Abstract
Study design:
Case report.
Objective:
Report rapid neurological changes in a complete tetraplegic following a cell injection procedure.
Setting:
Beijing, China.
Methods:
ASIA/IMSOP neurological scale. Immunostaining of cell cultures. Cellular transplantation to effect functional restoration following spinal cord injury (SCI) has been hypothesized to cause improvements through axonal regeneration, increased plasticity, or axonal remyelination. Several human trials are in preliminary phases. We report a rapid improvement in motor and sensory functions in the segment adjacent to the level of complete SCI within days following cellular transplantation of cultured fetal olfactory bulb-derived cells. The patient was an 18-year-old C3 ASIA A complete tetraplegic 18 months post-injury who had been neurologically stable for more than 6 months.
Results:
Within 48 h of cell transplantation, the patient improved one ASIA motor grade in the left elbow flexors and began to show right wrist extensor function. Descent of the sensory level occurred within 4 days and then the rate of change slowed. He is now a C5 motor and C4 sensory complete tetraplegic. Cellular cultures prepared in the same facility showed viable human cells that labeled for nestin and GFAP.
Conclusion:
We hypothesize that improved transmission in intact fibers subserving the zone of partial preservation accounts for these early improvements. We emphasize the need for further independent analysis of the outcomes of this and other preliminary cell transplant studies.
Similar content being viewed by others
Introduction
Experimental studies have indicated that olfactory ensheathing glia (OEG) may support partial neurological recovery following spinal cord injury (SCI).1, 2, 3, 4, 5 The mechanisms of such recovery have been shown to include axonal regeneration2 and local sprouting,6 and remyelination.7 Sources for donor tissue to derive OEGs are limited in quantity8 and access to the olfactory bulb (OB) is invasive.9 Therefore, fetal allografts represent a possible alternative source from which to derive the cells. OEGs have been derived from embryonic rodent OB and characterized.10, 11 However, it is not known at what developmental stage the human OB becomes populated by OEGs although it has been proposed that this may occur as early as 6.5 weeks of embryonic development.12 Currently, a small-scale phase one clinical trial is exploring the safety and efficacy of transplanting adult nasal-derived putative OEGs into the chronically injured spinal cord,13 but the number of patients treated with fetal cell preparations in China exceeds 500. The first and third authors of this case report acted as observers of this transplant series14 over a 12-day period and wrote this report. These authors systematically examined the patient prior to surgery, observed the operative procedure, and followed the patient clinically for 8 days post-operatively.
Materials and methods
An 18-year-old Japanese male had sustained a C3 complete SCI subsequent to traumatic C4/5 bilateral facet dislocation. He was initially treated with restoration of alignment and fixation via a posterior surgical approach. At 18 months post-injury, he was neurologically stable and reported no improvements within the past 6 months. On 8.27.2004, he was admitted to Chaoyang hospital for cellular transplantation. He was examined according to the criteria of the ASIA neurological assessment scale.15 The physical exam performed on the day prior to surgery (8.28.2004) showed a C3 sensory level intact at the supraclavical fossa for pinprick and light touch bilaterally. There was abnormal sensation in C4 at the top of the acromioclavical joints bilaterally and no sensation in other dermatomes below C4. Manual muscle testing showed grade 4 right-sided C5 function and grade 2 left-sided C5 function at the elbow flexors. No C6 function at either wrist and no other voluntary muscle movement below the C6 level was detected. The rectal exam indicated no sensory or motor function preserved in sacral segments S4/5; therefore, the deficit was classified as C3 ASIA A motor and sensory complete tetraplegia. The presurgical plain films showed posterior screws and plates immobilizing C4 to C5 (Figure 1). The presurgical MRI showed severe myelomalacia extending from C4 to C6 without evidence of spinal deformity, spinal cord compression, or spinal cord tethering (Figure 2).
Cell culture and preparation for transplantation
Two fetal OBs were obtained from a single early second trimester human fetus. This fetal tissue was obtained in the course of a therapeutic abortion that was conducted in accord with applicable Chinese institutional and governmental guidelines. The maternal fetal donor provided consent for the use of the fetus for the experimental procedure and serologic testing verified that she was free of transmissible diseases including HIV and hepatitis B and C. The patient receiving the tissue provided consent for both the transplantation procedure itself and the injection of the fetal cells. We certify that the procedure met all applicable institutional guidelines of the Chaoyang Hospital, Capital University of Medical Sciences, Beijing, China, and Chinese governmental regulations concerning the ethical use of human volunteers during the course of this research procedure.
The bulbs were minced and triturated to a suspension, which was plated onto a poly-L-lysine-coated cell culture flask. Cells were exposed to 10% fetal bovine serum (FBS) in DMEM/F12 for 4 days and then grown in DMEM without serum for an additional 10 days (Figures 3 and 4). The cells were harvested from the flasks and resuspended into DMEM 10% FBS at a concentration of 20 000 cells/μl for transplantation.
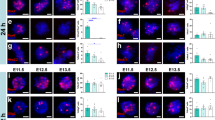
Immunostaining of human fetal OB-derived cells. (a) The same culture illustrated in Figure 3 is immunostained for GFAP. Extensive intensely stained GFAP-positive processes extend from a cellular cluster, blue nuclear label, × 200. (b) Anti-human-specific nestin antibody labeling of the cell culture shows many lengthy nestin-positive processes extending from the cell cluster, blue nuclear label, × 200. Bar=120 μm
Characterization of parallel cell cultures
Immunostaining procedures were carried out in Miami on a cell culture that was prepared as detailed above. For transportation from Beijing, the cells were fixed in 100% alcohol for 24 h and then switched to buffer. The cells were photographed under a phase contrast microscope and then the flasks were cut into 2.5 cm triplicate squares for immunostaining. Cells were permeabilized with 4% paraformaldehyde and 0.2% Triton X-100 in Dulbecco's phosphate-buffered saline (PBS) for 10 min at room temperature. Subsequently, the cultures were washed three times with PBS and once with Leibovitz's L-15 medium (Gibco, Invitrogen) and blocked with 20% normal goat serum in L-15 medium for 30 min. Cells were then exposed to anti-GFAP (rabbit anti-GFAP at 1:100; DAKO), rabbit anti-human nestin (1:1000; gift from Dr Urban Lendahl and Dr Per Almqvist), anti-human mitochondrial antibody (MAb 1273 at 1:200; Chemicon), and anti-S100 (rabbit anti-cow at 1:100; DAKO) for 2 h at room temperature. The squares of cells were then washed three times in 0.1 M PBS and exposed to secondary antibody (FITC anti-rabbit, 1:100; Molecular Probes) for 2 h at room temperature. Following this, they were washed three times and then inverted and mounted on glass slides using ‘MAGIC’ (Citifluor: 90% glycerol in PBS with 2.5 g DABCO-BDH 28642 and 0.1 g sodium azide) containing a nuclear marker (Hoechst 33342, 10 mM, 5.6 mg/ml; Molecular Probes). The immunostained cultures were studied using a confocal microscope and images acquired using Zeiss LSM software.
Surgical procedure
After inducing general anesthesia, the patient underwent intubation and was carefully placed into the prone position. The site of the previous surgery was identified by palpation and by reference to the previous incision. Two subperiosteal partial laminectomies were performed, one at C3/4 and the second at C5/6 and the dura was exposed. Following dural incision and identification of the spinal cord midline, two injections were performed at C3/4 and C5/6 as follows. At each site, 25 μl of the cell suspension was injected over approximately 4 min. Following injection, gentle pressure was maintained over the injection site using a cottonoid for a further 3–4 min. Simultaneous to the injections, the patient received an intravenous bolus of 30 mg/kg methylprednisolone and then 5.4 mg/kg/h for a subsequent 23 h.
Clinical course
The patient recovered from anesthesia, being extubated immediately, and was examined 4 h after surgery. He was found to have an exam similar to that obtained preoperatively with no new deficits. On the subsequent 8 days, his exam was documented daily. On the first postoperative day, a descent of the sensory level was noted as indicated in Figure 5. This progressed over the next 48 h and then changed more slowly. On the first postoperative day, a grade 1 contraction of the wrist extensor was detectable on the right side and this progressed to a full range of motion with gravity eliminated (grade 2) by the fourth postoperative day (Figure 6). On the left side, the elbow flexors recovered from a grade 2 to a grade 3 and subsequently a grade 4 strength. While weak contraction of the left wrist extensor was palpable, no joint motion was apparent. No changes in sensory and motor function were found in the sacral segment. Therefore, his neurological score changed from C3 ASIA A sensory and motor complete tetraplegia to C5 motor and C4 sensory ASIA A complete tetraplegia. On the fifth postoperative day, the patient complained of a headache and had a febrile spike. A lumbar puncture revealed elevated protein, several white cells, and a decreased CSF glucose relative to serum. The patient was treated with intravenous antibiotics and the meningitis resolved. Despite this meningitis, the neurological changes were maintained. Follow-up contact regarding the patient was obtained at 2 and 10 months post-transplantation through the language translator who had assisted the patient in Beijing. It was reported that he maintained the improvements in his right wrist and left biceps, but no further notable motor recovery occurred in the upper extremities and the sensory level did not change. After returning to Japan, he was admitted to a rehabilitation facility for several weeks and it was noted that his sitting balance improved. His meningitis did not recur and he did not develop neuropathic pain.
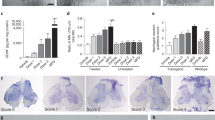
Postsurgical sensory changes. These partial changes occurred within 48 h of the transplant procedure with recovery of pinprick sensation in the regions noted, which extend into the C5 dermatome. (a) Right side. (b) Left side. The level for normal sensation did not change (marked on the left side in red)
Postsurgical motor changes. Prior to the transplant procedure, there was no detectable muscle contraction of the right wrist extensors. By the fourth postoperative day, movement of the wrist through almost the complete range of motion was detectable with gravity eliminated, (a–d) video 37fps, sequential fifth frames. Recovery of antigravity function was not observed
Immunostaining
The ethanol-fixed cultures were clearly positive for anti-human nestin and for GFAP (Figure 4), but negative for anti- S-100 and anti-human mitochondrial antibody. The distribution of the cells and outgrowth of nestin- and GFAP-positive cells was reminiscent of that seen in human neurosphere cultures.16, 17
Discussion
Neurological recovery
This report is important because rapid changes in a clinically complete stable tetraplegic patient are a novel observation. This patient had a rapid partial recovery of function in the C5 and C6 spinal segments within a few days of surgery. The mechanism of this recovery is unknown but is clearly linked to the procedure and possibly to the injected cells. The rapid changes are highly unlikely to be due to either regeneration or myelin repair, but may reflect increased function of intact fibers or strengthening of their synaptic connections. Because the surgery was not performed at the site of the SCI, decompression or untethering is unlikely to account for the observed changes but cannot be excluded. Furthermore, neither spinal cord compression nor tethering is evident on the preoperative imaging. Gradual recovery in the first two segments distal to an acute complete cervical SCI has been reported by several authors. Recovery of one adjacent segment is expected within 6 months following injury18, 19, 20 and a smaller proportion of patients recover a second segment. This recovery is usually complete within the first year post-injury.21, 22, 23, 24, 25 A relationship between preserved pinprick sensation and recovery of wrist extensor function has been reported in subacute quadriplegia.26, 27
Culture immunostaining
An important issue concerns the identity of the cells being transplanted in the Beijing study. A parallel culture showing robust growth at 11 days post-plating was assessed for human and OEG markers. Anti-human p75 was not tested since our human-specific antibody does not bind in fixed cultures. S-100 was negative as was anti-mitochondrial antibody; this may have been due to the fixation method employed. A significant proportion of cells were strongly anti-nestin and anti-GFAP positive. Nestin immunopositivity has been reported in OEG cultures28 but is typically a marker of immature neuroectodermally derived cells29 and only a small number of cells are positive in human adult OEG cultures (unpublished data). Nestin is known to be positive in cultured human stem cells30 and GFAP is also now considered a possible stem cell marker.31, 32 We do not find such strong GFAP labeling in human OEG cultures and suggest that the observed cells may be astrocytes. It should be noted that it is not known with certainty at what developmental stage the human fetal OB becomes populated by OEGs12, 33, 34 and the spectrum of cell types that are present in the primary cultures has not been published. Nor is known at what developmental stage conventional OEG markers begin to be identifiable. While these cells may be OEGs, they also could be neuroectodermally derived stem cells. Even the adult OB contains stem cells.35
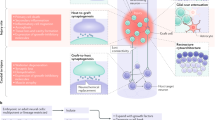
Possible mechanisms of rapid neurological changes
Trophic effects due to factors released from the transplanted cells could cause angiogenesis,36 neuronal plasticity, or influence synaptic conduction.37 Neonatal rodent OECs release nerve growth factor (NGF) and brain-derived neurotrophic factor (BDNF) into culture media38 but adult rodent OECs release negligible quantities of BNDF into culture media.39 Exogenous NGF and BDNF have been shown to enhance glutamatergic neurotransmission in the brain40 by both pre- and postsynaptic mechanisms41 and to induce formation of new synapses.42 In addition, NGF can influence expression of Na+ and Ca2+ channels on neurons in culture.43 The release of trophic molecules by cultured human fetal OB-derived cells should be studied. The possibility that the use of high-dose methylprednisolone influenced the properties44 of chronically injured neurons in this patient must also be considered. This issue has not been studied despite the frequent use of methylprednisolone for neuroprotection in elective spinal surgery.
Fetal OEC transplantation for SCI
The purpose of the author's observational study was to gather information about a treatment that has received a large amount of attention in the news media and has been reported at international conferences.13 The ability to derive objective data from this treatment group is currently limited by several factors, which include the absence of a control group and lack of systematic follow-up by independent clinicians. There is very little preclinical data on the use of fetal OB-derived cells11, 45 and there are no published experimental studies that have shown efficacy of such fetal cells in a contusion SCI model nor have long-term safety studies been performed. Grafts of embryonic brain and spinal cord tissue have been reported to survive in the spinal cord46, 47, 48, 49, 50, 51 of experimental animals and considerable experimental data from animal studies indicate that transplanted fetal spinal cord tissue improves recovery from SCI.52, 53 Fetal spinal cord tissue has previously been transplanted into patients with chronic SCI and symptomatic syringomyelia without reports of adverse events54, 55, 56 and there is only one definitive report of tumor growth following CNS transplantation of fetal tissue in a patient.57 While OEGs are very interesting cells with therapeutic potential, many important steps that normally are considered the essential groundwork of a clinical trial have not been completed for fetal OB-derived cell transplantation. Unless these steps are undertaken and the clinical studies conducted with a control group and independent outcome assessment, the potential for this therapy to advance medical knowledge remains limited.
Conclusion
Transplantation of cultured fetal OB-derived cells may be associated with limited rapid neurologic improvements in segments adjacent to the injury level. The mechanism is unknown but the time course is suggestive of a neurotrophic effect.
References
Plant GW, Christensen CL, Oudega M, Bunge MB . Delayed transplantation of olfactory ensheathing glia promotes sparing/regeneration of supraspinal axons in the contused adult rat spinal cord. J Neurotrauma 2003; 20: 1–16.
Lu J, Feron F, Mackay-Sim A, Waite PM . Olfactory ensheathing cells promote locomotor recovery after delayed transplantation into transected spinal cord. Brain 2002; 125(Part 1): 14–21.
Ramon-Cueto A, Cordero MI, Santos-Benito FF, Avila J . Functional recovery of paraplegic rats and motor axon regeneration in their spinal cords by olfactory ensheathing glia. Neuron 2000; 25: 425–435.
Li Y, Field PM, Raisman G . Regeneration of adult rat corticospinal axons induced by transplanted olfactory ensheathing cells. J Neurosci 1998; 18: 10514–10524.
Li Y, Field PM, Raisman G . Repair of adult rat corticospinal tract by transplants of olfactory ensheathing cells. Science 1997; 277: 2000–2002.
Keyvan-Fouladi N, Li Y, Raisman G . How do transplanted olfactory ensheathing cells restore function? Brain Res Brain Res Rev 2002; 40: 325–327.
Kato T, Honmou O, Uede T, Hashi K, Kocsis JD . Transplantation of human olfactory ensheathing cells elicits remyelination of demyelinated rat spinal cord. Glia 2000; 30: 209–218.
Herrera LP, Casas CE, Bates ML, Guest JD . Ultrastructural study of the primary olfactory pathway in Macaca fascicularis. J Comp Neurol 2005; 488: 427–441.
Franklin RJ . Obtaining olfactory ensheathing cells from extra-cranial sources a step closer to clinical transplant-mediated repair of the CNS? Brain 2002; 125(Part 1): 2–3.
Doucette R . Glial cells in the nerve fiber layer of the main olfactory bulb of embryonic and adult mammals. Microsc Res Tech 1993; 24: 113–130.
Boyd JG, Lee J, Skihar V, Doucette R, Kawaja MD . LacZ-expressing olfactory ensheathing cells do not associate with myelinated axons after implantation into the compressed spinal cord. Proc Natl Acad Sci USA 2004; 101: 2162–2166.
Muller F, O'Rahilly R . Olfactory structures in staged human embryos. Cells Tissues Organs 2004; 178: 93–116.
Steeves J, Fawcett J, Tuszynski M . Report of international clinical trials workshop on spinal cord injury February 20–21, 2004, Vancouver, Canada. Spinal Cord 2004; 42: 591–597.
Huang H et al. Influence of patients' age on functional recovery after transplantation of olfactory ensheathing cells into injured spinal cord injury. Chin Med J 2003; 116: 1488–1491.
Maynard Jr FM et al. International standards for neurological and functional classification of spinal cord injury. American Spinal Injury Association. Spinal Cord 1997; 35: 266–274.
Johansson CB, Svensson M, Wallstedt L, Janson AM, Frisen J . Neural stem cells in the adult human brain. Exp Cell Res 1999; 253: 733–736.
Uchida N et al. Direct isolation of human central nervous system stem cells. Proc Natl Acad Sci USA 2000; 97: 14720–14725.
Ditunno Jr JF, Sipski ML, Posunjak EA, Chen YT, Staas Jr WE, Herbison GJ . Wrist extensor recovery in traumatic quadriplegia. Arch Phys Med Rehabil 1987; 68(5 Part 1): 287–290.
Jacobs SR, Sarlo FB, Baron EM, Herbison GJ, Ditunno Jr JF . Extensor carpi radialis recovery predicted by qualitative SEP and clinical examination in quadriplegia. Arch Phys Med Rehabil 1992; 73: 790–793.
Ditunno Jr JF, Cohen ME, Hauck WW, Jackson AB, Sipski ML . Recovery of upper-extremity strength in complete and incomplete tetraplegia: a multicenter study. Arch Phys Med Rehabil 2000; 81: 389–393.
Mange KC, Ditunno Jr JF, Herbison GJ, Jaweed MM . Recovery of strength at the zone of injury in motor complete and motor incomplete cervical spinal cord injured patients. Arch Phys Med Rehabil 1990; 71: 562–565.
Wu L, Marino RJ, Herbison GJ, Ditunno Jr JF . Recovery of zero-grade muscles in the zone of partial preservation in motor complete quadriplegia. Arch Phys Med Rehabil 1992; 73: 40–43.
Mange KC, Marino RJ, Gregory PC, Herbison GJ, Ditunno Jr JF . Course of motor recovery in the zone of partial preservation in spinal cord injury. Arch Phys Med Rehabil 1992; 73: 437–441.
Waters RL, Adkins RH, Yakura JS, Sie I . Motor and sensory recovery following complete tetraplegia. Arch Phys Med Rehabil 1993; 74: 242–247.
Kornsgold LM, Herbison GJ, Decena III BF, Ditunno Jr JF . Biceps versus extensor carpi radialis recovery in Frankel grades A and B in spinal cord injury patients. Paraplegia 1994; 32: 340–348.
Browne BJ, Jacobs SR, Herbison GJ, Ditunno Jr JF . Pin sensation as a predictor of extensor carpi radialis recovery in spinal cord injury. Arch Phys Med Rehabil 1993; 74: 14–18.
Poynton AR, O'Farrell DA, Shannon F, Murray P, McManus F, Walsh MG . Sparing of sensation to pin prick predicts recovery of a motor segment after injury to the spinal cord. J Bone Joint Surg Br 1997; 79: 952–954.
Zhang X, Klueber KM, Guo Z, Lu C, Roisen FJ . Adult human olfactory neural progenitors cultured in defined medium. Exp Neurol 2004; 186: 112–123.
Almqvist PM, Mah R, Lendahl U, Jacobsson B, Hendson G . Immunohistochemical detection of nestin in pediatric brain tumors. J Histochem Cytochem 2002; 50: 147–158.
Revishchin AV et al. Structure of cell clusters formed in cultures of dissociated human embryonic brain. Bull Exp Biol Med 2001; 132: 856–860.
Imura T, Kornblum HI, Sofroniew MV . The predominant neural stem cell isolated from postnatal and adult forebrain but not early embryonic forebrain expresses GFAP. J Neurosci 2003; 23: 2824–2832.
Garcia AD, Doan NB, Imura T, Bush TG, Sofroniew MV . GFAP-expressing progenitors are the principal source of constitutive neurogenesis in adult mouse forebrain. Nat Neurosci 2004; 7: 1233–1241.
Chuah MI, Au C . Neural cell adhesion molecules are present in the fetal human primary olfactory pathway. Dev Neurosci 1992; 14: 357–361.
Chuah MI, Zheng DR . Olfactory marker protein is present in olfactory receptor cells of human fetuses. Neuroscience 1987; 23: 363–370.
Liu Z, Martin LJ . Olfactory bulb core is a rich source of neural progenitor and stem cells in adult rodent and human. J Comp Neurol 2003; 459: 368–391.
Ramer LM, Au E, Richter MW, Liu J, Tetzlaff W, Roskams AJ . Peripheral olfactory ensheathing cells reduce scar and cavity formation and promote regeneration after spinal cord injury. J Comp Neurol 2004; 473: 1–15.
Auld DS et al. Modulation of neurotransmission by reciprocal synapse-glial interactions at the neuromuscular junction. J Neurocytol 2003; 32: 1003–1015.
Woodhall E, West AK, Chuah MI . Cultured olfactory ensheathing cells express nerve growth factor, brain-derived neurotrophic factor, glia cell line-derived neurotrophic factor and their receptors. Brain Res Mol Brain Res 2001; 88: 203–213.
Ruitenberg MJ et al. Ex vivo adenoviral vector-mediated neurotrophin gene transfer to olfactory ensheathing glia: effects on rubrospinal tract regeneration, lesion size, and functional recovery after implantation in the injured rat spinal cord. J Neurosci 2003; 23: 7045–7058.
Lessmann V . Neurotrophin-dependent modulation of glutamatergic synaptic transmission in the mammalian CNS. Gen Pharmacol 1998; 31: 667–674.
Carmignoto G, Pizzorusso T, Tia S, Vicini S . Brain-derived neurotrophic factor and nerve growth factor potentiate excitatory synaptic transmission in the rat visual cortex. J Physiol 1997; 498(Part 1): 153–164.
Vicario-Abejon C, Collin C, McKay RD, Segal M . Neurotrophins induce formation of functional excitatory and inhibitory synapses between cultured hippocampal neurons. J Neurosci 1998; 18: 7256–7271.
Bouron A, Becker C, Porzig H . Functional expression of voltage-gated Na+ and Ca2+ channels during neuronal differentiation of PC12 cells with nerve growth factor or forskolin. Naunyn Schmiedebergs Arch Pharmacol 1999; 359: 370–377.
Hall ED . Glucocorticoid effects on the electrical properties of spinal motor neurons. Brain Res 1982; 240: 109–116.
Smale KA, Doucette R, Kawaja MD . Implantation of olfactory ensheathing cells in the adult rat brain following fimbria-fornix transection. Exp Neurol 1996; 137: 225–233.
Reier PJ, Bregman BS, Wujek JR . Intraspinal transplantation of embryonic spinal cord tissue in neonatal and adult rats. J Comp Neurol 1986; 247: 275–296.
Wirth III ED et al. In vivo magnetic resonance imaging of fetal cat neural tissue transplants in the adult cat spinal cord. J Neurosurg 1992; 76: 261–274.
Reier PJ, Stokes BT, Thompson FJ, Anderson DK . Fetal cell grafts into resection and contusion/compression injuries of the rat and cat spinal cord. Exp Neurol 1992; 115: 177–188.
Anderson DK, Howland DR, Reier PJ . Fetal neural grafts and repair of the injured spinal cord. Brain Pathol 1995; 5: 451–457.
Akesson E et al. Solid human embryonic spinal cord xenografts in acute and chronic spinal cord cavities: a morphological and functional study. Exp Neurol 2001; 170: 305–316.
Giovanini MA, Reier PJ, Eskin TA, Wirth E, Anderson DK . Characteristics of human fetal spinal cord grafts in the adult rat spinal cord: influences of lesion and grafting conditions. Exp Neurol 1997; 148: 523–543.
Stokes BT, Reier PJ . Fetal grafts alter chronic behavioral outcome after contusion damage to the adult rat spinal cord. Exp Neurol 1992; 116: 1–12.
Bregman BS, Kunkel-Bagden E, Reier PJ, Dai HN, McAtee M, Gao D . Recovery of function after spinal cord injury: mechanisms underlying transplant-mediated recovery of function differ after spinal cord injury in newborn and adult rats. Exp Neurol 1993; 123: 3–16.
Falci S et al. Obliteration of a posttraumatic spinal cord cyst with solid human embryonic spinal cord grafts: first clinical attempt. J Neurotrauma 1997; 14: 875–884.
Wirth III ED et al. Feasibility and safety of neural tissue transplantation in patients with syringomyelia. J Neurotrauma 2001; 18: 911–929.
Thompson FJ et al. Neurophysiological assessment of the feasibility and safety of neural tissue transplantation in patients with syringomyelia. J Neurotrauma 2001; 18: 931–945.
Mamelak AN et al. Fatal cyst formation after fetal mesencephalic allograft transplant for Parkinson's disease. J Neurosurg 1998; 89: 592–598.
Acknowledgements
This investigation was supported by the Miami Project to Cure Paralysis. The gracious hospitality and access to patients afforded by Dr H Huang, his team of surgeons, supporting staff and the Chaoyang hospital is gratefully acknowledged.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Guest, J., Herrera, L. & Qian, T. Rapid recovery of segmental neurological function in a tetraplegic patient following transplantation of fetal olfactory bulb-derived cells. Spinal Cord 44, 135–142 (2006). https://doi.org/10.1038/sj.sc.3101820
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.sc.3101820
Keywords
This article is cited by
-
Common olfactory ensheathing glial markers in the developing human olfactory system
Brain Structure and Function (2017)
-
Effects of transplantation of olfactory ensheathing cells in chronic spinal cord injury: a systematic review and meta-analysis
European Spine Journal (2015)
-
Neural plasticity and functional recovery of human central nervous system with special reference to spinal cord injury
Spinal Cord (2011)
-
Calponin is expressed by subpopulations of connective tissue cells but not olfactory ensheathing cells in the neonatal olfactory mucosa
BMC Neuroscience (2007)
-
An overview of tissue engineering approaches for management of spinal cord injuries
Journal of NeuroEngineering and Rehabilitation (2007)