Abstract
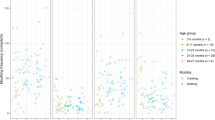
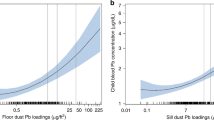
Understanding the routes of lead exposure in a very young infant is an essential precursor to identifying effective strategies for minimizing blood-lead (PbB) levels throughout infancy. The present study integrated observational data, lead-loading data, and household airborne particulate levels <10 μm (PM10) to understand the broad patterns of lead exposure in infants from Port Pirie, South Australia. Seven, 2–19-week-old infants were observed between three and six times, for 3–9 h per visit, at intervals of 1–9 weeks. Household lead-loading and PM10 data were collected for five of the families. Eight objects were observed in an infant's mouth, but only the infant's fingers, pacifier, and nipple of the mother's breast or teat of a bottle were observed in an infant's mouth for an average of more than 1% of an observation day. The objects most frequently put in an infant's mouth were their own fingers or their pacifier. Synthesizing our data on behavioral frequency, lead loading, and the surface area of contact, and using estimates of dose response, and sampling, transfer, and absorption efficiencies, the results suggest that a 4-month-old infant could absorb up to 4 μg of lead a day (equivalent to a PbB level of up to about 2.4 μg/dl) by mouthing their fingers, about two-thirds of all exposure routes identified in this study. Estimates also suggest that lead uptake via inhalation accounts for about 0.5–3% of an infant's PbB at 5 μg/dl. If our estimates reflect real routes and values, the majority of the average PbB level of 6-month-old infants in Port Pirie during 2002 could potentially be accounted for by the normal infant and family behaviors observed in this study. While the current level of concern is 10 μg/dl, recent studies indicate no safe threshold for Pb exposure, and so interventions for reducing chronic low-level exposure are useful. We suggest that home-based interventions for reducing Pb exposure should focus on maintaining low Pb loadings on objects that are directly associated with an infant, and outside objects that have few transfer steps to the infant.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 6 print issues and online access
$259.00 per year
only $43.17 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Aarts C., Hornell A., Kylberg E., Hofvander Y., and Gebre-Medhin M. Breastfeeding patterns in relation to thumb sucking and pacifier use. Pediatrics 1999: 104: e50.
Bellinger D., Leviton A., Rabinowitz M., Needleman H., and Waternaux C. Correlates of low-level lead exposure in urban children at 2 years of age. Pediatrics 1986: 77: 826–833.
Binns C.W., and Scott J.A. Using pacifiers: what are breastfeeding mothers doing? Breastfeeding Rev 2002: 10: 21–25.
Body P.E., Inglis G.R., and Mulcahy D.E. Lead Contamination in Port Pirie South Australia, SADEP Report number 101 South Australian Department of Environment and Planning, Adelaide, 1988.
Bornschein R.L., Succop P., Dietrich K.N., Clark C.S., Que Hee S., and Hammond P.B. The influence of social and environmental factors on dust lead, hand lead, and blood lead levels in young children. Environ Res 1985: 38: 108–118.
Brinkman S., Gialamas A., Jones L., Edwards P., and Maynard E. Child Activity Patterns for Environmental Exposure Assessment in the Home, National Environmental Health Forum Monographs Exposure Series No. 1 Department of Human Services, Adelaide, 1999.
Brouwer D.H., Kroese R., and Van Hemmen J.J. Transfer of contaminants from surface to hands: experimental assessment of linearity of the exposure process, adherence to the skin, and area exposed during fixed pressure and repeated contact with surfaces contaminated with a powder. Appl Occup Environ Hyg 1999: 14: 231–239.
Calder I.C., Maynard E.J., and Heyworth J.S. Port Pirie lead abatement program, 1992. Environ Geochem Health 1994: 16: 137–145.
Canfield R.L., Henderson Jr. C.R., Cory-Slechta D.A., Cox C., Jusko T.A., and Lanphear B.P. Intellectual impairment in children with blood lead concentrations below 10 microg per deciliter. New Engl J Med 2003: 348: 1517–1526.
Cook M., Chappell W.R., Hoffman R.E., and Mangione E.J. Assessment of blood lead levels in children living in a historic mining and smelting community. Am J Epidemiol 1993: 137: 447–455.
Cowan R.J., and Conley M.M. Surface area of the hand and digits. Can J Surg 1973: 16: 189–194.
Davies D.J., Thornton I., and Watt J.M., et al. Lead intake and blood lead in two-year-old U.K. urban children. Sci Total Environ 1990: 90: 13–29.
Diemel J.A., Brunekreef B., Boleij J.S., Biersteker K., and Veenstra S.J. The Arnhem Lead Study. II. Indoor pollution, and indoor/outdoor relationships. Environ Res 1981: 25: 449–456.
Freeman N.C., Sheldon L., Jimenez M., Melnyk L., Pellizzari E., and Berry M. Contribution of children's activities to lead contamination of food. J Expos Anal Environ Epidemiol 2001: 11: 407–413.
Gulson B.L., Jameson C.W., and Mahaffey K.R., et al. Relationships of lead in breast milk to lead in blood, urine and diet of the infant and mother. Environ Health Perspect 1998a: 106: 667–674.
Gulson B.L., Mahaffey K.R., and Jameson C.W., et al. Mobilization of lead from the skeleton during the postnatal period is larger than during pregnancy. J Lab Clin Med 1998b: 131: 295–297.
Gulson B.L., Pounds J.G., Mushak P., Thomas B.J., Gray B., and Korsch M.J. Estimation of cumulative lead releases (lead flux) from the maternal skeleton during pregnancy and lactation. J Lab Clin Med 1999: 134: 631–640.
Gulson B.L., Mizon K.J., Korsch M.J., Mahaffey K.R., and Taylor A.J. Dietary intakes of selected elements from longitudinal 6-day duplicate diets for pregnant and nonpregnant subjects and elemental concentrations of breast milk and infant formula. Environ Res 2001: 87: 160–174.
Hilts S.R., Pan U.W., White E.R., and Yates C.L. Trail Lead Program Exposure Pathways Investigations, Final report Community Lead Tank Force, Trail, 1995.
Hochberg Y. A sharper Bonferroni procedure for multiple tests of significance. Biometrika 1988: 75: 800–802.
Hsu D.J., and Swift D.J. The measurements of human inhalability of ultralarge aerosols in calm air using mannikins. J Aerosol Sci 1999: 30: 1331–1343.
International Commission on Radiological Protection. Human Respiratory Tract Model for Radiological Protection, Publication 66 Pergamon Press, Oxford, 1994.
Jackson J.M., and Mourino A.P. Pacifier use and otitis media in infants twelve months of age or younger. Pediatr Dent 1999: 21: 255–260.
Juberg D.R., Alfano K., Coughlin R.J., and Thompson K.M. An observational study of object mouthing behavior by young children. Pediatrics 2001: 107: 135–142.
Kopp C.B. Fine motor abilities of infants. Dev Med Child Neurol 1974: 16: 629–636.
Kutlaca A. Mechanisms of Dust Entry of Lead-Bearing Dusts into Houses in Port Pirie. PhD thesis, University of Adelaide 1998.
Lanphear B.P., Dietrich K., Auinger P., and Cox C. Cognitive deficits associated with blood lead concentrations <10 microg/dl in US children and adolescents. Public Health Rep 2000: 115: 521–529.
Lanphear B.P., Matte T.D., and Rogers J., et al. The contribution of lead-contaminated house dust and residential soil to children's blood lead levels. A pooled analysis of 12 epidemiologic studies. Environ Res 1998: 79: 51–68.
Lanphear M.D., Weitzman M., and Tanner M., et al. The Relation of Lead Contaminated House Dust and Blood Lead Levels among Urban Children, University of Rochester US HUD Grant # MLDP T0001-93 HUD, New York, 1994.
Mahaffey K.R. Quantities of lead producing health effects in humans: sources and bioavailability. Environ Health Perspect 1977: 19: 285–295.
Manton W.I. Total contribution of airborne lead to blood lead. Br J Ind Med 1985: 42: 168–172.
Maynard E.J., Thomas R., Simon D., Phipps C., Ward C., and Calder I. An evaluation of recent blood lead levels in Port Pirie, South Australia. Sci Total Environ 2003: 303: 25–33.
McClure N., and Burton J. A Baby's Story. Penguin, London, 1989.
Meyer I., Heinrich J., and Trepka M.J., et al. The effect of lead in tap water on blood lead in children in a smelter town. Sci Total Environ 1998: 209: 255–271.
Mielke H.W., and Reagan P.L. Soil is an important pathway of human lead exposure. Environ Health Perspect 1998: 106: 217–229.
Moore M.R., Goldberg A., and Pocock S.J., et al. Some studies of maternal and infant lead exposure in Glasgow. Scott Med J 1982: 27: 113–122.
Needleman H.L., and Bellinger D. The Health Effects of Low Level Exposure to Lead. Ann Rev Pub Health 1991: 12: 111–140.
O’Flaherty E.J. Physiologically based models for bone-seeking elements IV. Kinetics of lead disposition in humans. Toxicol Appl Pharmacol 1993: 118: 16–29.
Rabin R. Warnings unheeded: a history of child lead poisoning. Am J Pub Health 1989: 79: 1668–1674.
Rabinowitz M.B., Kopple J.D., and Wetherill G.W. Effect of food intake and fasting on gastrointestinal lead absorptions in humans. Am J Clin Nutr 1980: 33: 1784–1788.
Rabinowitz M.B., Wetherill G.W., and Kopple J.D. Magnitude of lead intake from respiration by normal man. J Lab Clin Med 1977: 90: 238–248.
Rice D. Issues in Developmental Neurotoxicology: Interpretation and Implication of the Data. Can J Pub Health 1998: 89, (Supp l l1) S31–36.
Rodes C., Newsome J.R., Vanderpool R.W., Antley J.T., and Lewis R.G. Experimental methodologies and preliminary transfer factor data for estimation of dermal exposure to particles. J Expos Anal Environ Epidemiol 2001: 11: 123–139.
Rosenblith J.F., and Sims-Knight J.E. In the Beginning. Brooks/Cole, Monterey, Ca, 1985.
Rossiter N.D., Chapman P., and Haywood I.A. How big is a hand? Burns 1996: 22: 230–231.
Schwartz J., and Levin R. The risk of lead toxicity in homes with lead paint hazard. Environ Res 1991: 54: 1–7.
Simon D., Thomas K., Swanepoel A., Banham D., Thomas R., and Jebb C. Infant Cohort Pilot Study Report: Investigation into the Change in Blood Lead Levels of Infants Born in Port Pirie. Department of Human Services Internal Report, Adelaide, 2002.
Sutton P.M., Athanasoulis M., and Flessel P., et al. Lead levels in the household environment of children in three high-risk communities in California. Environ Res 1995: 68: 45–57.
Thomas K. Estimating the Surface Area of the Child's Hand. Department of Human Services Internal Report, Adelaide, 2001.
US EPA. Exposure Factors Handbook: Vol. 1. General factors. US EPA, Washington, 1997.
US EPA. Review of Adult Lead Models, US EPA Office of Emergency and Remedial Response Draft report EPA 9285 EPA, Washington, 2001.
US EPA. Third External Review Draft of Air Quality Criteria for Particulate Matter, Draft report EPA/600/P-99/002aC Research Triangle, NC, 2002.
Warren J.J., and Bishara S.E. Duration of nutritive and nonnutritive sucking behaviors and their effects on the dental arches in the primary dentition. Am J Orthod Dentofacial Orthop 2002: 121: 347–356.
Watt G.C., Britton A., Gilmour H.G., Moore M.R., Murray G.D., and Robertson S.J. Public health implications of new guidelines for lead in drinking water: a case study in an area with historically high water lead levels. Food Chem Toxicol 2000: 38: S73–S79.
Weih L Child Observation Study. South Australian Health Commission Internal Report, Adelaide, 1997.
Willson K., and Ryan P. Report on the Statistical Analysis of the Port Pirie Mouthing Behaviour and Blood/Hand Lead Study. South Australian Health Commission Internal Report, Adelaide, 1999.
Yiin L.M., Rhoads G.G., and Lioy P.J. Seasonal influences on childhood lead exposure. Environ Health Perspec 2000: 108: 177–182.
Acknowledgements
We extend our special thanks to the families who participated in the project. Thanks also to Raylene Thomas and Charmayne Jebb for helping with the recruitment of families, for regular discussions and for following up on various requests. Ted Maynard, Cathy Phipps, Kathy Thomas, Monika Nitschke, Anna Swanepoel, Graham Ohmsen, and Deb Nelson provided ongoing discussions on the project, both scientific and sociological. Finally, thanks to all of the Port Pirie Lead group staff for feedback on the project.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kranz, B., Simon, D. & Leonardi, B. The behavior and routes of lead exposure in pregrasping infants. J Expo Sci Environ Epidemiol 14, 300–311 (2004). https://doi.org/10.1038/sj.jea.7500325
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.jea.7500325
Keywords
This article is cited by
-
Positive outcomes from U.S. lead regulations, continued challenges, and lessons learned for regulating emerging contaminants
Environmental Science and Pollution Research (2023)
-
The association between prenatal endocrine-disrupting chemical exposure and altered resting-state brain fMRI in teenagers
Brain Structure and Function (2020)
-
Follow-up study on lead exposure in children living in a smelter community in northern Mexico
Environmental Health (2011)
-
Living in a sea of lead — changes in blood- and hand-lead of infants living near a smelter
Journal of Exposure Science & Environmental Epidemiology (2007)
-
Video methods in the quantification of children's exposures
Journal of Exposure Science & Environmental Epidemiology (2006)