Abstract
Background/Objectives:
Little is known regarding whether or not combining daily exercise (EX) with caloric restriction (CR) additionally alleviates non-alcoholic fatty liver disease (NAFLD). The study investigated the effect of the combination of EX and CR on NAFLD and its underlying mechanisms in high-fat diet (HFD)-induced obese mice.
Methods:
C57BL/6 mice (N=50) were fed a standard chow (SC; n=10) or HFD (n=40) for 24 weeks. After 16 weeks, the HFD mice were further assigned to one of the following groups for the remaining 8 weeks: the first group of mice (HFD; n=10) remained to HFD, the second group of mice (HFD-EX; n=10) remained to HFD while subjected to EX, the third group of mice (HFD-CR; n=10) switched their diet from HFD to SC and the fourth group of mice (HFD-EX+CR; n=10) switched their diet from HFD to SC while simultaneously being subjected to EX.
Results:
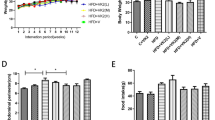
HFD resulted in obesity, impaired glucose tolerance, hypercholesterolemia and histology-based hepatic steatosis in conjunction with hypoadiponectinemia and downregulation of hepatic adiponectin receptors. However, EX or CR alleviated the fatty liver and its metabolic complications significantly. Compared with EX or CR alone, the combination of EX and CR resulted in further alleviations of NAFLD-associated conditions. The additive benefits of the combined treatment were associated with greater elevations of adiponectin and its hepatic receptors, in conjunction with greater expression of their downstream targets involved in fatty acid oxidation, de novo lipogenesis and anti-inflammation.
Conclusions:
The current findings provide experimental evidence in favor of the combination of EX and CR as a superior strategy for NAFLD treatment than EX or CR alone.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout





Similar content being viewed by others
References
Angulo P . Nonalcoholic fatty liver disease. N Engl J Med 2002; 346: 1221–1231.
Anderson EL, Howe LD, Jones HE, Higgins JP, Lawlor DA, Fraser A . The prevalence of non-alcoholic fatty liver disease in children and adolescents: a systematic review and meta-analysis. PLoS One 2015; 10: e0140908.
Browning JD, Szczepaniak LS, Dobbins R, Nuremberg P, Horton JD, Cohen JC et al. Prevalence of hepatic steatosis in an urban population in the United States: impact of ethnicity. Hepatology 2004; 40: 1387–1395.
Hallsworth K, Fattakhova G, Hollingsworth KG, Thoma C, Moore S, Taylor R et al. Resistance exercise reduces liver fat and its mediators in non-alcoholic fatty liver disease independent of weight loss. Gut 2011; 60: 1278–1283.
Thoma C, Day CP, Trenell MI . Lifestyle interventions for the treatment of non-alcoholic fatty liver disease in adults: a systematic review. J Hepatol 2012; 56: 255–266.
Yu H, Jia W, Guo Z . Reducing liver fat by low carbohydrate caloric restriction targets hepatic glucose production in non-diabetic obese adults with non-alcoholic fatty liver disease. J Clin Med 2014; 3: 1050–1063.
Kirk E, Reeds DN, Finck BN, Mayurranjan SM, Patterson BW, Klein S . Dietary fat and carbohydrates differentially alter insulin sensitivity during caloric restriction. Gastroenterology 2009; 136: 1552–1560.
Elias MC, Parise ER, de Carvalho L, Szejnfeld D, Netto JP . Effect of 6-month nutritional intervention on non-alcoholic fatty liver disease. Nutrition 2010; 26: 1094–1099.
Cava E, Fontana L . Will calorie restriction work in humans? Aging (Albany NY) 2013; 5: 507–514.
Barnosky AR, Hoddy KK, Unterman TG, Varady KA . Intermittent fasting vs daily calorie restriction for type 2 diabetes prevention: a review of human findings. Transl Res 2014; 164: 302–311.
Racette SB, Weiss EP, Villareal DT, Arif H, Steger-May K, Schechtman KB et alWashington University School of Medicine CALERIE Group. One year of caloric restriction in humans: feasibility and effects on body composition and abdominal adipose tissue. J Gerontol A Biol Sci Med Sci 2006; 61: 943–950.
Church TS, Kuk JL, Ross R, Priest EL, Biltoft E, Blair SN . Association of cardiorespiratory fitness, body mass index, and waist circumference to nonalcoholic fatty liver disease. Gastroenterology 2006; 130: 2023–2030.
Gerber L, Otgonsuren M, Mishra A, Escheik C, Birerdinc A, Stepanova M et al. Non-alcoholic fatty liver disease (NAFLD) is associated with low level of physical activity: a population-based study. Aliment Pharmacol Ther 2012; 36: 772–781.
Johnson NA, Sachinwalla T, Walton DW, Smith K, Armstrong A, Thompson MW et al. Aerobic exercise training reduces hepatic and visceral lipids in obese individuals without weight loss. Hepatology 2009; 50: 1105–1112.
Van Der Heijden GJ, Wang ZJ, Chu Z, Toffolo G, Manesso E, Sauer PJ et al. Strength exercise improves muscle mass and hepatic insulin sensitivity in obese youth. Med Sci Sports Exerc 2010; 42: 1973–1980.
Shojaee-Moradie F, Baynes KC, Pentecost C, Bell JD, Thomas EL, Jackson NC et al. Exercise training reduces fatty acid availability and improves the insulin sensitivity of glucose metabolism. Diabetologia 2007; 50: 404–413.
Rector RS, Thyfault JP, Morris RT, Laye MJ, Borengasser SJ, Booth FW et al. Daily exercise increases hepatic fatty acid oxidation and prevents steatosis in Otsuka Long-Evans Tokushima Fatty rats. Am J Physiol Gastrointest Liver Physiol 2008; 294: G619–G626.
Kapravelou G, Martínez R, Andrade AM, Nebot E, Camiletti-Moirón D, Aparicio VA et al. Aerobic interval exercise improves parameters of nonalcoholic fatty liver disease (NAFLD) and other alterations of metabolic syndrome in obese Zucker rats. Appl Physiol Nutr Metab 2015; 40: 1242–1252.
Berglund ED, Lustig DG, Baheza RA, Hasenour CM, Lee-Young RS, Donahue EP et al. Hepatic glucagon action is essential for exercise-induced reversal of mouse fatty liver. Diabetes 2011; 60: 2720–2729.
Oh S, Tanaka K, Tsujimoto T, So R, Shida T, Shoda J . Regular exercise coupled to diet regimen accelerates reduction of hepatic steatosis and associated pathological conditions in nonalcoholic fatty liver disease. Metab Syndr Relat Disord 2014; 12: 290–298.
Yamauchi T, Kamon J, Ito Y, Tsuchida A, Yokomizo T, Kita S et al. Cloning of adiponectin receptors that mediate antidiabetic metabolic effects. Nature 2003; 423: 762–769.
Yamauchi T, Nio Y, Maki T, Kobayashi M, Takazawa T, Iwabu M et al. Targeted disruption of AdipoR1 and AdipoR2 causes abrogation of adiponectin binding and metabolic actions. Nat Med 2007; 13: 332–339.
Iwabu M, Yamauchi T, Okada-Iwabu M, Sato K, Nakagawa T, Funata M et al. Adiponectin and AdipoR1 regulate PGC-1alpha and mitochondria by Ca(2+) and AMPK/SIRT1. Nature 2010; 464: 1313–1319.
Cho J, Kim S, Lee S, Kang H . Effect of training intensity on nonalcoholic fatty liver disease. Med Sci Sports Exerc 2015; 47: 1624–1634.
Hong F, Radaeva S, Pan HN, Tian Z, Veech R, Gao B . Interleukin 6 alleviates hepatic steatosis and ischemia/reperfusion injury in mice with fatty liver disease. Hepatology 2004; 40: 933–941.
Folch J, Lees M, Sloane Stanley GH . A simple method for the isolation and purification of total lipids from animal tissues. J Biol Chem 1957; 226: 497–509.
Rector RS, Uptergrove GM, Morris EM, Borengasser SJ, Laughlin MH, Booth FW et al. Daily exercise vs. caloric restriction for prevention of nonalcoholic fatty liver disease in the OLETF rat model. Am J Physiol Gastrointest Liver Physiol 2011; 300: G874–G883.
Schultz A, Mendonca LS, Aguila MB, Mandarim-de-Lacerda CA . Swimming training beneficial effects in a mice model of nonalcoholic fatty liver disease. Exp Toxicol Pathol 2012; 64: 273–282.
Linden MA, Lopez KT, Fletcher JA, Morris EM, Meers GM, Siddique S et al. Combining metformin therapy with caloric restriction for the management of type 2 diabetes and nonalcoholic fatty liver disease in obese rats. Appl Physiol Nutr Metab 2015; 40: 1038–1047.
Huang P, Li S, Shao M, Qi Q, Zhao F, You J et al. Calorie restriction and endurance exercise share potent anti-inflammatory function in adipose tissues in ameliorating diet-induced obesity and insulin resistance in mice. Nutr Metab (Lond) 2010; 7: 59.
Kurosaka Y, Shiroya Y, Yamauchi H, Kaneko T, Okubo Y, Shibuya K et al. Effects of habitual exercise and dietary restriction on intrahepatic and periepididymal fat accumulation in Zucker fatty rats. BMC Res Notes 2015; 8: 121.
Zhu M, Miura J, Lu LX, Bernier M, DeCabo R, Lane MA et al. Circulating adiponectin levels increase in rats on caloric restriction: the potential for insulin sensitization. Exp Gerontol 2004; 39: 1049–1059.
Wang Z, Masternak MM, Al-Regaiey KA, Bartke A . Adipocytokines and the regulation of lipid metabolism in growth hormone transgenic and calorie-restricted mice. Endocrinology 2007; 148: 2845–2853.
Maeda N, Shimomura I, Kishida K, Nishizawa H, Matsuda M, Nagaretani H et al. Diet-induced insulin resistance in mice lacking adiponectin/ACRP30. Nat Med 2002; 8: 731–737.
Ouchi N, Kihara S, Arita Y, Maeda K, Kuriyama H, Okamoto Y et al. Novel modulator for endothelial adhesion molecules: adipocyte-derived plasma protein adiponectin. Circulation 1999; 100: 2473–2476.
Yokota T, Oritani K, Takahashi I, Ishikawa J, Matsuyama A, Ouchi N et al. Adiponectin, a new member of the family of soluble defense collagens, negatively regulates the growth of myelomonocytic progenitors and the functions of macrophages. Blood 2000; 96: 1723–1732.
Bouassida A, Chamari K, Zaouali M, Feki Y, Zbidi A, Tabka Z . Review on leptin and adiponectin responses and adaptations to acute and chronic exercise. Br J Sports Med 2010; 44: 620–630.
Acknowledgements
The National Research Foundation Grants funded by the Korean Government (NRF-2013S1A2A2034953 and NRF-2015S1A5B5A02012775).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Cho, J., Koh, Y., Han, J. et al. Adiponectin mediates the additive effects of combining daily exercise with caloric restriction for treatment of non-alcoholic fatty liver. Int J Obes 40, 1760–1767 (2016). https://doi.org/10.1038/ijo.2016.104
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ijo.2016.104