Abstract
Cardiac damage is the major limiting factor for the clinical use of doxorubicin (DOX). Preclinical studies indicate that inflammatory effects may be involved in DOX-induced cardiotoxicity. Nɛ-(carboxymethyl) lysine (CML) is suggested to be generated subsequent to oxidative stress, including inflammation. Therefore, the aim of this study was to investigate whether CML increased in the heart after DOX and whether anti-inflammatory agents reduced this effect in addition to their possible protection on DOX-induced cardiotoxicity. These effects were compared with those of the potential cardioprotector 7-monohydroxyethylrutoside (monoHER). BALB/c mice were treated with saline, DOX alone or DOX preceded by ketoprofen (KP), dexamethasone (DEX) or monoHER. Cardiac damage was evaluated according to Billingham. Nɛ-(carboxymethyl) lysine was quantified immunohistochemically.
Compared to saline, a 21.6-fold increase of damaged cardiomyocytes was observed in mice treated with DOX (P<0.001). Addition of KP, DEX or monoHER before DOX significantly reduced the mean ratio of abnormal cardiomyocytes in comparison to mice treated with DOX alone (P⩽0.02). In addition, DOX induced a significant increase in the number of CML-stained intramyocardial vessels per mm2 (P=0.001) and also in the intensity of CML staining (P=0.001) compared with the saline-treated group. Nɛ-(carboxymethyl) lysine positivity was significantly reduced (P⩽0.01) by DOX-DEX, DOX-KP and DOX-monoHER. These results confirm that inflammation plays a role in DOX-induced cardiotoxicity, which is strengthened by the observed DOX-induced accumulation of CML, which can be reduced by anti-inflammatory agents and monoHER.
Similar content being viewed by others
Main
Doxorubicin (DOX) is a successfully used anticancer drug. However, DOX-induced cumulative cardiotoxic effects, including cardiomyopathy and congestive heart failure, limit the use of this agent (Von Hoff et al, 1979; Signal and Iliskovic, 1998; Gharib and Burnett, 2002). Various molecular mechanisms have been suggested. Doxorubicin-induced free radicals are believed to play a central role in its cardiotoxicity (Yen et al, 1996; Horenstein et al, 2000; Xu et al, 2001).
Earlier studies illustrated that DOX also induces inflammatory effects in the vasculature and in the myocardium (Hecker, 1990; Fujihira et al, 1993) and increases proinflammatory cytokines (TNF-α, IL-1β and IL-2). Doxorubicin elevates NF-κB (Baeuerle, 1991; Read et al, 1994; Goto et al, 1999; Hou et al, 2005; Deepa and Varalakshmi, 2006) and the adhesion molecules VCAM-1 and E-selectin (Abou El Hassan et al, 2003). In vitro data showed that DOX affected both the viability and neutrophil adhesion of endothelial cells with clinically achievable concentrations (Abou El Hassan et al, 2003). These inflammatory effects may play a role in DOX-induced cardiotoxicity and results of some studies support these indications (Inchiosa Jr and Smith, 1990; Chen et al, 2005; Hou et al, 2005).
Protein damage caused by oxidative stress, inflammation or hyperglycaemia leads to carbohydrate-derived advanced glycation end products (AGEs) such as Nɛ-(carboxymethyl)lysine (CML) (Miyata et al, 1997; Hudson et al, 2003). Elevated levels of CML were demonstrated in patients with renal failure, in intramyocardial arteries of the heart of diabetic patients (Schalkwijk et al, 2004) and in patients with atherosclerosis having inflammatory/pro-oxidative environments (Degenhardt et al, 1997; Schleicher et al, 1997). Nɛ-(carboxymethyl) lysine is produced under oxidative stress (Miyata et al, 1997; Nagai et al, 1997) and may therefore be regarded as a biomarker for local endogenous oxidative stress, next to local inflammatory stress (Baynes, 1991; Nerlich and Schleicher, 1999). After binding to the receptor for AGE, CML activates endothelial cells as indicated by the induction of adhesion molecules such as VCAM-1 (Boulanger et al, 2002). Therefore, the first aim of our study was to investigate whether CML increases in intramyocardial arteries after treatment with DOX. Because inflammatory processes are involved the second aim of our study was to investigate whether anti-inflammatory agents would reduce DOX-induced CML increase.
In the past, we have shown the cardioprotective properties of the antioxidant 7-monohydroxyethylrutoside (monoHER) against DOX-induced cardiotoxicity in mouse (Van Acker et al, 1997; Van Acker et al, 2000). In vitro, we have also shown that monoHER protects against DOX-induced inflammatory effects (Abou El Hassan et al, 2003). Therefore, the effect of monoHER on DOX-induced CML increase was also investigated in the in vivo mouse model.
Furthermore, a possible protective effect of the anti-inflammatory drugs ketoprofen (KP) and dexamethasone (DEX) on DOX-induced cardiotoxicity in comparison to the protective effect of monoHER was investigated in this model.
Materials and methods
Chemicals
7-Monohydroxyethylrutoside was kindly provided by Novartis Consumer Health (Nyon, Switzerland). The drug was formulated and dissolved as described before, giving a final concentration of 33 mg/ml (Bruynzeel et al, 2006). Formulated DEX (dexamethasone 4 mg/ml) was obtained from the Pharmacy Department, VU Medical Center (Amsterdam, the Netherlands). Before injection, the content of the ampoule was diluted in sterile saline to obtain a concentration of 2 mg/ml. Formulated KP (1% ketoprofen) was obtained from Merial B.V. (Amstelveen, the Netherlands). A volume of 0.5 ml KP was added to 19.5 ml PBS to obtain a concentration of 0.025% KP (0.25 mg/ml). Formulated DOX (doxorubicin hydrochloride, 2 mg/ml) was obtained from Pharmachemie B.V. (Haarlem, the Netherlands). Before injection, the content of the vial was diluted in a sterile 0.9% NaCl solution to a concentration of 1 mg/ml.
Animals
Thirty-six male BALB/c mice (20–25 g) obtained from Harlan Nederland (Horst, the Netherlands) were kept in a light and temperature-controlled room (21–22°C; humidity 60–65%). The animals were fed a standard diet (Harlan Teklad) and allowed to eat and drink tap water ad libitum. The animals were allowed to adapt to the laboratory housing conditions for 2 weeks before starting the experiment.
Experimental design
The protocol was approved by the ethics committee for animal experiments of the Vrije Universiteit (Amsterdam, the Netherlands) and the methodology was also in compliance with the UKCCCR guidelines on ethical use of animals.
Thirty mice were submitted to one of the following weekly dosing schedules for 6 weeks:
- Group 1 (n=6):
-
0.1 ml 0.9% NaCl solution i.v.+0.3 ml 0.9% NaCl solution s.c. 60 min before i.v. injection, and 6, 24 and 48 h after i.v. injection
- Group 2 (n=6):
-
4 mg/kg DOX i.v.+0.3 ml 0.9% NaCl solution s.c. 60 min before DOX and 6, 24 and 48 h after DOX
- Group 3 (n=6):
-
4 mg/kg DOX i.v.+2 mg/kg KP s.c. 30 min before DOX, and 6, 24 and 48 h after DOX
- Group 4 (n=6):
-
4 mg/kg DOX i.v.+8 mg/kg DEX s.c. 60 min before DOX, and 6, 24 and 48 h after DOX
- Group 5 (n=6):
-
4 mg/kg DOX i.v.+500 mg/kg monoHER i.p. 60 min before DOX
DOX was administered via the tail vein. Six mice were killed just before starting treatment (control group) and their heart tissue was used as a control at the beginning.
During treatment and a 2-week observation period thereafter, body weight was determined twice a week as a measure of general toxicity. After the treatments and the observation period, the mice were killed.
Tissue samples
The hearts were excised and the central part of both ventricles was cut into 5-mm-thick pieces of 2–3 mm, which were fixed in 2% phosphate-buffered glutaraldehyde solution or in 4% formalin.
Histological analyses
After fixation in 2% phosphate-buffered glutaraldehyde solution the heart tissue was post-fixed in 1% osmium tetroxide. The tissue was then dehydrated through a graded series of ethanol solutions of 70–95% and embedded in JB-4 Plus resin. Thereafter 0.5–3.0-μm-thick sections were cut with a glass knife. These semithin sections were examined by light microscopy and DOX-induced cardiac damage was evaluated according to Billingham et al (1978). For this purpose the percentage of cardiac cells that had been damaged was established. Cardiac myocytes with more than two vacuoles or loss of myofibrils were counted as deviant. The scoring area was measured using a commercially available interactive video overlay-based measuring system (Q-Prodit, Leica, Cambridge, UK; Vermeulen et al, 2001). For each mouse the number of aberrant myocytes per mm2 was scored.
Immunohistochemical methods
After fixation in 4% formalin the heart tissue was embedded in paraffin. Paraffin-embedded cardiac tissue sections (4 μm) were mounted on microscope slides and were deparaffinised for 10 min in xylene at room temperature and dehydrated by decreasing concentrations of ethanol. Sections were then stained with haematoxylin and eosin. Subsequent to deparaffinisation and dehydration, sections were incubated with 0.3% hydrogen peroxide in methanol for 30 min to block endogenous peroxidase activity. Sections were not heated to prevent artificial induction of CML by this procedure (Dunn et al, 1989). Sections were preincubated with normal rabbit serum (1:50, Dako, Glostrup, Denmark) for 10 min and incubated for 60 min with anti-CML (1 : 500), both at room temperature. After washing in phosphate-buffered saline (PBS), pH 7.4, sections were incubated for 30 min with rabbit anti-mouse biotin-labelled antibody (1 : 500, Dako) at room temperature and subsequently washed in PBS. After incubation with streptavidin horseradish peroxidase (1 : 200, Dako) for 60 min at room temperature, peroxidase was visualised with 3,3-diamino-benzidine-tetrahydrochloride/H2O2 (Sigma Chemical Company, St Louis, MO, USA) for 3–5 min.
The CML staining intensity was scored in the intramyocardial arteries. For the intensity scoring each positive vessel was given a score of: 1=weak positivity, 2=moderate positivity or 3=strong positivity, according to a previous study (Schalkwijk et al, 2004). Subsequently, the scoring area was calculated as described before (Vermeulen et al, 2001). For each mouse the total number of CML staining arteries per mm2 was scored. Thereafter the difference in the CML staining intensity of the intramyocardial arteries per mm2 was investigated between the experimental groups.
Statistical analysis
For the analyses, the number of aberrant cardiac myocytes was log-transformed, yielding an unskewed variable. Differences between experimental groups were assessed using Student's two-sided t-test. The level of significance was set at 5%. Ninety-five percent confidence intervals (CI) on the original scale were obtained by exponentiating the upper and lower bounds of the 95% confidence intervals constructed on the log-scale. All calculations were performed with SPSS version 9.0 (SPSS, Chicago, IL, USA). For the analyses, the difference between the experimental groups regarding the number of vessels positive for CML staining and the intensity scoring per mm2 was assessed using Student's two-sided t-test. The level of significance was chosen at 5%. These calculations were also performed with SPSS version 9.0. To examine whether the contribution of moderately and strongly stained CML vessel walls differed among treatment groups, Fisher's exact test was applied and also Student's two-sided t-test.
Results
Animals appeared lively throughout the study and no behavioral changes were observed between the treatment groups. There were no signs of decreased activity, indicating low general toxicity. No significant differences were observed in weight between the experimental groups. No signs of gastrointestinal toxicity were observed in the mice treated with KP.
Histological examination of the cardiomyocytes
Histology of the hearts from the control and saline group did not show damaged cardiac myocytes, indicating that environmental factors and treatment with saline did not influence cardiac health of the animals. Treatment with DOX alone induced a significant 21.6-fold (95% CI 6.2–74.5) increase of damaged cardiac myocytes in comparison to the saline-treated group (P<0.001). Heart tissue of all mice treated with DOX alone or in combination with KP, DEX or monoHER, particularly showed vacuolar degeneration, whereas loss of myofibrils was rarely detected.
Table 1 shows the ratio of the mean number of aberrant cardiac myocytes per mm2 in all groups in comparison to the group treated with DOX. The addition of KP 30 min before and 6, 24 and 48 h after DOX injection resulted in a significant protective effect by reducing the ratio of the mean number of abnormal cardiac cells per mm2 with a factor 4.4 (95% CI 1.4–14.3, P=0.021). When DEX was added 60 min before DOX injection and 6, 24 and 48 h after DOX administration, a significant protective effect was also detected (P=0.006). Cotreatment with DEX led to a 6.2-fold reduction of deviant cardiac cells (95% CI 1.9–20.0) compared to the mice treated with DOX alone. The protective effect by adding monoHER before DOX led to a significant 8.6-fold (P=0.002, 95% CI 2.6–27.8) reduction of abnormal cardiomyocytes.
Table 1 also shows the ratio of the mean number of aberrant cardiac myocytes per mm2 in treated versus saline treated animals. When KP or DEX was added before DOX administration, significantly more abnormal cardiac myocytes were observed in comparison to the saline group, indicating that the protection was not complete (for KP a 4.9-fold increase, 95% CI 1.4–17.0, P=0.014; for DEX a 3.5-fold increase, 95% CI 1.0–12.0, P=0.049). When monoHER was added before DOX treatment, no significant increase of aberrant cardiac myocytes was detected compared with the saline-treated group (P=0.137). No significant difference was found between the groups treated with the combinations DOX-monoHER, DOX-KP and DOX-DEX (P>0.05).
Immunohistochemical staining of CML
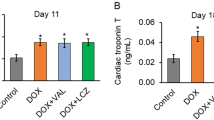
Nɛ-(carboxymethyl)lysine positivity was found in intramyocardial blood vessels, especially endothelium and partly smooth muscle cells in DOX-treated mice. Doxorubicin treatment induced a significant increase in the number of CML-stained vessels per mm2 compared with the group treated with saline (P=0.001) irrespective of the intensity score. Figure 1A illustrates immunohistochemical detection of CML in heart tissue of a mouse after treatment with DOX alone, whereas Figure 1B is a slide without addition of the primary antibody. Treatment of the animals with DOX in combination with DEX, KP or monoHER significantly reduced the amount of blood vessels positive for CML compared with the DOX-treated animals (P=0.004, 0.009 and 0.006, respectively). No difference was found in the number of vessels positive for CML between the groups treated with DOX combined with DEX, KP or monoHER and the animals treated with saline (P=0.633, 0.424 and 0.514, respectively). When comparing the amount of vessels positive for one of the three categories of intensity scores for CML (weak, moderate and strong) no difference was found between the five treatment groups for weakly stained positive CML vessels per mm2 (P=0.887), but when the mean number of moderately and strongly stained vessels per mm2 were combined for each experimental group, a significantly enhanced staining for CML (P=0.001) was found between the mice treated with DOX alone and the animals treated with saline (Figure 2). Dexamethasone, KP and monoHER reduced this enhancing effect of DOX significantly (P=0.003, 0.014 and 0.007, respectively). No significant difference in staining was found between the animals treated with saline and those treated with the combination DOX-DEX, DOX-KP or DOX-monoHER (P=0.659, 0.275 and 0.424, respectively). These results indicate that all three combinations significantly reduce the enhancing effect of DOX on CML intensity.
The mean number of vessels per mm2 weakly, moderately and strongly positive after staining for CML in intramyocardial vessels in the heart tissue of treated mice. A significant difference (P=0.001) was found between the mice treated with DOX alone and the animals treated with saline when the mean number of moderately plus strongly stained vessels per mm2 were considered (* no significant difference in the mean number of strongly plus moderately stained CML vessels per mm2 in comparison to the saline-treated group and P⩽0.01 when compared with the DOX-treated group).
Discussion
In this study, we showed that addition of ketoprofen and dexamethasone during treatment with DOX reduced its cardiac damage in vivo. In addition, it was demonstrated that treatment with DOX induces an increase of CML in intramyocardial arteries in mice, which is reduced by these anti-inflammatory agents and monoHER.
Although DOX-induced free radicals are believed to play a central role in its cardiotoxicity (Yen et al, 1996; Horenstein et al, 2000, 57; Xu et al, 2001), the precise mechanism of myocardial impairment remains unclear. Several studies showed that inflammatory effects are directly and indirectly caused by treatment with DOX. In vitro it was shown that DOX directly induced neutrophil adhesion of vascular endothelial cells via the overexpression of VCAM and E-selectin (Abou El Hassan et al, 2003), whereas results of another study suggest that treatment with DOX produced marked inflammatory changes in heart tissue, liver and kidneys (Deepa and Varalakshmi, 2005). Results of our study confirm the contribution of inflammation in DOX-induced cardiotoxicity, because anti-inflammatory agents can at least, in part, reduce DOX-induced cardiotoxicity.
It has been suggested that DOX also induces endothelial dysfunctions (Kotamraju et al, 2002; Wolf and Baynes, 2006), because it has been demonstrated in vivo that treatment with DOX caused oxidative stress and myeloperoxidase (MPO) activity (Fadillioglu et al, 2004). Nɛ-(carboxymethyl)lysine can be formed by oxidative stress (Baynes, 1991; Nerlich and Schleicher, 1999), and also by the enzyme MPO (Anderson et al, 1999). In a recent study, was found that CML positivity colocalised with E-selectin-positive endothelial cells in the heart (Baidoshvili et al, 2006). Earlier it was demonstrated that DOX induced neutrophil adhesion that was mediated via overexpression of E-selectin (Abou El Hassan et al, 2003). Therefore, it is tempting to speculate that CML is derived from these pathways and could play a role in DOX-induced vascular endothelial injury and subsequent cardiotoxicity.
It is known that CML interacts with cells through a specific receptor system for AGEs (RAGE) (Zill et al, 2001). Activation of RAGE by binding of CML is thought to lead to the nuclear translocation of NF-κB (Sousa et al, 2000) and the activation of several secondary messenger systems that increase the production of proinflammatory cytokines and adhesion molecules (Boulanger et al, 2002). These events lead to progressing inflammation and a further increase of formation and accumulation of CML. Several approaches have been used to block the formation of AGE or the interaction of AGEs with RAGE to reduce complications (Brownlee et al, 1986; Panagiotopoulos et al, 1998; Bucciarelli et al, 2002). From these studies it appeared that reduction or even prevention of the formation of CML seems to be important to prevent endothelial dysfunction, and besides, this also reduces inflammation.
In line with this, we have demonstrated in another study increased accumulation of CML in intramyocardial arteries of diabetic patients and suggested that CML contributes to the increased risk of heart complications in diabetes mellitus (C Schalkwijk and HWM Niessen, unpublished observation).
In the present study, we showed that monoHER significantly reduced CML positivity and intensity of intramyocardial arteries. As monoHER has been shown to have radical scavenging properties (Haenen et al, 1993; Van Acker et al, 1993, 1997, 2000), this again points to a role of free radicals in CML production by DOX. We also found that anti-inflammatory agents decreased CML positivity and intensity in intramyocardial arteries (Figure 1). It has indeed been suggested that inflammation is another source of CML formation (Daugherty et al, 1994; Anderson and Heinecke, 2003). It has, however, to be noticed that glucocorticoids and NSAIDs also have antioxidant properties (Hamburger and Mc Cay, 1990; Kataoka et al, 1997; Ozmen, 2005; Chen et al, 2005; Yamada et al, 2006) besides their anti-inflammatory properties (Koehler et al, 1990; Masferrer and Seibert, 1994; Auphan et al, 1995; Scheinman et al, 1995; Morteau, 2000).
As a representative of the NSAIDs, we used KP because it is a strong non-selective COX-inhibitor and it is available for s.c. injection. Dexamethasone was chosen as a representative of the glucocorticosteroids, because of its known strong anti-inflammatory properties.
By using the earlier mentioned treatment schedules for KP and DEX, we intended to maintain the presence of the anti-inflammatory agents when DOX was administered and during the first 2 days thereafter, because the high peak levels of DOX during that period (Van der Vijgh et al, 1990) are considered of major importance in the development of DOX-induced cardiotoxicity (Von Hoff et al, 1979).
Up to the present, two studies reported protective effects of cotreatment with ibuprofen and glucocorticoids on DOX-induced cardiac damage. The first study (Inchiosa Jr and Smith, 1990) only evaluated survival, whereas the effect of glucocorticoids on DOX toxicity was only evaluated in vitro (Chen et al, 2005). At present, our study quantifies to what extent cardioprotection occurred in animals cotreated with DEX, KP and monoHER. It strongly confirms the role of inflammation in DOX-induced cardiotoxicity and indicates a possible way to protect (in part) against this toxicity.
High-dose DEX or prednisone is part of the DOX containing therapeutic treatment regimens in patients with aggressive non-Hodgkin's lymphoma or multiple myeloma (VAD, CHOP). Considering the results of our study, we reviewed data of these clinical studies concerning the cardiac consequences of the combined use of DOX and glucocorticoids for these patients and found out that up to the present little is known about the long-term effects on their cardiac tissue (Limat et al, 2003; Elbl et al, 2006). These clinical aspects merit further attention.
As mentioned earlier, it was believed that the cardioprotective effect of monoHER was mainly owing to its radical scavenging and iron-chelating properties; however, the results of the present study in combination with the in vitro study of Abou El Hassan et al (2003) indicate that monoHER also has anti-inflammatory properties.
Recently, anti-inflammatory activity was also shown for the flavonoids quercetin (Comalada et al, 2005), myricetin (Kang et al, 2005) and luteolin (Kim and Jobin, 2005).
A quantitative comparison between the three compounds (KP, DEX and monoHER) regarding their intrinsic anti-inflammatory and/or radical scavenging activities is not possible yet, because none of the doses nor the dosing regimes of the investigated protectors are optimised.
In conclusion, two anti-inflammatory agents of different classes, ketoprofen (NSAID) and dexamethasone (synthetic glucocorticoid) clearly protected against DOX-induced cardiotoxicity in mice by decreasing the number of abnormal cardiac myocytes. These results establish the suggestion that inflammatory effects owing to treatment with DOX are involved in the development of DOX-induced cardiotoxicity. The role of DOX-induced inflammation in the development of its cardiac damage is confirmed by the observation that DOX induced accumulation of CML in intramyocardial arteries, which is significantly reduced after treatment with DEX, KP and monoHER. Further investigations are warranted to develop anti-inflammatory agents as a protector against DOX-induced cardiotoxicity.
Change history
16 November 2011
This paper was modified 12 months after initial publication to switch to Creative Commons licence terms, as noted at publication
References
Abou El Hassan MAI, Verheul HMW, Jorna AS, Schalkwijk C, Van Bezu J, Van der Vijgh WJF, Bast A (2003) The new cardioprotector monohydroxyethylrutoside protects against doxorubicin-induced inflammatory effects in vitro. Br J Cancer 89: 357–362
Anderson MM, Heinecke JW (2003) Production of N (epsilon)-(carboxymethyl)lysine is impaired in mice deficient in NADPH oxidase: a role for phagocyte-derived oxidants in the formation of advanced glycation end products during inflammation. Diabetes 52: 2137–2143
Anderson MM, Requena JR, Crowley JR, Thorpe SR, Heinecke JW (1999) The myeloperoxidase system of human phagocytes generates Nɛ – (carboxymethyl) lysine on proteins: a mechanism for producing advanced glycation end products at sites of inflammation. J Clin Invest 104: 103–113
Auphan N, DiDonato JA, Rosette C, Helmberg A, Karin M (1995) Immunosuppression by glucocorticoids: inhibition of NF-kappa B activity through induction of I kappa B synthesis. Science 270: 286–290
Baeuerle PA (1991) The inducible transcription activator NF-κB: regulation by distinct protein subunits. Biochim Biophys Acta 1072: 63–80
Baidoshvili A, Krijnen PAJ, Kupreishvili K, Ciurana C, Bleeker W, Nijmeijer R, Visser CA, Visser FC, Meijer CJLM, Stooker W, Eijsman L, Van Hinsbergh VW, Hack CE, Niessen HWM, Schalkwijk CG (2006) Nɛ-(carboxymethyl)lysine depositions in intramyocardial blood vessels in human and rat acute myocardial infarction. Arterioscler Thromb Vasc Biol 26: 2497–2503
Baynes JW (1991) Perspectives in diabetes. Role of oxidative stress in development of complications in diabetes. Diabetes 40: 405–412
Billingham ME, Mason JW, Bristow MR, Daniels JR (1978) Anthracycline cardiomyopathy monitored by morphologic changes. Cancer Treat Rep 62: 865–872
Boulanger E, Wautier MP, Wautier JL, Boval B, Panis Y, Wernert N, Danze PM, Dequiedt P (2002) AGEs bind to mesothelial cells via RAGE and stimulate VCAM-1 expression. Kidney Int 61: 148–156
Brownlee M, Vlassara H, Kooney A, Ulrich P, Cerami A (1986) Aminoguanidine prevents diabetes-induced arterial wall protein cross-linking. Science 232: 1629–1632
Bruynzeel AME, Mul PNN, Berkhof J, Bast A, Niessen HWM, van der Vijgh WJF (2006) The influence of the time-interval between monoHER and doxorubicin administration on the protection against doxorubicin-induced cardiotoxicity in mice. Cancer Chemother Pharmacol 58: 699–702
Bucciarelli LG, Wendt T, Qu W, Lu Y, Lalla E, Rong LL, Goova MT, Moser B, Kislinger T, Lee DC, Kashyap Y, Stern DM, Schmidt AM (2002) RAGE blockade stabilizes established atherosclerosis in diabetic apolipoprotein E-null mice. Circulation 106: 2827–2835
Chen QM, Alexander D, Sun H, Xie L, Lin Y, Terrand J, Morrissy S, Purdom S (2005) Corticosteroids inhibit cell death induced by doxorubicin in cardiomyocytes: induction of antiapoptosis, antioxidant, and detoxification genes. Mol Pharmacol 67: 1861–1873
Comalada M, Camuesco D, Sierra S, Ballester I, Xaus J, Galvez J, Zarzuelo A (2005) In vivo quercitrin anti-inflammatory effects involves release of quercitin, which inhibits inflammation through down-regulation of the NF-κB pathway. Eur J Immunol 35: 584–592
Daugherty A, Dunn JL, Rateri DL, Heinecke JW (1994) Myeloperoxidase, a catalyst for lipoprotein oxidation, is expressed in human atherosclerotic lesions. J Clin Invest 94: 437–444
Deepa PR, Varalakshmi P (2005) Biochemical evaluation of the inflammatory changes in cardiac, hepatic and renal tissues of adriamycin-administered rats and the modulatory role of exogenous heparin-derivative treatment. Chem Biol Interact 156: 93–100
Deepa PR, Varalakshmi P (2006) Influence of a low-molecular-weight heparin derivative on the nitric oxide levels and apoptotic DNA damage in adriamycin-induced cardiac and renal toxicity. Toxicology 217: 176–183
Degenhardt TP, Grass L, Reddy S, Thorpe SR, Diamandis EP, Baynes JW (1997) The serum concentration of the advanced glycation end-product N epsilon- (carboxymethyl) lysine is increased in uremia. Kidney Int 52: 1064–1067
Dunn JA, Patrick JS, Thorpe SR, Baynes JW (1989) Oxidation of glycated proteins: age-dependent accumulation of Nepsilon-(carboxymethyl) lysine in lens proteins. Biochemistry 28: 9464–9468
Elbl L, Vasova I, Tomaskova I, Jedlicka F, Navratil M, Pospisil Z, Vorlicek J (2006) Cardiac function and cardiopulmonary performance in patients after treatment for non-Hodgkin's lymphoma. Neoplasma 53: 174–181
Fadillioglu E, Oztas E, Erdogan H, Yagmurca M, Sogut S, Ucar M, irmak MK (2004) Protective effects of caffeic acid phenethyl ester on doxorubicin-induced cardiotoxicity in rats. J Appl Toxicol 24: 47–52
Fujihira S, Yamamoto T, Matsumoto M, Yoshizawa K, Oishi Y, Fujii T, Noquchi H, Mori H (1993) The high incidence of atrial thrombosis in mice given doxorubicin. Toxicol Pathol 21: 362–368
Gharib MI, Burnett AK (2002) Chemotherapy-induced cardiotoxicity: current practice and prospects of prophylaxis. Eur J Heart Fail 4: 235–242
Goto D, Izumi H, Ono M, Okamoto T, Kohno K, Kuwano M (1999) Tubular morphogenensis by genotoxic therapeutic agents that induce NF-κB activation in human vascular endothelial cells. Angiogenesis 2: 345–356
Haenen GRMM, Jansen FP, Bast A (1993) The antioxidant properties of five O- (beta-hydroxyethyl) rutosides of the flavonoid mixture Venoruton. Phlebology Suppl. 1: 10–17
Hamburger SA, Mc Cay PB (1990) Spin trapping of ibuprofen radicals: evidence that ibuprofen is a hydroxyl radical scavenger. Free Radic Res Commun 9: 337–342
Hecker JF (1990) Survival of intravenous chemotherapy infusion sites. Br J Cancer 62: 660–662
Horenstein MS, Van der Heide RS, L’Ecuyer TJ (2000) Molecular basis of anthracyclin-induced cardiotoxicity and its prevention. Mol Genet Metab 71: 436–444
Hou G, Dick R, Abrams GD, Brewer GJ (2005) Tetrathiomolybdate protects against cardiac damage by doxorubicin in mice. J Lab Clin Med 146: 299–303
Hudson BI, Bucciarelli LG, Wendt T, Sakaguchi T, Lalla E, Qu W, Lu Y, Lee L, Stern DM, Naka Y, Ramasamy R, Yan SD, Yan SF, D’Agati V, Schmidt AM (2003) Blockade of receptor for advanced glycation endproducts: a new target for therapeutic intervention in diabetic complications and inflammatory disorders. Arch Biochem Biophys 419: 80–88
Inchiosa Jr MA, Smith CM (1990) Effects of ibuprofen on doxorubicin toxicity. Res Commun Chem Pathol Pharmacol 67: 63–78
Kang BY, Kim SH, Cho D, Kim TS (2005) Inhibition of interleukin-12 production in mouse macrophages via decreased nuclear factor-kappaB DNA binding activity by myricetin, a naturally occurring flavonoid. Arch Pharm Res 28: 274–279
Kataoka M, Tonooka K, Ando T, Imai K, Aimoto T (1997) Hydroxyl radical scavenging activity of non-steroidal anti-inflammatory drugs. Free Radic Res 27: 419–427
Kim JS, Jobin C (2005) The flavonoid luteolin prevents lipopolysaccharide- induced NF-kappaB signaling and gene expression by blocking IkappaB kinase activity in intestinal epithelial cells and bone-marrow derived dendritic cells. Immunology 115: 375–387
Koehler L, Hass R, DeWitt DL, Resch K, Goppelt-Struebe M (1990) Glucocorticoid- induced reduction of prostanoid synthesis in TPA-differentiated U937 cells is mainly due to a reduced cyclooxygenase activity. Biochem Pharmacol 40: 1307–1316
Kotamraju S, Chitambar CR, Kalivendi SV, Joseph J, Kalyanaraman B (2002) Transferrin receptor-dependent iron uptake is responsible for doxorubicin-mediated apoptosis in endothelial cells. J Biol Chem 277: 17179–17187
Limat S, Demesmay K, Bernard Y, Deconinck E, Brion A, Sabbah A, Woronoff-Lemsi MC, Cahn JY (2003) Early cardiotoxicity of the CHOP regimen in aggressive non-Hodgkin's lymphoma. Ann Oncol 14: 277–281
Masferrer JL, Seibert K (1994) Regulation of prostaglandin synthesis by glucocorticosteroids. Receptor 4: 25–30
Miyata T, Wada Y, Cai Z, Iida Y, Horie K, Yasuda Y, Maeda K, Kurokawa K, van Ypersele de Strihou C (1997) Implication of an increased oxidative stress in the formation of advanced glycation end products in patients with end-stage renal failure. Kidney Int 51: 1170–1181
Morteau O (2000) Prostaglandins and inflammation: the cyclooxygenase controversy. Arch Immunol Ther Exp 48: 437–480
Nagai R, Ikeda K, Higashi T, Sano H, Jinnouchi Y, Araki T, Horiuchi S (1997) Hydroxyl radical mediates Nɛ – (carboxymethyl) lysine formation from amadori product. Biochem Biophys Res Comm 234: 167–172
Nerlich AG, Schleicher ED (1999) Nɛɛ – (carboxymethyl) lysine in atherosclerotic vascular lesions as a marker for local oxidative stress. Atherosclerosis 144: 41–47
Ozmen I (2005) Evaluation of effect of some corticosteroids on glucose-6-phosphate dehydrogenase and comparative study of antioxidant enzyme activities. J Enzyme Inhib Med Chem 20: 19–24
Panagiotopoulos S, O’Brien KD, Bucala R, Cooper ME, Jerums G (1998) Aminoguanidine has an anti-atherogenic effect in the cholesterol-fed rabbit. Atherosclerosis 136: 125–131
Read MA, Whitley MZ, Williams AJ, Collins T (1994) NF-κB and IκBα: an inducible regulatory system in endothelial activation. J Exp Med 179: 503–512
Schalkwijk CG, Baidoshvili A, Stehouwer CD, van Hinsbergh VW, Niessen HW (2004) Increased accumulation of the glycoxidation product Nepsilon- (carboxymethyl) lysine in hearts of diabetic patients: generation and characterisation of a monoclonal anti-CML antibody. Biochim Biophys Acta 1636: 82–89
Scheinman RI, Cogswell PC, Lofquist AK, Baldwin Jr AS (1995) Role of transcriptional activation of I kappa B alpha in mediation of immunosuppression by glucocorticoids. Science 270: 283–286
Schleicher ED, Wagner E, Nerlich AG (1997) Increased accumulation of the glycoxidation product N (epsilon)-(carboxymethyl) lysine in human tissues in diabetes and aging. J Clin Invest 99: 457–468
Signal PK, Iliskovic N (1998) Doxorubicin-induced cardiomyopathy. N Engl J Med 339: 900–904
Sousa MM, Yan SD, Stern D, Saraiva MJ (2000) Interaction of the receptor for advanced glycation end products (RAGE) with transthyretin triggers nuclear transcription factor κB (NF- κB) activation. Lab Invest 80: 1101–1110
Van Acker FA, van Acker SA, Kramer K, Haenen GRMM, Bast A, van der Vijgh WJF (2000) 7-monohydroxyethylrutoside protects against chronic doxorubicin-induced cardiotoxicity when administered only once per week. Clin Cancer Res 6: 1337–1341
Van Acker SABE, Boven E, Kuiper K, van den Berg DJ, Grimbergen JA, Kramer K, Bast A, van der Vijgh WJF (1997) Monohydroxyethylrutoside, a dose-dependent cardioprotective agent, does not affect the antitumor activity of doxorubicin. Clin Cancer Res 3: 1747–1754
Van Acker SABE, Towart R, Husken BCP, de Jong J, van der Vijgh WJF, Bast A (1993) The protective effect of Venoruton and its constituents on acute doxorubicin-induced cardiotoxicity. Phlebology Suppl. 1: 31–32
Van der Vijgh WJF, Maessen PA, Pinedo HM (1990) Comparative metabolism and pharmacokinetics of doxorubicin and 4’-epidoxorubicin in plasma, heart and tumor of tumor-bearing mice. Cancer Chemother Pharmacol 26: 9–12
Vermeulen EG, Niessen HW, Bogels M, Stehouwer CD, Rauwerda JA, v.Hinsbergh VW (2001) Decreased smooth muscle cell / extracellular matrix ratio of femoral artery in patients with atherosclerosis and hyperhomocysteinemia. Arterioscler Thromb Vasc Biol 21: 573–577
Von Hoff DD, Layard MW, Basa P, Davis Jr HL, Von Hoff AL, Rozencweiq M, Muqqia FM (1979) Risk factors for doxorubicin-induced congestive heart failure. Ann Intern Med 91: 710–717
Wolf Mb, Baynes JW (2006) The anti-cancer drug, doxorubicin, causes oxidant stress-induced endothelial dysfunction. Biochim Biophys Acta 1760: 267–271
Xu MF, Tang PL, Oian ZM, Ashraf M (2001) Effects by doxorubicin on the myocardium are mediated by oxygen free radicals. Life Sci 68: 889–901
Yamada K, Nakamura T, Utsumi H (2006) Enhanced intra-articular free radical reactions in adjuvant arthritis rats. Free Radic Res 40: 455–460
Yen HC, Oberley TD, Vichitbandha S, Ho YS, St Clair DK (1996) The protective role of manganese superoxide dismutase against adriamycin-induced acute cardiac toxicity in transgenic mice. J Clin Invest 98: 1253–1260
Zill H, Gunther R, Erbersdobler HF, Folsch UR, Faist V (2001) RAGE expression and AGE-induced MAP-kinase activation in Caco-2 cells. Biochem Biophys Res Commun 288: 1108–1111
Acknowledgements
We thank Paula Mul and Suzanne Vormer-Bonne from the Clinical Animal Laboratory and Jan Fritz from the Department of Pathology of the Vrije Universiteit, Amsterdam, the Netherlands, for their excellent assistance.
Author information
Authors and Affiliations
Corresponding author
Additional information
This work was supported in part by grant VU-97-1525 from the Koningin Wilhelmina Foundation, Amsterdam, the Netherlands.
Rights and permissions
From twelve months after its original publication, this work is licensed under the Creative Commons Attribution-NonCommercial-Share Alike 3.0 Unported License. To view a copy of this license, visit http://creativecommons.org/licenses/by-nc-sa/3.0/
About this article
Cite this article
Bruynzeel, A., Abou El Hassan, M., Schalkwijk, C. et al. Anti-inflammatory agents and monoHER protect against DOX-induced cardiotoxicity and accumulation of CML in mice. Br J Cancer 96, 937–943 (2007). https://doi.org/10.1038/sj.bjc.6603640
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.bjc.6603640
Keywords
This article is cited by
-
sFRP1 protects H9c2 cardiac myoblasts from doxorubicin-induced apoptosis by inhibiting the Wnt/PCP-JNK pathway
Acta Pharmacologica Sinica (2020)
-
Advantages of prophylactic versus conventionally scheduled heart failure therapy in an experimental model of doxorubicin-induced cardiomyopathy
Journal of Translational Medicine (2019)
-
Customized laboratory TLR4 and TLR2 detection method from peripheral human blood for early detection of doxorubicin-induced cardiotoxicity
Cancer Gene Therapy (2017)
-
Aldose reductase inhibitor increases doxorubicin-sensitivity of colon cancer cells and decreases cardiotoxicity
Scientific Reports (2017)
-
6-gingerol ameliorated doxorubicin-induced cardiotoxicity: role of nuclear factor kappa B and protein glycation
Cancer Chemotherapy and Pharmacology (2012)