyl isothiocyanate. Blood 116, 2732–2741 (2010).
Martin-Cordero, C., Leon-Gonzalez, A. J., Calderon-Montano, J. M., Burgos-Moron, E. & Lopez-Lazaro, M. Pro-oxidant natural products as anticancer agents. Curr Drug Targets 13, 1006–1028 (2012).
Gewirtz, D. A. A critical evaluation of the mechanisms of action proposed for the antitumor effects of the anthracycline antibiotics adriamycin and daunorubicin. Biochem Pharmacol 57, 727–741 (1999).
Pelicano, H. et al. Inhibition of mitochondrial respiration: a novel strategy to enhance drug-induced apoptosis in human leukemia cells by a reactive oxygen species-mediated mechanism. J Biol Chem 278, 37832–37839 (2003).
Gatenby, R. A. & Gillies, R. J. Why do cancers have high aerobic glycolysis? Nat Rev Cancer 4, 891–899 (2004).
Vegran, F., Boidot, R., Michiels, C., Sonveaux, P. & Feron, O. Lactate influx through the endothelial cell monocarboxylate transporter MCT1 supports an NF-kappaB/IL-8 pathway that drives tumor angiogenesis. Cancer Res 71, 2550–2560 (2011).
Wu, H. et al. Central role of lactic acidosis in cancer cell resistance to glucose deprivation-induced cell death. J Pathol 227, 189–199 (2012).
Griffith, O. W. Mechanism of action, metabolism and toxicity of buthionine sulfoximine and its higher homologs, potent inhibitors of glutathione synthesis. J Biol Chem 257, 13704–13712 (1982).
Broquist, H. P. Buthionine sulfoximine, an experimental tool to induce glutathione deficiency: elucidation of glutathione and ascorbate in their role as antioxidants. Nutr Rev 50, 110–111 (1992).
Fath, M. A., Ahmad, I. M., Smith, C. J., Spence, J. & Spitz, D. R. Enhancement of carboplatin-mediated lung cancer cell killing by simultaneous disruption of glutathione and thioredoxin metabolism. Clin Cancer Res 17, 6206–6217 (2011).
Miller, A. C., Gafner, J., Clark, E. P. & Samid, D. Posttranscriptional down-regulation of ras oncogene expression by inhibitors of cellular glutathione. Mol Cell Biol 13, 4416–4422 (1993).
Wardman, P. Fluorescent and luminescent probes for measurement of oxidative and nitrosative species in cells and tissues: progress, pitfalls and prospects. Free Radic Biol Med 43, 995–1022 (2007).
Wardman, P. Fluorescent and luminescent probes for measurement of oxidative and nitrosative species in cells and tissues: progress, pitfalls and prospects. Free Radic Biol Med 43, 995–1022 (2007).
Mi, L., Di Pasqua, A. J. & Chung, F. L. Proteins as binding targets of isothiocyanates in cancer prevention. Carcinogenesis 32, 1405–1413 (2011).
Trachootham, D., Alexandre, J. & Huang, P. Targeting cancer cells by ROS-mediated mechanisms: a radical therapeutic approach? Nat Rev Drug Discov 8, 579–591 (2009).
Chen, J. L. et al. The genomic analysis of lactic acidosis and acidosis response in human cancers. PLoS Genet 4, e1000293 (2008).
Sonveaux, P. et al. Targeting lactate-fueled respiration selectively kills hypoxic tumor cells in mice. J Clin Invest 118, 3930–3942 (2008).
Chen, J. L. et al. Lactic acidosis triggers starvation response with paradoxical induction of TXNIP through MondoA. PLoS Genet 6 (2010).
Dai, C., Sun, F., Zhu, C. & Hu, X. Tumor environmental factors glucose deprivation and lactic acidosis induce mitotic chromosomal instability--an implication in aneuploid human tumors. PLoS ONE 8, e63054 (2013).
Silva, A. S., Yunes, J. A., Gillies, R. J. & Gatenby, R. A. The potential role of systemic buffers in reducing intratumoral extracellular pH and acid-mediated invasion. Cancer Res 69, 2677–2684 (2009).
Robey, I. F. et al. Bicarbonate increases tumor pH and inhibits spontaneous metastases. Cancer Res 69, 2260–2268 (2009).
Brizel, D. M. et al. Elevated tumor lactate concentrations predict for an increased risk of metastases in head-and-neck cancer. Int J Radiat Oncol Biol Phys 51, 349–353 (2001).
Schwickert, G., Walenta, S., Sundfor, K., Rofstad, E. K. & Mueller-Klieser, W. Correlation of high lactate levels in human cervical cancer with incidence of metastasis. Cancer Res 55, 4757–4759 (1995).
Walenta, S. et al. High lactate levels predict likelihood of metastases, tumor recurrence and restricted patient survival in human cervical cancers. Cancer Res 60, 916–921 (2000).
Walenta, S. et al. Correlation of high lactate levels in head and neck tumors with incidence of metastasis. Am J Pathol 150, 409–415 (1997).
Yokota, H. et al. Lactate, choline and creatine levels measured by vitro 1H-MRS as prognostic parameters in patients with non-small-cell lung cancer. J Magn Reson Imaging 25, 992–999 (2007).
Paschen, W., Djuricic, B., Mies, G., Schmidt-Kastner, R. & Linn, F. Lactate and pH in the brain: association and dissociation in different pathophysiological states. J Neurochem 48, 154–159 (1987).
Glaysher, S. & Cree, I. A. Isolation and culture of colon cancer cells and cell lines. Methods Mol Biol 731, 135–140 (2011).
Park, J. G., Ku, J. L. & Park, S. Y. Isolation and culture of colon cancer cell lines. Methods Mol Biol 88, 79–92 (2004).
McBain, J. A., Weese, J. L., Meisner, L. F., Wolberg, W. H. & Willson, J. K. Establishment and characterization of human colorectal cancer cell lines. Cancer Res 44, 5813–5821 (1984).
Buege, J. A. & Aust, S. D. Microsomal lipid peroxidation. Method Enzymol 52, 302–310 (1978).
Sun, Y., Oberley, L. W. & Li, Y. A simple method for clinical assay of superoxide dismutase. Clin Chem 34, 497–500 (1988).
Goth, L. A simple method for determination of serum catalase activity and revision of reference range. Clin Chim Acta 196, 143–151 (1991).
Flohe, L. & Gunzler, W. A. Assays of glutathione peroxidase. Method Enzymol 105, 114–121 (1984).
Carlberg, I. & Mannervik, B. Glutathione reductase. Method Enzymol 113, 484–490 (1985).
Rahman, I., Kode, A. & Biswas, S. K. Assay for quantitative determination of glutathione and glutathione disulfide levels using enzymatic recycling method. Nat Protoc 1, 3159–3165 (2006).
Acknowledgements
This work has been supported in part by the China National 973 project (2013CB911303), China Natural Sciences Foundation projects (81071802, 81272456), China National 863 project (2007AA02Z143) and the Fundamental Research Funds for the Central Universities, National Ministry of Education, China, to X Hu.
Author information
Authors and Affiliations
Contributions
X.H. conceived the concept, designed the study and wrote the paper. C.Z., W.H. & H.W. conducted the experiments.
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Electronic supplementary material
Supplementary Information
Supplementary materials
Rights and permissions
This work is licensed under a Creative Commons Attribution-NonCommercial-ShareAlike 3.0 Unported License. The images in this article are included in the article's Creative Commons license, unless indicated otherwise in the image credit; if the image is not included under the Creative Commons license, users will need to obtain permission from the license holder in order to reproduce the image. To view a copy of this license, visit http://creativecommons.org/licenses/by-nc-sa/3.0/
About this article
Cite this article
Zhu, C., Hu, W., Wu, H. et al. No evident dose-response relationship between cellular ROS level and its cytotoxicity – a paradoxical issue in ROS-based cancer therapy. Sci Rep 4, 5029 (2014). https://doi.org/10.1038/srep05029
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/srep05029
This article is cited by
-
Iron-based metal-organic framework co-loaded with buthionine sulfoximine and oxaliplatin for enhanced cancer chemo-ferrotherapy via sustainable glutathione elimination
Journal of Nanobiotechnology (2023)
-
The deubiquitinase USP7 regulates oxidative stress through stabilization of HO-1
Oncogene (2022)
-
1-methylcyclopropene treatment improves postharvest quality and antioxidant activity of Prunus domestica L. cv. Ximei fruit
Horticulture, Environment, and Biotechnology (2022)
-
The role of reactive oxygen species in the immunity induced by nano-pulse stimulation
Scientific Reports (2021)
-
Lactate dehydrogenases amplify reactive oxygen species in cancer cells in response to oxidative stimuli
Signal Transduction and Targeted Therapy (2021)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.