Abstract
Despite the numerous common pathways connecting blood pressure regulation to somatostatin (SST) metabolism, the SST gene has never been seen as a significant blood pressure modulator. The aim of this study was to evaluate the association between a poly-T repeat sequence (rs34872250) in the promoter of the SST gene and blood pressure, according to the obesity status. We genotyped 1918 French-Canadian subjects from a founder population. Analyses were performed according to the length of the poly-T repeat sequence on both alleles and divided into two groups, the 13/13–13/14 group and the 13/15–13/16 group. The effect of age, gender, body mass index, antihypertensive drugs and diabetic status were considered. Systolic, diastolic and mean blood pressures are significantly higher among the 13/15–13/16 group in the whole sample (P<0.05). Whereas the differences remain significant in women, they turn to be non-significant when men are considered alone. The risk of hypertension is increased in the 13/15–13/16 group, particularly among overweight/obese subjects. Systolic blood pressure is significantly higher among overweight/obese carriers of the 13/15–13/16 alleles in the whole sample (P<0.001), in men (P=0.006) and in women (P=0.002), even after correction for age and antihypertensive drugs. These results suggest that the poly-T repeat sequence polymorphism in the promoter of the SST gene is associated with significant variations of blood pressure and could modulate the risk of hypertension, particularly among women.
Similar content being viewed by others
Introduction
Blood pressure is a highly variable trait with a strong and continuous association with cardiovascular disease (CVD), even in the normotensive range. Blood pressure is known to be influenced by several secondary factors, such as obesity, dyslipidemia, insulin resistance and type 2 diabetes (T2D).1 However, high blood pressure is often observed in the absence of known secondary factors: this is called essential hypertension.2 Essential hypertension accounts for almost 90% of all cases of hypertension and affects a large proportion of the adult population.3 Although it is frequently stated that the causes of essential hypertension are not known, some information suggests that genetic variations and intermediate phenotypes may interact to increase blood pressure.4 However, the genetic etiology of blood pressure variability is difficult to document. It may vary among different populations and may be dependent on the complex interactions between genes and the environment.4, 5
The linkage analysis we performed on hypertension and glycerolemia following a genome-wide microsatellite marker scan among 38 families has provided evidence for a susceptibility locus to blood pressure on chromosome 3q27 (unpublished data). A candidate gene approach for this region has led us to target the somatostatin (SST) gene.
SST, a natural and ubiquitous peptide, is the most effective inhibitor of growth hormone (GH) release. It exerts a negative action on a variety of physiological functions in the central nervous system, the pancreas and the gastrointestinal tract.6 SST influences somatic growth and body weight by regulating the intestinal absorption of nutrients, gastrointestinal motility, food intake and energy homeostasis.7, 8, 9 It induces the inhibition of both insulin and glucagon production7 and limits the absorption of carbohydrates and triglycerides in the small intestine.10 It has been used as a therapy in the management of obesity and T2D.11 Moreover, SST analogs have been shown to decrease plasma renin activity and water absorption in the kidneys, which could result in decreased vascular filling and secondary fall in portal pressure in patient with cirrhosis.8 The use of SST analogs has also resulted in a significant and sustained improvement of idiopathic intracranial hypertension.12 A direct action of SST on the vascular smooth muscle has been proposed, but other investigations have found no local effect of SST on the splanchnic vasculature.8, 13, 14 However, it has been proposed that SST may facilitate vasoconstrictors, such as protein kinase C or endothelin-1, which are already increased in patients with chronic hepatic diseases.15
A sequence analysis in a subsample of subjects has led us to identify various polymorphisms in the SST gene and, among them, a poly-T repeat sequence in the promoter. A total of 13 different genotypes associated with 6 alleles, ranging from 12 T to 17 T, were observed, suggesting that this sequence could be highly polymorphic in the general population (unpublished data). Although this polymorphism was previously identified (rs34872250), to the best of our knowledge, its effects have never been published. Considering (1) the involvement of SST in various blood pressure-related metabolic pathways, (2) the association of the 3q27 linkage peak with hypertension and hyperglycerolemia and (3) the association between glycerol and body composition, we hypothesized that the SST poly-T repeat sequence is a significant modulator of blood pressure, particularly among obese people.
The aim of the present study was therefore to investigate the relationship between the poly-T repeat polymorphism in the promoter of the SST gene and blood pressure, according to obesity status.
Methods
Subjects and clinical data
This study comprised a sample of 1918 French-Canadian subjects from the Saguenay-Lac-Saint-Jean region of Quebec (Canada) selected on the basis of having a positive family history of dyslipidemia or coronary artery diseases. All subjects had agreed to participate in studies on genetic determinants of T2D or coronary artery disease combining genome-wide association studies and candidate gene strategies.16, 17 T2D was defined according to the World Health Organization criteria as a 2-h glucose concentration ⩾11.1 mmol l−1 following a 75-g oral glucose load, whereas a normal glucose tolerance state was characterized as a 2-h glucose concentration <7.8 mmol l−1. Subjects with fasting triglyceride levels >20 mmol l−1 or body mass index (BMI) >40 kg m−2, those taking drugs known to affect blood lipid levels and those known to have abusive alcohol consumption were excluded. Body weight, height and waist girth were determined according to the procedures of the Airlie conference.18 Subjects gave their informed consent to participate in this study and were assigned a code that systematically de-identifies all clinical data.19 This project received the approval of the Chicoutimi Hospital Ethics Committee and was conducted in accordance with the Declaration of Helsinki.
Biochemical analysis
Blood samples were obtained after a 12-h overnight fast from the antecubital vein into vacutainer tubes containing EDTA. Cholesterol, triglyceride and glucose levels were measured by enzymatic assays on a CX7Analyser (Beckman, Fullerton, CA, USA).20 Total cholesterol was determined in plasma and high-density lipoprotein (HDL) after precipitation of very low-density lipoproteins (LDLs) and LDLs (d>1.006 g ml−1) in the infranatant with dextran sulfate and magnesium chloride (MgCl2). In this case, plasma LDL-cholesterol levels were estimated using the Friedewald formula.21 When triglycerides levels were >4.5 mmol l−1, plasma LDL-cholesterol levels were calculated using a validated method.22
Microsatellite analysis
The length of the poly-T sequence was determined by DNA sequencing using the BigDye Terminator Kit (Applied Biosystems Instruments, ABI, Foster City, CA, USA). The size standard was produced by PCR amplification of each individual clone with fluorescent label. Sample electrophoresis and data analysis PCR products were resolved and detected by capillary electrophoresis using the ABI PRISM 3100 Genetic Analyzer, a multi-color fluorescence-based DNA analysis system with 16 capillaries operating in parallel, with denaturing polymer POP4 (Perkin-Elmer, Shelton, CT, USA). Fragment sizing was supported using the Genescan (ABI).
Blood pressure measurements
Blood pressure was taken by trained certified personnel according to the American Heart Association guidelines by the Shared Care Method using a sphygmomanometer (Omron Healthcare Inc., Vernon Hills, IL, USA).23 After being seated for at least 5 min, two readings were obtained from each arm of the subject using an appropriately sized arm cuff. The average of the arm with the higher measurement was used for the visit reading. The diagnosis was made when the average of ⩾2 measurements of blood pressure, on at least two subsequent visits, were >140 mm Hg for systolic blood pressure or >90 mm Hg for diastolic blood pressure. 24 Those subjects already being treated for hypertension were immediately recognized as achieved and included as hypertensive subjects. Mean arterial pressure (MAP) was calculated as follows: MAP=((2 × diastolic)+systolic)/3.25
Statistical analysis
Differences in continuous variables were compared by T-tests or analysis of variance, whereas the Chi square (χ2) statistic was used to compare categorical variables. Logistic regression was used in order to estimate the relative risk of hypertension according to the SST poly-T repeat polymorphism between normal and overweight/obese individuals. All statistical analyses were performed with the SPSS package (release 11.5, SPSS, Chicago, IL, USA).
Results
We found six alleles ranging from 12 T to 17 T in the 5′ middle region of the SST gene promoter (Table 1). Three alleles were more frequent: 13, 15, and 16. Based on the allele frequency and data in public databases, we hypothesized that the 13 T polymorphism was the wild-type allele. We therefore selected the 13 T or 14 T sequence for the first allele and the 15 T or 16 T sequences for the second allele. We compared carriers of the 13/13 or 13/14 alleles to carriers of 15/15, 15/16 or 16/16. The analysis showed that systolic, diastolic and mean arterial blood pressures as well as the prevalence of hypertension tend to be higher in the last group (data not shown) without, however, reaching a significant level (α=0.05). The small sample size, especially when men and women are considered separately, and large heterogeneity could explain such results. According to our results, the 15/15, 15/16 or 16/16 ‘homozygotes’ seem to have a phenotype that tends to be similar to that of 13/15 or 13/16 ‘heterozygotes’. However, our results did not allow us to conclude beyond a reasonable doubt that grouping 15/15-15/16-16/16 subjects with the 13/15-13/16 subjects strategy is a scientifically sound strategy. Considering the small size of the 15/15-15/16-16/16 group, we therefore decided to exclude these subjects. The analyses were performed on the remaining subjects (901 men and 824 women) who represented almost 90% of the total sample. Two groups were then created based on preliminary analyses: Group 1, composed of 13/13 and 13/14 genotypes, and Group 2, composed of 13/15 and 13/16 genotypes.
Subjects’ characteristics are shown in Table 2a. Systolic (P<0.001), diastolic (P=0.04) and MAP (P<0.001) were significantly higher among Group 2 in the whole sample. These differences were also observed in women, in addition to significant differences in fasting glycemia (P=0.02). Furthermore, more women with hypertension (P<0.001), BMI⩾25 (P=0.005) and T2D (P=0.004) were observed in Group 2. In men, only systolic blood pressure was significantly different between the two groups when adjusted for antihypertensive drugs and waist girth (P=0.048). There was no significant difference in antihypertensive medication class according to the SST poly-A repeat polymorphism (Table 2b).
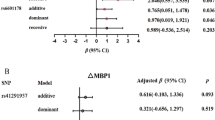
Table 3 shows that Group 2 subjects (13/15–13/16) are exposed to an increased risk of exhibiting hypertension if they are also overweight/obese. The odds ratio (OR) remained comparable even when confounders such as age, sex and T2D were added to the model. However, according to the 95% confidence interval, the OR associated with the Group 2 genotypes was not significantly different from the one associated with Group 1 among obese/overweight. Although these trends remained the same for both genders, the increase tended to be stronger in women (OR=4.01; P<0.001) than in men (OR=1.68; P=0.027). Moreover, we observed a significant (P<0.001) interactive effect between polymorphism and gender on the OR of hypertension (data not shown).
As shown in Figure 1, there are more hypertensive subjects among the overweight/obese carriers of the 13/15 or 13/16 genotypes. However, results reached significant levels only in women (P=0.010) and the whole sample (P=0.006).
Systolic blood pressure (Figure 2) is significantly increased among overweight/obese carriers of the 13/15 or 13/16 genotypes in the whole sample (P<0.001), men (P=0.006) and women (P=0.02). The results remained significant even after adjusting for the effects of age and antihypertension medication. In women, the increase was also significant in normal weight (P=0.027) subjects.
Figure 3 shows that MAP was significantly increased among women carrier of the 13/15 and 13/16 genotypes, whether they were overweight/obese (P=0.003) or not (P=0.034). The results remained significant even after adjusting for the effects of age and antihypertensive medication, except for normal weight women.
Discussion
Our results show that the length of the poly-T repeat polymorphism in the promoter of the SST gene is associated with an increase in arterial blood pressure and risk of hypertension, especially among women and overweight/obese individuals. To the best of our knowledge, these are the first results on the effects of a SST gene polymorphism on hypertension. Considering the increasing burden of obesity, not only in occidental populations but also in the whole world, combined to the apparent high frequency of this polymorphism, this association could bear a significant population attributable risk.
Among all variables associated with hypertension, the main recognized hypertensinogenic factor remains obesity.26 Our results have shown that the carriers of the SST poly-T repeat polymorphism in the 13/15–13/16 group have a greater risk of hypertension, present a greater proportion of hypertension diagnosis and show higher systolic and MAP especially when their BMI is >25 kg m−2. These results are consistent with those of other studies which proposed that the joint effect of genetic and environmental factors strengthens the association with the disease and may influence the individual’s risk of being affected.27
SST is mainly produced in the central and peripheral nervous system and the gastrointestinal tract. Its possible endocrine, paracrine or neurocrine secretions and its short half-life prevent the simple evaluation of plasma levels from being a reliable indicator of its function. SST could be related to blood pressure control via various pathways. It was suggested that the inhibitory effect of SST on the release of glucagon was the principal mechanism by which SST causes the splanchnic vasoconstriction used to treat portal hypertension. SST has also been shown to decrease plasma renin activity and water absorption in the kidneys.7 But evidence also exists for a local vasoconstrictive effect of SST on vascular smooth muscle cells, particularly in the presence of other vasoconstrictors.28, 29 Besides, the 3q27 linkage peak that led us to target SST was associated not only with hypertension but also with glycerol. Glycerol is inversely correlated to total body water and positively correlated to fat mass, in addition to be closely correlated to various blood pressure-related metabolic pathways.30 Those effects seem consistent with the association between increased arterial blood pressure and body composition with SST overproduction and its correlate, GH deficiency.31, 32
Our study points toward a significant interaction effect between gender and SST polymorphism on hypertension. This effect could be due, in part, to the link between SST and GH. SST was first defined as an inhibitor of GH secretion. GH is a pituitary hormone that exerts its biological action on almost every cell and has an important role in the control of metabolic processes.33 GH is regulated by the interplay of both GH-releasing hormone and SST. This hormone is known to have a release of a pulsatile nature that is gender dependent. In general, women display more frequent, but irregular, GH pulse release and higher baseline levels. It has been hypothesized that this increase is due to a decrease in SST output from the hypothalamus.34 It can therefore be suggested that GH production is decreased in Group 2, particularly when the poly-T repeat polymorphism is associated with overweight/obesity, as a result of an overproduction of SST, and this effect might be more important among women. This hypothesis is in accordance with other studies suggesting that SST output is more critical in females than in males but still relevant for both of them in case of obesity.34, 35, 36, 37, 38 Moreover, the results are in accordance with other studies, which hypothesized that endogenous SST not only suppresses GH release in females but also has a role in regulating the expression of genes important to the GH-axis function.36 The lack of effects observed in males could be related to a reduced hypothalamic sensitivity caused by differences in the SST-receptor activity between genders. However, it should be noted that the gender-dependent role SST has in regulating the GH pulse release in humans has not been directly studied. Therefore, caution should be exercised in extrapolating the results from rodent experiments across species. In addition, while SST is commonly regarded as an inhibitor of GH release at high doses, it can also stimulate GH release at low doses in pituitary cell cultures.39 Thus evidence indicates that the SST system is more complex than initially expected and may be a versatile regulator of biological activity. The study of this polymorphism could shed needed light on in vivo SST functions and their possible interactions with age, gender and metabolic environmental factors in humans.
Neuronostatin (NST), a recently discovered peptide, is another variable important to consider when trying to document and explain our results. SST and NST are derived from the same preprohormone, but despite their common origin, the two peptides differ in structure and biological activities. Moreover, NST fails to activate any of the SST receptors and seems to be differentially regulated.40, 41 NST is known to induce a significant rise in MAP by increasing sympathetic nervous system activity and initiating vasopressin release from the posterior pituitary.42 As SST and NST are both derived from the same preprohormone and endowed with their own biological activities, they could be released in diverse amounts upon specific stimuli. Conversely, it has also been proposed that any attempt to compromise the production of one of them would result in the loss of the other as well. A raised production of the SST preprohormone could increase the levels of both peptides, simultaneously increasing blood pressure by NST and weight gain by SST-induced GH deficiency.
This study can be seen as a useful first step in exploring potential causal pathways between the rs34872250 polymorphism and hypertension. It also supports the hypothesis that the sexually dimorphic pattern of GH release is influenced by the SST system and that females could be more sensitive than males. The genetic and phenotypic variants should now be explored in other diversified populations. Once established, the association could be used to shed some light on the molecular or biochemical mechanisms implicated. Furthermore, experiments might be designed to test its effect on SST concentration as well as assess its functional roles in biological processes and disease pathology. Such studies can provide a strong support for the development of new treatments.43, 44
Our study has some limitations. The blood pressure measurements made in the physician’s office continue to be frequently used to diagnose hypertension as well as to evaluate treatment efficacy. However, these conventional time-unspecified single measurements are indicative of only a brief and small fraction of the entire 24-h blood pressure pattern, which can be affected by the ‘white coat hypertension’ factor, ‘masked hypertension’ or other several sources of error.1 A new recommendation suggests to confirm the diagnosis by either a reliable repeated home blood pressure monitoring or 24-h ambulatory blood pressure monitoring.45 In addition, all groups have an average BMI beyond the limit of the overweight category. This could act as confounder, because as seen previously, obesity is well known to disrupt the SST tone. Another limitation is the selection bias, considering that participants were recruited among lipid clinic patients. Thus we cannot exclude that other primary disorders could have influenced the results. Moreover, the combined effect of two or more genes on a complex phenotype such as hypertension cannot be described as the sum of separate effects but only as epistasis. Thereby, it is mandatory to replicate these analyses in larger and more diversified populations before the results can be generalized.
However, the French-Canadian population of the Saguenay-Lac-Saint-Jean, from which our subjects originate from, could be seen as strength in such a study. This population descended from a founder population who settled in this region 300–400 years ago. This founder effect provides several benefits for mapping the genomic determinants of complex traits.46 Genetic heterogeneity remains a problem in disease identification strategies that can be avoided by analyzing homogeneous populations who have a geographic stability and are most likely uniform in their environmental exposure.47
The cross-sectional design of our study does not give any information about the potential causal pathway that may be implicated. SST expression and secretion mechanisms as well as functional genomic studies on microsatellites suggest that this polymorphism might have a significant impact on SST metabolism. The polymorphism is located on the promoter, a critical sequence for the DNA transcription process that could modulate the expression levels of many genes.48 Unfortunately, evidence on the potential effect on SST levels is not yet available in the literature. In addition, our study design does not allow to conclude beyond a reasonable doubt that the polymorphism has a direct effect on the expression level of SST or hypertension onset and/or severity. It is very difficult to measure SST because of its very short half-life (1–3 min).49 It was therefore impossible for us to obtain this data during the conduct of the study. Our research needs to be followed by appropriate, well-designed functional studies.
In conclusion, our study showed that the poly-T-repeat sequence polymorphism in the promoter of the SST gene is associated with significant variations of blood pressure and suggest that it could modulate the risk of hypertension, particularly among overweight/obese women.
References
Pimenta E, Oparil S . Management of hypertension in the elderly. Nat Rev Cardiol 2012; 9: 286–296.
Messerli FH, Williams B, Ritz E . Essential hypertension. Lancet 2007; 370: 591–603.
Perkovic V, Huxley R, Wu Y, Prabhakaran D, MacMahon S . The burden of blood pressure-related disease: a neglected priority for global health. Hypertension 2007; 50: 991–997.
Xi B, Chen M, Chandak GR, Shen Y, Yan L, He J, Mou SH . STK39 polymorphism is associated with essential hypertension: a systematic review and meta-analysis. PLoS ONE 2013; 8: e59584.
Wang L, Zhang B, Li M, Li C, Liu J, Liu Y, Wang Z, Zhou J, Wen S . Association between single-nucleotide polymorphisms in six hypertensive candidate genes and hypertension among northern Han Chinese individuals. Hypertens Res 2014; 37: 1068–1074.
Krantic S, Goddard I, Saveanu A, Giannetti N, Fombonne J, Cardoso A, Jaquet P, Enjalbert A . Novel modalities of somatostatin actions. Eur J Endocrinol 2004; 151: 643–655.
Ehrman MM, Melroe GT, Kittilson JD, Sheridan MA . Regulation of pancreatic somatostatin gene expression by insulin and glucagon. Mol Cell Endocrinol 2005; 235: 31–37.
Reynaert H, Geerts A . Pharmacological rationale for the use of somatostatin and analogues in portal hypertension. Aliment Pharmacol Ther 2003; 18: 375–386.
Scalera G, Tarozzi G . Somatostatin administration modifies food intake, body weight, and gut motility in rat. Peptides 1998; 19: 991–997.
Li W, Shi YH, Yang RL, Cui J, Xiao Y, Wang B, Le GW . Effect of somatostatin analog on high-fat diet-induced metabolic syndrome: involvement of reactive oxygen species. Peptides 31: 625–629 2009.
Colao A, De Block C, Gaztambide MS, Kumar S, Seufert J, Casanueva FF . Managing hyperglycemia in patients with Cushing's disease treated with pasireotide: medical expert recommendations. Pituitary 2014; 17: 180–186.
Panagopoulos GN, Deftereos SN, Tagaris GA, Gryllia M, Kounadi T, Karamani O, Panagiotidis D, Koutiola-Pappa E, Karageorgiou CE, Piadites G . Octreotide: a therapeutic option for idiopathic intracranial hypertension. Neurol Neurophysiol Neurosci 2007; 10: 1.
Chatila R, Ferayorni L, Gupta T, Groszmann RJ . Local arterial vasoconstriction induced by octreotide in patients with cirrhosis. Hepatology 2000; 31: 572–576.
Maison P, Tropeano AI, Macquin-Mavier I, Giustina A, Chanson P . Impact of somatostatin analogs on the heart in acromegaly: a metaanalysis. J Clin Endocrinol Metab 2007; 92: 1743–1747.
Yang JF, Wu XJ, Li JS, Cao JM, Han JM . Effect of somatostatin versus octreotide on portal haemodynamics in patients with cirrhosis and portal hypertension. Eur J Gastroenterol Hepatol 2005; 17: 53–57.
Gaudet D, Arsenault S, Perusse L, Vohl MC, St-Pierre J, Bergeron J, Despres JP, Dewar K, Daly MJ, Hudson T, Rioux JD . Glycerol as a correlate of impaired glucose tolerance: dissection of a complex system by use of a simple genetic trait. Am J Hum Genet 2000; 66: 1558–1568.
Vohl MC, Lepage P, Gaudet D, Brewer CG, Betard C, Perron P, Houde G, Cellier C, Faith JM, Despres JP, Morgan K, Hudson TJ . Molecular scanning of the human PPARa gene: association of the L162v mutation with hyperapobetalipoproteinemia. J Lipid Res 2000; 41: 945–952.
The Airlie (VA) Consensus Conference. In: Standardization of anthropometric measurements Lohman TRA, Martorel R (eds). Human Kinetics Publishers: Champaign, IL, USA. 1988, pp 39–80.
Gaudet D, Arsenault S, Belanger C, Hudson T, Perron P, Bernard M, Hamet P . Procedure to protect confidentiality of familial data in community genetics and genomic research. Clin Genet 1999; 55: 259–264.
McNamara JR, Schaefer EJ . Automated enzymatic standardized lipid analyses for plasma and lipoprotein fractions. Clin Chim Acta 1987; 166: 1–8.
Friedewald WT, Levy RI, Fredrickson DS . Estimation of the concentration of low-density lipoprotein cholesterol in plasma, without use of the preparative ultracentrifuge. Clin Chem 1972; 18: 499–502.
Chen Y, Zhang X, Pan B, Jin X, Yao H, Chen B, Zou Y, Ge J, Chen H . A modified formula for calculating low-density lipoprotein cholesterol values. Lipids Health Dis 2010; 9: 52.
Grim CM, Grim CE . A curriculum for the training and certification of blood pressure measurement for health care providers. Can J Cardiol 1995; 11 (Suppl H): 38H–42H.
Pickering TG, Hall JE, Appel LJ, Falkner BE, Graves JW, Hill MN, Jones DH, Kurtz T, Sheps SG, Roccella EJ,, Council on High Blood Pressure Research P, Public Education Subcommittee AHA. Recommendations for blood pressure measurement in humans: an AHA scientific statement from the Council on High Blood Pressure Research Professional and Public Education Subcommittee. J Clin Hypertens (Greenwich) 2005; 7: 102–109.
Miura K, Dyer AR, Greenland P, Daviglus ML, Hill M, Liu K, Garside DB, Stamler J . Pulse pressure compared with other blood pressure indexes in the prediction of 25-year cardiovascular and all-cause mortality rates: The Chicago Heart Association Detection Project in Industry Study. Hypertension 2001; 38: 232–237.
Zidek W, Naditch-Brule L, Perlini S, Farsang C, Kjeldsen SE . Blood pressure control and components of the metabolic syndrome: the GOOD survey. Cardiovasc Diabetol 2009; 8: 51.
Gaudet D, Gagne C, Perron P, Couture P, Tonstad S . Ethical issues in molecular screening for heterozygous familial hypercholesterolemia: the complexity of dealing with genetic susceptibility to coronary artery disease. Community Genet 1999; 2: 2–8.
Torrecillas G, Medina J, Diez-Marques ML, Rodriguez-Puyol D, Rodriguez-Puyol M . Mechanisms involved in the somatostatin-induced contraction of vascular smooth muscle cells. Peptides 1999; 20: 929–935.
Wells M, Chande N, Adams P, Beaton M, Levstik M, Boyce E, Mrkobrada M . Meta-analysis: vasoactive medications for the management of acute variceal bleeds. Aliment Pharmacol Ther 2012; 35: 1267–1278.
Brisson D, Vohl MC, St-Pierre J, Hudson TJ, Gaudet D . Glycerol: a neglected variable in metabolic processes? Bioessays 2001; 23: 534–542.
Murray RD, Wieringa GE, Lissett CA, Darzy KH, Smethurst LE, Shalet SM . Low-dose GH replacement improves the adverse lipid profile associated with the adult GH deficiency syndrome. Clin Endocrinol (Oxf) 2002; 56: 525–532.
Stanley TL, Grinspoon SK . Effects of growth hormone-releasing hormone on visceral fat, metabolic, and cardiovascular indices in human studies. Growth Hormone IGF Res 2015; 25: 59–65.
Dieguez C, Carro E, Seoane LM, Garcia M, Camina JP, Senaris R, Popovic V, Casanueva FF . Regulation of somatotroph cell function by the adipose tissue. Int J Obes Relat Metab Disord 2000; 24 (Suppl 2): S100–S103.
Luque RM, Park S, Kineman RD . Role of endogenous somatostatin in regulating GH output under basal conditions and in response to metabolic extremes. Mol Cell Endocrinol 2008; 286: 155–168.
Cordoba-Chacon J, Gahete MD, Castano JP, Kineman RD, Luque RM . Somatostatin and its receptors contribute in a tissue-specific manner to the sex-dependent metabolic (fed/fasting) control of growth hormone axis in mice. Am J Physiol Endocrinol Metab 2011; 300: E46–E54.
Luque RM, Kineman RD . Gender-dependent role of endogenous somatostatin in regulating growth hormone-axis function in mice. Endocrinology 2007; 148: 5998–6006.
Tzotzas T, Papazisis K, Perros P, Krassas GE . Use of somatostatin analogues in obesity. Drugs 2008; 68: 1963–1973.
Veldhuis JD, Bowers CY . Determinants of GH-releasing hormone and GH-releasing peptide synergy in men. Am J Physiol Endocrinol Metab 2009; 296: E1085–E1092.
Cordoba-Chacon J, Gahete MD, Culler MD, Castano JP, Kineman RD, Luque RM . Somatostatin dramatically stimulates growth hormone release from primate somatotrophs acting at low doses via somatostatin receptor 5 and cyclic AMP. J Neuroendocrinol 2012; 24: 453–463.
Yosten GL, Pate AT, Samson WK . Neuronostatin acts in brain to biphasically increase mean arterial pressure through sympatho-activation followed by vasopressin secretion: the role of melanocortin receptors. Am J Physiolo Regul Integr Compar Physiol 2011; 300: R1194–R1199.
Yosten GL, Samson WK . Pressor doses of vasopressin result in only transient elevations in plasma peptide levels. Peptides 2012; 33: 342–345.
Vainio L, Perjes A, Ryti N, Magga J, Alakoski T, Serpi R, Kaikkonen L, Piuhola J, Szokodi I, Ruskoaho H, Kerkela R . Neuronostatin, a novel peptide encoded by somatostatin gene, regulates cardiac contractile function and cardiomyocyte survival. J Biol Chem 2012; 287: 4572–4580.
Park SY, Lee HJ, Ji SM, Kim ME, Jigden B, Lim JE, Oh B . ANTXR2 is a potential causative gene in the genome-wide association study of the blood pressure locus 4q21. Hypertens Res 2014; 37: 811–817.
Tabor HK, Risch NJ, Myers RM . Candidate-gene approaches for studying complex genetic traits: practical considerations. Nat Rev Genet 2002; 3: 391–397.
Hermida RC, Ayala DE, Fontao MJ, Mojon A, Fernandez JR . Ambulatory blood pressure monitoring: importance of sampling rate and duration—48 versus 24 hours—on the accurate assessment of cardiovascular risk. Chronobiol Int 2013; 30: 55–67.
Engert JC, Lemire M, Faith J, Brisson D, Fujiwara TM, Roslin NM, Brewer CG, Montpetit A, Darmond-Zwaig C, Renaud Y, Dore C, Bailey SD, Verner A, Tremblay G, St-Pierre J, Betard C, Platko J, Rioux JD, Morgan K, Hudson TJ, Gaudet D . Identification of a chromosome 8p locus for early-onset coronary heart disease in a French Canadian population. Eur J Hum Genet 2008; 16: 105–114.
Qi Y, Zhao H, Wang Y, Wang Y, Lu C, Xiao Y, Cao J, Jia N, Wang B, Niu W . Replication of the top 10 most significant polymorphisms from a large blood pressure genome-wide association study of northeastern Han Chinese East Asians. Hypertens Res 2014; 37: 134–138.
Wray GA . The evolutionary significance of cis-regulatory mutations. Nat Rev Genet 2007; 8: 206–216.
Patel YC . Somatostatin and its receptor family. Front Neuroendocrinol 1999; 20: 157–198.
Acknowledgements
We thank all the staff of the ECOGENE-21 Clinical Research Center and Chicoutimi Hospital Lipid Clinic for their help in data collection and their dedicated work. Finally, we acknowledge the contribution of the subjects who participated in this project; without them, clinical studies would not be possible. This research was supported by ECOGENE-21, the CIHR team in community genetics (grant no. CTP-82941).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Tremblay, M., Brisson, D. & Gaudet, D. Association between a polymorphic poly-T repeat sequence in the promoter of the somatostatin gene and hypertension. Hypertens Res 39, 467–474 (2016). https://doi.org/10.1038/hr.2016.4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/hr.2016.4