Key Points
Discusses:
-
The importance of a thorough oral examination.
-
Tumour as a possible differential diagnosis of a rapidly loosening denture.
-
The role to be played by clinical dental technicians.
Abstract
The following report describes the treatment carried out by a UK high street dental technician on an elderly patient with a large malignancy invading the oral cavity through the hard palate from the nose. The lesion remained undiagnosed during treatment for three months. The consequences of this error, and the future role of the clinical dental technician are discussed.
Similar content being viewed by others
Introduction
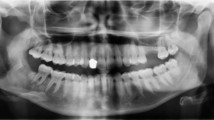
An 85-year-old female patient attended the Eastman Dental Hospital following referral from an ear, nose and throat surgeon. The patient had been diagnosed with a transitional cell carcinoma of the nasal septum (Fig. 1), which had invaded the oral cavity and presented with a large swelling of the hard palate (Fig. 2). The patient had been referred for the construction of a surgical plate to obturate the post-surgical defect, which would follow removal of the tumour from the hard palate.
A complete patient history was taken. The patient had been a denture wearer for 20 years. Although she had worn an upper complete denture for this length of time, she had never worn a lower complete denture. Three months previously, the patient experienced a sudden loss of retention of her upper complete denture. She attended a local high street denture technician who constructed a new denture. The patient reported that this denture was retentive initially but became loose within a few days. She returned to the dental technician who adjusted the denture, which again increased its retention. A few days later the same problem occurred, and the denture was adjusted again. This situation continued for three months, until following an examination of the oral cavity, the dental technician suggested the patient visited her dentist. Unfortunately the patient was not registered with a dental practitioner, and was seen by her general medical practitioner who, following examination, referred her to the Royal National Throat, Nose and Ear Hospital in London.
The patient was then examined, and impressions taken. Surgery was carried out, and a surgical plate fitted, which was later converted into a full coverage prosthetic obturator to cover the surgical defect (Fig. 3). Following this, the patient received a course of radiotherapy. The patient has experienced no recurrences, and continues to wear her obturator.
Discussion
The incidence of lip, mouth and pharyngeal cancer is relatively low, but increasing, with approximately 4,500 new cases being diagnosed each year in the United Kingdom. It is associated with a poor survival rate at five years of between 44% (male) and 52% (female).1 As well as primary lesions in the mouth, tumours may also arise as a result of metastasis2 or invade the oral cavity from adjacent tissues such as the nose.3 Nasal Transitional Cell Carcinoma is a rare malignancy which accounts for 8% of carcinomas of the nasal cavity and paranasal sinuses.4 In both oral and nasal cancer, diagnosis of an early stage tumour is essential, and is an important indicator of prognosis and hence survival.5,6
Delays in diagnosis7,8,9 and misdiagnosis10 of cancers presenting in the mouth have been reported in the literature. These have been due to errors by a range of healthcare professionals including referring practitioner, maxillofacial surgeon, and oral pathologist.11 A study12 investigating the culpability for delay in treatment looked at 1,000 cases of cancer originating at different sites around the body, and laid the blame on the following:
-
Patients, when a delay of over three months elapsed between onset of symptoms and visiting their physician and when they refused to accept their advice.
Physicians if they committed one of the following:
-
Wrong treatment.
-
Wrong advice.
-
No treatment or advice.
-
Acceptable treatment but delayed referral when no improvement for a month or more.
-
Unable to diagnose within a month, implying observation without treatment.
-
Patients and physicians were considered jointly responsible when errors relating to both occurred.
The majority of referrals for treatment of oral cancer come from general dental practitioners, though general medical practitioners also refer patients and have been shown to be better at diagnosing oral malignancy and referring patients early.7 Despite delays in referral by both types of practitioners, the most significant delay is still caused by the patient.13
Dental technicians carrying out clinical treatment legally or illegally have been given a variety of names, including denturists, denturologists, dental mechanics, or denture therapists.14 In Canada they have been carrying out clinical work legally since 1958, after organising public support.15 A survey regarding the opinions of dentists 20 years later showed the majority thought it was possible to work closely with a denturist, though they did not think they should be allowed to treat patients with natural teeth remaining.16
The number of people seeking treatment from dental technicians in the UK is unknown as any form of clinical treatment by them is illegal and therefore difficult to determine. Although dentists already provide a service for new and replacement dentures it is important and sometimes difficult to understand why they would need to visit a dental technician for treatment. In countries where denturism has been legal for some time, studies have shown that patients were equally satisfied with complete dentures provided by either dentists or denturists17,18 when they were not seeking to replace their dentures. However, mandibular dentures were more successful when provided by dentists in studies where patients were seeking replacement prostheses.19 From a patient's viewpoint, there appears to be little difference in perceived quality of care between dentists and denturists when information regarding this is available to patients,17 or not available when denturism is provided illegally.20 Patients attending both dentists and denturists come from similar socioeconomic backgrounds and on average pay similar fees for their dentures19 despite an attempt by some countries to introduce denturism to decrease the cost of prostheses.21 Interestingly, in a study looking at secondary school students' knowledge of oral cancer prevention and risk factors, a small percentage said a dental technician would be their first port of call on discovering a suspicious lesion.22
Where denturism is legalised, it has been found that those dental technicians who are not licensed continue to practice illegal dentistry and even those who legally practise it often provide treatment they are not supposed to.23 Denture technicians in the UK have no direct clinical role in the treatment of patients at present. General Dental Council (GDC) regulations prohibit clinical examination or treatment, though this situation will change when the role of clinical dental technician is established in the near future. Plans are already underway to extend the role of professions complementary to dentistry, and the establishment of the clinical dental technician is one of many ways in which the traditional service provided by general dental practitioners will be delegated to other professional colleagues.
At present, the only clinical professions complementary to dentistry are dental hygienists and dental therapists, both who work to prescription from registered dentists. This situation has been mutually beneficial, though hygienists and therapists have both had considerable training in clinically related matters. In countries where denturism is legal, co-operation between dentists and denturists is common, with both groups benefiting from more referrals from those they refer to.24 It has also been reported that following examination by dentists, patients appear to have better quality dentures (complete) when they have been provided by a trained denturist as compared to an illegally practising technician.25
This case report illustrates the importance of training in clinical examination, and also the importance of regular examination of edentulous patients. The delay in referral undoubtedly contributed to the morbidity associated with the case, in terms of the radical excision and radiotherapy needed. It would be hoped that the future training of clinical dental technicians would either involve working to a prescription from a registered dental practitioner, or would provide sufficient diagnostic skills to refer when necessary. As well as malignancy, non-fatal mucosal lesions associated with dentures are common in the elderly26 and sometimes require pre-prosthetic management.27 A proposed learning outcome set by the GDC is that clinical dental technicians should 'be competent at recognising abnormal oral mucosa and related underlying structures and at making an appropriate referral'.28 It would also be hoped that any future changes in the way that care is provided in the primary care setting, would include remuneration to general dental practitioners for examining edentulous patients as it does at present. Although no studies have shown screening reduces patient mortality, oral and oro-pharyngeal cancers found as a result of non-symptom driven examination have been found to be associated with a lower TNM stage which may require less aggressive and debilitating treatment to be carried out.29
Clinical treatment provided by high street dental technicians, apart from denture repairs needing no clinical treatment, is to be deplored. Although the potential for serious consequences resulting from non-diagnosis of malignancy presenting in the mouth by professions complementary to dentistry have been recognised for some time, no cases appear to have been documented.
Changes in legislation allowing the establishment of the clinical dental technician should be welcomed, as this will provide the necessary clinical training in areas excluding prosthesis construction, necessary for oral disease diagnosis.28 Hopefully the training places needed will be developed to fulfil this role quickly, unlike the case in New Zealand where despite changes in the law it took 11 years before anyone graduated in the discipline.30 It is hoped that this case report will be unique and no further cases are reported, and with good training established under the GDC regulations, malignancy should will be detected early by a greater range of dental professionals as it has in other countries.29
References
Office for National Statistics. Cancer trends in England and Wales: 1950-1999. London: The Stationary Office, 2001.
Florio SJ, Hurd TC. Gastric carcinoma metastatic to the mucosa of the hard palate. J Oral Maxillofac Surg 1995; 53: 1097–1098.
Tsang WM, Tong ACK, Lam KY, Tideman H. Nasal T/NK lymphoma: Report of three cases involving the palate. J Oral Maxillofac Surg 2000; 58: 1323–1327.
Robin PE, Jean PowellD, Stansbie JM. Carcinoma of the nasal cavity and paranasal sinuses: incidence and presentation of different histological types. Clin Otolaryngol 1979; 4: 431–456.
Platz H, Fries R, Hudec M. Prognoses of oral cavity carcinomas. p 187. München: Carl Hanser Verlag, 1986.
Bhattacharyya N. Cancer of the nasal cavity. Survival and factors influencing prognosis. Arch Otolaryngol Head Neck Surg 2002; 128: 1079–1083.
Schnetler JFC. Oral cancer diagnosis and delays in referral. Br J Oral Maxillofac Surg 1992; 30: 210–213.
Shafer WG. Initial mismanagement and delay in diagnosis of oral cancer. J Am Dent Assoc 1975; 90: 1262–1264.
Cooke BED, Tapper-Jones L. Recognition of oral cancer. Br Dent J 1977; 142: 96–98.
Gallagher CS, Svirsky JA. Misdiagnosis of squamous cell carcinoma as advanced periodontal disease. J Oral Med 1984: 39: 35–38.
Lovas JGL, Daley TD, Kaugers GE, Wright JM. Errors in the diagnosis of oral malignancies. J Can Dent Assoc 1993; 59: 935–938.
Pack GT, Gallo JS. The culpability for delay in the treatment of cancer. Am J Cancer 1938; 33: 443–462.
Hollows P, McAndrew PG, Perini MG. Delays in the referral and treatment of oral squamous cell carcinoma. Br Dent J 2000; 188: 262–265.
Rubinoff MS. Denturism — is the public at risk? J Can Dent Assoc 1996; 62: 167.
MacEntee MI. The denturist movement in Canada, Part I: growth and development in the western provinces. J Can Dent Assoc 1981; 47: 521–544.
MacEntee MI, Pierce CA, Williamson MF. Removable prosthodontic services by dentists in BC. J Can Dent Assoc 1980; 46: 764–767.
Friedrichsen SW, Herzog AE, Christie CA. A socioeconomic comparison of patients receiving prostheses in a two tier delivery system. J Prosthet Dent 1992; 67: 348–357.
Tuominen R. A comparison of dentists' and denturists' complete denture patients. Proc Finn Dent Soc 1988; 84: 53–59.
Morin C, Lund JP, Sioufi C, Feine JS. Patient satisfaction with dentures made by dentists and denturologists. J Can Dent Assoc 1998; 64: 205–212.
Garfunkel E. The consumer speaks: how patients select and how much they know about health care personnel. J Prosthet Dent 1980; 43: 380–384.
Rosenstein D, Empey G, Chiodo G, Phillips D. The effects of denturism on denture prices. Am J Public Health 1985; 75: 671.
Orlando A, Salerno P, Tarsitani G. Opinions and attitudes on oral cancer in a sample of students attending a state secondary school in Rome. Minerva Stomatol 2001; 50: 139–143.
Tuominen R. Removable dentures provided by dentists, denturists and laboratory technicians. J Oral Rehabil 2003a; 30: 55–59.
Tuominen, R. Cooperation and competition between dentists and denturists in Finland. Acta Odontol Scand 2002; 60: 98–102.
Tuominen, R. Clinical quality of removable dentures provided by dentists, denturists and laboratory technicians. J Oral Rehabil 2003; 30: 347–352.
MacEntee MI, Scully C. Oral disorders and treatment implications in people over 75 years. Comm Dent Oral Epidemiol 1988; 16: 271–273.
Bloem T, Razzoog M. Evaluation of denture supporting tissue health (Abstract). J Dent Res 1981; 60 (Special issue):784.
General Dental Council. Developing the dental team: Curricula frameworks for registrable qualifications for Professions Complimentary to Dentistry (PCDs). London: GDC, 2003.
Holmes JD, Dierks EJ, Homer LD, Potter BE. Is detection of oral and oropharyngeal squamous cancer by a dental health care provider associated with a lower stage at diagnosis? J Oral Maxillofac Surg 2003; 61: 285–291.
Carter GM, Innes PB. The postgraduate diploma in clinical dental technology. New Zealand Dent J 2000; 96: 53–56.
Author information
Authors and Affiliations
Corresponding author
Additional information
Refereed Paper
Rights and permissions
About this article
Cite this article
St George, G., Welfare, R. & Lund, V. An undiagnosed case of malignancy: Case report. Br Dent J 198, 341–343 (2005). https://doi.org/10.1038/sj.bdj.4812173
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.bdj.4812173
This article is cited by
-
Diffuse swelling of the buccal mucosa and palate as first and only manifestation of an extranodal non-Hodgkin ‘double-hit’ lymphoma: report of a case
Oral and Maxillofacial Surgery (2012)
-
Missed diagnosis
British Dental Journal (2005)
-
Missed diagnosis
British Dental Journal (2005)