Key Points
-
Hypertension is the most common modifiable risk factor for cardiovascular disease (CVD), and the risk of CVD events, including myocardial infarction, stroke, heart failure and end-stage renal disease, can be greatly reduced by lowering blood pressure.
-
The best-known regulator of blood pressure and determinant of target-organ damage from hypertension is the renin–angiotensin–aldosterone system (RAAS). Overexpression of renin and its metabolic products predisposes to hypertension and related target-organ damage.
-
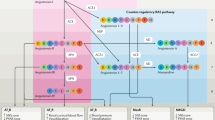
Renin cleaves angiotensinogen to produce the inactive peptide angiotensin I. Cleavage of angiotensin I by angiotensin-converting enzyme (ACE) gives the active peptide angiotensin II (although there are alternative routes). Most of the known functions of the RAAS are mediated through the activation of the angiotensin II type 1 receptor (AT1 receptor) by angiotensin II, which leads to vasoconstriction, aldosterone release and other functions that tend to elevate blood pressure and cause hypertrophy or hyperplasia of target cells.
-
Approved drugs that act on the RAAS that are discussed here include ACE inhibitors, AT1-receptor blockers (ARBs) and aldosterone-receptor antagonists (ARAs). These agents have been shown to be highly effective in lowering blood pressure and, particularly in the case of the ARBs, are extremely well tolerated. A novel class of combined ACE and neutral-endopeptidase inhibitors that are in development, called vasopeptidase inhibitors, are also discussed.
-
Clinical-trial evidence is beginning to clarify some of the key issues in the use of ACE inhibitors and ARBs, such as clinical benefits beyond blood-pressure lowering. These drugs are also helping to better define the role of the RAAS in the pathogenesis of hypertension, stroke, myocardial infarction, heart failure and end-stage renal disease.
Abstract
Effective antihypertensive therapy has made a major contribution to the reductions in the morbidity and mortality of cardiovascular disease that have been achieved since the 1960s. However, blood-pressure control with conventional drugs has not succeeded in reducing cardiovascular disease risks to levels seen in normotensive persons. Drugs that inhibit or antagonize components of the renin–angiotensin–aldosterone system are addressing this deficiency by targeting both blood pressure and related structural and functional abnormalities of the heart and blood vessels, thus preventing target-organ damage and related cardiovascular events.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout





Similar content being viewed by others
References
Geneva World Health Organization. The World Health Report 2001. Mental health: New Understanding, New Hope [online], (cited 3 June 2002), 〈http://www.who.int/whr/2001/main/en/index.htm〉 (2001).
Mosterd, A. et al. Trends in the prevalence of hypertension, antihypertension therapy, and left ventricular hypertrophy from 1950 to 1999. N. Engl. J. Med. 340, 1221–1227 (1999).
Havlik, R. J. et al. Antihypertensive drug therapy and survival by treatment status in a national survey. Hypertension 13, I-28–I-32 (1989).
Lonn, E. M. et al. Emerging role of angiotensin-converting enzyme inhibitors in cardiac and vascular protection. Circulation 90, 2056–2069 (1994).
Burnier, M. & Brunner, H. R. Angiotensin II receptor antagonists. Lancet 355, 637–645 (2000).
Oparil, S. & Haber, E. The renin–angiotensin system. N. Engl. J. Med. 291, 389–401, 446–457 (1974).
Goodfriend, T. L., Elliot, M. E. & Catt, K. J. Angiotensin receptors and their antagonists N. Engl. J. Med. 334, 1649–1654 (1996).
Kerins, D. M., Haq, Q. & Vaughan, D. E. Angiotensin induction of PAI-1 expression in endothelial cells is mediated by the hexapeptide angiotensin IV. J. Clin. Invest. 96, 2515–2520 (1995).
Cesari, M., Rossi, G. P. & Pessina, A. C. Biological properties of the angiotensin peptides other than angiotensin II: implications for hypertension and cardiovscular disease. J. Hypertens. 20, 793–799 (2002).
Bergma, D. J. et al. Cloning and characterization of a human angiotensin II type 1 receptor. Biochem. Biophys. Res. Commun. 183, 989–995 (1992).
Mukoyama, M. et al. Expression cloning of type 2 angiotensin II receptor reveals a unique class of seven-transmembrane receptors. J. Biol. Chem. 68, 24539–24542 (1993).
de Gasparo, M. et al. The angiotensin receptors. Pharmacol. Rev. 52, 415–472 (2000).
Albiston, A. L. et al. Evidence that the angiotensin IV (AT(4)) receptor is the enzyme insulin-regulated aminopeptidase. J. Biol. Chem. 276, 48623–48626 (2001).
Fernandez, L. et al. AT2 receptor stimulation increases survival in gerbils with abrupt unilateral carotid ligation. J. Cardiovasc. Pharmacol. 24, 937–940 (1994).
Achard, J. M. et al. Protection against ischemia: a physiological function of the renin angiotensin system. Biochem. Pharmacol. 62, 261–272 (2001).
Makino, I. et al. Transient upregulation of the AT2 receptor mRNA level after global ischemia in the rat brain. Neuropeptides 30, 596–601 (1996).
Blume, A. et al. AT2 receptor inhibition in the rat brain reverses the beneficial effects of AT1 receptor blockade on neurological outcome after focal brain ischemia. Hypertension 36, 656 (2000).
Unger, T. The angiotensin II type 2 receptor: variations on an enigmatic theme. J. Hypertens. 17, 1775–1786 (1999).
Levy, B. I. et al. Chronic blockade of AT2 subtype receptors prevents the effect of angiotensin II on the rat vascular structure. J. Clin. Invest. 98, 418–425 (1996).
Henrion, D., Kubis, N. & Levy, B. Physiological and patho-physiological functions of the AT2 subtype receptor of angiotensin II from large arteries to the microcirculation. Hypertension 38, 1150–1157 (2001).
Griendling, K. K. et al. Angiotensin II stimulates NADH and NADPH oxidase in cultured vascular smooth muscle cells. Circ. Res. 74, 1141–1148 (1994).
Huraux, C. et al. Superoxide production, risk factors, and endothelium-dependent relaxations in human internal mammary arteries. Circulation 99, 53–59 (1999).
Vaughan, D. E., Lazos, S. A. & Tong, K. Angiotensin II regulates the expression of plasminogen activator inhibitor-1 in cultured endothelial cells. J. Clin. Invest. 95, 995–1001 (1995).
Ricker, P. M. et al. Stimulation of plasminogen activator inhibitor in vivo by infusion of angiotensin II. Circulation 87, 1969–1973 (1993).
Brown, N. J., Agirbasli, M. A., Williams, G. H., Litchfield, W. R. & Vaughan, D. E. Effect of activation and inhibition of the renin–angiotensin system on plasma PAI-1. Hypertension 32, 965–971 (1998).
The Heart Outcomes Prevention Evaluation Study Investigators. Effects of an angiotensin-converting-enzyme inhibitor, ramipril, on death from cardiovascular causes, myocardial infarction, and stroke in high-risk patients. N. Engl. J. Med. 342, 145–153 (2000).HOPE is the landmark trial that showed for the first time that ACE-inhibitor treatment can prevent CVD events in both hypertensive and non-hypertensive patients with established CVD. This was the first demonstration that ACE-inhibitor treatment has beneficial effects on vascular disease above and beyond blood-pressure lowering and prevention of heart failure.
Brunner, H. R. et al. Essential hypertension: renin and aldosterone, heart attack and stroke. N. Engl. J. Med. 286, 441–449 (1972).This study, highly controversial at the time of its publication, showed that plasma renin activity was inversely related to risk of heart attack and stroke independent of other risk factors in hypertensive patients. These findings provided a basis for the hypothesis that drugs that interrupt the RAAS might have vasoprotective effects beyond blood-pressure lowering.
Alderman, M. et al. Association of the renin–sodium-profile with the risk of myocardial infarction in patients with hypertension. N. Engl. J. Med. 324, 1098–1104 (1991).
Linz, W., Scholkens, B. A. & Ganten, D. Converting enzyme inhibition specifically prevents the development and induces regression of cardiac hypertrophy in rats. Clin. Exp. Hypertens. A 11, 1325–1350 (1989).
Lindpaintner, K. et al. Cardiac angiotensinogen and its local activation in the isolated perfused beating heart. Circ. Res. 67, 564–573 (1990).
Baker, R. R. et al. Endogenous xanthine oxidase-derived O2 metabolites inhibit surfactant. Am. J. Physiol. 259, H324–H332 (1990).
Dzau, V. J., Ellison, K. E., Brody, T., Ingelfinger, J. & Pratt, R. E. A comparative study of the distributions of renin and angiotensinogen messenger ribonucleic acids in rat and mouse tissue. Endocrinology 120, 2334–2338 (1987).
Pescott, G., Silversides, D. W., Chiu, S. M. & Reudelhuber, T. L. Contribution of circulating renin to local synthesis of angiotensin peptides in the heart. Physiol. Genomics 4, 67–73 (2000).
Dzau, V. J. Local expression and pathophysiological role of renin–angiotensin in the blood vessels and heart. Basic Res. Cardiol. 88, 2–14 (1993).
Husain, A. The chymase–angiotensin system in humans. J. Hypertens. 11, 1155–1159 (1993).
Chandrasekharan, U. M., Sanker, S., Glynias, M. J., Karnik, S. S. & Husain, A. Angiotensin II-forming activity in a reconstructed ancestral chymase. Science 271, 502–505 (1996).
Balcells, E., Meng, Q. C., Johnson, W. C., Oparil, S. & Dell'Italia, L. J. Angiotensin II formation from ACE and chymase in human and animal hearts: methods and species considerations. Am. J. Physiol. 273, H1769–H1774 (1997).
Wolny, A. et al. Functional and biochemical analysis of angiotensin II-forming pathways in the human heart. Circ. Res. 80, 219–227 (1997).
Dell'Italia, L. J. et al. Compartmentalization of angiotensin II generation in the dog heart: evidence for independent mechanisms in intravascular and interstitial spaces. J. Clin. Invest. 100, 253–258 (1997).
Funder, J. W. Mineralocorticoid receptors and hypertension. J. Steroid Biochem. Mol. Biol. 53, 53–55 (1995).
Slight, S. H. et al. Extra-adrenal mineralocorticoids and cardiovascular tissue. J. Mol. Cell Cardiol. 31, 1175–1184 (1999).
Brilla, C. G. & Weber, K. T. Mineralocorticoid excess, dietary medium and myocardial fibrosis. J. Lab. Clin. Med. 120, 893–901 (1992).
Delcayre, C. et al. Cardiac aldosterone production and ventricular remodeling. Kidney Intl 57, 1346–1351 (2000).
Skeggs, L. T., Kahn, J. R., Lentz, K. & Shumway, N. P. Preparation, purification, and amino acid sequence of a polypeptide renin substrate. J. Exp. Med. 106, 439–453 (1957).
Wood, J. M., Stanton, J. L. & Hofbauer, K. G. Inhibitors of renin as potential therapeutic agents J. Enzyme Inhibit. 1, 169–185 (1987).
Stanton, A. et al. Dose response antihypertensive efficacy of aliskiren (SPP100), an orally active renin inhibitor. Am. J. Hypertens. 15 (Suppl. 1), A56–A57 (2002).
Ferreira, S. H. A bradykinin-potentiating factor (BPF) present in the venom of Bothrops jararaca. Br. J. Pharmacol. Chemother. 24, 163 (1965).This fascinating combination of rigorous science and serendipity showed that peptides present in snake venom can inhibit kininase II (ACE), reducing blood pressure in animal models. The orally active ACE inhibitors were ultimately synthesized on the basis of this information.
Ondetti, M. A., Rubin, B. & Cushman, D. W. Design of specific inhibitors of angiotensin converting enzyme: new class of orally acting active antihypertensive agents. Science 196, 441–444 (1977).
Garg, R. & Yusuf, S. for the Collaborative Group on ACE-Inhibitor Trials. Overview of randomized trials of angiotensin-converting enzyme inhibitors on mortality and morbidity in patients with heart failure. JAMA 273, 1450–1456 (1995).
Schmeider, R. E., Martus, P. & Klingbeil, A. Reversal of left ventricular hypertrophy in essential hypertension: a meta-analysis of randomized double-blind studies. JAMA 275, 1507–1513 (1996).
Pfeffer, et al. Effect of captropil on progressive ventricular dilatation after anterior myocardial infarction. N. Engl. J. Med. 319, 80–86 (1988).
Williams, G. H. Converting-enzyme inhibitors in the treatment of hypertension. N. Engl. J. Med. 319, 1517–1525 (1988).
Giatras, I., Lau, J. & Levey, A. S. for the Angiotensin-converting Enzyme Inhibition and Progressive Renal Disease Study Group. Effect of angiotensin-converting enzyme inhibitors on the progression of nondiabetic renal disease: a meta-analysis of randomized trials. Ann. Intern. Med. 127, 337–345 (1997).
Jafar, T. et al. Angiotensin-converting enzyme inhibitors and progression of nondiabetic renal disease: a meta-analysis of patient-level data. Ann. Intern. Med. 135, 73–87 (2001).This meta-analysis tested whether antihypertensive regimens that include an ACE inhibitor are superior to other regimens in slowing the progression of renal disease in non-diabetic patients with renal dysfunction. Large benefits that did not seem to depend on reduction in blood pressure or urinary protein excretion were seen in patients with baseline proteinuria, leading to a treatment indication for ACE inhibitors in patients with non-diabetic chronic renal disease and proteinuria.
Ravid, M., Lang, R., Rachmani, R. & Lishner, M. Long-term renoprotective effect of angiotensin-converting enzyme inhibition on non-insulin dependent diabetes mellitus: a 7-year follow-up study. Arch. Int. Med. 156, 286–289 (1996).
Lewis, E. J., Hunsicker, L. G., Bain, R. P. & Rhode, R. D. for the Collaborative Study Group. The effect of angiotensin-converting enzyme inhibition on diabetic nephropathy. N. Engl. J. Med. 329, 1456–1462 (1993).This was the first study to show that ACE-inhibitor treatment is effective in slowing the progression of renal disease in diabetic (insulin-dependent) patients with proteinuria. The contribution of blood-pressure reduction to this effect is still debated.
Sica, D. A. & Gehr, T. W. B. in Hypertension: A Companion to Brenner and Rector's The Kidney (eds Oparil, S. & Weber, M. A.) 599–609 (W. B. Saunders Co., Philadelphia, 2000).
Clement, D. L. in Manual of Hypertension (eds Mancia, G. et al.) 359–373 (Harcourt, London, 2002)
Brunner, H. R., Waeber, B. & Nussberger, J. in Cardiovascular Drug Therapy 2nd edn (ed. Messerli, F.) 690–711 (W. B. Saunders Co., Philadelphia, 1996).
Ruddy, M. C., Kostis, J. B. & Frishman, W. H. in Cardiovascular Pharmotherapeutics (eds Frishman, W. H. & Sonnenblick, E. H.) 131–192 (McGraw–Hill, New York, 1996).
Leonetti, G. & Cusipidi, C. Choosing the right ACE inhibitors: a guide to selection. Drugs 49, 516–535 (1995).
Biollaz, J., Brunner, H. R., Gavras, I., Waeber, B. & Gavras, H. Antihypertensive therapy with MK421: angiotensin II–renin relationships to evaluate efficiency of converting enzyme blockade. J. Cardiovasc. Pharmacol. 44, 966–972 (1982).
King, S. J. & Oparil, S. Converting enzyme (CE) inhibitors increase CE mRNA and activity in endothelial cells. Am. J. Physiol. Cell Physiol. 263, C743–C749 (1992).
Brown, N. J., Gainer, J. V., Stein, C. M. & Vaughan, D. E. Bradykinin stimulates tissue plasminogen activator release in human vasculature. Hypertension 33, 1431–1435 (1999).
Bouaziz, H., Joulin, Y., Safar, M. & Benetos, A. Effects of bradykinin B2 receptor antagonism on the hypotensive effects of ACE inhibition. Br. J. Pharmacol. 113, 717–722 (1994).
Barbe, F. et al. Bradykinin pathway is involved in acute hemodynamic effects of enalaprilat in dogs with heart failure. Am. J. Physiol. 270, H1985–H1992 (1996).
Linz, W. & Scholkens, B. A. Specific B2-bradykinin receptor antagonist HOE 140 abolishes the anithypertrophic effect of ramipril. Br. J. Pharmacol. 105, 771–772 (1992).
Hornig, B., Kohler, C. & Drexler, H. Role of bradykinin in mediating vascular effects of angiotensin-converting enzyme inhibitors in humans. Circulation 95, 1115–1118 (1997).
Gainer, J. V., Morrow, J. D., Loveland, A., King, D. & Brown, N. J. Effect of bradykinin receptor blockade on the response to angiotensin-converting-enzyme inhibitor in normotensive and hypertensive subjects. N. Engl. J. Med. 339, 1285–1292 (1998).
Blood Pressure Lowering Treatment Trialists' Collaboration. Effects of ACE inhibitors, calcium antagonists, and other blood-pressure-lowering drugs: results of prospectively designed overviews of randomized trials. Lancet 356, 1955–1964 (2000).
Hansson, L. et al. Effects of angiotensin-converting-enzyme inhibition compared with conventional therapy on cardiovascular morbidity and mortality in hypertension: The Captopril Prevention Project (CAPPP) randomized trial. Lancet 353, 611–616 (1999).
Hansson, L. et al. Randomized trial of old and new antihypertensive drugs in elderly patients: cardiovascular mortality and morbidity the Swedish Trial in Old Patients with Hypertension-2 Study. Lancet 354, 1751–1756 (1999).
PROGRESS Collaborative Group. Randomised trial of a perindopril-based blood pressure-lowering regimen among 6105 individuals with previous stroke or transient ischemic attack. Lancet 358, 1033–1041 (2001).
PATS Collaborating Group. Post-stroke antihypertensive treatment study: a preliminary result. Chin. Med. J. 108, 710–717 (1995).
Davis, B. R. et al. Rationale and design for the antihypertensive and lipid lowering treatment to prevent heart attack trial (ALLHAT). Am. J. Hypertens. 9, 342–360 (1996).
Agadoa, L. Y. et al. Effect of ramipril vs amlodipine on renal outcomes in hypertensive nephrosclerosis: a randomized controlled trial. JAMA 285, 2719–2728 (2001).
CONSENSUS Trial Study Group. Effects of enalapril on mortality in severe congestive heart failure. Results of the Cooperative North Scandanavian Enalapril survival Study (CONSENSUS). N. Engl. J. Med. 316, 1429–1435 (1987).
The SOLVD Investigators. Effects of enalapril on survival in patients with reduced left ventricular ejection fractions and congestive heart failure. N. Engl. J. Med. 325, 293–302 (1991).
The SOLVD Investigators. Effect of enalapril on mortality and the development of heart failure in asymptomatic patients with reduced left ventricular ejection fractions. N. Engl. J. Med. 327, 685–691 (1992).
Cohn, J. N. et al. A comparison of enalapril with hydralazine-isosorbide dinitrate in the treatment of chronic congestive heart failure. N. Engl. J. Med. 325, 303–310 (1991).
ACE Inhibitor Myocardial Infarction Collaborative Group. Indications for ACE inhibitors in the early treatment of acute myocardial infarction. Systematic overview of individual data from 100,000 patients in randomized trials. Circulation 97, 2202–2212 (1998).
The sixth report of the Joint National Committee on prevention, detection, evaluation, and treatment of high blood pressure. Arch. Intern. Med. 157, 2413–2446 (1997).
Bakris, G. L. et al. Preserving renal function in adults with hypertension and diabetes: a consensus approach. National Kidney Foundation Hypertension and Diabetes Executive Committees Working Group. Am. J. Kidney Dis. 36, 646–661 (2000).
Koike, H., Sada, T. & Mizuno, M. In vitro and in vivo pharmacology of olmesartan medoxomil, an angiotensin II type AT1 receptor antagonist. J. Hypertens. (Suppl 1) 19, S3–S14 (2001).
Reif, M. et al. Effects of candesartan cilexetil in patients with systemic hypertension. Am. J. Cardiol. 82, 961–965 (1998).
Oparil, et al. An elective-titration study of the comparative effectiveness of two angiotensin II receptor blockers irbesartan and losartan. Clin. Ther. 20, 398–409 (1998).
Mallion, J. M., Siche, J. P. & Lacouriere, Y. ABPM comparison of the antihypertensive profiles of the selective angiotensin II receptor antagonists telmisartan and losartan in patients with mild-to-moderate hypertension. J. Hum. Hypertens. 13, 657–664 (1999).
Anderson, O. K. & Neldman, S. The antihypertensive effect and tolerability of candesartan cilexetil, a new generation angiotensin II antagonist, in comparison with losartan. Blood Pressure 7, 53–59 (1998).
Oparil, S., Williams, D., Chrysant, S. G., Marbury, T. C. & Neutel, J. Comparative efficacy of olmesartan, losartan, valsartan, and irbesartan in the control of essential hypertension. J. Clin. Hypertens. 3, 283–291 (2001).
Conlin, P. R. et al. Angiotensin II antagonists for hypertension: are there differences in efficacy? Am. J. Hypertens. 13, 418–426 (2000).
Chiu, A. G., Krowiak, E. J. & Deeb, Z. E. Angioedema associated with angiotensin II receptor antagonists: challenging our knowledge of angioedema and its etiology. Laryngoscope 111, 1729–1731 (2001).
Nakashima, M., Uematsu, T., Kosuge, K. & Kanamaru, M. Pilot study of the uricosuric effect of DuP-753, a new angiotensin II receptor antagonist, in healthy subjects. Eur. J. Clin. Pharmacol. 42, 333–335 (1992).
Dahlöf, B. et al. Cardiovascular morbidity and mortality in the Losartan Intervention For Endpoint reduction in hypertension study (LIFE): a randomized trial against atenolol. Lancet 359, 995–1003 (2002).LIFE is the first randomized, controlled outcome trial to show that any particular antihypertensive drug (or drug class) confers benefits beyond blood-pressure reduction and is more effective than any other class in preventing CVD events and mortality. ARB-based treatment resulted in 25% greater reductions in stroke and new-onset diabetes compared with treatment based on beta-blockers in high-risk patients with left ventricular hypertrophy by ECG.
Lindholm, L. H. et al. Cardiovascular morbidity and mortality in patients with diabetes in the Losartan Intervention For Endpoint reduction in hypertension study (LIFE): a randomized trial against atenolol. Lancet 359, 1004–1010 (2002).A prespecified analysis of outcomes in the more than 1,100-patient diabetic subgroup in LIFE showed a 39% reduction in total mortality and a 37% reduction in CVD mortality with ARB treatment compared to beta-blocker treatment. LIFE is the only study to show that ARB treatment of hypertensive diabetic patients has survival benefits beyond blood-pressure lowering.
Brenner, B. M. et al. Effects of losartan on renal and cardiovascular outcomes in patients with type 2 diabetes and nephropathy. N. Engl. J. Med. 345, 861–869 (2001).RENAAL showed that, compared with placebo (usual care), treatment with the ARB losartan slowed the progression of renal disease, reduced proteinuria and led to other clinical benefits in normotensive or hypertensive patients with type 2 diabetes. The favourable renal effects of the ARB seemed to be, at least in part, independent of blood pressure.
Lewis, E. J. et al. Renoprotective effect of the angiotensin-receptor antagonist irbesartan in patients with nephropathy due to type 2 diabetes. N. Engl. J. Med. 345, 851–860 (2001).IDNT clearly showed a slowing of the progression of renal disease with the ARB irbesartan compared with amlodipine or placebo (usual care) in patients with type 2 diabetes, nephropathy and renal dysfunction, despite equivalent blood-pressure reductions with amlodipine. The irbesartan effect was dose dependent.
Parving, H. H. et al. The effect of irbesartan on the development of diabetic nephropathy in patients with type 2 diabetes. N. Engl. J. Med. 345, 870–878 (2001).
Wheeldon, N. M. & Viberti, G. C. Microalbuminuria reduction with valsartan. Am. J. Hypertens. 14, Abstract 0–6 (2001).
Pitt, B. et al. on behalf of the ELITE Study Investigators. Randomised trial of Losartan versus captopril in patients over 65 with heart failure. Lancet 349, 747–752 (1997).
McKelvie, R. S. et al. Comparison of candesartan, enalapril, and their combination in congestive heart failure: Randomised Evaluation of Strategies for Left Ventricular Dysfunction (RESOLVD) pilot study. Circulation 100, 1056–1064 (1999).
Pitt, B. et al. Effect of losartan compared with captopril on mortality in patients with symptomatic heart failure: randomised trial – the Losartan Heart Failure Survival Study ELITE II. Lancet 355, 1582–1587 (2000).
Cohn, J. N. & Tognoni, G. for the Val-HeFT Investigators. A randomized trial of the angiotensin-receptor blocker valsartan in chronic heart failure. N. Engl. J. Med. 345, 1667–1675 (2001).
Zannad, F. et al. Limitation of excessive extracellular matrix turnover may contribute to survival benefit of spironolactone therapy in patients with congestive heart failure: insight from Randomized Aldactone Evaluation Study (RALES). Circulation 102, 2700–2706 (2000).
Jeunemaitre, X. et al. Efficacy and tolerance of spironolactone in essential hypertension. Am. J. Cardiol. 60, 820–825 (1987).
Pitt, B. et al. The effect of spironolactone on morbidity and mortality in patients with severe heart failure. N. Engl. J. Med. 341, 709–717 (1999).RALES showed that aldosterone receptor blockade with spironolactone, along with conventional therapy, significantly reduces the risk of morbidity and mortality in patients with severe heart failure. This is the first demonstration that aldosterone antagonists have CVD benefits beyond blood-pressure lowering.
Calhoun, D. A., Zaman, M. A. & Nishizaka, M. K. Resistant hypertension. Curr. Hypertens. Rep. 4, 221–228 (2002).
Ouzan, J. et al. The role of spironolactone in the treatment of patients with refractory hypertension. Am. J. Hypertens. 15, 333–339 (2002).
Burgess, E. et al. The selective aldosterone blocker eplerenone is safe and efficacious for the treatment of long-term treatment of mild to moderate hypertension. Am. J. Hypertens. 15 (Suppl. 1), A57–A58 (2002).
Weber, M. A. Vasopeptidase inhibitors. Lancet 358, 1525–1532 (2001).
de Gasparo, M. et al. Proposed update of angiotensin receptor nomenclature. Hypertension 25, 924–927 (1995).
Bauer, J. H. & Reams, G. P. The angiotensin II type I receptor antagonists — a new class of antihypertensive drugs. Arch. Intern. Med. 155, 1361–1368 (1995).
Eberhardt, R. T., Kevak, R. M., Kang, P. M. & Frishman, W. H. Angiotensin II receptor blockade: an innovative approach to cardiovascular pharmacotherapy. J. Clin. Pharmacol. 33, 1023–1038 (1993).
Foote, E. F. & Halstenson, C. E. New therapeutic agents in the management of hypertension: angiotension II-receptor antagonists and renin inhibitors. Ann. Pharmacother. 27, 1495–1503 (1993).
Corti, R. et al. Vasopeptidase inhibitors: a new therapeutic concept in cardiovascular diseases. Circulation. 104, 1856–1862 (2001).
Brunner, H. R. The new oral angiotensin II antagonist Olmesartan: a concise overview. J. Hum. Hypertens. 169 (Suppl. 2), S13–S16 (2002).
Ruddy, M. C & Kostis, J. B. in Hypertension: A Companion to Brenner and Rector's The Kidney (eds Oparil, S. & Weber, M. A.) 621–637 (W. B. Saunders Co., Philadelphia, 2000).
Author information
Authors and Affiliations
Corresponding author
Related links
Related links
DATABASES
OMIM
Locuslink
Medscape DrugInfo
FURTHER INFORMATION
Glossary
- MYOCARDIAL INFARCTION
-
Commonly known as a heart attack, this is the death of part of the heart muscle owing to a sudden loss of blood supply.
- HYPERTROPHY
-
An increase in the size of a tissue or organ resulting from an increase in the size of the cells present.
- HYPERPLASIA
-
An increase in the size of a tissue or organ resulting from an increase in the total number of cells present.
- ATHEROSCLEROSIS
-
A degenerative condition that is characterized by a narrowing of the arteries, owing to deposits of fatty substances, cholesterol, cellular waste products, calcium and other substances in the arterial inner lining.
- MINERALOCORTICOID
-
A corticosteroid that acts primarily on water and electrolyte balance by promoting the renal retention of sodium ions and excretion of potassium ions. Aldosterone is the most potent of the naturally occuring mineralocorticoids.
- FIBROSIS
-
The production of fibrous connective tissue as a consequence of chronic inflammation or healing.
- PROTEINURIA
-
The presence of protein in urine.
- ANGIOEDEMA
-
The development of tissue swelling, most commonly around the eyes and lips, which can lead to airway obstruction in rare cases.
- PRESSOR RESPONSE
-
An increase in blood pressure due to angiotensin II-induced activation of AT1 receptors.
- HYPERKALAEMIA
-
The presence in the blood of an abnormally high concentration of potassium.
- URICOSURIC ACTION
-
A tendency to promote urinary excretion of uric acid.
Rights and permissions
About this article
Cite this article
Zaman, M., Oparil, S. & Calhoun, D. Drugs targeting the renin–angiotensin–aldosterone system. Nat Rev Drug Discov 1, 621–636 (2002). https://doi.org/10.1038/nrd873
Issue Date:
DOI: https://doi.org/10.1038/nrd873
This article is cited by
-
Advances in the allostery of angiotensin II type 1 receptor
Cell & Bioscience (2023)
-
Candesartan, an angiotensin-II receptor blocker, ameliorates insulin resistance and hepatosteatosis by reducing intracellular calcium overload and lipid accumulation
Experimental & Molecular Medicine (2023)
-
Network analysis of atherosclerotic genes elucidates druggable targets
BMC Medical Genomics (2022)
-
ATR1 Angiotensin II Receptor Reduces Hemoglobin S Polymerization, Phosphatidylserine Exposure, and Increases Deformability of Sickle Cell Disease Erythrocytes
Cell Biochemistry and Biophysics (2022)
-
A Complex Approach to the Determination of Authenticity in the Development of Standard Samples for Ace Inhibitors
Pharmaceutical Chemistry Journal (2022)