Abstract
As many as half of obsessive-compulsive disorder (OCD) patients treated with an adequate trial of serotonin reuptake inhibitors (SRIs) fail to fully respond to treatment and continue to exhibit significant symptoms. Many studies have assessed the effectiveness of antipsychotic augmentation in SRI-refractory OCD. In this systematic review, we evaluate the efficacy of antipsychotic augmentation in treatment-refractory OCD. The electronic databases of PubMed, PsychINFO (1967–2005), Embase (1974–2000) and the Cochrane Central Register of Controlled Trials (CENTRAL, as of 2005, Issue 3) were searched for relevant double-blind trials using keywords ‘antipsychotic agents’ or ‘neuroleptics’ and ‘obsessive-compulsive disorder’. Search results and analysis were limited to double-blind, randomized control trials involving the adult population. The proportion of subjects designated as treatment responders was defined by a greater than 35% reduction in Yale Brown Obsessive-Compulsive Scale (Y-BOCS) rating during the course of augmentation therapy. Nine studies involving 278 participants were included in the analysis. The meta-analysis of these studies demonstrated a significant absolute risk difference (ARD) in favor of antipsychotic augmentation of 0.22 (95% confidence interval (CI): 0.13, 0.31). The subgroup of OCD patients with comorbid tics have a particularly beneficial response to this intervention, ARD=0.43 (95% CI: 0.19, 0.68). There was also evidence suggesting OCD patients should be treated with at least 3 months of maximal-tolerated therapy of an SRI before initiating antipsychotic augmentation owing to the high rate of treatment response to continued SRI monotherapy (25.6%). Antipsychotic augmentation in SRI-refractory OCD is indicated in patients who have been treated for at least 3 months of maximal-tolerated therapy of an SRI. Unfortunately, only one-third of treatment-refractory OCD patients show a meaningful treatment response to antipsychotic augmentation. There is sufficient evidence in the published literature, demonstrating the efficacy of haloperidol and risperidone, and evidence regarding the efficacy of quetiapine and olanzapine is inconclusive. Patients with comorbid tics are likely to have a differential benefit to antipsychotic augmentation.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout





Similar content being viewed by others
Change history
26 July 2006
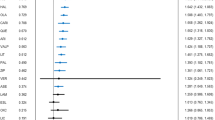
Correction to: Molecular Psychiatry (2006) 11, 622–632. doi: 10.1038/sj.mp.4001823 Following publication of the above article, the authors noted the following: while the captions for Figures 4 and 5 were correct, the actual figures themselves were incorrectly transposed. They appear correctly below:
References
Coryell W . Obsessive-compulsive disorder and primary unipolar depression: Comparison of background, family history, course, and mortality. Journal of Nervous and Mental Disease 1981; 164: 220–224.
Hollander E, Greenwald S, Nerville D, Johnson J, Hornig CD, Weissman MM . Uncomplicated and comorbid obsessive-compulsive disorder in an epidemiologic sample. Depress Anxiety 1996/1997; 4: 111–119.
Koran LM, Thienemann ML, Davenport R . Quality of life for patients with obsessive-compulsive disorder. Am J Psychitry 1996; 153: 783–788.
Karno M, Golding JM, Sorenson SB, Burnam MA . The epidemiology of obsessive-compulsive disorder in five US communities. Arch Gen Psychiatry 1988; 45: 1094–1099.
Kessler RC, McGonagle KA, Zhao S, Hughes M, Swartz M, Blazer DG . Lifetime and 12-month prevalence of DSM-III-R psychiatric disorders in the United States. Arch Gen Psychiatry 1994; 51: 8–19.
Rasmussen SA, Eisen JL . Epidemiology and differential diagnosis of obsessive compulsive disorder. J Clin Psychiatry 1994; 55: 5–14.
Sasson Y, Zohar J, Chopra M, Lustig M, Iancu I, Hendler T . Epidemiology of obsessive-compulsive disorder: a world view. J Clin Psychiatry 1997; 58: 7–10.
Murray CJ, Lopez AD . The Global Burden of Disease: a Comprehensive Assessment of Mortality and Morbidity from Diseases, Injuries, and Risk Factors in 1990 and Projected to 2020. Cambridge, Mass.: Harvard University Press, 1996.
Clomipramine Collaborative Study Group. Clomipramine in the treatment of patients with obsessive-compulsive disorder. Arch Gen Psychiatry 1991; 48: 730–738.
Goodman WK, Price LH, Rasmussen SA, Delgado PL, Heninger GR, Charney DS . Efficacy of fluvoxamine in obsessive-compulsive disorder: a double-blind comparison with placebo. Arch Gen Psychiatry 1989; 46: 36–43.
Skoog G, Skoog I . A 40-year follow-up of patients with obsessive-compulsive disorder. Arch Gen Psychiatry 1999; 56: 121–127.
Berrios GE, Chiu H . Obsessive-compulsive disorders in Cambridgeshire: a follow-up study of up to 20 years. Br J Psychiatry 1989; 154 (suppl 4): 17–20.
Delkeskamp H . Langstrecken-Katamnesen von Zwangsneurose. Acta Psychiatr Scand 1965; 41: 565–581.
Goodwin DW, Guze SB, Robins E . Follow-up studies in obsessional neurosis. Arch Gen Psychiatry 1969; 20: 182–187.
Kringlen E . Obsessional neurotics: a long-term follow-up. Br J Psychiatry 1965; 111: 709–722.
Muller C . Vorlaufige Mitteilung zur langen Katamnese der Zwangskranken. Nervenartz 1953; 24: 112–115.
Rennie TAC . Prognosis in the Psychoneurosis: Benign and Malignant Developments, Current Problems in Psychiatric Diagnosis. New York: Grune & Stratton Inc, 1953.
Rudin E . Beitrag zur Frage der Zwangskrankheit, insbesondere ihrer hereditaren Beziehungen. Arch Psychiatr Nervenkrankh 1953; 191: 14–54.
Expert Consensus Panel for Obsessive-Compulsive Disorder. Treatment of obsessive-compulsive disorder. J Clin Psychiatry 1997; 58 (suppl 4): 2–72.
Goodman WK . Obsessive-compulsive disorder: diagnosis and treatment. J Clin Psychiatry 1999; 60 (suppl 18): 27–32.
McDonough M, Kennedy N . Pharmacological management of obsessive-compulsive disorder: a review for clinicians. Harvard Rev Psychiatry 2002; 10: 127–137.
Alacron RD, Libb JW, Spitler D . A predictive study of obsessive compulsive response to clomipramine. J Clin Psychopharmacol 1993; 13: 210–213.
Erzegovesi S, Cavellini MC, Cavedini P, Diaferia G, Locatelli M, Bellodi L . Clinical predictors of drug response in obsessive-compulsive disorder. J Clin Psychopharmacol 2001; 21: 272–275.
Ravizza L, Barzega G, Bellino S, Bogetto F, Maina G . Predictors of drug treatment response in obsessive-compulsive disorder. J Clin Psychiatry 1995; 56: 368–373.
Goodman WK, McDougle CJ, Barr LC, Aronson SC, Price LH . Biological approaches to treatment-resistant obsessive compulsive disorder. J Clin Psychiatry 1993; 54 (suppl 6): 16–26.
Wheadon DE, Bushnell WD, Steiner M . A fixed-dose comparison of 20, 40 or 60 mg paroxetine or placebo in the treatment of obsessive-compulsive disorder. Presented at the 32nd annual meeting of the American College of Neuropsychopharmacology Dec. 13–17, 1993.
McDougle CJ, Price LH, Goodman WK, Charney DS, Heninger GR . A controlled trial of lithium augmentation in fluvoxamine-refractory obsessive compulsive disorder: lack of efficacy. J Clin Psychopharmacol 1991; 11: 175–184.
Pigott TA, L'Heureux F, Hill JL, Bihari K, Bernstein SE, Murphy DL . A double-blind study of adjuvant buspirone hydrochloride in clomipramine-treated patients with obsessive-compulsive disorder. J Clin Psychopharmacol 1992; 12: 11–18.
Jacobsen FM . Risperidone in the treatment of affective illness and obsessive-compulsive disorder. J Clin Psychiatry 1995; 56: 423–429.
McDougle CJ, Goodman WK, Price LH, Delgado PL, Krystal JH, Charney DS et al. Neuroleptic addition in fluvoxamine-refractory obsessive compulsive disorder. Am J Psychiatry 1990; 147: 652–654.
McDougle CJ, Fleishmann RL, Epperson CN, Wasylink S, Leckman JF, Price LH . Risperidone addition in fluvoxamine-refractory obsessive-compulsive disorder: three cases. J Clin Psychiatry 1995; 56 (suppl 11): 526–528.
Stein DJ, Bouwer C, Hawkridge S, Emsley RA . Risperidone augmentation of serotonin reuptake inhibitors in obsessive-compulsive disorder. J Clin Psychiatry 1997; 58 (suppl 3): 119–122.
Pallantini S, Hollander E, Bienstock C, Koran L, Leckman J, Marazziti D et al. Treatment non-response in OCD: methodological issues and operational definitions. International Journal of Neuropsychopharmacology 1997; 5: 181–191.
Mulrow CD, Oxman AD . Cochrane Collaboration Handbook. Oxford: Update Software, 1997.
Moncrieff J, Churchill R, Drummond C, McGuire H . Development of a quality assessment instrument for trials of treatments for depression and neurosis. International Journal of Methods in Psychiatric Research 2001; 10 (3): 126–133.
Egger M, Davey G, Schneider M, Minder C . Bias in meta-analysis detected by a simple, graphical test. BMJ 1997; 315: 629–634.
Deeks J, Higgins J, Altman D . Cochrane Reviewers' Handbook 4.2.1. In: Alderson P, Green S, Higgins J (eds). The Cochrane Library. Chichester: John Wiley & Sons, Ltd, 2003.
Bystritsky A, Ackerman DL, Rosen RM, Vapnik T, Gorbis E, Maidment KM et al. Olanzapine augmentation of serotonin reuptake Inhibitors in refractory obsessive-compulsive disorder using adjunctive olanzapine: a placebo-controlled trial. J Clin Psychiatry 2004; 65: 565–568.
Carey PD, Vythilingum B, Seedat S, Muller JE, van Amerigen M, Stein DJ . Quetiapine augmentation of SRIs in treatment refractory obsessive-compulsive disorder: a double-blind, randomised, placebo-controlled sudy. BMC Psychiatry 2005; 5: 5.
Denys D, de Geus F, van Megen HJGM, Wstenberg HGM . A double-blind, randomized, placebo-controlled trial of quetiapine addition in patients with obsessive-compulsive disorder refractory to serotonin reuptake inhibitors. J Clin Psychiatry 2004; 65: 1040–1048.
Erzegovesi S, Guglielimo E, Siliprandi F, Bellodi L . Low-dose risperidone augmentation of fluvoxamine treatment in obsessive-compulsive disorder: a double-blind, placebo-controlled study. European Neuropsychopharmacology 2005; 15: 69–74.
Fineberg NA, Sivakumaran T, Roberts A, Gale T . Adding quetiapine to SRI in treatment-resistant obsessive-compulsive disorder: a randomized controlled treatment study. International Clinical Psychopharmacology 2005; 20: 223–226.
Hollander E, Rossi NB, Sood E, Pallanti S . Risperidone augmentation in treatment-resistant obsessive-compulsive disorder: a double-blind, placebo-controlled study. International Journal of Neuropsychopharmacology 2003; 6: 397–401.
McDougle CJ, Goodman WK, Leckman JF, Lee NC, Heninger GR, Price LH . Haloperidol addition in fluvoxamine-refractory obsessive-compulsive disorder: A double-blind, placebo-controlled study in patients with and without tics. Arch Gen Psychiatry 1994; 51: 302–308.
McDougle CJ, Epperson CN, Pelton GH, Wasylink S, Price LH . A double-blind, placebo-controlled study of risperidone addition in serotonin reuptake inhibitor-refractory obsessive-compulsive disorder. Arch Gen Psychiatry 2000; 57: 794–801.
Shapira NA, Ward HE, Mandoki M, Murphy TK, Yang MCK, Blier P et al. A double-blind, placebo-controlled trial of olanzapine addition in fluoxetine-refractory obsessive-compulsive disorder. Biol Psychiatry 2004; 550: 553–555.
Li X, May RS, Tolbert LC, Jackson WT, Flournoy JM, Baxter LR . Risperidone and Haloperidol Augmentation of Serotonin Reuptake Inhibitors in Refractory Obsessive-Compulsive Disorder: A crossover study. J Clin Psychiatry 2005; 66: 736–743.
Scahill L, Leckman JF, Schultz RT, Katsovich L, Peterson BS . A placebo-controlled trial of risperidone in Tourette syndrome. Neurology 2003; 60: 1130–1135.
Shapiro E, Shapiro AK, Fulop G, Hubbard M, Mandeli J, Nordlie J et al. Controlled study of haloperidol, pimozide and placebo for the treatment of Gilles de la Tourette's syndrome. Arch Gen Psychiatry 1989; 46: 722–730.
Acknowledgements
We thank Bryann Baker BA, Alexander Bystritsky MD, Paul Carey MD, Damiaan Denys MD, Stefano Erzegovesi MD, Naomi Fineberg MD, Eric Hollander MD, Nathan Shapira MD and Thanusha Sivakumaran BA for conducting data analysis and answering questions related to their respective studies and to Christopher McDougle MD for leaving the individual patient data necessary to conduct this meta-analysis within his manuscript. Without their generosity and openness with regard to their study data and spirit of collegiality, this analysis would not have been possible. Dr Michael Bloch was supported through a Tourette Syndrome Association Research Award, the NIH Loan Repayment Program and an institutional NIMH T32 training grant.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Bloch, M., Landeros-Weisenberger, A., Kelmendi, B. et al. A systematic review: antipsychotic augmentation with treatment refractory obsessive-compulsive disorder. Mol Psychiatry 11, 622–632 (2006). https://doi.org/10.1038/sj.mp.4001823
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.mp.4001823
Keywords
This article is cited by
-
The Sapap3−/− mouse reconsidered as a comorbid model expressing a spectrum of pathological repetitive behaviours
Translational Psychiatry (2023)
-
A biophysical model for dopamine modulating working memory through reward system in obsessive–compulsive disorder
Cognitive Neurodynamics (2023)
-
Obsessive–Compulsive Disorder and Tourette’s Disorder Symptom Presentations: Differential Diagnosis and Treatment Considerations
Current Developmental Disorders Reports (2023)
-
Granisetron-mediated augmentation of sertraline therapeutic effect in obsessive-compulsive disorder: a double-blind placebo-controlled, randomized clinical trial
BMC Pharmacology and Toxicology (2022)
-
Developmental impact of glutamate transporter overexpression on dopaminergic neuron activity and stereotypic behavior
Molecular Psychiatry (2022)