Abstract
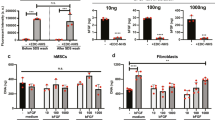
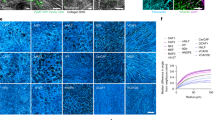
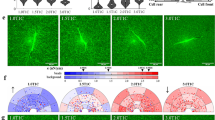
Scarring is a long-lasting problem in higher animals, and reductionist approaches could aid in developing treatments. Here, we show that copolymerization of collagen I with polyacrylamide produces minimal matrix models of scars (MMMS), in which fractal-fibre bundles segregate heterogeneously to the hydrogel subsurface. Matrix stiffens locally—as in scars—while allowing separate control over adhesive-ligand density. The MMMS elicits scar-like phenotypes from mesenchymal stem cells (MSCs): cells spread and polarize quickly, increasing nucleoskeletal lamin-A yet expressing the ‘scar marker’ smooth muscle actin (SMA) more slowly. Surprisingly, expression responses to MMMS exhibit less cell-to-cell noise than homogeneously stiff gels. Such differences from bulk-average responses arise because a strong SMA repressor, NKX2.5, slowly exits the nucleus on rigid matrices. NKX2.5 overexpression overrides rigid phenotypes, inhibiting SMA and cell spreading, whereas cytoplasm-localized NKX2.5 mutants degrade in well-spread cells. MSCs thus form a ‘mechanical memory’ of rigidity by progressively suppressing NKX2.5, thereby elevating SMA in a scar-like state.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout






Similar content being viewed by others
References
Gurtner, G. C., Werner, S., Barrandon, Y. & Longaker, M. T. Wound repair and regeneration. Nature 453, 314–321 (2008).
Georges, P. C. et al. Increased stiffness of the rat liver precedes matrix deposition: Implications for fibrosis. Am. J. Physiol. 293, G1147–G1154 (2007).
Liu, F. et al. Feedback amplification of fibrosis through matrix stiffening and COX-2 suppression. J. Cell Biol. 190, 693–706 (2010).
Berry, M. F. et al. Mesenchymal stem cell injection after myocardial infarction improves myocardial compliance. Am. J. Physiol. 290, H2196–H2203 (2006).
Engler, A. J., Rehfeldt, F., Sen, S. & Discher, D. E. Microtissue elasticity: Measurements by atomic force microscopy and its influence on cell differentiation. Methods Cell Biol. 83, 521–545 (2007).
Discher, D. E., Janmey, P. & Wang, Y. L. Tissue cells feel and respond to the stiffness of their substrate. Science 310, 1139–1143 (2005).
Khorasani, H. et al. A quantitative approach to scar analysis. Am. J. Pathol. 178, 621–628 (2011).
Martin, P. Wound healing–aiming for perfect skin regeneration. Science 276, 75–81 (1997).
Bakay, M., Zhao, P., Chen, J. & Hoffman, E. P. A web-accessible complete transcriptome of normal human and DMD muscle. Neuromuscul. Disord. 12 (suppl. 1), S125–S141 (2002).
Hinz, B. Formation and function of the myofibroblast during tissue repair. J. Invest. Dermatol. 127, 526–537 (2007).
Willems, I. E. M. G., Havenith, M. G., Demey, J. G. R. & Daemen, M. J. A. P. The alpha-smooth muscle actin-positive cells in healing human myocardial scars. Am. J. Pathol. 145, 868–875 (1994).
Swift, J. et al. Nuclear lamin-A scales with tissue stiffness and enhances matrix-directed differentiation. Science 341, 1240104 (2013).
Kasahara, H., Bartunkova, S., Schinke, M., Tanaka, M. & Izumo, S. Cardiac and extracardiac expression of Csx/Nkx2.5 homeodomain protein. Circ. Res. 82, 936–946 (1998).
Pittenger, M. F. et al. Multilineage potential of adult human mesenchymal stem cells. Science 284, 143–147 (1999).
Hare, J. M. et al. A randomized, double-blind, placebo-controlled, dose-escalation study of intravenous adult human mesenchymal stem cells (prochymal) after acute myocardial infarction. J. Am. Coll. Cardiol. 54, 2277–2286 (2009).
Engler, A. J., Sen, S., Sweeney, H. L. & Discher, D. E. Matrix elasticity directs stem cell lineage specification. Cell 126, 677–689 (2006).
Shin, J. W. et al. Contractile forces sustain and polarize hematopoiesis from stem and progenitor cells. Cell Stem Cell 14, 81–93 (2014).
Gregory, C. A., Ylostalo, J. & Prockop, D. J. Adult bone marrow stem/progenitor cells (MSCs) are preconditioned by microenvironmental “niches” in culture: A two-stage hypothesis for regulation of MSC fate. Science STKE 2005, pe37 (2005).
Barberi, T., Willis, L. M., Socci, N. D. & Studer, L. Derivation of multipotent mesenchymal precursors from human embryonic stem cells. PLoS Med 2, 554–560 (2005).
Wong, S., Guo, W. H., Hoffecker, I. & Wang, Y. L. Preparation of a micropatterned rigid-soft composite substrate for probing cellular rigidity sensing. Methods Cell Biol. 121, 3–15 (2014).
Benoit, D. S., Schwartz, M. P., Durney, A. R. & Anseth, K. S. Small functional groups for controlled differentiation of hydrogel-encapsulated human mesenchymal stem cells. Nature Mater. 7, 816–823 (2008).
Huebsch, N. et al. Harnessing traction-mediated manipulation of the cell/matrix interface to control stem-cell fate. Nature Mater. 9, 518–526 (2010).
Khetan, S. et al. Degradation-mediated cellular traction directs stem cell fate in covalently crosslinked three-dimensional hydrogels. Nature Mater. 12, 458–465 (2013).
Trappmann, B. et al. Extracellular-matrix tethering regulates stem-cell fate. Nature Mater. 11, 642–649 (2012).
Dalby, M. J., Gadegaard, N. & Oreffo, R. O. Harnessing nanotopography and integrin-matrix interactions to influence stem cell fate. Nature Mater. 13, 558–569 (2014).
Corr, D. T., Gallant-Behm, C. L., Shrive, N. G. & Hart, D. A. Biomechanical behavior of scar tissue and uninjured skin in a porcine model. Wound Repair Regen. 17, 250–259 (2009).
Achterberg, V. F. et al. The nano-scale mechanical properties of the extracellular matrix regulate dermal fibroblast function. J. Invest. Dermatol. 134, 1862–1872 (2014).
MacQueen, L., Sun, Y. & Simmons, C. A. Mesenchymal stem cell mechanobiology and emerging experimental platforms. J. R. Soc. Interface 10, 20130179 (2013).
Dembo, M. & Wang, Y. L. Stresses at the cell-to-substrate interface during locomotion of fibroblasts. Biophys. J. 76, 2307–2316 (1999).
Storm, C., Pastore, J. J., MacKintosh, F. C., Lubensky, T. C. & Janmey, P. A. Nonlinear elasticity in biological gels. Nature 435, 191–194 (2005).
Vader, D., Kabla, A., Weitz, D. & Mahadevan, L. Strain-induced alignment in collagen gels. PLoS ONE 4, e5902 (2009).
Buxboim, A., Rajagopal, K., Brown, A. E. & Discher, D. E. How deeply cells feel: Methods for thin gels. J. Phys. Condens. Matter 22, 194116 (2010).
Engler, A. et al. Substrate compliance versus ligand density in cell on gel responses. Biophys. J. 86, 617–628 (2004).
Mann, C. J. et al. Aberrant repair and fibrosis development in skeletal muscle. Skeletal Muscle 1, 21 (2011).
Raab, M. et al. Crawling from soft to stiff matrix polarizes the cytoskeleton and phosphoregulates myosin-II heavy chain. J. Cell Biol. 199, 669–683 (2012).
Zemel, A., Rehfeldt, F., Brown, A. E. X., Discher, D. E. & Safran, S. A. Cell shape, spreading symmetry, and the polarization of stress-fibers in cells. J. Phys. Condens. Matter 22, 194110 (2010).
Schmiedel, J. M. et al. MicroRNA control of protein expression noise. Science 348, 128–132 (2015).
Rinkevich, Y. et al. Skin fibrosis. Identification and isolation of a dermal lineage with intrinsic fibrogenic potential. Science 348, aaa2151 (2015).
Miralles, F., Posern, G., Zaromytidou, A. I. & Treisman, R. Actin dynamics control SRF activity by regulation of its coactivator MAL. Cell 113, 329–342 (2003).
Dupont, S. et al. Role of YAP/TAZ in mechanotransduction. Nature 474, U179–U212 (2011).
Sullivan, K. E., Quinn, K. P., Tang, K. M., Georgakoudi, I. & Black, L. D. Extracellular matrix remodeling following myocardial infarction influences the therapeutic potential of mesenchymal stem cells. Stem Cell Res. Theory 5, 14 (2014).
Couzin-Frankel, J. The elusive heart fix. Science 345, 252–257 (2014).
Dingal, P. C. & Discher, D. E. Systems mechanobiology: Tension-inhibited protein turnover is sufficient to physically control gene circuits. Biophys. J. 107, 2734–2743 (2014).
Kasahara, H. & Izumo, S. Identification of the in vivo casein kinase II phosphorylation site within the homeodomain of the cardiac tissue-specifying homeobox gene product Csx/Nkx2.5. Mol. Cell. Biol. 19, 526–536 (1999).
Ryan, T. et al. Myosin phosphatase modulates the cardiac cell fate by regulating the subcellular localization of Nkx2.5 in a Wnt/Rho-associated protein kinase-dependent pathway. Circ. Res. 112, 257–266 (2013).
Yang, C., Tibbitt, M. W., Basta, L. & Anseth, K. S. Mechanical memory and dosing influence stem cell fate. Nature Mater. 13, 645–652 (2014).
Costa, M. W. et al. Complex SUMO-1 regulation of cardiac transcription factor Nkx2-5. PLoS ONE 6, e24812 (2011).
Breitbach, M. et al. Potential risks of bone marrow cell transplantation into infarcted hearts. Blood 110, 1362–1369 (2007).
Rehfeldt, F. et al. Hyaluronic acid matrices show matrix stiffness in 2D and 3D dictates cytoskeletal order and myosin-II phosphorylation within stem cells. Integr. Biol. 4, 422–430 (2012).
Addis, R. C. et al. Optimization of direct fibroblast reprogramming to cardiomyocytes using calcium activity as a functional measure of success. J. Mol. Cell. Cardiol. 60, 97–106 (2013).
Lo, C. M. et al. Nonmuscle myosin IIb is involved in the guidance of fibroblast migration. Mol. Biol. Cell 15, 982–989 (2004).
Domke, J. & Radmacher, M. Measuring the elastic properties of thin polymer films with the atomic force microscope. Langmuir 14, 3320–3325 (1998).
Acknowledgements
We thank H. Kasahara (University of Florida), H. L. Sweeney, C. Van Dang, J. D. Gearhart, A. Raj, and D. Lee (University of Pennsylvania), respectively, for NLS mutant NKX2.5 plasmids, normal and mdx mouse muscle, mouse liver tumour tissue, inducible NKX2.5 in virus, fluorescent probes against lamin-A mRNA, and help with peeling measurements. We thank the University of Pennsylvania’s Stem Cell Xenograft Core, Microscopy Core, and Microarray Core. We thank the Wistar Institute Proteomics Core for assistance with MS and standard data analyses. This work was supported by the National Institutes of Health, National Cancer Institute (grant U54-CA193417, D.E.D.), National Institute of Biomedical Imaging and Bioengineering (grant R01-EB007049, D.E.D.), National Heart, Lung, and Blood Institute (grant R01-HL124106, D.E.D.), National Institute of Diabetes and Digestive and Kidney Diseases (grants P01-DK032094 and P30-DK090969), National Center for Advancing Translational Sciences (grant 8UL1TR000003), the American Heart Association (14GRNT20490285, D.E.D.), the US/Israel Binational Science Foundation, and the National Science Foundation (1200834, Materials Research Science and Engineering Center, and Nano Science and Engineering Center-Nano Bio Interface Center).
Author information
Authors and Affiliations
Contributions
P.C.D.P.D., A.M.B., M.R. and A.B. performed experiments; P.C.D.P.D., S.C., A.B., J.S. and D.E.D. analysed results; P.C.D.P.D. and D.E.D. created figures and wrote the paper; and P.C.D.P.D. and D.E.D. designed the research.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Supplementary information
Supplementary Information
Supplementary Information (PDF 8914 kb)
Rights and permissions
About this article
Cite this article
Dingal, P., Bradshaw, A., Cho, S. et al. Fractal heterogeneity in minimal matrix models of scars modulates stiff-niche stem-cell responses via nuclear exit of a mechanorepressor. Nature Mater 14, 951–960 (2015). https://doi.org/10.1038/nmat4350
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/nmat4350
This article is cited by
-
Classes of Stem Cells: From Biology to Engineering
Regenerative Engineering and Translational Medicine (2023)
-
Inhibition of aberrant tissue remodelling by mesenchymal stromal cells singly coated with soft gels presenting defined chemomechanical cues
Nature Biomedical Engineering (2021)
-
Exercise enhances skeletal muscle regeneration by promoting senescence in fibro-adipogenic progenitors
Nature Communications (2020)
-
Mesenchymal stem cell perspective: cell biology to clinical progress
npj Regenerative Medicine (2019)
-
NKX2.5 is expressed in papillary thyroid carcinomas and regulates differentiation in thyroid cells
BMC Cancer (2018)