Abstract
Increase in cerebrospinal fluid (CSF) Na+ concentration ([Na+]) precedes hypertension and is a key step in the development of salt-induced hypertension. In the choroid plexus (CP), epithelial Na+ channels (ENaCs) have an important role in Na+ transport from the blood into the CSF. However, it remains unknown whether the mineralocorticoid receptors (MR)/ENaCs pathway in the CP of stroke-prone spontaneously hypertensive rats (SHRSP) is involved in neural mechanisms of hypertension. Therefore, we examined the role of the MR/ENaCs pathway in the CP in the development of hypertension in SHRSP associated with an increase in CSF [Na+]. As a marker of MR activation, serum/glucocorticoid-inducible kinase 1 (Sgk1) expression levels in the CP were measured and found to be greater in SHRSP than in Wistar–Kyoto (WKY) rats. CSF [Na+] levels were also higher in SHRSP than in WKY rats. In SHRSP, high-salt intake (8%) increased blood pressure and urinary norepinephrine excretion compared with those in animals fed a regular salt diet (0.5%) for 2 weeks. Furthermore, the expression levels of MR, Sgk1 and ENaCs in the CP and the increase in CSF [Na+] were greater in SHRSP fed a high-salt diet than in those fed a regular salt diet. These alterations were attenuated by intracerebroventricular infusion of eplerenone (10 μg kg−1 per day), except for α-ENaC and β-ENaC. We conclude that activation of the MR/ENaCs pathway in the CP contributes to hypertension via an increase in CSF [Na+], thereby exaggerating salt-induced hypertension with sympathetic hyperactivation in SHRSP.
Similar content being viewed by others
Introduction
Hypertension is a major risk factor for cardiovascular diseases.1 The percentages of essential hypertension patients who are salt sensitive have varied widely among study cohorts, ranging between 30 and 70%.2 The appropriate therapeutic target of salt-induced hypertension has been determined to be volume overload, so that sodium restriction and diuretics are beneficial for salt-induced hypertension.3, 4 Abnormal sympathetic hyperactivity has also been detected in patients with salt-induced hypertension.5, 6 Thus, in addition to the role of kidney, the central nervous system has an important role in salt-induced hypertension.6, 7
An increase in cerebrospinal fluid (CSF) Na+ concentration ([Na+]) is responsible for activation of the central sympathetic outflow.8, 9 High-salt intake elicits an increase in CSF [Na+] and causes sympathetic hyperactivity and hypertension in salt-sensitive model rats, such as Dahl S rats.7, 10 It has also been demonstrated that an increase in CSF [Na+] causes central aldosterone production, mineralocorticoid receptors (MR) activation and renin–angiotensin system (RAS) activation, thereby leading to sympathetic hyperactivity.11 On the other hand, high-salt intake does not affect CSF [Na+], blood pressure (BP) or heart rate (HR) in normotensive model rats.8 However, intracerebroventricular (ICV) infusion of Na+-rich artificial CSF elicits MR activation in the hypothalamus, leading to increase in BP through sympathoexcitation in both salt-sensitive model rats and normotensive model rats, although the extent of sympathoexcitation is greater in salt-sensitive rats than in normotensive rats.12, 13 These observations suggest that an increase in Na+ in the brain elicits sympathoexcitation irrespective of the presence/absence of salt-sensitive hypertension. However, it is possible that the mechanisms of Na+ transport into the brain might be different between normotensive and hypertensive models.
The epithelium of the choroid plexus (CP) is the major site for production of CSF, which is later absorbed by arachnoid granulations.14, 15 Enhanced Na+ uptake from the plasma to the CSF might therefore be an important step in the initiation of salt-induced hypertension in salt-sensitive hypertensive models. Epithelial Na+ channels (ENaCs) in the choroidal epithelia actively support Na+ influx from the plasma and, in general, Na+ levels in the CSF are higher than those in the plasma.16 The ENaCs form a heteromultimeric channel that is composed of three homologous α-, β- and γ-subunits.17 Both MR activation itself and the resulting MR-induced activation of serum/glucocorticoid-inducible kinase 1 (Sgk1) augment the expression of ENaCs in the kidney.18 Sgk1 is a key downstream effector of MR signaling in the kidneys, inducing the early and late responses through regulation of the epithelial sodium channel activity, trafficking, and transcription.19, 20, 21 The Sgk1 expression level also reflects MR activation, and used for this purpose because MR expression itself is not equal to MR activation.22 However, the mechanism by which the MR/ENaCs pathway in the CP contributes to an increase in CSF [Na+] and sympathoexcitation, and leads to hypertension in hypertensive model rats, remains unclear.
Stroke-prone spontaneously hypertensive rats (SHRSP) serve as an experimental model of salt-loading-accelerated hypertension.23, 24 We hypothesized that an increase in CSF [Na+] might be involved in the development of hypertension in the absence of sodium loading, or might worsen hypertension in the presence of sodium loading in SHRSP via irregularities in the MR/ENaCs pathway in the CP. Therefore, the aim of the present study was to determine whether the MR/ENaCs pathway in the CP was altered in SHRSP and, if so, to examine whether this alteration was involved in abnormal sympathetic hyperactivity with or without sodium loading in SHRSP. For this purpose, we compared the expressions of MR, Sgk1 and ENaCs in the CP without sodium loading between SHRSP and Wistar–Kyoto (WKY) rats. Furthermore, we investigated these expressions in SHRSP fed a high-salt diet. Finally, we investigated the effect of ICV infusion of an MR blocker concomitant with high-salt loading on sympathetic activity and CSF [Na+].
Methods
Animals
This study was reviewed and approved by the Committee on Ethics of Animal Experiments, Kyushu University Graduate School of Medical Sciences, and conducted according to the Guidelines for Animal Experiments of Kyushu University. Male WKY rats and SHRSP (260–330 g; 12–14 weeks old) were obtained from SLC Japan (Hamamatsu, Japan). They were housed in temperature- (23±2°C) and light-controlled animal quarters and were provided with rat chow ad libitum.
Western blot analysis
Rats were killed with an overdose of sodium pentobarbital and the tissues of CP were obtained. The tissues were removed and homogenized in a lysis buffer. The protein concentration was determined using a bicinchonic acid protein assay kit (Pierce Chemical, Rockford, IL, USA). A 15-μg aliquot of protein from each sample was separated on a polyacrylamide gel with 10% sodium dodecyl sulfate. The proteins were then transferred onto polyvinylidene difluoride membranes (Immobilon-P membranes; Millipore, Billerica, MA, USA), and the membranes were incubated with rabbit immunoglobulin G (IgG) polyclonal antibody to MR (1:1000; Santa Cruz Biotechnology, Santa Cruz, CA, USA), with goat IgG polyclonal antibody to α-ENaC, rabbit polyclonal antibody to β-ENaC or rabbit polyclonal antibody to γ-ENaC (1:1000; Santa Cruz Biotechnology), or with rabbit IgG polyclonal antibody to Sgk1 (1:1000; Abcam, Cambridge, UK). Next, the membranes were incubated with horseradish peroxidase-conjugated horse anti-rabbit or anti-goat IgG antibody (1:10 000). Glyceraldehyde 3-phosphate dehydrogenase (GAPDH) was used as an internal control for the brain tissues. Immunoreactivity was detected by enhanced chemiluminescence autoradiography (ECL Western blotting detection kit; Amersham Pharmacia Biotech, Uppsala, Sweden), and the film was analyzed using the public domain software NIH Image (developed at the US National Institutes of Health and available on the Internet at http://rsb.info.nih.gov/nih-image/).
Measurement of CSF [Na+] and plasma [Na+]
The CSF was collected via puncture of the cisterna magna. CSF [Na+] was measured using an ion-selective electrode (model MI-425; Microelectrodes, Bedford, NH, USA). Plasma [Na+] was measured at SRL (Tokyo, Japan).
Intracarotid artery (ICA) infusion of NaCl in acute experiments
Rats were anesthetized with pentobarbital (50 mg kg−1 i.p. followed by 20 mg kg−1 h−1 i.v.) and artificially ventilated. A catheter (polyethylene (PE)-50 tubing) was inserted into the left internal carotid artery and NaCl (0.5 M, 1 M, 10 s for each injection, total infusion volume; 300 μl) was administered. A catheter was implanted into the left ICA and advanced 1.0–1.3 cm beyond the carotid sinus to avoid activation of arterial baroreceptors. Another catheter was then inserted into the left femoral artery to measure BP and HR. A pair of stainless steel bipolar electrodes was placed beneath the renal nerve to record multifiber renal sympathetic nerve activity.25, 26 All signals were recorded on a computer using a PowerLab system (AD Instruments, Colorado Springs, CO, USA). The signal from the electrodes was amplified, passed through a band pass filter, and then rectified and integrated (resetting every 0.1 s).
Measurements of BP and sympathetic activity in chronic experiments
Systolic BP of conscious animals was measured using tail-cuff plethysmography (BP-98 A; Softron, Tokyo, Japan). Sympathetic activity was evaluated by measuring 24-h urinary norepinephrine excretion using high-performance liquid chromatography before and at day 14. Urinary norepinephrine excretion was calculated as described previously.27
ICV infusion of eplerenone
Under sodium pentobarbital anesthesia (50 mg kg−1 i.p.) rats were placed in a stereotaxic frame. The skin overlying the midline of the skull was incised and a small hole was made with a dental drill at the following coordinates: 0.8 mm posterior and 1.5 mm lateral relative to bregma. The infusion cannula from an Alzet brain infusion kit 2 (DURECT Corporation, Cupertino, CA, USA) connected to an osmotic pump (model 2002; Alzet) was lowered 3.5 mm below the skull surface and fixed to the skull surface with tissue adhesive. The osmotic mini pump was inserted subcutaneously in the back. The ICV infusion of artificial CSF+vehicle (1% DMSO) or artificial CSF+eplerenone (10 μg kg−1per day in vehicle) (kindly provided by Pfizer Pharmaceutical Company, New York, NY, USA) for 2 weeks was performed in conjunction with feeding of a high-salt diet, and the infusion and diet were started simultaneously.
Experimental protocols
Protocol 1: Experiments with rats without salt loading
(1) Western blot analysis of MR, Sgk1 and ENaCs in the CP of SHRSP and WKY rats; (2) evaluations of CSF [Na+] and plasma [Na+] in SHRSP and WKY rats; (3) acute bolus ICA injection of NaCl (0.5 M, 1 M, 300 μl per 10 s) in SHRSP and WKY rats. The rats were fed a regular diet.
Protocol 2: Experiments with rats fed a high-salt diet
SHRSP and WKY rats were divided randomly into two groups: rats fed a high-salt (8% NaCl) diet for 2 weeks and rats fed a regular (0.5% NaCl) diet for 2 weeks. Then, the following protocols were performed. (1) Western blot analysis of MR, Sgk1 and ENaCs in the CP of SHRSP and WKY rats fed a high-salt or regular diet; (2) evaluations of CSF [Na+] in SHRSP and WKY rats fed a high-salt diet.
Protocol 3: Experiments with SHRSP fed a high-salt diet with eplerenone
ICV infusion of artificial CSF or eplerenone for 2 weeks in SHRSP fed a high-salt diet. Then, the following protocols were performed. (1) Measurement of BP and HR using the tail-cuff method; (2) western blot analysis of MR, Sgk1 and ENaCs in the CP; (3) Evaluations of CSF [Na+] and urinary norepinephrine in SHRSP.
Statistical analysis
All values are expressed as the means±s.e.m. Intergroup differences in the mean arterial pressure (MAP) and HR values obtained using the PowerLab and tail-cuff method were compared using two-way analysis of variance. In the analysis of variance, comparisons between any two mean values were performed using Bonferroni’s correction for multiple comparisons. The MR, Sgk1 and ENaCs protein expression values (western blot analysis), and the CSF [Na+] and plasma [Na+] values were compared using an unpaired t-test. Values of P<0.05 were considered statistically significant.
Results
Baseline MR, Sgk1 and ENaCs expressions in the CP of SHRSP and WKY rats fed a regular diet
MR expression in SHRSP did not differ from that in WKY rats, while Sgk1 expression was significantly greater in SHRSP (Figure 1a). The expressions of α-ENaC, β-ENaC and γ-ENaC were also significantly higher in SHRSP than in WKY rats (Figure 1b).
Western blot analysis demonstrating the expression levels of (a) the MR and Sgk1, and (b) α-, β- and γ-ENaCs in the CP of 12-week-old WKY and SHRSP rats. The densitometric average was normalized to the values obtained from the analysis of glyceraldehyde-3-phosphatase dehydrogenase (GAPDH) as an internal control. Expressions are shown relative to those seen in WKY rats, which are assigned a value of 1. Values are expressed as the mean±s.e.m. #P<0.01; n=4–5. (c) Plasma [Na+] and CSF [Na+] levels in WKY rats and SHRSP. #P<0.01; n=6–7.
Baseline plasma [Na+] and CSF [Na+] of SHRSP and WKY rats fed a regular diet
Plasma [Na+] levels did not differ between WKY rats and SHRSP (WKY, 145.4±0.8 mM; SHRSP, 145.1±0.8 mM; n=7 for each), but the level of CSF [Na+] was greater in SHRSP (WKY, 151.9±0.4 mM; SHRSP, 155.5±0.3 mM, n=6 for each; Figure 1c).
Effect of ICA NaCl infusion on MAP, HR and renal sympathetic nerve activity in SHRSP and WKY rats
ICA hypertonic NaCl (0.5 M, 1.0 M) infusions increased MAP in both WKY rats and SHRSP dose-dependently. However, the degrees of increase in MAP were greater in SHRSP than in WKY rats (% change of ΔMAP: WKY vs. SHRSP, 3.0±2.3% vs. 14.4±2.5%, P<0.05 (0.5 M); 7.5±4.3% vs. 35.1±5.5%, P<0.005 (1.0 M); n=5 for each; Figure 2). The duration of the responses lasted longer in SHRSP than WKY rats (WKY vs. SHRSP, 2.3±0.4 vs. 5.9±0.6 min, P<0.01 (0.5 M); 4.3±0.5 vs. 14.3±1.5 min, P<0.01 (1.0 M); n=5 for each). Peak responses of renal sympathetic nerve activity (% baseline) to NaCl were also greater in SHRSP than in WKY rats (% baseline: WKY vs. SHRSP, 6.5±3.7% vs. 20.3±1.1%, P<0.01 (0.5 M); 13.8±1.7% vs. 30.0±5.3%, P<0.05 (1.0 M); n=4-5 for each; Figure 2).
The responses of arterial pressure (AP) and renal sympathetic nerve activity (RSNA) to ICA NaCl (0.5 M, 1 M) infusions. (a) Raw data of the changes in AP and RSNA after ICA NaCl (1 M) infusions in WKY rats and SHRSP. (b) Group data of the changes in MAP and RSNA in response to ICA NaCl (0.5 M, 1 M) infusions. Values are expressed as the mean±s.e.m. *P<0.05, #P<0.01; n=4–5.
Effects of high-salt diet on systolic BP and CSF [Na+] in SHRSP and WKY rats
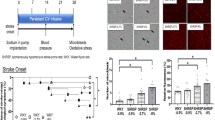
Systolic BP and HR of in SHRSP groups were significantly higher than those of WKY rats throughout the study (Table 1). SHRSP fed a high-salt diet exhibited a significantly higher systolic BP and HR than SHRSP fed a regular diet, starting at 12 weeks of age (P<0.05). Systolic BP also slightly increased in SHRSP fed a regular diet (P<0.05). Systolic BP and HR values for 2 weeks are shown in Table 1. CSF [Na+] in SHRSP also started to increase from day 4 (152.3±0.8 vs.158.6±0.4 mM, P<0.05). At day 14, CSF [Na+] in SHRSP fed a high-salt diet was significantly greater than in WKY fed a high-salt diet (152.4±0.4 vs.161.1±0.4 mM; Figure 3a). In contrast, in WKY rats, there were no significant changes in systolic BP and CSF [Na+] during the observation (Figure 3a and Table 1).
(a) CSF [Na+] in WKY rats and SHRSP by feeding with a high-salt diet at day 14. Values are expressed as the mean±s.e.m. *P<0.05; n=7 for each. (b) Western blot analysis demonstrating MR, Sgk1, α-, β- and γ- ENaC expression in the CP in SHRSP fed a high-salt or regular diet. The densitometric average is normalized to the values obtained from the analysis of GAPDH as an internal control. Expressions are shown relative to those in SHRSP fed a regular diet, which are assigned a value of 1. (c) Western blot analysis demonstrating MR, Sgk1, α-, β- and γ- ENaC expression in the CP in WKY rats fed a high-salt or regular diet. The densitometric average is normalized to the values obtained from the analysis of GAPDH as an internal control. Expressions are shown relative to those in WKY rats fed a regular diet, which are assigned a value of 1. Values are expressed as the mean±s.e.m. *P<0.05, #P<0.01; n=4–6.
Expression of MR, Sgk1 and ENaCs in the CP in SHRSP and WKY rats fed a high-salt diet
The expressions of MR, Sgk1 and ENaCs were significantly greater in SHRSP fed a high-salt diet than in those fed a regular diet (Figure 3b). The expressions of MR, Sgk1 and ENaCs were similar between WKY rats fed a high-salt diet and those fed a regular diet (Figure 3c).
Effects of eplerenone on systolic BP, sympathetic activity, CSF [Na+], and expression levels of MR, Sgk1 and ENaCs in SHRSP fed a high-salt diet
ICV infusion of eplerenone attenuated the increases in urinary norepinephrine and systolic BP in SHRSP fed a high-salt diet (Figures 4a and b). ICV infusion of eplerenone attenuated the increase in CSF [Na+] in SHRSP fed a high-salt diet (157.8±0.92 vs. 161.0±0.73 mM; Figure 4c). ICV infusion of eplerenone did not attenuate the enhanced expressions of MR, α-ENaC and β-ENaC, but did attenuate Sgk1 and γ-ENaC expression (Figures 5a and b).
Effects of ICV infusion of artificial CSF (aCSF) (high salt+aCSF) vs. eplerenone at 10 μg kg−1 per day (high salt+epl) in CP of SHRSP on systolic BP (SBP), heart rate (HR), sympathetic nerve activity and CSF [Na+] induced by high-salt intake. (a) Changes in resting SBP and HR response to ICV infusion of aCSF or eplerenone in rats fed a high-salt diet. #P<0.01; n=6 for each. (b) Group data for urinary norepinephrine excretion in SHRSP given a regular diet, a high-salt diet plus ICV infusion of aCSF (high salt+aCSF) or a high-salt diet plus eplerenone (high salt+epl). *P<0.05; n=5–6. (c) Group data for CSF [Na+] in SHRSP given a regular diet (regular), a high-salt diet plus ICV infusion of aCSF (high salt+aCSF) or a high-salt diet plus eplerenone (high salt+epl). *P<0.05, #P<0.01; n=10 for each.
Effects of ICV infusion of artificial CSF (aCSF) (high salt+aCSF) vs. eplerenone at 10 μg kg−1 per day (high salt+epl) in the CP of SHRSP. Western blot analysis demonstrating the expression of (a) MR, Sgk1, or (b) α-, β- and γ- ENaC in the CP in high salt+aCSF vs. high salt+epl. The densitometric average was normalized to the values obtained from the analysis of glyceraldehyde-3-phosphatase dehydrogenase (GAPDH) as an internal control. Expressions are shown relative to those seen in the high salt+aCSF group, which were assigned a value of 1. Values are expressed as the mean±s.e.m. #P<0.01; n=4–6.
Discussion
The present study demonstrated that the MR/ENaCs pathway in the CP of SHRSP was activated before salt loading, leading to an increase in the CSF [Na+] and eliciting sympathetic hyperactivity. Salt loading then elicited further activation of this pathway in the CP and an additional increase in CSF [Na+], thereby causing further sympathetic hyperactivity and BP elevation.
We first investigated the alterations of the Na+ transport system in the CP of SHRSP and found that the expressions of all subunit types of ENaCs were greater in SHRSP than in WKY rats. These data suggest that the function of the Na+ transport system in the CP was enhanced in SHRSP. In fact, the plasma [Na+] level was similar between SHRSP and WKY rats, but the CSF [Na+] level was greater in SHRSP than in WKY rats. Taken together, these data suggest that activation of ENaCs in the CP elicited increase in CSF [Na+] in SHRSP.
We considered that these alterations occurring in SHRSP may contribute to the development of hypertension. Thus, we investigated whether activated ENaCs in the CP contribute to the development of hypertension with sympathetic hyperactivity. ICA infusions of hypertonic NaCl solutions increased renal sympathetic nerve activity and AP and the degrees of these changes were greater in SHRSP than in WKY rats. It has been reported that increases in the amount of plasma [Na+] perfusing the forebrain evoke a prompt increase of sympathetic nerve activity.28, 29 An increase in CSF [Na+] may excite Na+-sensitive neurons in the circumventricular organs, such as the subfornical organ.30 This increased neuronal activity could be relayed to the paraventricular nucleus of the hypothalamus or rostral ventrolateral medulla, thereby increasing sympathetic nerve activity and BP.31, 32, 33 Furthermore, an increase in CSF [Na+] would increase the level of hypothalamic tissue [Na+]34 and could thereby enhance the firing activity of Na+-sensitive neurons in the paraventricular nucleus.35 We also need to consider the possibility that circumventricular organs could sense hyperosmolality after ICA infusions of hypertonic NaCl solutions thereby activates sympathetic activity, although there is a clear difference between SHRSP and WKY rats.36 In addition, the duration of the responses lasted longer in SHRSP than WKY rats. We were not able to measure CSF [Na+] before and after ICA infusion because of technical difficulties. However, these data indirectly suggest that Na+ uptake into the CSF is enhanced and this contributes to hypertension with sympathoexcitation in SHRSP without salt loading.
In salt-sensitive model rats, high-salt intake causes an increase in CSF [Na+] and leads to sympathetic hyperactivity and hypertension.7, 37, 38 SHRSP are also known as a salt-induced hypertension model.24 A high-salt diet elicited hypertension with sympathetic hyperactivity in SHRSP as previously described.24, 39 We found that the expressions of all subtypes of ENaCs in the CP and CSF [Na+] were increased in SHRSP fed a high-salt diet concomitant with changes in MAP. These data suggest that activated ENaCs in the CP of SHRSP accelerated the increase in CSF [Na+], and this increase further enhanced the levels of ENaCs, leading to sympathetic hyperactivity (Figure 6).
The possible cascade that Na+ transport mechanisms in the central nervous system contributing to sympathetic hyperactivity and hypertension in SHRSP on high-salt intake. In SHRSP on high-salt intake, Na+ transport into CSF is enhanced and CSF [Na+] is increased. Activation of MR/ENaCs pathway in the choroid plexus is involved in Na+ transport from the blood into the CSF in SHRSP. The increased CSF [Na+] increased the neuronal activity in the PVN or other autonomic nuclei, thereby increasing the central sympathetic outflow. This, in turn, leads to sympathetic hyperactivity and hypertension. The broken lines indicate hypothetical mechanisms suggested by other investigators. RAS indicates renin–angiotensin system.
It has been shown that aldosterone binds to MR and increases expression and activity of ENaCs in the distal nephron of the kidney, resulting in enhanced Na+ and water reabsorption, and presumably thereby elevated BP.18 We recently reported that activation of the MR/ENaCs pathway is considered to be an initial step in the acquisition of Na+ sensitivity in the brain in a pressure overload model.40 In fact, Western blotting in the present study revealed that the expression of Sgk1 was increased in SHRSP compared with WKY rats before salt loading, although the expression levels of MR did not differ between SHRSP and WKY rats. Moreover, expressions of MR and ENaCs in the CP were increased by salt loading in SHRSP. Taken together with the alterations of ENaCs, our findings suggest that MR and ENaCs in the CP are altered in parallel with or without salt loading in SHRSP. We also found that ICV infusion of an MR blocker attenuated BP elevation and increase in CSF [Na+] induced by chronic salt loading in SHRSP. Furthermore, the MR blocker inhibited the increase in Sgk1 expressions and γ-ENaC in the CP of SHRSP. However, we do not have a clear explanation why only γ-ENaC was smaller for eplerenon treated SHRSP on high-salt diet at the present time. There may be subunit-type-specific regulation of ENaC.40 These findings suggest that MR regulates Na+transport into the CSF by regulating the expressions of ENaCs in the CP of SHRSP, although we did not find the increased expression levels of α-ENaC and β-ENaC.
In consistent with the results of a previous study, SHRSP have significantly higher plasma aldosterone levels compared with WKY rats, indicating upregulation of the aldosterone system in SHRSP.24 If the aldosterone is the ligand of MR in the CP of SHRSP, MR is activated in SHRSP. In salt-sensitive model rats, high-salt intake produces aldosterone locally in the hypothalamus.11, 41 Another possibility is that locally produced aldosterone may affect MR activation in the CP via CSF.41, 42 In the absence of 11β-hydroxysteroid dehydrogenase type 2 in the CP, corticosterone is also a ligand for MR.43 On the other hand, Rac1 enhances MR independent of aldosterone in the kidney.44 We did not address precise mechanisms how MR in the CP was activated in SHRSP in the present study. Nevertheless, our findings suggest that MR activation has an important role for the increase in central sympathetic outflow in SHRSP. Further studies are necessary to clarify this important question.
The present study has some additional limitations. First, ENaCs exist on both the apical and basolateral side of the CP.34, 45 We did not examine the distribution of ENaCs in the CP in the present study because of the technical difficulty. Second, ICV infusion of an MR blocker may act on the nuclei other than those in the CP.46, 47 Third, Na+-K+-ATPase activity in the CP is also dependent on CSF [Na+] in Dahl salt-sensitive rats.48 MR regulates the transcription of Na+-K+-ATPase.49 Both ENaCs and Na+-K+-ATPase regulate Na+ transport in the CP. Further studies will be needed to clarify whether Na+-K+-ATPase alterations are involved in our observations in the present study.
In conclusion, our findings suggest that the MR/ENaCs pathway in the CP of SHRSP is activated before salt loading, leading to an increased CSF [Na+] and eliciting sympathetic hyperactivity. Second suggestion is that salt loading elicited further activation of this pathway in the CP and additional enhancement of the CSF [Na+] levels, leading to further sympathetic hyperactivity.
References
Rosamond W, Flegal K, Friday G, Furie K, Go A, Greenlund K, Haase N, Ho M, Howard V, Kissela B, Kittner S, Lloyd-Jones D, McDermott M, Meigs J, Moy C, Nichol G, O'Donnell CJ, Roger V, Rumsfeld J, Sorlie P, Steinberger J, Thom T, Wasserthiel-Smoller S, Hong Y. American Heart Association Statistics Committee and Stroke Statistics Subcommittee. Heart disease and stroke statistics–2007 update: A report from the american heart association statistics committee and stroke statistics subcommittee. Circulation 2007; 115: e69–e171.
Rassler B . The renin-angiotensin system in the development of salt-sensitive hypertension in animal models and humans. Pharmaceuticals 2010; 3: 940–960.
Kawano Y . Diurnal blood pressure variation and related behavioral factors. Hypertens Res 2011; 34: 281–285.
Sica DA, Carter B, Cushman W, Hamm L . Thiazide and loop diuretics. J Clin Hypertens 2011; 13: 639–643.
Kawano Y, Yoshida K, Kawamura M, Yoshimi H, Ashida T, Abe H, Imanishi M, Kimura G, Kojima S, Kuramochi M . Sodium and noradrenaline in cerebrospinal fluid and blood in salt-sensitive and non-salt-sensitive essential hypertension. Clin Exp Pharmacol Physiol 1992; 19: 235–241.
Adrogue HJ, Madias NE . Sodium and potassium in the pathogenesis of hypertension. N Engl J Med 2007; 356: 1966–1978.
Huang BS, Amin MS, Leenen FH . The central role of the brain in salt-sensitive hypertension. Curr Opin Cardiol 2006; 21: 295–304.
Huang BS, Van Vliet BN, Leenen FH . Increases in CSF [Na+] precede the increases in blood pressure in dahl S rats and SHR on a high-salt diet. Am J Physiol Heart Circ Physiol 2004; 287: H1160–H1166.
Takahashi H, Yoshika M, Komiyama Y, Nishimura M . The central mechanism underlying hypertension: a review of the roles of sodium ions, epithelial sodium channels, the renin-angiotensin-aldosterone system, oxidative stress and endogenous digitalis in the brain. Hypertens Res 2011; 34: 1147–1160.
Fujita M, Ando K, Nagae A, Fujita T . Sympathoexcitation by oxidative stress in the brain mediates arterial pressure elevation in salt-sensitive hypertension. Hypertension 2007; 50: 360–367.
Huang BS, White RA, Jeng AY, Leenen FH . Role of central nervous system aldosterone synthase and mineralocorticoid receptors in salt-induced hypertension in dahl salt-sensitive rats. Am J Physiol Regul Integr Comp Physiol 2009; 296: R994–R1000.
Huang BS, Wang H, Leenen FH . Enhanced sympathoexcitatory and pressor responses to central Na+ in dahl salt-sensitive vs. -resistant rats. Am J Physiol Heart Circ Physiol 2001; 281: H1881–H1889.
Huang BS, White RA, Ahmad M, Jeng AY, Leenen FH . Central infusion of aldosterone synthase inhibitor prevents sympathetic hyperactivity and hypertension by central Na+ in wistar rats. Am J Physiol Regul Integr Comp Physiol 2008; 295: R166–R172.
Praetorius J . Water and solute secretion by the choroid plexus. Pflugers Arch 2007; 454: 1–18.
Brown PD, Davies SL, Speake T, Millar ID . Molecular mechanisms of cerebrospinal fluid production. Neuroscience 2004; 129: 957–970.
Amin MS, Wang HW, Reza E, Whitman SC, Tuana BS, Leenen FH . Distribution of epithelial sodium channels and mineralocorticoid receptors in cardiovascular regulatory centers in rat brain. Am J Physiol Regul Integr Comp Physiol 2005; 289: R1787–R1797.
Canessa CM, Schild L, Buell G, Thorens B, Gautschi I, Horisberger JD, Rossier BC . Amiloride-sensitive epithelial Na+ channel is made of three homologous subunits. Nature 1994; 367: 463–467.
Schild L . The epithelial sodium channel and the control of sodium balance. Biochim Biophys Acta 2010; 1802: 1159–1165.
Wulff P, Vallon V, Huang DY, Volkl H, Yu F, Richter K, Jansen M, Schlunz M, Klingel K, Loffing J, Kauselmann G, Bosl MR, Lang F, Kuhl D . Impaired renal Na+ retention in the sgk1-knockout mouse. J Clin Invest 2002; 110: 1263–1268.
Pearce D, Kleyman TR . Salt, sodium channels, and SGK1. J Clin Invest 2007; 117: 592–595.
Zhang W, Xia X, Reisenauer MR, Rieg T, Lang F, Kuhl D, Vallon V, Kone BC . Aldosterone-induced Sgk1 relieves Dot1a-Af9-mediated transcriptional repression of epithelial na+ channel alpha. J Clin Invest 2007; 117: 773–783.
Quinkler M, Zehnder D, Eardley KS, Lepenies J, Howie AJ, Hughes SV, Cockwell P, Hewison M, Stewart PM . Increased expression of mineralocorticoid effector mechanisms in kidney biopsies of patients with heavy proteinuria. Circulation 2005; 112: 1435–1443.
Camargo MJ, von Lutterotti N, Campbell WG, Pecker MS, James GD, Timmermans PB, Laragh JH . Control of blood pressure and end-organ damage in maturing salt-loaded stroke-prone spontaneously hypertensive rats by oral angiotensin II receptor blockade. J Hypertens 1993; 11: 31–40.
Endemann DH, Touyz RM, Iglarz M, Savoia C, Schiffrin EL . Eplerenone prevents salt-induced vascular remodeling and cardiac fibrosis in stroke-prone spontaneously hypertensive rats. Hypertension 2004; 43: 1252–1257.
Nishihara M, Hirooka Y, Matsukawa R, Kishi T, Sunagawa K . Oxidative stress in the rostral ventrolateral medulla modulates excitatory and inhibitory inputs in spontaneously hypertensive rats. J Hypertens 2012; 30: 97–106.
Matsukawa R, Hirooka Y, Nishihara M, Ito K, Sunagawa K . Neuregulin-1/ErbB signaling in rostral ventrolateral medulla is involved in blood pressure regulation as an antihypertensive system. J Hypertens 2011; 29: 1735–1742.
Ito K, Kimura Y, Hirooka Y, Sagara Y, Sunagawa K . Activation of rho-kinase in the brainstem enhances sympathetic drive in mice with heart failure. Auton Neurosci 2008; 142: 77–81.
Schad H, Seller H . Influence of intracranial osmotic stimuli on renal nerve activity in anaesthetized cats. Pflugers Arch 1975; 353: 107–121.
Kumagai H, Oshima N, Matsuura T, Iigaya K, Imai M, Onimaru H, Sakata K, Osaka M, Onami T, Takimoto C, Kamayachi T, Itoh H, Saruta T . Importance of rostral ventrolateral medulla neurons in determining efferent sympathetic nerve activity and blood pressure. Hypertens Res 2012; 35: 132–141.
Denton DA, McKinley MJ, Weisinger RS . Hypothalamic integration of body fluid regulation. Proc Natl Acad Sci USA 1996; 93: 7397–7404.
Cato MJ, Toney GM . Angiotensin II excites paraventricular nucleus neurons that innervate the rostral ventrolateral medulla: An in vitro patch-clamp study in brain slices. J Neurophysiol 2005; 93: 403–413.
Li DP, Chen SR, Pan HL . Angiotensin II stimulates spinally projecting paraventricular neurons through presynaptic disinhibition. J Neurosci 2003; 23: 5041–5049.
Hirooka Y . Oxidative stress in the cardiovascular center has a pivotal role in the sympathetic activation in hypertension. Hypertens Res 2011; 34: 407–412.
Wang HW, Amin MS, El-Shahat E, Huang BS, Tuana BS, Leenen FH . Effects of central sodium on epithelial sodium channels in rat brain. Am J Physiol Regul Integr Comp Physiol 2010; 299: R222–R233.
Gabor A, Leenen FH . Mechanisms in the PVN mediating local and central sodium-induced hypertension in wistar rats. Am J Physiol Regul Integr Comp Physiol 2009; 296: R618–R630.
Shi P, Martinez MA, Calderon AS, Chen Q, Cunningham JT, Toney GM . Intra-carotid hyperosmotic stimulation increases fos staining in forebrain organum vasculosum laminae terminalis neurones that project to the hypothalamic paraventricular nucleus. J Physiol 2008; 586: 5231–5245.
Suzuki J, Ogawa M, Tamura N, Maejima Y, Takayama K, Maemura K, Honda K, Hirata Y, Nagai R, Isobe M . A critical role of sympathetic nerve regulation for the treatment of impaired daily rhythm in hypertensive Dahl rats. Hypertens Res 2010; 33: 1060–1065.
Brooks VL, Haywood JR, Johnson AK . Translation of salt retention to central activation of the sympathetic nervous system in hypertension. Clin Exp Pharmacol Physiol 2005; 32: 426–432.
Koga Y, Hirooka Y, Araki S, Nozoe M, Kishi T, Sunagawa K . High salt intake enhances blood pressure increase during development of hypertension via oxidative stress in rostral ventrolateral medulla of spontaneously hypertensive rats. Hypertens Res 2008; 31: 2075–2083.
Ito K, Hirooka Y, Sunagawa K . Blockade of mineralocorticoid receptors improves salt-induced left-ventricular systolic dysfunction through attenuation of enhanced sympathetic drive in mice with pressure overload. J Hypertens 2010; 28: 1449–1458.
Gomez-Sanchez EP, Ahmad N, Romero DG, Gomez-Sanchez CE . Is aldosterone synthesized within the rat brain? Am J Physiol Endocrinol Metab 2005; 288: E342–E346.
Geerling JC, Loewy AD . Aldosterone in the brain. Am J Physiol Renal Physiol 2009; 297: F559–F576.
Funder JW . Mineralocorticoid receptors: distribution and activation. Heart Fail Rev 2005; 10: 15–22.
Shibata S, Nagase M, Yoshida S, Kawarazaki W, Kurihara H, Tanaka H, Miyoshi J, Takai Y, Fujita T . Modification of mineralocorticoid receptor function by Rac1 GTPase: implication in proteinuric kidney disease. Nat Med 2008; 14: 1370–1376.
Duc C, Farman N, Canessa CM, Bonvalet JP, Rossier BC . Cell-specific expression of epithelial sodium channel alpha, beta, and gamma subunits in aldosterone-responsive epithelia from the rat: localization by in situ hybridization and immunocytochemistry. J Cell Biol 1994; 127: 1907–1921.
Nakagaki T, Hirooka Y, Matsukawa R, Nishihara M, Nakano M, Ito K, Hoka S, Sunagawa K . Activation of mineralocorticoid receptors in the rostral ventrolateral medulla is involved in hypertensive mechanisms in stroke-prone spontaneously hypertensive rats. Hypertens Res 2012; 35: 470–476.
Kumar NN, Goodchild AK, Li Q, Pilowsky PM . An aldosterone-related system in the ventrolateral medulla oblongata of spontaneously hypertensive and wistar-kyoto rats. Clin Exp Pharmacol Physiol 2006; 33: 71–75.
Amin MS, Reza E, Wang H, Leenen FH . Sodium transport in the choroid plexus and salt-sensitive hypertension. Hypertension 2009; 54: 860–867.
Kolla V, Litwack G . Transcriptional regulation of the human Na/K ATPase via the human mineralocorticoid receptor. Mol Cell Biochem 2000; 204: 35–40.
Acknowledgements
We express our sincere thanks to Naomi Shirouzu for help with the western blot analysis. This study was supported by the Grants-in-Aid for Scientific Research from the Japan Society for Promotion of Science (23220013, 24390198) and, in part, a Grant from the Salt Science Research Foundation (1233).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Nakano, M., Hirooka, Y., Matsukawa, R. et al. Mineralocorticoid receptors/epithelial Na+ channels in the choroid plexus are involved in hypertensive mechanisms in stroke-prone spontaneously hypertensive rats. Hypertens Res 36, 277–284 (2013). https://doi.org/10.1038/hr.2012.174
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/hr.2012.174
Keywords
This article is cited by
-
Cycle-dependent sex differences in expression of membrane proteins involved in cerebrospinal fluid secretion at rat choroid plexus
BMC Neuroscience (2023)
-
Review of the health benefits of habitual consumption of miso soup: focus on the effects on sympathetic nerve activity, blood pressure, and heart rate
Environmental Health and Preventive Medicine (2020)
-
Brain perivascular macrophages contribute to the development of hypertension in stroke-prone spontaneously hypertensive rats via sympathetic activation
Hypertension Research (2020)
-
The Role of CNS in the Effects of Salt on Blood Pressure
Current Hypertension Reports (2016)
-
Role of hypothalamic angiotensin type 1 receptors in pressure overload-induced mineralocorticoid receptor activation and salt-induced sympathoexcitation
Hypertension Research (2013)