Abstract
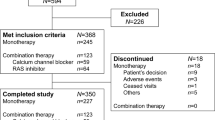
This randomised, double-blind study was designed to investigate the efficacy of a once-daily (OD) combination of the AT1 receptor blocker, eprosartan 600 mg, and the thiazide diuretic, hydrochlorothiazide (HCTZ) 12.5 mg, in patients with mild to moderate hypertension (sitting diastolic blood pressure (sitDBP) ⩾98 mm Hg and ⩽114 mm Hg) not adequately controlled with eprosartan 600 mg OD. A total of 494 patients entered the open-label monotherapy run-in phase, which consisted of eprosartan 600 mg OD for 3 weeks. Patients who responded to monotherapy were not eligible to enter the randomised phase of the study and were withdrawn. The remaining 309 patients were then randomised to either eprosartan 600 mg plus HCTZ 12.5 mg OD or to continue on eprosartan 600 mg OD. In the eprosartan plus HCTZ combination group, both sitDBP and sitting systolic blood pressure (sitSBP) were significantly reduced compared with the eprosartan monotherapy group. In addition, the response rate was higher in the combination group compared with the monotherapy group. There were no significant effects on reduction of sitDBP due to gender, prior use of antihypertensives or baseline severity of hypertension. The tolerability profile for the combination group was similar to that for the monotherapy group. Headache was the most frequent adverse event in both treatment groups. The majority of adverse events were mild to moderate in intensity. In this study of patients who were unresponsive to eprosartan monotherapy for 3 weeks, a combination product of eprosartan 600 mg and HCTZ 12.5 mg was shown to be an effective and well tolerated treatment.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 digital issues and online access to articles
$119.00 per year
only $9.92 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
References
Materson BJ, Preston RA . Angiotensin-converting enzyme inhibitors in hypertension: a dozen years of experience Arch Intern Med 1994 154: 513–523
Hedner T et al. Dyspnoea, asthma, and bronchospasm in relation to treatment with angiotensin converting enzyme inhibitors BMJ 1992 304: 941–946
Nishimura H et al. Angiotensin converting enzyme and chymase in cardiovascular tissues Kidney Int 1996 49: S18–S23
Gradman AH et al. Assessment of once-daily eprosartan, an angiotensin II antagonist, inpatients with systemic hypertension Clin Therapeut 1999 21: 442–453
Hedner T, Himmelmann A for the Eprosartan Multinational Study Group. The efficacy and tolerance of one and two daily doses of eprosartan in essential hypertension J Hypertens 1999 17: 129–136
Sega R et al. Efficacy and safety of eprosartan in severe hypertension Blood Press 1999 8: 114–121
Gavras I, Gavras H . Effects of eprosartan versus enalapril in hypertensivepatients on the renin-angiotensin-aldosterone system and safety parameters: results from a 26-week, double-blind, multicentre study Curr Med Res Opin 1999 15: 15–24
Weber M . Clinical efficacy of eprosartan Pharmacotherapy 1999 19: 95S–101S
Neutel JM, Black HR, Weber MA . Combination therapy with diuretics: an evolution of understanding Am J Med 1996 101: 61S–70S
McVeigh GE, Flack J, Grimm R . Goals of antihypertensive therapy Drugs 1995 49: 161–175
Plat F, Saini R . Management of hypertension – the role of combination therapy Am J Hypertens 1997 10: 262S–271S
Langtry H, McClellan K . Valsartan/hydrochloro-thiazide Drugs 1999 57: 751–758
Elliott WJ . Double-blind comparison of eprosartan and enalapril on cough and blood pressure in unselected hypertensivepatients J Hum Hypertens 1999 13: 413–417
Levine B . Eprosartan provides safe and long-term maintenance of blood pressure control inpatients with mild to moderate hypertension Curr Med Res Opin 2001 17: 8–17
Hedner T . Long-term safety and tolerability of once-daily eprosartan inpatients with essential hypertension In preparation
Mackay JH et al. Losartan and low dose hydrochlorothiazide inpatients with essential hypertension Arch Intern Med 1996 156: 278–285
Chrysant SG, Wombolt DG, Feliciano N, Zheng H . Long-term efficacy, safety, and tolerability of valsartan and hydrochlorothiazide inpatients with essential hypertension Curr Ther Res 1998 59: 762–771
Alper AB Jr, Calhoun . Contemporary management of refractory hypertension Curr Hypertens Rep 1999 1: 402–407
Acknowledgements
This trial was performed at the following centres:
Belgium: Creytens GJJ, Dufour AGR, Borschette C, Narcisse D, Kivits A, van Esch C.
France: Farhaf S, Pithon M, Gabriello JL, Willman J-F, Mascherpa E, Fonteny R, Blaignan J, Giner M, Lalanue G, Voiriot P, Letzelter J-M, Sicard J, Campagne A, Cadinot D, Etchegaray G, Boye A, Lejay D, Boucher L.
Ireland: Bradbury FN, Forde D, McGarry P, Sullivan J, Belton M, O'Doherty BP.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Sachse, A., Verboom, C. & Jäger, B. Efficacy of eprosartan in combination with HCTZ in patients with essential hypertension. J Hum Hypertens 16, 169–176 (2002). https://doi.org/10.1038/sj.jhh.1001317
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.jhh.1001317
Keywords
This article is cited by
-
Combining angiotensin receptor blockers with chlorthalidone or hydrochlorothiazide – which is the better alternative? A meta-analysis
Systematic Reviews (2020)
-
The Comparative Efficacy and Safety of the Angiotensin Receptor Blockers in the Management of Hypertension and Other Cardiovascular Diseases
Drug Safety (2015)
-
Ambulatory monitoring of systolic hypertension in the elderly: Eprosartan/hydrochlorothiazide compared with losartan/hydrochlorothiazide (INSIST trial)
Advances in Therapy (2010)
-
Hypertension in patients with type-II diabetes: relation to urinary albumin excretion, endothelial function and inflammation
Journal of Human Hypertension (2005)
-
Once-daily eprosartan mesylate in the treatment of elderly patients with isolated systolic hypertension: data from a 13-week double-blind, placebo-controlled, parallel, multicenter study
Journal of Human Hypertension (2004)