Abstract
Objective:
To determine which neuroimaging, clinical and sociodemographic factors predict neurodevelopment at 18–22 months age among extremely preterm infants with intraparenchymal hemorrhage (IPH).
Study Design:
Cranial ultrasounds performed before 42 days of age and cranial ultrasounds/magnetic resonance images of the brain performed near discharge were reviewed for hemorrhage location and other abnormalities. Clinical and sociodemographic factors were extracted from existing databases. The primary outcome was presence of cerebral palsy (CP) and the secondary outcome was cognitive development (Bayley Scales of Infant Development).
Result:
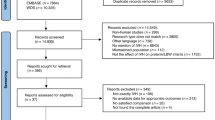
Of 1168 infants (<1000 g or <27 weeks), 141 infants had an IPH and 48 infants were seen in follow-up. All infants with extensive hemorrhages (involving three or more lobes) developed CP. In early imaging (before 42 days of age), ventriculomegaly, intraventricular hemorrhage (IVH) and extensive hemorrhage were predictors of CP. In imaging performed near discharge, ventriculomegaly, intraventricular echodensity and having a ventricular shunt were predictors of CP. Clinical, imaging and sociodemographic factors were not associated with low cognitive score.
Conclusion:
In preterm infants surviving with IPH, extensive hemorrhage, ventriculomegaly, IVH and having a shunt increased the risk of developing CP.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Volpe JJ . Neurology of the Newborn 4th edn. W.B. Saunders Company, 2001.
Bassan H, Feldman HA, Limperopoulos C, Benson CB, Ringer SA, Veracruz E et al. Periventricular hemorrhagic infarction: risk factors and neonatal outcome. Pediatr Neurol 2006; 35 (2): 85–92.
Papile LA, Munsick-Bruno G, Schaefer A . Relationship of cerebral intraventricular hemorrhage and early childhood neurologic handicaps. J Pediatr 1983; 103 (2): 273–277.
Bassan H, Limperopoulos C, Visconti K, Mayer DL, Feldman HA, Avery L et al. Neurodevelopmental outcome in survivors of periventricular hemorrhagic infarction. Pediatrics 2007; 120 (4): 785–792.
Maitre NL, Marshall DD, Price WA, Slaughter JC, O'Shea TM, Maxfield C et al. Neurodevelopmental outcome of infants with unilateral or bilateral periventricular hemorrhagic infarction. Pediatrics 2009; 124 (6): e1153–e1160.
Roze E, Kerstjens JM, Maathuis CG, ter Horst HJ, Bos AF . Risk factors for adverse outcome in preterm infants with periventricular hemorrhagic infarction. Pediatrics 2008; 122 (1): e46–e52.
Brouwer A, Groenendaal F, van Haastert IL, Rademaker K, Hanlo P, de Vries L . Neurodevelopmental outcome of preterm infants with severe intraventricular hemorrhage and therapy for post-hemorrhagic ventricular dilatation. J Pediatr 2008; 152 (5): 648–654.
Vohr B, Garcia Coll C, Flanagan P, Oh W . Effects of intraventricular hemorrhage and socioeconomic status on perceptual, cognitive, and neurologic status of low birth weight infants at 5 years of age. J Pediatr 1992; 121 (2): 280–285.
Kuban KC, Allred EN, O'Shea TM, Paneth N, Pagano M, Dammann O et al. Cranial ultrasound lesions in the NICU predict cerebral palsy at age 2 years in children born at extremely low gestational age. J Child Neurol 2009; 24 (1): 63–72.
O'Shea TM, Kuban KC, Allred EN, Paneth N, Pagano M, Dammann O et al. Neonatal cranial ultrasound lesions and developmental delays at 2 years of age among extremely low gestational age children. Pediatrics 2008; 122 (3): e662–e669.
Ment LR, Vohr B, Allan W, Westerveld M, Katz KH, Schneider KC et al. The etiology and outcome of cerebral ventriculomegaly at term in very low birth weight preterm infants. Pediatrics 1999; 104 (2 Pt 1): 243–248.
Goldstein RF, Cotten CM, Shankaran S, Gantz MG, Poole WK . Eunice Kennedy Shriver National Institute of Child Health and Human Development Neonatal Research Network. Influence of gestational age on death and neurodevelopmental outcome in premature infants with severe intracranial hemorrhage. J Perinatol 2013; 33 (1): 25–32.
Roze E, Van Braeckel KN, van der Veere CN, Maathuis CG, Martijn A, Bos AF . Functional outcome at school age of preterm infants with periventricular hemorrhagic infarction. Pediatrics 2009; 123 (6): 1493–1500.
Merhar SL, Tabangin ME, Meinzen-Derr J, Schibler KR . Grade and laterality of intraventricular haemorrhage to predict 18-22 month neurodevelopmental outcomes in extremely low birthweight infants. Acta Paediatr 2012; 101 (4): 414–418.
Luu TM, Ment LR, Schneider KC, Katz KH, Allan WC, Vohr BR . Lasting effects of preterm birth and neonatal brain hemorrhage at 12 years of age. Pediatrics 2009; 123 (3): 1037–1044.
Acknowledgements
NICHD Neonatal Research Network (U10 HD21373): Jon E Tyson, MD MPH; Nora I Alaniz, BS; Beverly Foley Harris, RN BSN; Charles Green, PhD; Margarita Jiminez, MD MPH; Anna E Lis, RN BSN; Sarah Martin, RN BSN; Georgia E McDavid, RN; Brenda H Morris, MD; Margaret L Poundstone, RN BSN; Stacy Reddoch, BA; Saba Siddiki, MD; Patti L Pierce Tate, RCP; Laura L Whitely, MD; Sharon L Wright, MT (ASCP).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Tsai, A., Lasky, R., John, S. et al. Predictors of neurodevelopmental outcomes in preterm infants with intraparenchymal hemorrhage. J Perinatol 34, 399–404 (2014). https://doi.org/10.1038/jp.2014.21
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/jp.2014.21
Keywords
This article is cited by
-
Impact of quality improvement outreach education on the incidence of acute brain injury in transported neonates born premature
Journal of Perinatology (2022)
-
Preterm neuroimaging and neurodevelopmental outcome: a focus on intraventricular hemorrhage, post-hemorrhagic hydrocephalus, and associated brain injury
Journal of Perinatology (2018)
-
Severe intraventricular hemorrhage and withdrawal of support in preterm infants
Journal of Perinatology (2017)
-
Long-Term Neurodevelopmental and Growth Outcomes of Premature Infants Born at <29 week Gestational Age with Post-Hemorrhagic Hydrocephalus Treated with Ventriculo-Peritoneal Shunt
The Indian Journal of Pediatrics (2017)
-
Mental health assessed by the Strengths and Difficulties Questionnaire for children born extremely preterm without severe disabilities at 11 years of age: a Norwegian, national population-based study
European Child & Adolescent Psychiatry (2017)