Summary:
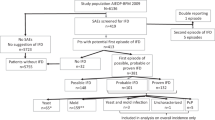
Invasive fungal infections (IFI) are the leading cause of infectious mortality in adult patients undergoing hematopoietic cell transplantation (HCT) after myeloablative conditioning, but the extent of this problem in the pediatric population is unclear. We retrospectively examined risk factors for IFI among 120 consecutive pediatric patients undergoing allogeneic HCT at a single center. The incidence of proven or probable IFI in pediatric patients during the first year after allogeneic HCT was 13%, comparable to the rate reported in adult patients; however, unlike IFI in adult patients, the majority of IFI in children occurred within the first month after transplantation. The primary risk factors for IFI were duration of neutropenia, age greater than 10 years, transplant for severe aplastic anemia or Fanconi anemia, and high-dose corticosteroid administration for 10 days or longer. IFI were more likely to be successfully treated (42%, 5/12 patients) in pediatric HCT recipients when compared to previous reports of adult recipients. Nonrelapse mortality was estimated at 17% (20/120 patients) after allogeneic HCT, of which 35% (seven patients) were directly attributed to IFI. Thus, IFI is a significant cause of nonrelapse mortality in children undergoing allogeneic HCT and more effective strategies are needed to prevent and treat IFI.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Gross TG, Egeler RM, Smith FO . Pediatric hematopoietic stem cell transplantation. Hematol Oncol Clin N Am 2001; 15: 795–808.
Marr KA, Carter RA, Crippa F et al. Epidemiology and outcome of mould infections in hematopoietic stem cell transplant patients. Clin Infect Dis 2002; 34: 909–917.
Van Burik JH, Weisdorf DJ . Infections in recipients of blood and marrow transplantation. Hematol Oncol Clin N Am 1999; 13: 1065–1089.
Brown JMY . Fungal infections in bone marrow transplant patients. Curr Opin Infect Dis 2004; 17: 347–352.
Momin F, Chandrasekar PH . Antimicrobial prophylaxis in bone marrow transplantation. Ann Intern Med 1995; 123: 205–215.
Rolston K . Overview of systemic fungal infections. Oncology (Huntington) 2001; 15 (11 Suppl. 9): S11–S14.
Hovi L, Saarinen-Pihkala UM, Vettenranta K, Saxen H . Invasive fungal infections in pediatric bone marrow transplant recipients: single center experience for 10 years. Bone Marrow Transplant 2000; 26: 999–1004.
Busca A, Saroglia EM, Giacchino M et al. Analysis of early infectious complications in pediatric patients undergoing bone marrow transplantation. Support Care Cancer 1999; 7: 253–259.
Benjamin DKJ, Miller WC, Bavliff S et al. Infections diagnosed in the first year after pediatric stem cell transplantation. Pediatr Infect Dis J 2002; 21: 227–234.
Hoover M, Morgan ER, Kletzel M . Prior fungal infection is not a contraindication to bone marrow transplant in patients with acute leukemia. Med Pediatr Oncol 1997; 28: 268–273.
Martino R, Nomdedeu J, Altes A et al. Successful bone marrow transplantation in patients with previous invasive fungal infections: report of four cases. Bone Marrow Transplant 1994; 13: 265–269.
Richard C, Romon I, Baro J et al. Invasive pulmonary aspergillosis prior to BMT in acute leukemia patients does not predict a poor outcome. Bone Marrow Transplant 1993; 12: 237–241.
Fukuda T, Boeckh M, Guthrie KA et al. Invasive aspergillosis before allogeneic hematopoietic stem cell transplantation: 10-year experience at a single transplant center. Biol Blood Marrow Transplant 2004; 10: 494–503.
Bielorai B, Toren A, Wolach B et al. Successful treatment of invasive aspergillosis in chronic granulomatous disease by granulocyte transfusions followed by peripheral blood stem cell transplantation. Bone Marrow Transplant 2000; 26: 1025–1028.
Dallorso S, Manzitti C, Dodero P et al. Uneventful outcome of unrelated hematopoietic stem cell transplantation in a patient with leukemic transformation of Kostmann syndrome and long-lasting invasive pulmonary mycosis. Eur J Haematol 2003; 70: 322–325.
Przepiorka D, Weisdorf D, Martin P et al. Consensus conference on acute GVHD grading. Bone Marrow Transplant 1995; 15: 825–828.
Sullivan KM, Agura E, Anasetti C et al. Chronic graft-versus-host disease and other late complications of bone marrow transplantation. Semin Hematol 1991; 28: 250–259.
Riley DK, Pavia AT, Beatty PG et al. The prophylactic use of low-dose amphotericin B in bone marrow transplant patients. Am J Med 1994; 97: 509–514.
Ascioglu S, Rex JH, de Pauw B et al. Defining opportunistic invasive fungal infections in immunocompromised patients with cancer and hematopoietic stem cell transplants: an international consensus. Clin Infect Dis 2002; 34: 7–14.
Dini G, Castagnola E, Comoli P et al. Infections after stem cell transplantation in children: state of the art and recommendations. Bone Marrow Transplant 2001; 28 (Suppl. 1): S18–S21.
Fukada T, Boeckh M, Carter RA et al. Risks and outcomes of invasive fungal infections in recipients of allogeneic hematopoietic stem cell transplants after nonmyeloablative conditioning. Blood 2003; 102: 827–833.
Busca A, Locatelli F, Barbui A et al. Infectious complications following nonmyeloablative allogeneic hematopoietic stem cell transplantation. Transplant Infect Dis 2004; 5: 132–139.
Wolff SN, Fay J, Stevens D et al. Fluconazole vs low-dose amphotericin B for the prevention of fungal infections in patients undergoing bone marrow transplantation: a study of the North American Marrow Transplant Group. Bone Marrow Transplant 2000; 25: 853–859.
Baddley JW, Stroud TP, Salzman D, Pappas PG . Invasive mold infections in allogeneic bone marrow transplant recipients. Clin Infect Dis 2001; 32: 1319–1324.
Benhamou E, Hartmann O, Nogues C et al. Does ketoconazole prevent fungal infection in children treated with high dose chemotherapy and bone marrow transplantation? Results of a randomized placebo-controlled trial. Bone Marrow Transplant 1991; 7: 127–131.
Klingspor L, Stintzing G, Fasth A, Tollemar J . Deep candidal infections in children receiving allogeneic bone marrow transplants: incidence, risk factors and diagnosis. Bone Marrow Transplant 1996; 17: 1043–1049.
Hoppe JE, Klausner M, Klingebiel T, Niethammer D . Retrospective analysis of yeast colonization and infections in paediatric bone marrow transplant recipients. Mycoses 1997; 40: 47–54.
Sullivan KM, Dykewicz CA, Longworth DL et al. Preventing opportunistic infections after hematopoietic stem cell transplantation. American Society of Hematology Education Program Book. American Society of Hematology: Washington, DC, USA, 2003, pp 392–397.
Wald A, Leisenring W, van Burik JA, Bowden RA . Epidemiology of Aspergillus infection in a large cohort of patients undergoing bone marrow transplantation. J Infect Dis 1997; 175: 1459–1466.
Ayas M, Solh H, Mustafa MM et al. Bone marrow transplantation from matched siblings in patients with Fanconi anemia utilizing low-dose cyclophosphamide, thoracoabdominal radiation and antithymocyte globulin. Bone Marrow Transplant 2001; 27: 139–143.
Flowers ME, Doney KC, Storb R et al. Marrow transplantation for Fanconi anemia with or without leukemic transformation: an update of the Seattle experience. Bone Marrow Transplant 1992; 9: 167–173.
Marr KA . Antifungal prophylaxis in hematopoietic stem cell transplant recipients. Oncology (Huntington) 2001; 15: 15–19.
Koh LP, Kurup A, Goh YT et al. Randomized trial of fluconazole versus low-dose amphotericin B in prophylaxis against fungal infections in patients undergoing hematopoietic stem cell transplantation. Am J Hematol 2002; 71: 260–267.
Stevens DA, Kan VL, Judson MA et al. Practice guidelines for diseases caused by Aspergillus. Infectious Diseases Society of America. Clin Infect Dis 2000; 30: 696–709.
Avivi I, Oren I, Haddad N et al. Stem cell transplantation post invasive fungal infection is a feasible task. Am J Hematol 2004; 75: 6–11.
Acknowledgements
We thank Michael Amylon, Yisheng Lee, Karen Kristovich, and the medical & nursing staffs at Lucile Packard Children's Hospital at Stanford University Medical Center for their dedicated care of the patients in this study.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Dvorak, C., Steinbach, W., Brown, J. et al. Risks and outcomes of invasive fungal infections in pediatric patients undergoing allogeneic hematopoietic cell transplantation. Bone Marrow Transplant 36, 621–629 (2005). https://doi.org/10.1038/sj.bmt.1705113
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.bmt.1705113
Keywords
This article is cited by
-
Allogeneic Hematopoietic Stem Cell Transplant in a Pediatric Patient with Invasive Fungal Infections: Challenges and Indications
Current Fungal Infection Reports (2021)
-
A phase I dose finding study of intravenous voriconazole in pediatric patients undergoing hematopoietic cell transplantation
Bone Marrow Transplantation (2020)
-
Risk factors associated with development and mortality by invasive fungal diseases in pediatric allogeneic stem cell transplantation. A pediatric subgroup analysis of data from a prospective study of the Gruppo Italiano Trapianto di Midollo Osseo (GITMO)
Bone Marrow Transplantation (2018)
-
Antifungal Prophylaxis in Children Receiving Antineoplastic Chemotherapy
Current Fungal Infection Reports (2018)
-
Impact of the D-index deduced from duration and intensity of neutropenia following chemotherapy on the risk of invasive fungal infection in pediatric acute myeloid leukemia
International Journal of Hematology (2018)