Abstract
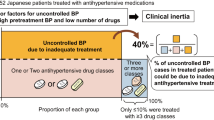
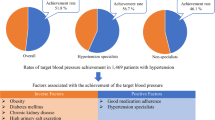
Insufficient awareness of hypertension guidelines by physicians may be an impediment to achieving adequate blood pressure (BP) control rates in clinical practice. We therefore conducted an open intervention survey among primary care physicians in 1596 centres from 16 countries in four different continents to prospectively assess what is the BP goal defined by physicians for individual patients and what are the reasons for not intensifying antihypertensive treatment when BP goals are not achieved. Enrolled patients (N=35 302) were either not treated to goal (N=22 887) or previously untreated (N=12 250). Baseline systolic and diastolic BP averaged 159/95±15/12 mm Hg. BP goals defined by physicians averaged 136±6 mm Hg for systolic and 86±5 mm Hg for diastolic BP. Patients' individual risk stratification determined BP goals. At last visit BP averaged 132/81±11/8 mm Hg and values of ⩽140/90 were reached in 92% of untreated and 80% of previously uncontrolled treated hypertensives. The main reasons for not intensifying antihypertensive treatment when BP remained above goal were the assumption that the time after starting the new drug was too short to attain its full effect, the satisfaction with a clear improvement of BP or with a BP nearing the goal, and the acceptance of good self-measurements. In this open intervention program in primary care, a large proportion of patients achieved recommended BP goals. The belief that a clear improvement in BP is acceptable and that the full drug effect may take up to several weeks to be reached are frequent reasons for treatment inertia when goals are not achieved.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 digital issues and online access to articles
$119.00 per year
only $9.92 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Chobanian AV, Bakris GL, Black HR, Cushman WC, Green LA, Izzo Jr JL et al. Seventh report of the Joint National Committee on prevention, detection, evaluation, and treatment of high blood pressure. Hypertension 2003; 42: 1206–1252.
Whitworth JA . 2003 World Health Organization (WHO)/International Society of Hypertension (ISH) statement on management of hypertension. J Hypertens 2003; 21: 1983–1992.
JNC 6. National High Blood Pressure Education Program. The Sixth Report of the Joint National Committee on prevention, detection, evaluation, and treatment of high blood pressure. Arch Intern Med 1997; 157: 2413–2446.
Hajjar I, Kotchen TA . Trends in prevalence, awareness, treatment, and control of hypertension in the United States, 1988–2000. JAMA 2003; 290: 199–206.
Ferrari P, Hess L, Pechere-Bertschi A, Muggli F, Burnier M . Reasons for not intensifying antihypertensive treatment (RIAT): a primary care antihypertensive intervention study. J Hypertens 2004; 22: 1221–1229.
Dusing R, Weisser B, Mengden T, Vetter H . Changes in antihypertensive therapy—the role of adverse effects and compliance. Blood Press 1998; 7: 313–315.
Degli Esposti E, Sturani A, Di Martino M, Falasca P, Novi MV, Baio G et al. Long-term persistence with antihypertensive drugs in new patients. J Hum Hypertens 2002; 16: 439–444.
Hyman DJ, Pavlik VN . Self-reported hypertension treatment practices among primary care physicians: blood pressure thresholds, drug choices, and the role of guidelines and evidence-based medicine. Arch Intern Med 2000; 160: 2281–2286.
Hyman DJ, Pavlik VN . Characteristics of patients with uncontrolled hypertension in the United States. N Engl J Med 2001; 345: 479–486.
Okonofua EC, Simpson KN, Jesri A, Rehman SU, Durkalski VL, Egan BM . Therapeutic inertia is an impediment to achieving the Healthy People 2010 blood pressure control goals. Hypertension 2006; 47: 345–351.
Ferrari P, Kim SK, Wu CJ, Pham NV, Ageev F, Hermosillo LD et al. Aim, design and methods of the ‘reasons for not intensifying antihypertensive treatment’ (RIAT): an international registry in essential hypertension. J Hum Hypertens 2006; 20: 31–36.
Rehman SU, Hutchison FN, Hendrix K, Okonofua EC, Egan BM . Ethnic differences in blood pressure control among men at Veterans Affairs clinics and other health care sites. Arch Intern Med 2005; 165: 1041–1047.
Burt VL, Whelton P, Roccella EJ, Brown C, Cutler JA, Higgins M et al. Prevalence of hypertension in the US adult population. Results from the Third National Health and Nutrition Examination Survey, 1988–1991. Hypertension 1995; 25: 305–313.
The ALLHAT Officers and Coordinators for the ALLHAT Collaborative Research Group. Major outcomes in high-risk hypertensive patients randomized to angiotensin-converting enzyme inhibitor or calcium channel blocker vs diuretic: The Antihypertensive and Lipid-Lowering Treatment to Prevent Heart Attack Trial (ALLHAT). JAMA 2002; 288: 2981–2997.
Julius S, Kjeldsen SE, Weber M, Brunner HR, Ekman S, Hansson L et al. Outcomes in hypertensive patients at high cardiovascular risk treated with regimens based on valsartan or amlodipine: the VALUE randomised trial. Lancet 2004; 363: 2022–2031.
Poulter NR, Wedel H, Dahlöf B, Sever PS, Beevers DG, Caulfield M et al. Role of blood pressure and other variables in the differential cardiovascular event rates noted in the Anglo-Scandinavian Cardiac Outcomes Trial-Blood Pressure Lowering Arm (ASCOT-BPLA). Lancet 2005; 366: 907–913.
Hagemeister J, Schneider CA, Barabas S, Schadt R, Wassmer G, Mager G et al. Hypertension guidelines and their limitations--the impact of physicians' compliance as evaluated by guideline awareness. J Hypertens 2001; 19: 2079–2086.
Oliveria SA, Lapuerta P, McCarthy BD, L'Italien GJ, Berlowitz DR, Asch SM . Physician-related barriers to the effective management of uncontrolled hypertension. Arch Intern Med 2002; 162: 413–420.
Lee JK, Grace KA, Taylor AJ . Effect of a pharmacy care program on medication adherence and persistence, blood pressure, and low-density lipoprotein cholesterol: a randomized controlled trial. JAMA 2006; 296: 2563–2571.
Burnier M . Medication adherence and persistence as the cornerstone of effective antihypertensive therapy. Am J Hypertens 2006; 19: 1190–1196.
Preston RA, Materson BJ, Reda DJ, Williams DW . Placebo-associated blood pressure response and adverse effects in the treatment of hypertension: observations from a Department of Veterans Affairs Cooperative Study. Arch Intern Med 2000; 160: 1449–1454.
Nietert PJ, Wessell AM, Feifer C, Ornstein SM . Effect of terminal digit preference on blood pressure measurement and treatment in primary care. Am J Hypertens 2006; 19: 147–152.
Graves JW, Bailey KR, Grossardt BR, Gullerud RE, Meverden RA, Grill DE et al. The impact of observer and patient factors on the occurrence of digit preference for zero in blood pressure measurement in a hypertension specialty clinic: evidence for the need of continued observation. Am J Hypertens 2006; 19: 567–572.
Cranney M, Warren E, Barton S, Gardner K, Walley T . Why do GPs not implement evidence-based guidelines? A descriptive study. Fam Pract 2001; 18: 359–363.
Burnier M . Blood pressure control and the implementation of guidelines in clinical practice: can we fill the gap? J Hypertens 2002; 20: 1251–1253.
Romain TM, Patel RP, Heaberlin AM, Zarowitz BJ . Assessment of factors influencing blood pressure control in a managed care population. Pharmacotherapy 2003; 23: 1060–1070.
Carter BL . Implementing the new guidelines for hypertension: JNC 7, ADA, WHO-ISH. J Manag Care Pharm 2004; 10: S18–S25.
Acknowledgements
This study was supported by Sanofi-Aventis Intercontinental. We acknowledge the 1596 centres who participated in the RIAT study: Argentina (13), China (92), Colombia (57), Dominican Republic (4), Indonesia (114), Korea (808), Lebanon (103), Malaysia (117), Mexico (76), Morocco (41), Philippines (9), Russia (53), Saudi Arabia (10), Singapore (18), Taiwan (56) and Vietnam (25).
Author information
Authors and Affiliations
Consortia
Corresponding author
Additional information
Disclosure
PF has acted as a consultant for Sanofi-Aventis.
Appendix
Appendix
National Coordinators
Argentina: R Esper, Clinica Cardiovascular, Buenos Aires. China: P Changyu, Department of Endocrinology, Beijing; L Shanyan, Nephrology Research Institute, Shanghai; Q WenHang, Department of Cardiology, Shanghai. Colombia: J Duperly, Asociacion Medica de Los Andes, Bogota. Dominican Republic: E Dina, Clinica Corominas, Santiago. Indonesia: M Yogiarto, Department of Cardiology, Dr Soetomo Hospital, Surabaya. Korea: JH Kim, Department of Medicine, St Paul's Hospital, Seoul; SK Kim, Department of Cardiology, Hanyang University, Seoul. Lebanon: A Berberi, Division of Hypertension and Vascular Medicine, American Hospital, Beirut. Malaysia: AM Daud, Gleneagles Intan Medical Center, Kuala Lumpur; Z Morad, International Medical University, Negeri Sembilan. Mexico: MA Mendez Bello, Puebla. Morocco: M Alami, Casablanca. Russia: F Ageev, Cardiology Research Center, Moscow. Saudi Arabia: MH Odeh, Dr. Sulaiman Al-Habib Medical Center, Riyadh. Singapore: P Yan, Peter Yan Cardiology Clinic, Singapore. Taiwan: CJ Wu, Chang Gung Memorial Hospital, Taipei. Vietnam: NV Pham, Heart Institute, Ho Chi Minh City.
Rights and permissions
About this article
Cite this article
Ferrari, P., the National Coordinators for the Reasons for not Intensifying Antihypertensive Treatment (RIAT) trial. Reasons for therapeutic inertia when managing hypertension in clinical practice in non-Western countries. J Hum Hypertens 23, 151–159 (2009). https://doi.org/10.1038/jhh.2008.117
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/jhh.2008.117
Keywords
This article is cited by
-
Management of Hypertension in the Asia-Pacific Region: A Structured Review
American Journal of Cardiovascular Drugs (2024)
-
Polypills for primary prevention of cardiovascular disease
Nature Reviews Cardiology (2019)
-
Resistant Hypertension and Chronic Kidney Disease: a Dangerous Liaison
Current Hypertension Reports (2016)
-
Impact of ethnic-specific guidelines for anti-hypertensive prescribing in primary care in England: a longitudinal study
BMC Health Services Research (2014)
-
The concept and definition of therapeutic inertia in hypertension in primary care: a qualitative systematic review
BMC Family Practice (2014)