Abstract
In boys, the hormonal changes that accompany normal puberty are well defined, as are the physical signs of pubertal development and the kinetics of the growth spurt. Most androgens are derived from the testes, although adrenal androgens may also contribute; testosterone can also be aromatized to estrogen to exert important effects during puberty. Androgens, but especially their conversion to estrogens by aromatase, have a major role in the dramatic changes in linear growth, secondary sexual characteristics, and changes to bone, muscle and fat distribution that occur during puberty. Androgen therapy for delayed puberty should permit full normal pubertal development and thereby also address some of the associated psychosocial problems. Adolescent boys with conditions of permanent hypogonadism (hypogonadotropic or hypergonadotropic) or transient hypogonadotropic hypogonadism (constitutional delay of growth and puberty) can benefit from testosterone therapy. Long-term testosterone therapy should be given for hypothalamic or pituitary gonadotropin deficiency, or for primary hypogonadism such as for adolescents with Klinefelter syndrome, if endogenous testosterone levels drop or levels of luteinizing hormone rise. Intramuscular administration every few weeks is effective, but newer cutaneous forms, for example, gels or patches, also show promise in permitting adolescent males to reach adult body composition.
Key Points
-
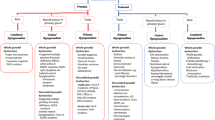
Constitutional delay of growth and puberty (CDGP) is a common form of (transiently) delayed pubertal development in males
-
Testosterone therapy increases growth and leads to lean body mass accrual in boys with primary or secondary hypogonadism
-
Adolescent males with CDGP benefit from short-term administration of testosterone
-
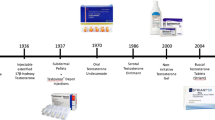
Long acting testosterone esters are the primary form of androgen replacement therapy in adolescents, but newer cutaneous forms are beginning to be used in this group
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
References
Herman-Giddens ME et al. (1997) Secondary sexual characteristics and menses in young girls seen in office practice: a study from the Pediatric Research in Office Settings network. Pediatrics 99: 505–512
Kaplowitz PB and Oberfield SE (1999) Reexamination of the age limit for defining when puberty is precocious in girls in the United States: implications for evaluation and treatment. Drug and Therapeutics and Executive Committees of the Lawson Wilkins Pediatric Endocrine Society. Pediatrics 104: 936–941
Sonis WA et al. (1985) Behavior problems and social competence in girls with true precocious puberty. J Pediatr 106: 156–160
Biro FM et al. (1995) Pubertal staging in boys. J Pediatr 127: 100–102
Tanner JM (1962) Growth at Adolescence. Springfield: Charles C Thomas
Zachmann M et al. (1974) Testicular volume during adolescence: cross-sectional and longitudinal studies. Helv Paediatr Acta 29: 61–72
Sutherland RS et al. (1996) The effect of prepubertal androgen exposure on adult penile length. J Urol 156: 783–787
Karlberg P and Taranger J (1976) The somatic development of children in a Swedish urban community. Acta Paediatr Scand Suppl 258: 1–48
Tanner JM et al. (1976) The adolescent growth spurt of boys and girls of the Harpenden growth study. Ann Hum Biol 3: 109–126
Largo RH et al. (1978) Analysis of the adolescent growth spurt using smoothing spline functions. Ann Hum Biol 5: 421–434
Abbassi V (1998) Growth and normal puberty. Pediatrics 102: 507–511
Greulich WS and Pyle SI (1959) Radiograph Atlas of Skeletal Development of the Hand and Wrist. Stanford: Stanford University Press
Veldhuis JD et al. (2005) Endocrine control of body composition in infancy, childhood, and puberty. Endocr Rev 26: 114–146
Bonjour JP et al. (1994) Peak bone mass. Osteoporos Int 4 (Suppl 1): 7–13
Delemarre-Van De Waal HA et al. (1991) Gonadotrophin and growth hormone secretion throughout puberty. Acta Paediatr Scand Suppl 372: 26–31
Knobil E (1980) The neuroendocrine control of the menstrual cycle. Recent Prog Horm Res 36: 53–88
Albertsson-Wikland K et al. (1997) Twenty-four-hour profiles of luteinizing hormone, follicle-stimulating hormone, testosterone, and estradiol levels: a semi-longitudinal study throughout puberty in healthy boys. J Clin Endocrinol Metab 82: 541–549
Boyar RM et al. (1974) Human puberty. Simultaneous augmented secretion of luteinizing hormone and testosterone during sleep. J Clin Invest 54: 609–618
August GP et al. (1972) Hormonal changes in puberty. 3. Correlation of plasma testosterone, LH, FSH, testicular size, and bone age with male pubertal development. J Clin Endocrinol Metab 34: 319–326
Knorr D et al. (1974) Plasma testosterone in male puberty. I. Physiology of plasma testosterone. Acta Endocrinol (Copenh) 75: 181–194
Weinstein RL et al. (1974) Secretion of unconjugated androgens and estrogens by the normal and abnormal human testis before and after human chorionic gonadotropin. J Clin Invest 53: 1–6
Mauras N et al. (2000) Insulin-like growth factor I and growth hormone (GH) treatment in GH-deficient humans: differential effects on protein, glucose, lipid, and calcium metabolism. J Clin Endocrinol Metab 85: 1686–1694
Klein KO et al. (1996) A longitudinal assessment of hormonal and physical alterations during normal puberty in boys. II. Estrogen levels as determined by an ultrasensitive bioassay. J Clin Endocrinol Metab 81: 3203–3207
Sklar CA et al. (1980) Evidence for dissociation between adrenarche and gonadarche: studies in patients with idiopathic precocious puberty, gonadal dysgenesis, isolated gonadotropin deficiency, and constitutionally delayed growth and adolescence. J Clin Endocrinol Metab 51: 548–556
Veldhuis JD et al. (2000) Gender and sexual maturation-dependent contrasts in the neuroregulation of growth hormone secretion in prepubertal and late adolescent males and females—a general clinical research center-based study. J Clin Endocrinol Metab 85: 2385–2394
Metzger DL and Kerrigan JR (1994) Estrogen receptor blockade with tamoxifen diminishes growth hormone secretion in boys: evidence for a stimulatory role of endogenous estrogens during male adolescence. J Clin Endocrinol Metab 79: 513–518
Keenan BS et al. (1993) Androgen-stimulated pubertal growth: the effects of testosterone and dihydrotestosterone on growth hormone and insulin-like growth factor-I in the treatment of short stature and delayed puberty. J Clin Endocrinol Metab 76: 996–1001
Houchin LD and Rogol AD (1998) Androgen replacement in children with constitutional delay of puberty: the case for aggressive therapy. Baillieres Clin Endocrinol Metab 12: 427–440
Sanayama K et al. (1987) Spontaneous growth hormone secretion and plasma somatomedin-C in children of short stature. Endocrinol Jpn 34: 627–633
Kerrigan JR et al. (1990) Variations of pulsatile growth hormone release in healthy short prepubertal boys. Pediatr Res 28: 11–14
Crowne EC et al. (1990) Final height in boys with untreated constitutional delay in growth and puberty. Arch Dis Child 65: 1109–1112
LaFranchi S et al. (1991) Constitutional delay of growth: expected versus final adult height. Pediatrics 87: 82–87
Albanese A and Stanhope R (1995) Predictive factors in the determination of final height in boys with constitutional delay of growth and puberty. J Pediatr 126: 545–550
Bertelloni S et al. (1995) Short-term effect of testosterone treatment on reduced bone density in boys with constitutional delay of puberty. J Bone Miner Res 10: 1488–1495
Schoenau E et al (2004) From bone biology to bone analysis. Horm Res 61: 257–269
Bourguignon JP (1988) Linear growth as a function of age at onset of puberty and sex steroid dosage: therapeutic implications. Endocr Rev 9: 467–48855
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
EJ Richmond declared he has no competing interests. A Rogol is a consultant to Solvay Pharmaceuticals, Inc., the manufacturer of Androgel®.
Rights and permissions
About this article
Cite this article
Richmond, E., Rogol, A. Male pubertal development and the role of androgen therapy. Nat Rev Endocrinol 3, 338–344 (2007). https://doi.org/10.1038/ncpendmet0450
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1038/ncpendmet0450
This article is cited by
-
Neonatal gonadotropin therapy in male congenital hypogonadotropic hypogonadism
Nature Reviews Endocrinology (2012)
-
Vorzeitiger, verspäteter und ausbleibender Pubertätsbeginn
Monatsschrift Kinderheilkunde (2012)
-
The role of homeodomain transcription factors in heritable pituitary disease
Nature Reviews Endocrinology (2011)
-
Leydig cell transplantation restores androgen production in surgically castrated prepubertal rats
Asian Journal of Andrology (2009)
-
Testosterone treatment in elderly men
Advances in Therapy (2009)