Abstract
Recent studies have suggested that 5-aminosalicylic acid (5-ASA) inhibits colorectal cancer (CRC) development. However, the mechanism underlying the antineoplastic effect of 5-ASA remains unknown. We here examined the effect of 5-ASA on epidermal growth factor receptor (EGFR) activation, a pathway that triggers mitogenic signals in CRC cells. We show that 5-ASA inhibits EGFR activation, through a mechanism that does not rely on CRC cell death induction. 5-ASA enhances the activity, but not expression, of phosphorylated (p)-EGFR-targeting phosphatases (PTPs), and treatment of cells with PTP inhibitors abrogates the 5-ASA-mediated EGFR dephosphorylation. Both SH-PTP1 and SH-PTP2 interact with EGFR upon 5-ASA treatment. However, knockdown of SH-PTP2 but not SH-PTP1 by small interference RNAs prevents the 5-ASA-induced EGFR dephosphorylation. Finally, we show that 5-ASA attenuates p-EGFR in ex vivo organ cultures of CRC explants. Data indicate that 5-ASA disrupts EGFR signalling by enhancing SH-PTP2 activity, and suggest a mechanism by which 5-ASA interferes with CRC growth.
Similar content being viewed by others
Introduction
Despite considerable advance in our understanding of colorectal cancer (CRC) pathogenesis, the overall incidence of this neoplasia is yet increasing. Moreover, CRC is the second most common fatal malignancy in Western world, due to the lack of effective treatment of advanced disease.1 The development of new preventive therapies is thus worth pursuing.
CRC often develops in a stepwise fashion from normal mucosa to adenomatous polyps to carcinoma, a complex and multistage process involving specific gene alterations and environmental insults that ultimately affect cell proliferation and death of intestinal epithelial cells.2 Several lines of epidemiological and experimental investigation have shown that regular intake of nonsteroidal anti-inflammatory drugs (NSAIDs) is effective in the chemoprevention of CRC in the general population.3, 4, 5 Unfortunately, the widespread use of NSAIDs in the chemoprevention of CRC has been limited by their frequent and often severe side effects.6, 7, 8
Epidermal growth factor receptor (EGFR) is thought to play a key role in the pathogenesis or maintenance of a number of human cancers of epithelial origin, including CRC.9 This supposition is based on the demonstration that EGFR itself is overexpressed in CRC cells and that within the neoplastic microenvironment there is secretion of factors that activate EGFR in an autocrine/paracrine manner.10, 11 Evidence also indicates that the aberrant activation of EGFR contributes to sustain the growth of CRC cells.12 Indeed, EGFR expression seems to represent an independent predictor of decreased survival in CRC patients. Consistent with this, the EGFR has become a biochemical target for chemoprevention and chemotherapeutic agents against CRC.11, 13, 14
The clinically well-characterised 5-aminosalicylic acid (5-ASA) or mesalazine is the drug of choice in the maintenance of remission, and treatment of mild flare-ups of inflammatory bowel disease (IBD). 5-ASA has been proven to be safe and free of serious adverse effects. In recent years, evidence has also been provided to suggest that long-term consumption of 5-ASA reduces the rates of CRC developing in patients with ulcerative colitis.15, 16 Moreover, studies both in vitro and animal models of carcinogenesis have shown that 5-ASA negatively regulates the growth of CRC cells,17, 18, 19, 20 further supporting the antineoplastic properties of this drug. The molecular mechanism by which 5-ASA exerts the antiproliferative effect on CRC cells remains however unknown.
In the present study, we have examined whether 5-ASA directly regulates the activation of EGFR in CRC cell lines and human CRC explants, and explored the molecular mechanism by which 5-ASA controls EGFR activation.
Results
5-ASA inhibits the activation of EGFR in colon cancer cells
To examine the effect of 5-ASA on the constitutive level of p-EGFR, we used four different CRC cell lines (i.e. HT-29, HT-115, T84 and Caco-2), which express high levels of p-EGFR. To this end, CRC cell lines were either left untreated or treated with physiological doses of 5-ASA, and then p-EGFR assessed by Western blotting. Immunoblot analysis of lysates of CRC cells showed a dramatic reduction in the constitutive level of p-EGFR after culture with physiological concentrations of 5-ASA (Figure 1a),21, 22 and this was evident in each of the four CRC cell lines used (not shown).
5-ASA dose-dependently inhibits the phosphorylation of epidermal growth factor receptor (p-EGFR) in HT-29 cell lines. HT-29 cells were starved overnight and then cultured in Mc Coy's medium containing no FBS in the absence (uns=unstimulated) or presence of increasing concentrations of 5-ASA or mannitol for 6 h. After analysis of p-EGFR, blot was stripped and incubated with an antibody recognizing total EGFR. One of eight representative experiments, in which similar results were obtained, is shown. (b) The inhibitory effect of 5-ASA on p-EGFR is reversible. HT-29 cells were cultured with or without graded doses of 5-ASA for 6 h (1st culture), then extensively washed and cultured with Mc Coy's medium containing 10% FBS for additional 16 h (2nd culture). Both p- and total EGFR were assessed by Western blotting. One of four representative experiments, in which similar results were obtained, is shown. (c–d) 5-ASA does not enhance HT-29 cell death. HT-29 cells were cultured in Mc Coy's medium containing no FBS in the absence (unstimulated) or presence of 50 mM 5-ASA. After 6 h cells were recovered and the percentage of AV and/or PI positive cells assessed by flow cytometry. One of four representative experiments is shown. (d)The content of cytoplasmic histone-associated-DNA-fragments in HT-29 cells cultured with the indicated compounds for 6 h. As a positive control, HT-29 were treated with staurosporin (500 ng/ml). Data are expressed in densitometric arbitrary units (a.u.) and indicate mean±S.D. of four separate experiments
We then attempted to dissect the mechanism by which 5-ASA interferes with p-EGFR. First, we showed no change in p-EGFR in cells treated with equivalent concentrations of mannitol (Figure 1a) or butyric acid (not shown), suggesting that the 5-ASA-mediated EGFR dephosphorylation is due to neither osmotic nor pH shifts in the culture medium. Data in Figure 1b also show that the effect of 5-ASA on p-EGFR was reversible. Indeed, 5-ASA-treated cells recovered the p-EGFR expression upon removal of the drug. Such experiments were carried out in parallel to those depicted in Figure 1a in order to prove that 5-ASA inhibits p-EGFR when maintained in the culture medium. Moreover, flow cytometry analysis revealed that 5-ASA did not change the percentage of annexin V (AV)/propidium iodide (PI) positive cells (11±4.5% in 5-ASA-treated cells versus 10±3.9% in unstimulated cells) within the timeframe of p-EGFR analysis (Figure 1c). A similar finding was seen when analysis of cell apoptosis was assessed by a colorimetric kit (Figure 1d), thus indicating that the dephosphorylation of EGFR by 5-ASA does not rely on induction of cell death.
Finally, no change in the expression of the extracellular EGFR was seen after 5-ASA exposure (not shown), thus excluding the possibility that the reduced content of p-EGFR in 5-ASA-treated cells was due to a shedding of the receptor.
We also evaluated whether 5-ASA negatively regulates the activation of EGFR induced by EGF. For this purpose, CRC cells were cultured in the absence of serum for 12 h, in order to reduce the basal level of p-EGFR, then treated with 5-ASA for different time points followed by various concentrations of exogenous EGF for 10 min. As expected, EGF dose-dependently enhanced p-EGFR (Figure 2a). However, preincubation of cells with 5-ASA largely reduced the EGF-induced p-EGFR expression, at all applied EGF concentrations (Figure 2a). Importantly, the inhibitory effect of 5-ASA was also confirmed when the overall level of p-EGFR was analyzed (Figure 2b). Time course studies revealed that the inhibition of EGF-induced p-EGFR in 5-ASA-treated cells occurred as early as 1 h after 5-ASA preincubation (Figure 2c). In contrast, no inhibition in EGF-induced p-EGFR was seen in cells preincubated with mannitol or butyric acid (Figure 2d).
5-ASA inhibits EGF-induced EGFR activation. (a) Representative expression of phosphorylated-EGFR (p-EGFR) (upper blot) and total EGFR (lower blot) protein in HT-29 cells cultured in the presence or absence of 50 mM 5-ASA for 4 h and then treated or not with various concentrations of EGF for 10 min. p-EGFR was examined by Western blotting using an antibody that recognizes phosphorylation of EGFR on tyrosine residue 1173. One of three representative blots is shown. Note that the level of p-EGFR in unstimulated cells is lower than that shown in the first lane of the Figure 1a. This is due to the fact that the amount of total proteins used in the present experiment was lower than that in the experiment depicted in Figure 1a. (b) Total extracts of HT-29 cells cultured with or without the initial addition of 50 mM 5-ASA for 4 h followed by EGF (200 ng/ml) for 10 min were immunoprecipitated using a monoclonal anti-human EGFR antibody and then incubated with a p-Tyr antibody. No band was seen when proteins were immunoprecipitated using a control isotype antibody (ve−). After detection of p-EGFR, bots were stripped and incubated with a second anti-EGFR to ascertain equivalent loading of the lanes (lower blot). (c) Effect of 50 mM 5-ASA preincubated for the indicated time points on the expression of p-EGFR induced in HT-29 cells by 10 min stimulation with EGF (200 ng/ml) is shown. One of three representative experiments, in which p-EGFR was assessed as indicated in the (a), is shown. (d) Effect of mannitol or butyric acid on the EGF-induced p-EGFR expression in HT-29 cells. Cells were preincubated with 50 mM mannitol or 400 μM butyric acid for 4 h then stimulated with EGF (200 ng/ml) for 10 min. One of three representative Western blots is shown. (e–f) 5-ASA inhibits HT-29 cell proliferation induced by EGF or FGF or FBS. HT-29 cells were cultured in the presence or absence of EGF (200 ng/ml), FGF (100 ng/ml) or FBS (10%) with or without the initial addition of 50 mM 5-ASA. EGF, FGF and FBS significantly enhance HT-29 cell growth (P=0.02), but the proliferative effect exerted by each of these reagent is inhibited by 5-ASA (P<0.01). Data are expressed in arbitrary units and indicate mean±S.D. of four separate experiments
To confirm the functional relevance of these findings, we examined whether 5-ASA blocks CRC cell proliferation induced by exogenous EGF. EGF enhanced HT-29 cell growth, but this effect was significantly inhibited by 5-ASA (Figure 2e) (P<0.01). Similar findings were seen when 5-ASA was added to cultures of HT-115, T84 or Caco-2 cells (not shown). The fact that inhibition of p-EGFR occurred in a very short time after 5-ASA treatment (i.e. 1 h) and was also maintained in CRC cell cultures to which exogenous EGF was added, would suggest that the 5-ASA-mediated inhibition of EGFR activation is not due to a reduced synthesis of EGFR ligands, such as EGF. The demonstration that the level of p-EGFR was higher in cells cultured with 50 mM 5-ASA and 200 ng/ml EGF than in unstimulated cells, whereas the result of proliferation was inverted (Figure 2, panels A, C, E) prompted us to explore the possibility that 5-ASA may negatively regulate additional pathways, which eventually sustain CRC cell growth. To this end, we analyzed the effect of 5-ASA on HT-29 cell growth induced by basic fibroblast growth factor (FGF) or fetal bovine serum (FBS). As expected both FGF and FBS enhanced HT-29 cell growth, but this effect was inhibited by 5-ASA (Figure 2f).
5-ASA enhances PTP activity in colon cancer cells
EGFR phosphorylation is a tightly controlled phenomenon being the net result of the action of the tyrosine kinase and PTPs.23 Therefore, we then examined whether the 5-ASA-mediated inhibition of p-EGFR reflected changes in the expression/activity of PTPs, which have been reported to control the extent of EGFR activation. To this end, we first evaluated the PTPs activity in total extracts from CRC cells using a synthetic phosphorylated EGFR peptide as a substrate. Data depicted in Figure 3a indicate that treatment of HT-29 cells with 5-ASA resulted in a significant increase in the activity of p-EGFR-targeting PTPs in comparison to untreated cells, regardless of whether cells were stimulated or not with EGF (P=0.01). The addition of Na3VO4 to proteins extracted from 5-ASA-treated EGF-stimulated cells significantly reduced the p-EGFR-targeting PTP(s) activity (P=0.03). In contrast, exposure of CRC cells to 5-ASA resulted in no increase in the general PTPs activity (Figure 3b). In the light of these observations, we then examined whether the inhibitory effect of 5-ASA on p-EGFR could be prevented by treatment of CRC cells with PTPs inhibitors. Preincubation of cells with Na3VO4 largely reduced the inhibitory effect of 5-ASA on EGF-induced p-EGFR (Figure 3c). As Na3VO4 is quickly inactivated once inside the cell, we also carried out experiments in which CRC cells were preincubated with iodoacetamide, an irreversible PTP inhibitor,24 prior to adding 5-ASA. Iodoacetamide completely blocked the ability of 5-ASA to dephosphorylate EGFR (Figure 3d). These findings were also seen when experiments were carried out using HT-115, T84 and Caco-2 (not shown).
5-ASA enhances the activity of p-EGFR-targeting (a) but not general (b) PTPs. HT-29 cells were cultured with or without the initial addition of 50 mM 5-ASA for 4 h and then stimulated with 200 ng/ml EGF for 10 min. At the end, total extracts were prepared and incubated with a synthetic p-EGFR peptide (a) or 4-nitrophenyl phosphate (b). 5-ASA significantly enhances p-EGFR targeting PTP activity regardless of whether cells are treated or not with EGF (P=0.01). In vitro incubation of proteins extracted from 5-ASA-treated EGF-stimulated cells with Na3VO4 significantly reduces PTP activity (P=0.03). (c, d) The addition of general PTPs inhibitors Na3VO4 (c) or iodoacetamide (d) to HT-29 cell cultures reduces the 5-ASA-mediated EGFR dephosphorylation. Cells were cultured with or without the initial addition of Na3VO4 (100 μM) or iodoacetamide (250 μM) for 30 min prior to adding 50 mM 5-ASA. After 4 h culture, cells were stimulated with 200 ng/ml EGF for 10 min. At the end, total extracts were prepared and the expression of EGFR assessed by Western blotting. Blots are representative of four experiments in which similar results were obtained
5-ASA does not alter the global expression of PTPs but enhances the interaction of SH-PTP1 and SH-PTP2 with EGFR
The data described above prompted us to investigate the PTP(s) implicated in the 5-ASA-mediated EGFR dephosphorylation. To address this issue, we first looked at the expression of several PTPs, which have been reported to control the strength of EGFR signaling.23 For this purpose, protein extracts from CRC cells cultured in the presence or absence of 5-ASA were analyzed for the content of SH-PTP1, SH-PTP2, PTP1β, RPTPα, LAR and PEST by Western blotting. As shown in Figure 4, 5-ASA did not alter the expression of any PTP regardless of whether HT-29 cells were either left untreated or treated with EGF.
5-ASA does not enhance the expression of p-EGFR-targeting PTPs. HT-29 cells were cultured with or without 50 mM 5-ASA for the indicated time points (a). In addition, HT-29 cells were cultured with or without the initial addition of 50 mM 5-ASA for 4 h and then stimulated with 200 ng/ml EGF for 10 min (b). The indicated PTPs were evaluated by Western blotting. Blots in (a) and (b) are representative of three separate experiments in which similar results were obtained
As PTPs selectively couple to EGFR in the course of the dephosphorylation reaction,23 we then examined whether 5-ASA enhances the interaction of specific PTP(s) with EGFR. For this purpose, EGFR immunoprecipitates from EGF-stimulated CRC cell cultures preincubated with medium or 5-ASA were blotted onto a nitrocellulose membrane and screened for interaction between EGFR and PTPs. By using this procedure, we showed that 5-ASA enhanced the association of both SH-PTP1 and SH-PTP2 with EGFR (Figure 5a). In contrast, immunoreactivity corresponding to the interaction between EGFR and PEST was evident at the same level in cells cultured with or without 5-ASA. No association between EGFR and any of the remaining PTPs investigated was induced by 5-ASA (Figure 5a, left panels). At the end, blots were stripped an incubated with a second EGFR antibody to confirm the nature of immunoprecipitates (Figure 5a, right panels, lower blot). To prove that SH-PTP1 and SH-PTP2 interact with EGFR upon 5-ASA treatment, EGFR immunoprecipitates from EGF-stimulated CRC cells cultured with or without the addition of 5-ASA were separated on a SDS gel and incubated with a specific monoclonal anti-human SH-PTP1 or SH-PTP2 antibody. Data in Figure 5b show that 5-ASA stably enhanced the interaction of both these PTPs with EGFR. No PTP band was detectable when immunoprecipitation was carried out with isotype-matched IgG (ve−), confirming the specificity of the assay (Figure 5b).
5-ASA enhances the interaction of both SH-PTP1 and SH-PTP2 with EGFR. (a) Total extracts of HT-29 cells cultured with or without the initial addition of 50 mM 5-ASA for 4 h followed by EGF (200 ng/ml) for 10 min were immunoprecipitated using a monoclonal anti-human EGFR antibody and dot-blotted on nitrocellulose, then incubated with the indicated PTPs and EGFR antibodies. (b) HT-29 cells were cultured with or without 50 mM 5-ASA for 1–4 h followed by EGF (200 ng/ml) for 10 min. Total extracts were then immunoprecipitated using a monoclonal ant-human EGFR or control isotype antibody (ve−), separated by SDS/PAGE, and incubated with a monoclonal anti-human SH-PTP1 or SH-PTP2 antibody. At the end, blots were stripped and incubated with a second anti-human EGFR antibody. Blots are representative of four separate experiments
Knockdown of SH-PTP2 but not SH-PTP1 expression prevents the 5-ASA-induced EGFR dephosphorylation
To establish the role of SH-PTP1 and SH-PTP2 in the 5-ASA-mediated attenuation of p-EGFR, we specifically knocked down the expression of these two PTPs by small interference RNA (siRNA) and then examined the effect of 5-ASA on p-EGFR. As shown in Figure 6a, transfection of CRC cells with PTP1 or PTP2 but not control siRNA reduced the level of the corresponding PTP, without altering the rate of cell death (not shown). Importantly, 5-ASA still inhibited EGF-induced p-EGFR in cells with knockdown of SH-PTP1. In contrast, SH-PTP2-deficient cells were largely resistant to the inhibitory effect of 5-ASA on p-EGFR (Figure 6b, c and right inset). This finding was seen independently on the CRC cell line used (not shown).
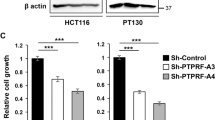
(a) Representative Western blots for SH-PTP1, SH-PTP2 and β-actin in total extracts from HT-29 cells transfected with control (ctr), SH-PTP1 and SH-PTP2 small interference (si)-RNA for 48 h. (b) Knockdown of SH-PTP2 prevents the inhibitory effect of 5-ASA on p-EGFR. HT-29 cells were either left untreated (Uns) or transfected with the above-indicated siRNA. After 48 h culture, cells were washed and cultured with or without 50 mM 5-ASA for 4 h followed by 200 ng/ml EGF for 10 min. Total extracts were then prepared and assessed for both p- and total EGFR. p-EGFR was analyzed by Western blotting using a monoclonal anti-human antibody that recognizes phosphorylation of the 1173 residue (central panel) or by immunoprecipitating total proteins with a specific monoclonal anti-human EGFR followed by incubation with p-Tyr ab (right inset). After detection of p-EGFR, blots were stripped and incubated with a total EGFR antibody. Blots in (a, b) are representative of three experiments in which similar results were obtained. (c) Quantitative analysis of p-EGFR/total EGFR protein ratio in HT-29 cells cultured as indicated in (b) and measured by densitometry scanning of Western blots. Values are expressed in arbitrary units (a.u.). Data are expressed as mean±S.D. of three separate experiments
5-ASA enhances PTP activity and attenuates p-EGFR in human CRC tissue
To extend our observations to primary CRC cells, we used a well-characterized ex vivo organ culture system of tissue explants from patients with primary CRC. Freshly obtained CRC explants were either left untreated or treated with 5-ASA for 6 h. At the end, epithelial cancer cells were purified and analyzed for the level of PTPs activity and p-EGFR. As shown in Figure 7a, 5-ASA caused a two-fold increase in the activity of PTPs that target p-EGFR (P=0.02). Consistent with this, 5-ASA reduced p-EGFR in CRC cells (Figure 7b,c), thus confirming the data obtained with the CRC cell lines. No change in cell viability was observed after 6 h treatment with 5-ASA (not shown). Similar results were obtained when PTPs activity and p-EGFR analysis was carried out in whole mucosal CRC samples (not shown).
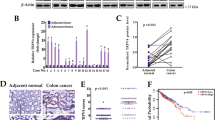
5-ASA enhances PTP activity (a) and attenuates p-EGFR (b) in primary CRC cells. Freshly obtained CRC explants were cultured in the absence (Uns=unstimulated) or presence of 50 mM 5-ASA. After 6 h, epithelial cells were purified and used for preparing total extracts, which were then incubated with a synthetic p-EGFR peptide for 15 min. Data indicate mean±S.D. of three separate experiments in which total extracts from five CRC mucosal explants were analyzed. (b) Total extracts were also analyzed for the content of both p- and total EGFR by Western blotting. One of two representative Western blots analyzing in total five CRC samples is shown. (c) Quantitative analysis of p-EGFR/totalEGFR protein ratio in epithelial cells of CRC explants, cultured with or without 5-ASA (Uns) for 6 h. Values are expressed in arbitrary units (a.u.). Each point represents the value (a.u.) of p-EGFR/totalEGFR protein ratio in epithelial cells taken from a single subject. Horizontal bars indicate the mean
Discussion
This study was undertaken to examine whether 5-ASA inhibits the activation of EGFR, a transmembrane tyrosine kinase, which triggers mitogenic signalling in CRC cells.11, 12 We show that 5-ASA is able to downregulate p-EGFR both in established CRC cell lines and ex vivo mucosal explants of patients with CRC. Importantly, attenuation of p-EGFR is obtained with 5-ASA concentrations, which are reached within the gut tissue under standard oral treatment.21, 22 The effect of 5-ASA on p-EGFR is reversible and associates with no induction of cell death. In contrast to our data, two different groups have recently shown that 5-ASA promotes apoptosis of adherent HT-29 cells.17, 18 To this regard, it is however noteworthy that, in both those studies, the induction of apoptosis by 5-ASA was seen only after 2 and 4 days of culture, respectively. In addition, when cell death was quantified by Reinacher-Schick et al.,17 it appeared evident that 5-ASA induced only a slight increase in the percentage of apoptotic cells (9 versus 4% in unstimulated cells). Together, these data therefore suggest that the early EGFR dephosphorylation documented in the present study is not secondary to a toxic effect of 5-ASA. It is also unlikely that 5-ASA inhibits p-EGFR by promoting ubiquitin-mediated degradation of the receptor, given that no change in the total level of EGFR was seen in 5-ASA-treated cells. In contrast, some observations made in this study strongly support the possibility that the attenuation of p-EGFR by 5-ASA relies on the activity of specific PTPs. First, the activity of PTPs targeting the p-EGFR was significantly enhanced by 5-ASA both in fully transformed cell lines and primary CRC cells. Second, PTPs inhibitors, such as sodium orthovanadate or iodoacetamide, prevented the 5-ASA-induced EGFR dephosphorylation. An analysis of the expression of several PTPs, which have been reported to control the extent of p-EGFR,23 revealed, however, no induction upon 5-ASA treatment. As PTPs, which dephosphorylate a receptor tyrosine kinase, should at least transiently bind to their substrate in the course of the dephosphorylation reaction, we have carried out experiments to examine whether and which PTP interacts with EGFR in 5-ASA-treated CRC cell lines. Our dot blot and coimmunoprecipitation assays indicate that both SH-PTP-1 and SH-PTP2 stably interact with EGFR in 5-ASA-treated CRC cells. However, the activity of SH-PTP-2 but not SH-PTP1 appears to be important in the 5-ASA-mediated EGFR dephosphorylation. Indeed, knockdown of SH-PTP2 but not SH-PTP1 by siRNA largely prevents the inhibitory effect of 5-ASA on p-EGFR. A semiquantitative analysis of Western blots reveals that the level of p-EGFR in SH-PTP2-deficient cells after 5-ASA treatment is, however, lower than that measured in wild-type cells. As we were not able to completely knockout SH-PTP2 by siRNA strategy, we do not know if this finding is due to either the activity of the remaining SH-PTP2 or additional PTP(s), which could contribute to dephosphorylate EGFR in 5-ASA-treated cells.
SH-PTP2 has been implicated as either a positive or negative mediator in receptor tyrosine kinase signalling pathways. For example, SH-PTP2 mediates activation of the mitogen-activated protein (MAP) kinase cascade in response to a variety of growth factors and biological evidence that SHP-2 is an important component of growth factor signalling pathways has been provided by multiple genetic studies as well as studies with both negative and activated mutants.25, 26 On the other hand, there is overwhelming evidence that SH-PTP2 may have negative regulatory influences. For instance, in Chinese hamster ovary cells expressing insulin receptors, SHP-2 attenuates insulin metabolic responses by reducing insulin receptor substrate-1 tyrosine phosphorylation.27 SH-PTP2 also acts as a negative regulator in both platelet-derived growth factor (PDGF) receptor-mediated signalling and the RAS pathway in T-cell receptor cascade.28, 29 In addition, SH-PTP2 has been shown to negatively regulate EGFR signalling in cells which overexpress EGFR, such as tumour cells.30 It is thus plausible that the ability of SH-PTP2 to differently transduce receptor tyrosine kinase signals is regulated in a cell-specific manner, and that this stems, at least in part, from the capacity of SH-PTP2 to participate in a multitude of protein–protein interactions. Our data do not help to clarify the biochemical mechanism by which 5-ASA promotes and stabilizes the interaction of SH-PTP2 with EGFR. Similarly, we do not yet know whether, upon 5-ASA, SH-PTP2 causes dephosphorylation of EGFR either directly or indirectly via adapter proteins.31, 32, 33 Studies are now in progress to specifically address these issues.
Both epidemiological and experimental data suggest that 5-ASA exerts antiproliferative effects on CRC cells.15, 16, 17, 18, 19, 20 Data of the present study confirm and expand on these observations and suggest a potential mechanism by which 5-ASA could interfere with CRC cell growth. We would like, however, to point out that our results also suggest the possibility that 5-ASA may affect additional pathways other than EGFR that sustain CRC cell growth. Indeed, we were able to show that 5-ASA inhibited CRC cell growth induced by FGF or FBS.
The demonstration that 5-ASA inhibits p-EGFR in CRC cells, and particularly in freshly obtained mucosal explants from CRC patients, strongly suggests the necessity of additional in vivo studies, both in animal models of CRC and human, in order to confirm the antineoplastic properties of 5-ASA. In designing such studies, it would however be necessary considering that the majority of both sporadic and IBD-related CRC occurs in the left colon, a site that is not reached by the current oral formulations of 5-ASA.
Materials and Methods
Cell culture and proliferation
The human colon adenocarcinoma cell lines HT-29, HT-115, T84 and Caco-2 were used in this study, given that we preliminarily documented high levels of p-EGFR in all these cell lines (not shown). Cells were maintained in appropriate media supplemented with 10% FBS. For cell growth assay, single-cell suspensions were plated at 2 × 103 cells/well in 96-well culture dishes and allowed to adhere overnight. Nonadherent cells were then removed and fresh media containing 0.5% bovine serum albumin (BSA), (Sigma-Aldrich, Milan, Italy) but not FBS and the desired concentrations of the test compounds were added and incubated for the indicated times points. Additionally, cells were cultured in the presence of 10% FBS with or without 5-ASA. 5-ASA was kindly provided by Giuliani S.p.A. (Milan, Italy) and dissolved as a 100 mM stock solution in culture medium. The pH of the drug solution was adjusted to 7.4 with NaOH, and experiments carried out protected from light. Mannitol (50 mM, pH 7.4, Sigma-Aldrich) was used as both osmolar and pH control. As additional pH control, cells were incubated with butyric acid (400 μM, pH 7.4, Sigma-Aldrich). To assess the effect of 5-ASA on cell proliferation induced by either EGF or basic FGF, cells were preincubated with 5-ASA (50 mM) for 4 h prior to adding EGF (200 ng/ml) or basic FGF (100 ng/ml) (both from Peprotech EC Ltd, London, UK). Bromodeoxiuridin (BrdU) was added to the cells during the last 6 h of incubation, and the level of BrDU-positive cells assessed after 22 h culture by a colorimetric kit (Roche Diagnostic, Monza, Italy).
For analysis of EGFR and PTPs expression, single-cell suspensions were plated at 1–2 × 106 cells/well in six-well culture dishes and allowed to adhere for 24–72 h. Nonadherent cells were then removed and fresh media containing no FBS and the desired concentrations of the test compounds were added and incubated for the indicated time points. To examine if the effect of 5-ASA on p-EGFR was reversible, cells were stimulated with graded doses of 5-ASA for 3–6 h, then extensively washed and cultured with medium containing 10% FBS for additional 16 h. To examine if general inhibitors of PTPs modified the effect of 5-ASA on p-EGFR, HT-29 cells were cultured in medium with no FBS in the absence (unstimulated) or presence of iodoacetamide (250 μg/ml) or sodium orthovanadate (Na3VO4, 100 μg/ml) (both from Sigma) for 30 min prior to adding 5-ASA. To examine the overall expression of PTPs and the interaction between EGFR and PTPs, cells were cultured with or without 5-ASA for 1–4 h and then stimulated with EGF (200 ng/ml) for 10 min. To assess the role of SH-PTP1 and SH-PTP2 in the control of p-EGFR by 5-ASA, HT-29 cells were transfected with SH-PTP1, SH-PTP-2 or control siRNA according to the manufacturer's instructions (Santa Cruz Biotechnology, Santa Cruz, CA, USA) using a Nucleofector (Amaxa GmbH, Koeln, Germany). Cells were then cultured in complete medium for 48 h. Nonadherent cells were then removed and fresh media containing no FBS and the desired concentrations of the test compounds were added and incubated for the indicated time points.
Organ culture
Freshly obtained CRC mucosal explants were taken from five patients undergoing colon resection for primary adenocarcinoma, as confirmed by histological analysis of the resected tissue. Patients received neither radiotherapy nor chemotherapy prior to undergoing surgery. Organ culture was performed as previously described.34 Briefly, CRC explants were cultured with or without the initial addition of 50 mM 5-ASA in medium containing no FBS. After 6 h, mucosal explants were harvested and used for isolating epithelial cells by treatment with 2 mM EDTA for 5 min. At the end, morphology and viability of isolated cells was checked, and total extracts prepared for analysis of PTP activity and Western blotting.
Western blot analysis
To analyze p-EGFR, total proteins were separated on an 8% SDS-PAGE gel and then incubated with a mouse anti-human monoclonal EGFR antibody (0.2 μg/ml) (Inalco, Milan Italy), which specifically recognizes phosphorylation of EGFR on tyrosine residue 1173. Phosphorylation of such a residue reflects EGFR activation. After analysis of p-EGFR, blots were stripped and incubated with an antibody recognizing total EGFR (Santa Cruz Biotechnology, sc-03). Analysis of SH-PTP1 (sc-7289), SH-PTP2 (sc-7384), LAR (sc-25434), PTP1β(sc-14021) and RPTPα (sc-19116) was carried out using antibodies (1 : 500 final dilution) from Santa Cruz Biotechnology, whereas PTP-PEST was from Cell Signalling (DBA Milan Italy, 4864). Binding of the primary antibody was detected using a horseradish peroxidase-conjugated secondary antibody (Dako S.p.A., Milan, Italy) (final dilution 1 : 20 000) and chemiluminescent substrate (Pierce, Rockford, IL, USA). At the end, each blot was stripped and incubated with a mouse-anti-human monoclonal β-actin antibody (1 : 5000, Sigma) to ascertain equivalent loading of the lanes. Computer-assisted scanning densitometry (Total lab, AB.EL Sience-Ware Srl, Rome, Italy) was used to analyze the intensity of the immunoreactive bands.
Immunoprecipitation and PTPs identification
Total extracts were prepared from CRC cells cultured as indicated above and immunoprecipitated using an anti-human monoclonal EGFR antibody (2 μg/sample, Santa Cruz Biotechnology, sc 120) or control isotype antiserum for 2 h followed by incubation with protein A/G agarose beads overnight. The resulting immunoprecipitates were washed thoroughly four times with cold lysis buffer, and then transferred onto the nitrocellulose membrane using a dot blot apparatus and incubated with the indicated PTPs and EGFR antibodies. In parallel, immunoprecipitates were also separated by SDS/PAGE, and immunoblotted with antibodies for SH-PTP1 and SH-PTP2 (Santa Cruz Biotechnology). To further confirm the effect of 5-ASA on p-EGFR, EGFR-immunoprecipitates were also incubated with a human phosphotyrosine antibody (Santa Cruz Biotechnology). After analysis of PTPs and p-EGFR blots were stripped and incubated with a monoclonal anti-human EGFR antibody.
Analysis and quantification of cell death
Adherent CRC cells (2 × 105) were cultured in Mc Coy's medium containing no FBS in the absence (unstimulated) or presence of graded doses of 5-ASA or mannitol (50 mM) for 6 h. To score cell death, cells were incubated for 20 min with 5 μg/ml PI (Sigma) and stained with FITC-AV in appropriate staining buffer. In addition, cell apoptosis was examined using a commercially available colorimetric kit (Roche Diagnostic), which is able to determine cytoplasmic histone-associated-DNA-fragments after induced cell death. To this end, adherent HT-29 cells (2 × 103) were cultured in DMEM containing no FBS in the presence or absence of graded doses of 5-ASA, mannitol (50 mM) or staurosporin (500 ng/ml, Sigma) for 6 h, and then cell apoptosis assessed according to the manufacturer's instructions.
PTP activity assay
For PTP assay, 20 μg of total extracts from HT-29 cells or 40 μg from epithelial cells of CRC explants were incubated in a final volume of 100 μl at 23°C for 15 min in reaction buffer containing 50 mM HEPES, 150 mM NaCl, 2 mM EDTA, 10 mM DTT, and a synthetic phosphorylated EGFR peptide as a substrate (50 μM, DBA Italia s.r.l., Milan, Italy). The reaction was then terminated by the addition of 1 ml BIOMOL GREEN Reagent, and the absorption was determined at 620 nm. Serial dilutions of phosphate standard (Biomol) were also used in order to calculate the amount of PO2 released in the reaction. To examine whether 5-ASA regulates general PTP activity, 20 μg of total extracts from HT-29 cells were incubated in a final volume of 100 μl at 37°C for 15–30 min in reaction buffer containing 50 mM HEPES, 2 mM EDTA, 1 mM DTT, and 10 mM 4-nitrophenyl phosphate (Sigma) as a substrate. The reaction was stopped by the addition of 50 μl of 1 M NaOH and the absorption was determined at 405 nm.
Statistical analysis
Differences between groups were compared using the Student t-test or Mann–Whitney U test.
Abbreviations
- CRC:
-
colorectal cancer
- NSAIDs:
-
nonsteroidal anti-inflammatory drugs
- EGFR:
-
epidermal growth factor receptor
- 5-ASA:
-
5-aminosalicylic acid
- IBD:
-
inflammatory bowel disease
- AV:
-
annexin V
- PI:
-
propidium iodide
- FBS:
-
fetal bovine serum
- EGF:
-
epidermal growth factor
- FGF:
-
fibroblast growth factor
- PTPs:
-
phosphatases
- siRNA:
-
small interference RNA
- MAP:
-
mitogen-activated protein
- PDGF:
-
platelet-derived growth factor
- BSA:
-
bovine serum albumin
- BrdU:
-
bromodeoxiuridin
References
Keighley MRB (2003) Gastrointestinal cancers in Europe. Aliment. Pharmacol. Ther. 18 (Suppl. 3): 7–30
Beauchamp RD, Peeler MO and DuBois RN (1996) Recent advances in the management of colorectal polyps. Curr. Opin. Gastroenterol. 12: 12–17
Huls G, Koornstra JJ and Kleibeuker JH (2003) Non-steroidal anti-inflammatory drugs and molecular carcinogenesis of colorectal carcinomas. Lancet 362: 230–232
Smalley WE and DuBois RN (1997) Colorectal cancer and nonsteroidal anti-inflammatory drugs. Adv. Pharmacol. 39: 1–20
Koehne CH and Dubois RN (2004) COX-2 inhibition and colorectal cancer. Semin. Oncol. 31 (Suppl 7): 12–21
Silverstein FE, Faich G, Goldstein JL, Simon LS, Pincus T, Whelton A, Makuch R, Eisen G, Agrawal NM, Stenson WF, Burr AM, Zhao WW, Kent JD, Lefkowith JB, Verburg KM and Geis GS (2000) Gastrointestinal toxicity with celecoxib vs nonsteroidal anti-inflammatory drugs for osteoarthritis and rheumatoid arthritis. The CLASS study: a randomized controlled trial. JAMA 284: 1247–1255
Mukherjee D, Nissen SE and Topol EJ (2001) Risk of cardiovascular events associated with selective COX-2 inhibitors. JAMA 286: 954–959
Juni P, Nartey L, Reichenbach S, Sterchi R, Dieppe PA and Egger M (2004) Risk of cardiovascular events and rofecoxib: cumulative meta-analysis. Lancet 364: 2021–2029
Jorissen RN, Walker F, Pouliot N, Garrett TP, Ward CW and Burgess AW (2003) Epidermal growth factor receptor: mechanisms of activation and signalling. Exp. Cell Res. 284: 31–53
Bradley SJ, Garfinkle G, Walker E, Salem R, Chen LB and Steele Jr G (1986) Increased expression of the epidermal growth factor receptor on human colon carcinoma cells. Arch. Surg. 121: 1242–1247
Janmaat ML and Giaccone G (2003) The epidermal growth factor receptor pathway and its inhibition as anticancer therapy. Drugs Today 39 (Suppl C): 61–80
Roberts RB, Min L, Washington MK, Olsen SJ, Settle SH, Coffey RJ and Threadgill DW (2002) Importance of epidermal growth factor receptor signaling in establishment of adenomas and maintenance of carcinomas during intestinal tumorigenesis. Proc. Natl. Acad. Sci. 99: 1521–1526
Mendelsohn J (2001) The epidermal growth factor receptor as a target for cancer therapy. Endocrine –Relat. Cancer 8: 3–9
Mendelsohn J and Baselga J (2000) The EGF receptor family as targets for cancer therapy. Oncogene 19: 6550–6565
Eaden J, Abrams K, Ekbom A, Jackson E and Mayberry J (2000) Colorectal cancer prevention in ulcerative colitis: a case–control study. Aliment. Pharmacol. Ther. 14: 145–153
Eaden J (2003) Review article: the data supporting a role for aminosalicylates in the chemoprevention of colorectal cancer in patients with inflammatory bowel disease. Aliment. Pharmacol. Ther. 182: 15–21
Reinacher-Schick A, Schoeneck A, Graeven U, Schwarte-Waldhoff I and Schmiegel W (2003) Mesalazine causes a mitotic arrest and induces caspase-dependent apoptosis in colon carcinoma cells. Carcinogenesis 24: 443–451
Narisawa T and Fukaura Y (2003) Prevention by intrarectal 5-aminosalicylic acid of N-methylnitrosourea-induced colon cancer in F344 rats. Dis. Colon Rectum 46: 900–903
Brown WA, Farmer KC, Skinner SA, Malcontenti-Wilson C, Misajon A and O'Brien PE (2000) 5-aminosalicyclic acid and olsalazine inhibit tumor growth in a rodent model of colorectal cancer. Dig. Dis. Sci. 45: 1578–1584
MacGregor DJ, Kim YS, Sleisenger MH and Johnson LK (2000) Chemoprevention of colon cancer carcinogensis by balsalazide: inhibition of azoxymethane-induced aberrant crypt formation in the rat colon and intestinal tumor formation in the B6-Min/+ mouse. Int. J. Oncol. 17: 173–179
Frieri G, Pimpo MT, Palumbo GC, Onori L, Viscido A, Latella G, Galletti B, Pantaleoni GC and Caprilli R (1999) Rectal and colonic mesalazine concentration in ulcerative colitis: oral vs oral plus topical treatment. Aliment. Pharmacol. Ther. 13: 1413–1417
Frieri G, Giacomelli R, Pimpo M, Palumbo G, Passacantando A, Pantaleoni G and Caprilli R (2000) Mucosal 5-aminosalicylic acid concentration inversely correlates with severity of colonic inflammation in patients with ulcerative colitis. Gut 47: 410–414
Moghal N and Sternberg PW (1999) Multiple positive and negative regulators of signaling by the EGF-receptor. Curr. Opin. Cell Biol. 11: 190–196
Zhang ZY (1998) Protein-tyrosine phosphatases: biological function, structural characteristics, and mechanism of catalysis. Crit. Rev. Biochem. Mol. Biol. 33: 1–52
Noguchi T, Matozaki T, Horita K, Fujioka Y and Kasuga M (1994) Role of SH-PTP2, a protein-tyrosine phosphatase with Src homology 2 domains, in insulin-stimulated Ras activation. Mol. Cell. Biol. 14: 6674–6682
Tonks NK and Neel BG (2001) Combinatorial control of the specificity of protein tyrosine phosphatases. Curr. Opin. Cell Biol. 13: 182–195
Noguchi T, Matozaki T, Fujioka Y, Yamao T, Tsuda M, Takada T and Kasuga M (1996) Characterization of a 115-kDa protein that binds to SH-PTP2, a protein–tyrosine phosphatase with Src homology 2 domains, in Chinese hamster ovary cells. J. Biol. Chem. 271: 27652–27658
Cossette LJ, Hoglinger O, Mou L and Shen SH (1996) Localization and down-regulating role of the protein tyrosine phosphatase PTP2C in membrane ruffles of PDGF-stimulated cells. Exp. Cell Res. 223: 459–466
Marengere LE, Waterhouse P, Duncan GS, Mittrucker HW, Feng GS and Mak TW (1996) Regulation of T cell receptor signaling by tyrosine phosphatase SYP association with CTLA-4. Science 272: 1170–1173
Reeves SA, Sinha B, Baur I, Reinhold D and Harsh G (1995) An alternative role for the src-homology-domain-containing phosphotyrosine phosphatase (SH-PTP2) in regulating epidermal-growth-factor-dependent cell growth. Eur. J. Biochem. 233: 55–61
Cunnick JM, Dorsey JF, Munoz-Antonia T, Mei L and Wu J (2000) Requirement of SHP2 binding to Grb2-associated binder-1 for mitogen-activated protein kinase activation in response to lysophosphatidic acid and epidermal growth factor. J. Biol. Chem. 275: 13842–13848
Schaeper U, Gehring NH, Fuchs KP, Sachs M, Kempkes B and Birchmeier W (2000) Coupling of Gab1 to c-Met, Grb2, and Shp2 mediates biological responses. J. Cell Biol. 149: 1419–1432
Neel BG, Gu H and Pao L (2003) The ‘Shp'ing news: Sh2 domain-containing tyrosine phosphatses in cell signalling. Trends Biochem. Sci. 28: 284–293
Monteleone G, Kumberova A, Croft NM, McKenzie C, Steer HW and MacDonald TT (2001) Blocking Smad7 restores TGF-beta1 signaling in chronic inflammatory bowel disease. J. Clin. Invest. 108: 601–609
Acknowledgements
The study was supported by the Associazione Italiana per la Ricerca sul Cancro and Fondazione ‘Umberto Di Mario’, Rome, Italy.
Author information
Authors and Affiliations
Author notes
G Monteleone, L Franchi, D Fina: These authors contributed equally to the study.
Corresponding author
Additional information
Edited by M Blagosklonny
Rights and permissions
About this article
Cite this article
Monteleone, G., Franchi, L., Fina, D. et al. Silencing of SH-PTP2 defines a crucial role in the inactivation of epidermal growth factor receptor by 5-aminosalicylic acid in colon cancer cells. Cell Death Differ 13, 202–211 (2006). https://doi.org/10.1038/sj.cdd.4401733
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.cdd.4401733
Keywords
This article is cited by
-
Use of patient-derived explants as a preclinical model for precision medicine in colorectal cancer: A scoping review
Langenbeck's Archives of Surgery (2023)
-
Combination of metformin and 5-aminosalicylic acid cooperates to decrease proliferation and induce apoptosis in colorectal cancer cell lines
BMC Cancer (2016)
-
A functional role for Smad7 in sustaining colon cancer cell growth and survival
Cell Death & Disease (2014)
-
Cost Effectiveness of Ulcerative Colitis Surveillance in the Setting of 5-Aminosalicylates
The American Journal of Gastroenterology (2009)