Abstract
The clinical entities that comprise acute coronary syndromes (ACS)—ST-segment elevation myocardial infarction (STEMI), non-STEMI, and unstable angina—have been recognized as widespread causes of death and disability for more than a century. Seminal research in the past 50 years has led to important scientific and medical advances in our understanding of ACS. Rapid modernization of the developing world has led to a pandemic of coronary artery disease and its manifestation as ACS, with profound implications for personal, societal, and global health. Epidemiological studies have provided insight into the changing demographics of ACS, and highlighted the importance of modifiable risk factors and adherence to guideline-recommended therapy.
Key Points
-
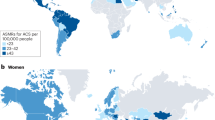
The prevalence of acute coronary syndromes (ACS) has reached a pandemic level as a consequence of modernization of the developing world
-
The demographics of ACS have evolved, with a precipitous decline in the incidence of ST-segment elevation myocardial infarction (STEMI) and a progressive rise in the incidence of non-STEMI
-
Modifiable risk factors account for >90% of the risk of myocardial infarction
-
Cardiac mortality has declined steadily over the past 50 years
-
Improvement in outcomes after ACS reflects increased adoption and utilization of evidence-based therapies, although racial, ethnic, and socioeconomic differences in care still exist
-
Epidemiological surveillance and population-based studies will be essential to evaluate the successful translation of evidence-based medicine into clinical practice
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout





Similar content being viewed by others
References
Heberden, W. Some account of a disorder of the breast. Med. Trans. R. Coll. Physicians Lond. 2, 59–67 (1772).
Osler, W. The Lumleian lectures on angina pectoris. Lancet 175, 697–701 (1910).
Lopez, A. D., Mathers, C. D., Ezzati, M., Jamison, D. T. & Murray, C. J. (Eds). Global Burden of Disease and Risk Factors (Oxford University Press and The World Bank, New York, 2006).
Lloyd-Jones, D. et al. for the AHA Statistics Committee and Stroke Statistics Subcommittee. Executive summary: heart disease and stroke statistics—2010 update: a report from the American Heart Association. Circulation 121, 948–954 (2010).
Yusuf, S., Reddy, S., Ounpuu, S. & Anand, S. Global burden of cardiovascular diseases: part I: general considerations, the epidemiologic transition, risk factors, and impact of urbanization. Circulation 104, 2746–2753 (2001).
Armstrong, G. L., Conn, L. A. & Pinner, R. W. Trends in infectious disease mortality in the United States during the 20th century. JAMA 281, 61–66 (1999).
Centers for Disease Control and Prevention (CDC). Control of infectious diseases. MMWR Morb. Mortal. Wkly Rep. 48, 621–629 (1999).
Omran, A. R. The epidemiologic transition. A theory of the epidemiology of population change. Milbank Mem. Fund Q. 49, 509–538 (1971).
Gaziano, J. M. in Braunwald's Heart Disease: A Textbook of Cardiovascular Medicine 8th edn (Eds Libby, P., Bonow, R. O., Mann, D. L. & Zipes, D. P.) 1–22 (Saunders, Philadelphia, 2007).
Olshansky, S. J. & Ault, A. B. The fourth stage of the epidemiologic transition: the age of delayed degenerative diseases. Milbank Q. 64, 355–391 (1986).
Steyn, K. et al. for the INTERHEART Investigators in Africa. Risk factors associated with myocardial infarction in Africa: the INTERHEART Africa study. Circulation 112, 3554–3561 (2005).
Gaziano, T. A. Cardiovascular disease in the developing world and its cost-effective management. Circulation 112, 3547–3553 (2005).
Clark, A. M., DesMeules, M., Luo, W., Duncan, A. S. & Wielgosz, A. Socioeconomic status and cardiovascular disease: risks and implications for care. Nat. Rev. Cardiol. 6, 712–722 (2009).
Gersh, B. J., Sliwa, K., Mayosi, B. M. & Yusuf, S. Novel therapeutic concepts: the epidemic of cardiovascular disease in the developing world: global implications. Eur. Heart J. 31, 642–648 (2010).
Cooper, R. et al. Trends and disparities in coronary heart disease, stroke, and other cardiovascular diseases in the United States: findings of the national conference on cardiovascular disease prevention. Circulation 102, 3137–3147 (2000).
Hoyert, D. L., Heron, M. P., Murphy, S. L. & Kung, H. C. Deaths: final data for 2003. Natl Vital Stat. Rep. 54, 1–120 (2006).
Chobanian, A. V. et al. The Seventh Report of the Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure: the JNC7 report. JAMA 289, 2560–2572 (2003).
Centers for Disease Control and Prevention (CDC). Cigarette smoking among adults—United States, 2004. MMWR Morb. Mortal. Wkly Rep. 54, 1121–1124 (2005).
Dobson, A. J. et al. Changes in estimated coronary risk in the 1980s: data from 38 populations in the WHO MONICA Project. World Health Organization. Monitoring trends and determinants in cardiovascular diseases. Ann. Med. 30, 199–205 (1998).
Flegal, K. M., Carroll, M. D., Ogden, C. L. & Curtin, L. R. Prevalence and trends in obesity among US adults, 1999–2008 JAMA 303, 235–241 (2010).
Hannon, T. S., Rao, G. & Arslanian, S. A. Childhood obesity and type 2 diabetes mellitus. Pediatrics 116, 473–480 (2005).
Muntner, P., He, J., Cutler, J. A., Wildman, R. P. & Whelton, P. K. Trends in blood pressure among children and adolescents. JAMA 291, 2107–2113 (2004).
Notzon, F. C. et al. Causes of declining life expectancy in Russia. JAMA 279, 793–800 (1998).
Plavinski, S. L., Plavinskaya, S. I. & Klimov, A. N. Social factors and increase in mortality in Russia in the 1990s: prospective cohort study. BMJ 326, 1240–1242 (2003).
Yeh, R. W. et al. Population trends in the incidence and outcomes of acute myocardial infarction. N. Engl. J. Med. 362, 2155–2165 (2010).
Rogers, W. J. et al. Trends in presenting characteristics and hospital mortality among patients with ST-elevation and non-ST elevation myocardial infarction in the National Registry of Myocardial Infarction from 1990 to 2006. Am. Heart J. 156, 1026–1034 (2008).
Roger, V. L. et al. Trends in incidence, severity, and outcome of hospitalized myocardial infarction. Circulation 121, 863–869 (2010).
Avezum, A. et al. Impact of age on management and outcome of acute coronary syndrome: observations from the Global Registry of Acute Coronary Events (GRACE). Am. Heart J. 149, 67–73 (2005).
Björck, L., Wallentin, L., Stenestrand, U., Lappas, G. & Rosengren, A. Medication in relation to ST-segment elevation myocardial infarction in patients with a first myocardial infarction: Swedish Register of Information and Knowledge About Swedish Heart Intensive Care Admissions (RIKS-HIA). Arch. Intern. Med. 170, 1375–1381 (2010).
Mukamal, K. J. et al. Recent aspirin use is associated with smaller myocardial infarct size and lower likelihood of Q-wave infarction. Am. Heart J. 137, 1120–1128 (1999).
Spencer, F. A. et al. Association of statin therapy with outcomes of acute coronary syndromes: the GRACE study. Ann. Intern. Med. 140, 857–866 (2004).
Spencer, F. A. et al. Impact of aspirin on presentation and hospital outcomes in patients with acute coronary syndromes (The Global Registry of Acute Coronary Events [GRACE]). Am. J. Cardiol. 90, 1056–1061 (2002).
Antithrombotic Trialists' Collaboration. Collaborative meta-analysis of randomised trials of antiplatelet therapy for prevention of death, myocardial infarction, and stroke in high risk patients. BMJ 324, 71–86 (2002).
Freemantle, N., Cleland, J., Young, P., Mason, J. & Harrison, J. Beta blockade after myocardial infarction: systematic review and meta regression analysis. BMJ 318, 1730–1737 (1999).
Gruppo Italiano per lo Studio della Streptochinasi nell'Infarto Miocardico (GISSI). Effectiveness of intravenous thrombolytic treatment in acute myocardial infarction. Lancet 1, 397–402 (1986).
ISIS-4 (Fourth International Study of Infarct Survival) Collaborative Group. ISIS-4: a randomised factorial trial assessing early oral captopril, oral mononitrate, and intravenous magnesium sulfate in 58,050 patients with suspected acute myocardial infarction. Lancet 345, 669–685 (1995).
Lonn, E. M. et al. Emerging role of angiotensin-converting enzyme inhibitors in cardiac and vascular protection. Circulation 90, 2056–2069 (1994).
LaRosa, J. C. Pleiotropic effects of statins and their clinical significance. Am. J. Cardiol. 88, 291–293 (2001).
Ray, K. K. & Cannon, C. P. The potential relevance of the multiple lipid-independent (pleiotropic) effects of statins in the management of acute coronary syndromes. J. Am. Coll. Cardiol. 46, 1425–1433 (2005).
Alpert, J. S., Thygesen, K., Antman, E. & Bassand, J. P. Myocardial infarction redefined—a consensus document of The Joint European Society of Cardiology/American College of Cardiology Committee for the redefinition of myocardial infarction. J. Am. Coll. Cardiol. 36, 959–969 (2000).
Thygesen, K., Alpert, J. S. & White, H. D. for the Joint ESC/ACCF/AHA/WHF Task Force for the Redefinition of Myocardial Infarction. Universal definition of myocardial infarction. Eur. Heart J. 28, 2525–2538 (2007).
Bertoni, A. G., Bonds, D. E., Thom, T., Chen, G. J. & Goff, D. C., Jr. Acute coronary syndrome national statistics: challenges in definitions. Am. Heart J. 149, 1055–1061 (2005).
Trevelyan, J., Needham, E. W., Smith, S. C. & Mattu, R. K. Impact of the recommendations for the redefinition of myocardial infarction on diagnosis and prognosis in an unselected United Kingdom cohort with suspected cardiac chest pain. Am. J. Cardiol. 93, 817–821 (2004).
McGovern, P. G. et al. Trends in acute coronary heart disease mortality, morbidity, and medical care from 1985 through 1997: the Minnesota heart survey. Circulation 104, 19–24 (2001).
Goldberg, A., Yalonetsky, S., Kopeliovich, M., Azzam, Z. & Markiewicz, W. Appropriateness of diagnosis of unstable angina pectoris in patients referred for coronary arteriography. Exp. Clin. Cardiol. 13, 133–137 (2008).
Tunstall-Pedoe, H. et al. Myocardial infarction and coronary deaths in the World Health Organization MONICA Project. Registration procedures, event rates, and case-fatality rates in 38 populations from 21 countries in four continents. Circulation 90, 583–612 (1994).
Hardoon, S. L. et al. How much of the recent decline in the incidence of myocardial infarction in British men can be explained by changes in cardiovascular risk factors? Evidence from a prospective population-based study. Circulation 117, 598–604 (2008).
Parikh, N. I. et al. Long-term trends in myocardial infarction incidence and case fatality in the National Heart, Lung, and Blood Institute's Framingham Heart study. Circulation 119, 1203–1210 (2009).
Yusuf, S. et al. for the INTERHEART Study Investigators. Effect of potentially modifiable risk factors associated with myocardial infarction in 52 countries (the INTERHEART study): case-control study. Lancet 364, 937–952 (2004).
Sytkowski, P. A., D'Agostino, R. B., Belanger, A. & Kannel, W. B. Sex and time trends in cardiovascular disease incidence and mortality: the Framingham Heart Study, 1950–1989. Am. J. Epidemiol. 143, 338–350 (1996).
Anand, S. S. et al. for the INTERHEART Investigators. Risk factors for myocardial infarction in women and men: insights from the INTERHEART study. Eur. Heart J. 29, 932–940 (2008).
Tibazarwa, K. et al. A time bomb of cardiovascular risk factors in South Africa: results from the Heart of Soweto Study “Heart Awareness Days”. Int. J. Cardiol. 132, 233–239 (2009).
Schwartz, J. B. & Zipes, D. P. in Braunwald's Heart Disease: A Textbook of Cardiovascular Medicine 8th edn (Eds Libby, P., Bonow, R. O., Mann, D. L. & Zipes, D. P.) 1923–1953 (Saunders, Philadelphia, 2007).
Blomkalns, A. L. et al. Gender disparities in the diagnosis and treatment of non-ST-segment elevation acute coronary syndromes: large-scale observations from the CRUSADE (Can Rapid Risk Stratification of Unstable Angina Patients Suppress Adverse Outcomes With Early Implementation of the American College of Cardiology/American Heart Association Guidelines) National Quality Improvement Initiative. J. Am. Coll. Cardiol. 45, 832–837 (2005).
McLaughlin, T. J. et al. Adherence to national guidelines for drug treatment of suspected acute myocardial infarction: evidence for undertreatment in women and the elderly. Arch. Intern. Med. 156, 799–805 (1996).
Watkins, S. et al. Fourteen-year (1987 to 2000) trends in the attack rates of, therapy for, and mortality from non-ST-elevation acute coronary syndromes in four United States communities. Am. J. Cardiol. 96, 1349–1355 (2005).
Rosamond, W. D., Folsom, A. R., Chambless, L. E. & Wang, C. H. Atherosclerosis Risk in Communities. Coronary heart disease trends in four United States communities. The Atherosclerosis Risk in Communities (ARIC) study 1987–1996. Int. J. Epidemiol. 30 (Suppl. 1), S17–S22 (2001).
Rosamond, W. D. et al. Trends in the incidence of myocardial infarction and in mortality due to coronary heart disease, 1987 to 1994. N. Engl. J. Med. 339, 861–867 (1998).
Fox, C. S., Evans, J. C., Larson, M. G., Kannel, W. B. & Levy, D. Temporal trends in coronary heart disease mortality and sudden cardiac death from 1950 to 1999: the Framingham Heart Study. Circulation 110, 522–527 (2004).
Mandelzweig, L. et al. for the Euro Heart Survey Investigators. The second Euro Heart Survey on acute coronary syndromes: characteristics, treatment, and outcome of patients with ACS in Europe and the Mediterranean Basin in 2004. Eur. Heart J. 27, 2285–2293 (2006).
Shah, R., Wang, Y., Masoudi, F. A. & Foody, J. M. National impact of the troponin diagnostic standard on the prevalence and prognosis of acute myocardial infarction in older persons. Crit. Pathw. Cardiol. 5, 160–166 (2006).
Krumholz, H. M. et al. Reduction in acute myocardial infarction mortality in the United States: risk-standardized mortality rates from 1995–2006. JAMA 302, 767–773 (2009).
Ford, E. S. et al. Explaining the decrease in U. S. deaths from coronary disease, 1980–2000. N. Engl. J. Med. 356, 2388–2398 (2007).
Peterson, E. D. et al. Association between hospital process performance and outcomes among patients with acute coronary syndromes. JAMA 295, 1912–1920 (2006).
Weir, R. A., McMurray, J. J. & Velazquez, E. J. Epidemiology of heart failure and left ventricular systolic dysfunction after acute myocardial infarction: prevalence, clinical characteristics, and prognostic importance. Am. J. Cardiol. 97, 13F–25F (2006).
Spencer, F. A. et al. Twenty year trends (1975–1995) in the incidence, in-hospital and long-term death rates associated with heart failure complicating acute myocardial infarction: a community-wide perspective. J. Am. Coll. Cardiol. 34, 1378–1387 (1999).
Goldberg, R. J. et al. A 25-year perspective into the changing landscape of patients hospitalized with acute myocardial infarction (the Worcester Heart Attack Study). Am. J. Cardiol. 94, 1373–1378 (2004).
Hellermann, J. P. et al. Incidence of heart failure after myocardial infarction: is it changing over time? Am. J. Epidemiol. 157, 1101–1107 (2003).
Velagaleti, R. S. et al. Long-term trends in the incidence of heart failure after myocardial infarction. Circulation 118, 2057–2062 (2008).
Sutton, M. G. & Sharpe, N. Left ventricular remodeling after myocardial infarction: pathophysiology and therapy. Circulation 101, 2981–2988 (2000).
McWilliams, J. M., Meara, E., Zaslavsky, A. M. & Ayanian, J. Z. Differences in control of cardiovascular disease and diabetes by race, ethnicity, and education: US trends from 1999 to 2006 and effects of Medicare coverage. Ann. Intern. Med. 150, 505–515 (2009).
Steinberg, B. A. et al. Nine-year trends in achievement of risk factor goals in the US and European outpatients with cardiovascular disease. Am. Heart J. 156, 719–727 (2008).
Bhatt, D. L. et al. for the REACH Registry Investigators. International prevalence, recognition, and treatment of cardiovascular risk factors in outpatients with atherothrombosis. JAMA 295, 180–189 (2006).
EUROASPIRE Study Group. EUROASPIRE. A European Society of Cardiology survey of secondary prevention of coronary heart disease: principal results. European Action on Secondary Prevention through Intervention to Reduce Events. Eur. Heart J. 18, 1569–1582 (1997).
EUROASPIRE I and II Group. EUROASPIRE I and II Group & European Action on Secondary Prevention by Intervention to Reduce Events. Clinical reality of coronary prevention guidelines: a comparison of EUROASPIRE I and II in nine countries. European Action on Secondary Prevention by Intervention to Reduce Events. Lancet 357, 995–1001 (2001).
Kotseva, K. et al. EUROASPIRE III: a survey on the lifestyle, risk factors and use of cardioprotective drug therapies in coronary patients from 22 European countries. Eur. J. Cardiovasc. Prev. Rehabil. 16, 121–137 (2009).
Kotseva, K. et al. Cardiovascular prevention guidelines in daily practice: a comparison of EUROASPIRE I, II, and III surveys in eight European countries. Lancet 373, 929–940 (2009).
Peterson, E. D. et al. Trends in quality of care for patients with acute myocardial infarction in the National Registry of Myocardial Infarction from 1990 to 2006. Am. Heart J. 156, 1045–1055 (2008).
McGlynn, E. A. et al. The quality of health care delivered to adults in the United States. N. Engl. J. Med. 348, 2635–2645 (2003).
Sonel, A. F. et al. Racial variations in treatment and outcomes of black and white patients with high-risk non-ST-elevation acute coronary syndromes: insights from CRUSADE (Can Rapid Risk Stratification of Unstable Angina Patients Suppress Adverse Outcomes with Early Implementation of the ACC/AHA Guidelines?). Circulation 111, 1225–1232 (2005).
Yeh, R. W. & Go, A. S. Rethinking the epidemiology of acute myocardial infarction: challenges and opportunities. Arch. Intern. Med. 170, 759–764 (2010).
Author information
Authors and Affiliations
Contributions
C. T. Ruff and E. Braunwald researched data for the article, contributed to discussion of the content, and reviewed and edited the article before submission and after peer review. The article was written by C. T. Ruff.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Rights and permissions
About this article
Cite this article
Ruff, C., Braunwald, E. The evolving epidemiology of acute coronary syndromes. Nat Rev Cardiol 8, 140–147 (2011). https://doi.org/10.1038/nrcardio.2010.199
Published:
Issue Date:
DOI: https://doi.org/10.1038/nrcardio.2010.199
This article is cited by
-
Dynamic myocardial CT perfusion imaging—state of the art
European Radiology (2023)
-
A three-year longitudinal study of healthy lifestyle behaviors and adherence to pharmacological treatments in newly diagnosed patients with acute coronary syndrome: hierarchical linear modeling analyses
Journal of Public Health (2022)
-
YINGLONG: A Multicenter, Prospective, Non-Interventional Study Evaluating the Safety and Tolerability of Ticagrelor in Chinese Patients with Acute Coronary Syndrome
Advances in Therapy (2019)
-
A review in enormity of OCT and its enduring understanding of vulnerable plaque in coronary bifurcation lesion
The International Journal of Cardiovascular Imaging (2018)
-
Association of polymorphisms in the MAFB gene and the risk of coronary artery disease and ischemic stroke: a case–control study
Lipids in Health and Disease (2015)