Abstract
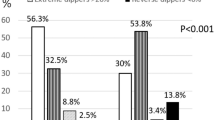
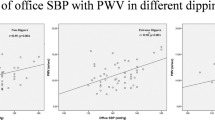
We investigated the effect of the diverse definition criteria of the dipping and non-dipping status on the assessed differences in inflammatory activation between dippers and non-dippers with essential hypertension. 269 consecutive subjects (188 males, aged 50±7 years) with untreated stage I–II essential hypertension underwent ambulatory blood pressure (BP) monitoring and high-sensitivity C-reactive protein (hs-CRP) level determination. The population was classified into dippers and non-dippers based on the three following different definitions: true non-dippers (TND): non-dippers (nocturnal fall of systolic and diastolic BP of <10% of the daytime values, n=95) and dippers (the remaining subjects, n=174); true dippers and true non-dippers (TD–TND): non-dippers (nocturnal fall of systolic and diastolic BP<10%, n=95) and dippers (nocturnal fall of systolic and diastolic BP⩾10%, n=75); systolic non-dippers (SND): non-dippers (nocturnal systolic BP fall of <10% of the daytime values, n=145) and dippers (the remaining subjects, n=124). Non-dippers compared to dippers in the TND, TD–TND and SND classification exhibited higher levels of log hs-CRP (by 0.11 mg l−1, P=0.02; 0.13 mg l−1, P=0.03 and 0.14 mg l−1, P=0.02, respectively) and 24 h pulse pressure (PP) (by 4 mm Hg, P=0.006; by 5 mm Hg, P=0.003 and by 5 mm Hg, P<0.0001, respectively). Twenty-four hour PP and nocturnal systolic BP fall were independent predictors of log hs-CRP (P<0.05 for both) in multiple regression analysis. In conclusion, essential hypertensive non-dippers compared to dippers exhibit higher hs-CRP values, irrespective of the dipping status definition. Furthermore, ambulatory PP and nocturnal systolic BP fall interrelate and participate in the inflammatory processes that accompany non-dipping state.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 digital issues and online access to articles
$119.00 per year
only $9.92 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Hackam DG, Anand SS . Emerging risk factors for atherosclerotic vascular disease: a critical review of the evidence. J Am Med Assoc 2003; 290: 932–940.
Ridker PM, Hennekens CH, Buring JE, Rifai N . C-reactive protein and other markers of inflammation in the prediction of cardiovascular disease in women. N Engl J Med 2000; 342: 836–843.
Sesso HD, Buring JE, Rifai N, Blake G, Gaziano M, Ridker P . C- Reactive protein and the risk of developing hypertension. JAMA 2003; 290: 2945–2951.
Virdis A, Schiffrin EL . Vascular inflammation: a role in vascular disease in hypertension? Curr Opin Nephrol Hypertens 2003; 12: 181–187.
Chon H, Gaillard C, Van Der Meijden B, Dijstelbloem H, Kraaijenhagen R, Van Leenen D et al. Broadly altered gene expression in blood leukocytes in essential hypertension is absent during treatment. Hypertension 2004; 43: 947–995.
Tsioufis C, Stougiannos P, Kakkavas A, Toutouza M, Mariolis A, Vlasseros I et al. Relation of left ventricular concentric remodeling to levels of C-reactive protein and serum amyloid A in patients with essential hypertension. Am J Cardiol 2005; 2: 252–256.
Tsioufis C, Dimitriadis K, Chatzis D, Vasiliadou C, Tousoulis D, Papademetriou V et al. Relation of microalbuminuria to adiponectin and augmented C-reactive protein levels in men with essential hypertension. Am J Cardiol 2005; 96: 946–951.
Verdecchia P . Prognostic value of ambulatory blood pressure, current evidence and clinical implications. Hypertension 2000; 35: 844–851.
Tsioufis C, Stefanadis C, Antoniadis D, Kallikazaros I, Zambaras P, Pitsavos C et al. Absence of any significant effects of circadian blood pressure variations on carotid artery elastic properties in essential hypertensive subjects. J Hum Hypertens 2000; 14: 813–818.
Verdecchia P, Schillaci G, Guerrieri M, Gatteschi C, Benemio G, Boldrini F et al. Circadian blood pressure changes and left ventricular hypertrophy in essential hypertension. Circulation 1990; 81: 528–536.
Metoki H, Ohkubo T, Kikuya M, Asayama K, Obara T, Hashimoto J et al. Prognostic significance for stroke of a morning pressor surge and a nocturnal blood pressure decline: The Ohasama Study. J Hypertens 2006; 47: 149–154.
Pearson TA, Mensah GA, Alexander RW, Anderson JL, Cannon RO, Criqui M et al. Markers of inflammation and cardiovascular disease: application to clinical and public health practice: a statement for healthcare professionals from the Centres for Disease Control and Prevention and the American Heart Association. Circulation 2003; 107: 499–511.
Gottdiener JS, Bednarz J, Devereux R, Gardin J, Klein A, Manning WJ et al. American society of echocardiography: recommendations for use of echocardiography in clinical trials; a report from the American society of echocardiography. J Am Soc Echocardiogr 2004; 17: 1086–1119.
Verdecchia P, Schillaci G, Borgioni C, Ciucci A, Sacchi N, Battistelli M et al. Gender, daynight blood pressure changes and left ventricular mass in essential hypertension. Dippers and Peakers. Am J Hypertens 1995; 8: 193–196.
Gorostidi M, Sobrino J, Segura J, Sierra C, de la Sierra A, Hernandez Del Rey R et al. Ambulatory blood pressure monitoring in hypertensive patients with high cardiovascular risk: a cross-sectional analysis of a 20 000-patient database in Spain. J Hypertens 2007; 25: 977–984.
Maeda K, Yasunari K, Watanabe T, Nakamura M . Oxidative stress by peripheral blood mononuclear cells is increased in hypertensives with an extreme-dipper pattern and/or morning surge in blood pressure. Hypertens Res 2005; 28: 755–761.
Von Kanel R, Jain S, Mills PJ, Nelesen RA, Adler KA, Hong S et al. Relation of nocturnal blood pressure dipping to cellular adhesion, inflammation and hemostasis. J Hypertens 2004; 22: 2087–2093.
Schillaci G, Pirro M, Gemelli F, Pasqualini L, Vaudo G, Marchesi S et al. Increased C-reactive protein concentrations in never-treated hypertension: the role of systolic and pulse pressures. J Hypertens 2003; 21: 1841–1846.
Abramson J, Weintraub W, Vaccarino V . Association between pulse pressure and C-reactive protein among apparently healthy US adults. Hypertension 2002; 39: 197–202.
Tsioufis C, Antoniadis D, Stefanadis C, Tzioumis K, Pitsavos C, Kallikazaros I et al. Relationships between new risk factors and circadian blood pressure variation in untreated subjects with essential hypertension. Am J Hypertens 2002; 15: 600–604.
Gilardini L, Parati G, Sartorio A, Mazzilli G, Pontiggia B, Invitti C . Sympathoadrenergic and metabolic factors re involved in ambulatory blood pressure rise in childhood obesity. J Hum Hypertens 2008; 22: 75–82.
Author information
Authors and Affiliations
Corresponding author
Additional information
Conflict of interest
None.
Rights and permissions
About this article
Cite this article
Tsioufis, C., Syrseloudis, D., Dimitriadis, K. et al. Disturbed circadian blood pressure rhythm and C-reactive protein in essential hypertension. J Hum Hypertens 22, 501–508 (2008). https://doi.org/10.1038/jhh.2008.20
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/jhh.2008.20
Keywords
This article is cited by
-
Association of nocturnal blood pressure patterns with inflammation and central and peripheral estimates of vascular health in rheumatoid arthritis
Journal of Human Hypertension (2018)
-
Determinants of day–night difference in blood pressure, a comparison with determinants of daytime and night-time blood pressure
Journal of Human Hypertension (2017)
-
Higher Frequency of Nocturnal Blood Pressure Dipping but Not Heart Rate Dipping in Inflammatory Bowel Disease
Digestive Diseases and Sciences (2017)
-
Improving the detection of preclinical organ damage in newly diagnosed hypertension: nocturnal hypertension versus non-dipping pattern
Journal of Human Hypertension (2015)
-
Subendocardial viability ratio as an index of impaired coronary flow reserve in hypertensives without significant coronary artery stenoses
Journal of Human Hypertension (2012)