Abstract
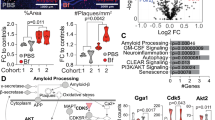
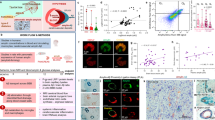
The amyloid-β protein (Aβ) protein plays a pivotal role in the pathogenesis of Alzheimer’s disease (AD). It is believed that Aβ deposited in the brain originates from the brain tissue itself. However, Aβ is generated in both brain and peripheral tissues. Whether circulating Aβ contributes to brain AD-type pathologies remains largely unknown. In this study, using a model of parabiosis between APPswe/PS1dE9 transgenic AD mice and their wild-type littermates, we observed that the human Aβ originated from transgenic AD model mice entered the circulation and accumulated in the brains of wild-type mice, and formed cerebral amyloid angiopathy and Aβ plaques after a 12-month period of parabiosis. AD-type pathologies related to the Aβ accumulation including tau hyperphosphorylation, neurodegeneration, neuroinflammation and microhemorrhage were found in the brains of the parabiotic wild-type mice. More importantly, hippocampal CA1 long-term potentiation was markedly impaired in parabiotic wild-type mice. To the best of our knowledge, our study is the first to reveal that blood-derived Aβ can enter the brain, form the Aβ-related pathologies and induce functional deficits of neurons. Our study provides novel insight into AD pathogenesis and provides evidence that supports the development of therapies for AD by targeting Aβ metabolism in both the brain and the periphery.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout





Similar content being viewed by others
References
Selkoe DJ. Alzheimer's disease: genes, proteins, and therapy. Physiol Rev 2001; 81: 741–766.
Zlokovic BV, Martel CL, Mackic JB, Matsubara E, Wisniewski T, McComb JG et al. Brain uptake of circulating apolipoproteins J and E complexed to Alzheimer's amyloid beta. Biochem Biophys Res Commun 1994; 205: 1431–1437.
Deane R, Zlokovic BV. Role of the blood-brain barrier in the pathogenesis of Alzheimer's disease. Curr Alzheimer Res 2007; 4: 191–197.
Kane MD, Lipinski WJ, Callahan MJ, Bian F, Durham RA, Schwarz RD et al. Evidence for seeding of beta-amyloid by intracerebral infusion of Alzheimer brain extracts in beta -amyloid precursor protein-transgenic mice. J Neurosci 2000; 20: 3606–3611.
Meyer-Luehmann M, Coomaraswamy J, Bolmont T, Kaeser S, Schaefer C, Kilger E et al. Exogenous induction of cerebral beta-amyloidogenesis is governed by agent and host. Science 2006; 313: 1781–1784.
Eisele YS, Obermuller U, Heilbronner G, Baumann F, Kaeser SA, Wolburg H et al. Peripherally applied Abeta-containing inoculates induce cerebral beta-amyloidosis. Science 2010; 330: 980–982.
Eisele YS, Fritschi SK, Hamaguchi T, Obermuller U, Fuger P, Skodras A et al. Multiple factors contribute to the peripheral induction of cerebral beta-amyloidosis. J Neurosci 2014; 34: 10264–10273.
Jucker M, Walker LC. Self-propagation of pathogenic protein aggregates in neurodegenerative diseases. Nature 2013; 501: 45–51.
Jaunmuktane Z, Mead S, Ellis M, Wadsworth JD, Nicoll AJ, Kenny J et al. Evidence for human transmission of amyloid-beta pathology and cerebral amyloid angiopathy. Nature 2015; 525: 247–250.
Ritchie DL, Adlard P, Peden AH, Lowrie S, Le Grice M, Burns K et al. Amyloid-beta accumulation in the CNS in human growth hormone recipients in the UK. Acta Neuropathol 2017; 134: 221–240.
Li QX, Evin G, Small DH, Multhaup G, Beyreuther K, Masters CL. Proteolytic processing of Alzheimer's disease beta A4 amyloid precursor protein in human platelets. J Biol Chem 1995; 270: 14140–14147.
Evin G, Zhu A, Holsinger RM, Masters CL, Li QX. Proteolytic processing of the Alzheimer's disease amyloid precursor protein in brain and platelets. J Neurosci Res 2003; 74: 386–392.
Citron M, Vigo-Pelfrey C, Teplow DB, Miller C, Schenk D, Johnston J et al. Excessive production of amyloid beta-protein by peripheral cells of symptomatic and presymptomatic patients carrying the Swedish familial Alzheimer disease mutation. Proc Natl Acad Sci USA 1994; 91: 11993–11997.
Kuo YM, Kokjohn TA, Watson MD, Woods AS, Cotter RJ, Sue LI et al. Elevated abeta42 in skeletal muscle of Alzheimer disease patients suggests peripheral alterations of AbetaPP metabolism. Am J Pathol 2000; 156: 797–805.
Van Nostrand WE, Melchor JP. Disruption of pathologic amyloid beta-protein fibril assembly on the surface of cultured human cerebrovascular smooth muscle cells. Amyloid 2001; 8(Suppl 1): 20–27.
Xiang Y, Bu XL, Liu YH, Zhu C, Shen LL, Jiao SS et al. Physiological amyloid-beta clearance in the periphery and its therapeutic potential for Alzheimer's disease. Acta Neuropathol 2015; 130: 487–499.
Jin WS, Shen LL, Bu XL, Zhang WW, Chen SH, Huang ZL et al. Peritoneal dialysis reduces amyloid-beta plasma levels in humans and attenuates Alzheimer-associated phenotypes in an APP/PS1 mouse model. Acta Neuropathol 2017; 134: 207–220.
Harris RB, Martin RJ. Specific depletion of body fat in parabiotic partners of tube-fed obese rats. Am J Physiol 1984; 247(Pt 2): R380–R386.
Harris RB. Parabiosis between db/db and ob/ob or db/+ mice. Endocrinology 1999; 140: 138–145.
Nilsson LN, Gografe S, Costa DA, Hughes T, Dressler D, Potter H. Use of fused circulations to investigate the role of apolipoprotein E as amyloid catalyst and peripheral sink in Alzheimer's disease. Technol Innov 2012; 14: 199–208.
Wu X, Bai Y, Tan T, Li H, Xia S, Chang X et al. Lithium ameliorates autistic-like behaviors induced by neonatal isolation in rats. Front Behav Neurosci 2014; 8: 234.
Bliss TV, Collingridge GL. A synaptic model of memory: long-term potentiation in the hippocampus. Nature 1993; 361: 31–39.
Mandybur TI. The incidence of cerebral amyloid angiopathy in Alzheimer's disease. Neurology 1975; 25: 120–126.
Esiri MM, Wilcock GK. Cerebral amyloid angiopathy in dementia and old age. J Neurol Neurosurg Psychiatry 1986; 49: 1221–1226.
Ellis RJ, Olichney JM, Thal LJ, Mirra SS, Morris JC, Beekly D et al. Cerebral amyloid angiopathy in the brains of patients with Alzheimer's disease: the CERAD experience, Part XV. Neurology 1996; 46: 1592–1596.
Brenowitz WD, Nelson PT, Besser LM, Heller KB, Kukull WA. Cerebral amyloid angiopathy and its co-occurrence with Alzheimer's disease and other cerebrovascular neuropathologic changes. Neurobiol Aging 2015; 36: 2702–2708.
Duyckaerts C, Potier MC, Delatour B. Alzheimer disease models and human neuropathology: similarities and differences. Acta Neuropathol 2008; 115: 5–38.
Bates KA, Verdile G, Li QX, Ames D, Hudson P, Masters CL et al. Clearance mechanisms of Alzheimer's amyloid-beta peptide: implications for therapeutic design and diagnostic tests. Mol Psychiatry 2009; 14: 469–486.
Rosen RF, Fritz JJ, Dooyema J, Cintron AF, Hamaguchi T, Lah JJ et al. Exogenous seeding of cerebral beta-amyloid deposition in betaAPP-transgenic rats. J Neurochem 2012; 120: 660–666.
Morales R, Duran-Aniotz C, Castilla J, Estrada LD, Soto C. De novo induction of amyloid-beta deposition in vivo. Mol Psychiatry 2012; 17: 1347–1353.
Frontzek K, Lutz MI, Aguzzi A, Kovacs GG, Budka H. Amyloid-beta pathology and cerebral amyloid angiopathy are frequent in iatrogenic Creutzfeldt-Jakob disease after dural grafting. Swiss Med Wkly 2016; 146: w14287.
Jankowsky JL, Slunt HH, Ratovitski T, Jenkins NA, Copeland NG, Borchelt DR. Co-expression of multiple transgenes in mouse CNS: a comparison of strategies. Biomol Eng 2001; 17: 157–165.
Fukuchi K, Ho L, Younkin SG, Kunkel DD, Ogburn CE, LeBoeuf RC et al. High levels of circulating beta-amyloid peptide do not cause cerebral beta-amyloidosis in transgenic mice. Am J Pathol 1996; 149: 219–227.
Jankowsky JL, Younkin LH, Gonzales V, Fadale DJ, Slunt HH, Lester HA et al. Rodent A beta modulates the solubility and distribution of amyloid deposits in transgenic mice. J Biol Chem 2007; 282: 22707–22720.
Li QX, Whyte S, Tanner JE, Evin G, Beyreuther K, Masters CL. Secretion of Alzheimer's disease Abeta amyloid peptide by activated human platelets. Lab Invest 1998; 78: 461–469.
Selkoe DJ, Podlisny MB, Joachim CL, Vickers EA, Lee G, Fritz LC et al. Beta-amyloid precursor protein of Alzheimer disease occurs as 110- to 135-kilodalton membrane-associated proteins in neural and nonneural tissues. Proc Natl Acad Sci USA 1988; 85: 7341–7345.
Sandbrink R, Masters CL, Beyreuther K. Beta A4-amyloid protein precursor mRNA isoforms without exon 15 are ubiquitously expressed in rat tissues including brain, but not in neurons. J Biol Chem 1994; 269: 1510–1517.
Chen M, Inestrosa NC, Ross GS, Fernandez HL. Platelets are the primary source of amyloid beta-peptide in human blood. Biochem Biophys Res Commun 1995; 213: 96–103.
Liu WW, Todd S, Craig D, Passmore AP, Coulson DT, Murphy S et al. Elevated platelet beta-secretase activity in mild cognitive impairment. Dement Geriatr Cogn Disord 2007; 24: 464–468.
Johnston JA, Liu WW, Coulson DT, Todd S, Murphy S, Brennan S et al. Platelet beta-secretase activity is increased in Alzheimer's disease. Neurobiol Aging 2008; 29: 661–668.
Li S, Liu B, Zhang L, Rong L. Amyloid beta peptide is elevated in osteoporotic bone tissues and enhances osteoclast function. Bone 2014; 61: 164–175.
Zhou R, Deng J, Zhang M, Zhou HD, Wang YJ. Association between bone mineral density and the risk of Alzheimer's disease. J Alzheimers Dis 2011; 24: 101–108.
Tarasoff-Conway JM, Carare RO, Osorio RS, Glodzik L, Butler T, Fieremans E et al. Clearance systems in the brain-implications for Alzheimer disease. Nat Rev Neurol 2015; 11: 457–470.
Zlokovic BV, Deane R, Sagare AP, Bell RD, Winkler EA. Low-density lipoprotein receptor-related protein-1: a serial clearance homeostatic mechanism controlling Alzheimer's amyloid beta-peptide elimination from the brain. J Neurochem 2010; 115: 1077–1089.
Storck SE, Meister S, Nahrath J, Meissner JN, Schubert N, Di Spiezio A et al. Endothelial LRP1 transports amyloid-beta(1-42) across the blood-brain barrier. J Clin Invest 2016; 126: 123–136.
Elali A, Rivest S. The role of ABCB1 and ABCA1 in beta-amyloid clearance at the neurovascular unit in Alzheimer's disease. Front Physiol 2013; 4: 45.
Do TM, Noel-Hudson MS, Ribes S, Besengez C, Smirnova M, Cisternino S et al. ABCG2- and ABCG4-mediated efflux of amyloid-beta peptide 1-40 at the mouse blood-brain barrier. J Alzheimers Dis 2012; 30: 155–166.
Deane R, Du Yan S, Submamaryan RK, LaRue B, Jovanovic S, Hogg E et al. RAGE mediates amyloid-beta peptide transport across the blood-brain barrier and accumulation in brain. Nat Med 2003; 9: 907–913.
Bu XL, Yao XQ, Jiao SS, Zeng F, Liu YH, Xiang Y et al. A study on the association between infectious burden and Alzheimer's disease. Eur J Neurol 2015; 22: 1519–1525.
Wang YR, Wang QH, Zhang T, Liu YH, Yao XQ, Zeng F et al. Associations between hepatic functions and plasma amyloid-beta levels—implications for the capacity of liver in peripheral amyloid-beta clearance. Mol Neurobiol 2016; 54: 2338–2344.
Bu XL, Cao GQ, Shen LL, Xiang Y, Jiao SS, Liu YH et al. Serum amyloid-beta levels are increased in patients with chronic obstructive pulmonary disease. Neurotox Res 2015; 28: 346–351.
Troncone L, Luciani M, Coggins M, Wilker EH, Ho CY, Codispoti KE et al. Abeta amyloid pathology affects the hearts of patients with Alzheimer's disease: mind the heart. J Am Coll Cardiol 2016; 68: 2395–2407.
Wang J, Gu B, Masters CL, Wang YJ. A systemic view of Alzheimer's disease: insights from amyloid-beta metabolism beyond the brain. Nat Rev Neurol 2017; 13: 612–623.
Acknowledgments
This study was supported by National Natural Science Foundation of China (NSFC) Grant 81701043 (to X-LB) and 81625007 (to Y-JW) and 81622015 (to Z-FD), and Canadian Institutes of Health Research (CIHR) Grant TAD-117948 (to WS). WS is the holder of the Tier 1 Canada Research Chair in Alzheimer’s Disease.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of Interest
The authors declare no conflict of interest.
Electronic supplementary material
Rights and permissions
About this article
Cite this article
Bu, XL., Xiang, Y., Jin, WS. et al. Blood-derived amyloid-β protein induces Alzheimer’s disease pathologies. Mol Psychiatry 23, 1948–1956 (2018). https://doi.org/10.1038/mp.2017.204
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/mp.2017.204
This article is cited by
-
Peripheral extracellular vesicles in neurodegeneration: pathogenic influencers and therapeutic vehicles
Journal of Nanobiotechnology (2024)
-
Peripheral blood amyloid-β involved in the pathogenesis of Alzheimer’s disease via impacting on peripheral innate immune cells
Journal of Neuroinflammation (2024)
-
A multi-cohort study of the hippocampal radiomics model and its associated biological changes in Alzheimer’s Disease
Translational Psychiatry (2024)
-
Aβ-Aggregation-Generated Blue Autofluorescence Illuminates Senile Plaques as well as Complex Blood and Vascular Pathologies in Alzheimer’s Disease
Neuroscience Bulletin (2024)
-
Healthy blood, healthy brain: a window into understanding and treating neurodegenerative diseases
Journal of Neurology (2024)