Abstract
Thiazide-type diuretics are the most commonly used blood pressure (BP)-lowering drug for patients with uncomplicated hypertension. However, it has remained unclear whether hydrochlorothiazide (HCTZ) or chlorthalidone (CTD) shows better improvement in central aortic pressure. We conducted an open-label, randomized, prospective cross-over study with an 8-week active treatment (HCTZ of 25 mg with candesartan of 8 mg or CTD of 12.5 mg with candesartan of 8 mg) with a 4-week washout period (only candesartan during this period). Twenty-eight treatment-naïve patients of hypertension were enrolled (mean age: 50±9 years, male: 44.4%). Central aortic pressure, pulse wave velocity (PWV), augmentation index (AIx) and other BP-derived parameters were measured. After 8 weeks of active treatment, there was no significant difference in changes of central aortic pressure between HCTZ and CTD treatments (Δ=−14±8 vs. −16±7 mm Hg, P=0.645). However, CTD treatment showed a significant reduction in PWV compared with baseline (1321±194 vs. 1439±190 cm s−1, P=0.007) and HCTZ treatment (Δ=−118±82 vs. Δ=5±72 cm s−1, P=0.033), whereas HCTZ treatment showed a marginal, but not a significant reduction in AIx compared with baseline. In conclusion, CTD of 12.5 mg is as potent as HCTZ of 25 mg, when combined with candesartan of 8 mg, in lowering central aortic pressure. In addition, CTD treatment resulted in a significant reduction of PWV.
Similar content being viewed by others
Introduction
Although thiazide-type diuretics are a favored initial treatment option for patients with uncomplicated hypertension, the Seventh Report of the Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure (JNC-7) guideline does not specify which drug from this class is preferred.1 Among thiazide-type diuretics, hydrochlorothiazide (HCTZ) in a daily dose of 12.5–25 mg has been widely employed as initial therapy for most patients with hypertension, but recently chlorthalidone (CTD) has regained clinical usage as a substitute for HCTZ because of better clinical outcomes and blood pressure (BP)-lowering effects.2, 3
Although CTD and HCTZ are structurally similar compounds, they are quite dissimilar pharmacokinetically. CTD is distinguished from HCTZ in that the former has an extremely long half-life and a very large volume of distribution owing to its extensive partitioning into red blood cells.4 CTD, at half the dose, is more effective in lowering systolic BP (SBP) than HCTZ, mainly because of its BP-lowering efficacy throughout the night time hours.5 Therefore, it is postulated that difference in persistence of BP-lowering efficacy would contribute to differences in central BP and arterial stiffness.
Whether these two drugs have different effects on clinical outcomes remains unclear, but evidence indicates that the benefit of low-dose thiazide-based regimens to reduce cardiovascular events is primarily derived from studies using CTD, whereas HCTZ is inferior to other classes of hypertensive drugs, including angiotensin-converting enzyme inhibitors6 and calcium channel blockers.7 Furthermore, a retrospective comparative analysis demonstrated that CTD reduces cardiovascular events more than HCTZ.3 Therefore, a recent guideline recommended the use of CTD or indapamide in preference to HCTZ.2
The central arterial system serves as a conduit delivering blood to the organs and tissues, and acts as a ‘buffer’ by distending during cardiac ejection to provide an optimal and continuous peripheral blood flow.8 The distending pressure in the large elastic arteries (aorta and carotid artery) is a key determinant of the degenerative changes that characterize accelerated aging and hypertension. In contrast, the muscular peripheral arteries, such as the brachial and the radial ones, are less influenced by these changes.9 Central aortic pressure more accurately reflects loading conditions of the LV myocardium, coronary arteries and cerebral vasculature and, thereby, better relates to target-organ damage and cardiovascular events than brachial pressures.10, 11, 12
The object of the current study was to compare the effect of HCTZ and CTD on central aortic pressure, when combined with candesartan, in treatment-naïve patients of hypertension.
Methods
Study patients
All subjects aged 30–69 years with never-treated hypertension who visited the Outpatient Department of Cardiology at St Paul’s Hospital, Catholic University of Korea, from March 2010 to February 2011 were asked to participate in the study. Hypertension was defined as clinic SBP ⩾140 mm Hg and/or diastolic BP (DBP) ⩾90 mm Hg on ⩾2 different occasions. None of the subjects were knowingly taking any form of antihypertensive drugs. All of the patients were Asians.
Patients were excluded for the following reasons: (1) office BP ⩾180/110 mm Hg; (2) secondary hypertension; (3) hypokalemia (serum potassium <3.5 mEq l−1); (4) hyponatremia (serum sodium <135 mEq l−1); (5) current treatment for congestive heart failure; (6) type 1 or 2 diabetes; (7) renal insufficiency (serum creatinine ⩾2.0 mg dl−1); (8) pregnancy; (9) history of ischemic stroke, unstable angina or myocardial infarction; (10) clinically significant valvular heart disease; (11) chronic atrial fibrillation; (12) known allergy to study medications; (13) severe noncardiovascular disease (for example, cancer or liver cirrhosis); and (14) chronic inflammatory disease.
This study was approved by the institutional review board of the Catholic University and St Paul’s Hospital, and written informed consent was obtained from all of the participants.
Study design
We conducted an open-label, randomized, prospective cross-over study between HCTZ and CTD with an 8-week active treatment with a 4-week washout period (only candesartan during this period). The end points were evaluated in a blinded manner.
Study protocol
Subjects were initially treated with candesartan (8 mg per day) given once daily in the morning for 4 weeks. If clinic SBP and/or DBP exceeded the safety parameters of ⩾180 mm Hg and/or 110 mm Hg, respectively, at any point during the run-in period, patients were withdrawn from the study. After completion of a run-in period, eligible patients were randomized to add either HCTZ (25 mg per day) or CTD (12.5 mg per day) to the candesartan. Patient randomization and allocation to treatment was performed using the envelope method by a researcher who was not involved in any other aspect of the study and blinded to the study procedure. The doses of HCTZ and CTD that were selected for the study were based on a previous review of the literature, which suggested that CTD is approximately two times as potent as HCTZ.5, 13 Both treatments were given as a fixed dose for 8 weeks, and dose titration was not permitted, unless BP was <90/60 mm Hg or symptomatic orthostatic hypotension, dizziness and intolerance occurred. Patients were instructed not to take any antihypertensive medication other than study medications. Other drugs that had the potential to interfere with the safety and efficacy of the study medications were also not allowed. At baseline and at the end of the study, central BP and other related parameters were measured. Then, subjects were treated with only candesartan (8 mg per day) during a 4-week washout period and crossed over to the other drug for another 8 weeks. Before and after a second 8-week active treatment period, central BP and other related parameters were measured again.
Assessments
After 10 min of rest in a supine position, the subjects underwent radial applanation tonometry. An electrocardiogram and brachial cuff oscillometric pressure in the right upper arm were measured, with pulse tracings and ECG digitized at 1.2 kHz. Simultaneously, high-fidelity and left radial arterial pressure waveforms were recorded by a separate tonometer system (HEM-9000AI; Omron Healthcare, Kyoto, Japan),14, 15, 16 consisting of a holder to immobilize the wrist, and a 40-element phased-array tonometer fitted within a wrist band and hold-down pressure were optimized by an automated servo motor. One of these 40 sensor elements was selected automatically to obtain the optimal radial pressure waveforms. The signals were digitized at 500 Hz. In addition, an augmentation index (AIx), defined as an increase in pressure from the first systolic shoulder to the peak pressure of the aortic pressure waveform expressed as a percentage of peak pressure, was measured for the indexes of wave reflections.17 Because an AIx is influenced by heart rate (HR), an index normalized for HR 75 per min (AIx@75) was used in accord with the findings of Wilkinson et al.18 All measurements were taken in the sitting position in a quiet, temperature-controlled room (22±1 °C) by a nurse who was not involved in the performance or interpretation of the study. All measurements were made in duplicate unless they differed by >5%, in which case a third reading was taken and the mean values were used in the subsequent analysis.
The following BP-derived parameters were evaluated: (1) pulse pressure (PP) was calculated as the difference between the respective SBP and DBP; (2) mean BP was calculated from the SBP and DBP by adding one-third of PP to DBP; (3) fractional PP was presented as the ratio of PP to mean BP to quantify the relative magnitude of the pulsatile-to-mean aortic pressure;19, 20 (4) the ratio of PP to DBP (pulsatility index) was used as an index of aortic stiffness;19 (5) PP amplification was calculated as the ratio of the brachial PP to the central PP; and (6) rate-pressure product, defined as the product of HR (b.p.m.) and SBP (mm Hg) divided by 102, for the estimation of myocardial oxygen consumption, was calculated.21
Finally, the brachial-ankle pulse wave velocity (PWV), a surrogate of vascular stiffness, was measured with a volume-plethysmographic apparatus (Form/ABI; Colin Company, Komaki, Japan).22 The body mass index was calculated as the weight (kg) divided by the height (m) squared. The estimated glomerular filtration rate was calculated by the Modification of Diet in Renal Disease formula.23
Main outcome measures
The primary outcome was a comparison of changes in central BP from baseline to week 8 between HCTZ and CTD. Secondary outcomes analyzed included a comparison of changes in brachial BP, AIx, PWV and BP-derived parameters between HCTZ and CTD.
Sample size
We assumed a difference of 5 mm Hg in central SBP between the treatment groups, because a difference that large has been demonstrated to have prognostic significance.12 A priori calculations suggested that a sample size of 27 should provide 80% to detect a difference in mean change of ⩾5 mm Hg in central BP between the two treatments at the 0.05 significance level, assuming a standard deviation of 6.5 mm Hg. Total sample size was estimated to be 31 patients for the trial on the expectation of a 10% drop-out rate.
Statistical analyses
Continuous data were expressed as mean±s.d. and compared using an unpaired t-test; categorical data were expressed as number (percentage). The changes of BP and derived parameters from the beginning to the end of the 8-week active treatment period were compared with paired t-tests. Comparisons of change were regarded as primary efficacy variables, and others as secondary efficacy variables not to control the overall significance level in multitesting. A general estimating equation repeated measures analysis was performed to check for order effects of the test (HCTZ first group and HCTZ second group). For all tests, a P-value <0.05 was considered statistically significant. All statistical analyses were performed using SPSS for Windows (SPSS, Chicago, IL, USA), version 15.
Results
Study population and baseline clinical characteristics
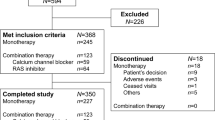
Thirty-two patients fulfilling the inclusion criteria were initially evaluated and underwent random allocations for the study drugs. Of those, four were excluded because two suffered from dizziness and intolerance to the study drugs and the other two had withdrawn the consent form. Finally, of the 28 patients enrolled, 15 were initially allocated to the HCTZ/candesartan treatment and the remaining 13 were allocated to CTD/candesartan treatment. Of course, each group did cross-over to the other treatment combination.
Baseline characteristics of the patients are summarized in Table 1.
Changes of brachial BPs between the two antihypertensive treatment combinations
Patients were categorized into HCTZ/candesartan and CTD/candesartan assignments. After 8 weeks of the active treatment, both treatments achieved significant improvements in brachial SBP, DBP, PP, mean BP and rate-pressure product compared with baseline (Table 2). Only the HCTZ/candesartan treatment showed a significant increase in HR. However, there was no significant difference in changes of brachial BP and BP-derived parameters between the two therapies.
Changes of central BPs between the two antihypertensive treatment combinations
A significant order-drug-time interaction implied the order in which the two drugs were given had a significant effect on differences of the magnitude of change in central SBP between the two drugs. After the planned patients completed both active treatments, an order-drug-time interaction was found not to be significant (P=0.170, data not shown). Moreover, a carryover effect was found not to be significant (P=0.395, data not shown). This ensured that there was an adequate washout period.
After 8 weeks of active treatment, both drug combinations showed significant improvements in central SBP, DBP, PP and mean BP (Table 3). Fractional PP and pulsatility index were marginally reduced with HCTZ/candesartan, but this was not significant. Rate-pressure product was significantly improved with CTD/candesartan treatment compared with baseline. However, there was no significant difference between the two treatment regarding changes in central BP or changes in BP-derived parameters.
Changes in aortic stiffness between the two antihypertensive treatment combinations
After 8 weeks of active treatment, the CTD/candesartan treatment showed a significant reduction in PWV compared with baseline and the HCTZ/candesartan treatment, whereas the HCTZ/candesartan treatment showed a marginal, but nonsignificant, reduction in AIx and AIx@75 compared with baseline (Table 4).
Discussion
The main finding of this study was that changes in central BPs were not significantly different between the HCTZ (25 mg per day) and CTD (12.5 mg per day) treatment combined with candesartan after an 8-week active treatment.
Central BP can be measured invasively by the use of a catheter (fluid-filled or high-fidelity micro-tip pressure transducers), but it has not got widespread use in large epidemiological studies and in daily clinical practice because of technical limitations and high costs. In contrast, noninvasive techniques have provided a great impetus for the spread of central pressure estimation in clinical practice. The application of generalized transfer functions for the indirect estimation of aortic pressure waveforms based on pressure recordings at the radial artery.24 The correspondence between calculated and directly recorded central BP has been found to be within 1 mm Hg.25, 26, 27
Several potential mechanisms could explain the reason why there were no differences in central BPs between HCTZ and CTD treatment in our study. First, it is possible that candesartan might lessen the effect of thiazide-type diuretics. It is known that various antihypertensive drugs have differential effects on central SBP, despite their similar effects on brachial SBP.12, 28, 29, 30, 31, 32 Indeed, inhibitors of the renin-angiotensin system cause a greater fall in central BP.31, 33 However, diuretics are not as effective as vasodilating drugs in reducing central SBP,29, 34 because they poorly modify the microvascular structure.35 Angiotensin receptor blockers are one of the first-line antihypertensive drugs for most patients, but monotherapy achieves the target BP that is recommended by the treatment guidelines36, 37 in only a limited number of patients. Thus, combination therapy is required in a majority of patients.36 A thiazide-type diuretic is commonly used in combination with angiotensin receptor blocker because it has an additive effect on BP reduction due to the complementary mechanisms of action of the components,36 and the efficacy of this combination has been demonstrated in many clinical trials.32, 38, 39 Although we designed a comparison adopting combination drugs rather than diuretics alone to reflect real-world antihypertensive therapy, angiotensin receptor blockers might have attenuated the effect of diuretics on central BP. Second, central aortic pressure is dependent not only on PWV but also on AIx.40 The reduction in PWV and AIx has a significant role in central SBP reduction. Therefore, the different responses of two hemodynamic measurements in our study may explain why the central BPs were not different between HCTZ and CTD treatment. Third, an increase in HR is associated with lower central aortic pressure.12, 28, 31, 34 Our study displayed HR increases in HCTZ treatment, which may cause a potential bias and contribute to an unexpected result. Fourth, a previous study demonstrated that the CTD was more effective in lowering BP during night time hours than HCTZ, but failed to show any difference in office BP and BP during the day time hours.5 Therefore, the measurement of central aortic pressure in day time had an inherent limitation, but measuring central BP during the night time has been unavailable.
Our study has several strengths and implications. First, to our knowledge, our trial is the first study to compare the effect on central BPs between HCTZ and CTD. Our results lend further support to the notion that HCTZ and CTD, using half the dose of HCTZ, present similar BP-lowering efficacy even in central BP.
Second, interestingly, the impact on arterial stiffness between the two treatments displayed different results depending on the evaluation methods. The PWV is likely to be a better measure in older individuals (>50 years) but AIx might be a more sensitive marker in younger individuals (<50 years).41 Taken together, we assume that there is a different response between the HCTZ and CTD according to age in terms of arterial stiffness. Anyway, CTD treatment significantly reduced PWV compared with baseline and HCTZ, whereas HCTZ shows a trend toward reduction of AIx.
The increased arterial stiffness is believed to originate from a medial calcification,42 and a correlation between PWV and large artery calcification has been shown.43 Thiazide-like diuretic is known to inhibit carbonic anhydrase, the major source of protons used by osteoclasts, resulting in inhibition of medial calcification,44 and CTD more potently inhibits carbonic anhydrase than HCTZ.45 Therefore, this may explain a greater decline in PWV during CTD treatment. Vascular stiffness may better summate chronic damage to blood vessels from aging, hypertension and diabetes than brachial or even central BP.11 PWV has been related to cardiovascular risk in hypertensive patients,46 the elderly,47 patients with end-stage renal disease48 and population-based samples.49 Therefore, better reduction in PWV than HCTZ may contribute to decrease in cardiovascular events.
The beneficial effect on AIx in the HCTZ treatment can be explained, at least in part, by a substantial increase in HR. HR is an independent determinant of AIx and an increase in HR can result in a decrease in AIx.18 However, AIx@75 that is independent of the HR influence also showed a marginal decrease in our study.
Third, there are only a few fixed-dose antihypertensive combinations that contain CTD, whereas HCTZ combo drugs are abundant.4 Because CTD treatment causes similar reductions in central aortic pressure and peripheral BP with half the dose of HCTZ, manufacturing fixed-dose combinations containing CTD should be more prevalent.
There are limitations to our study. First, although the power calculation was based on anticipated central pressure difference, the study population was too small to detect significant difference in central BP, given the large s.d. Based on our results, over 500 subjects would be needed to show a superiority of CTD in reduction in central BP. Second, the study period was relatively short. It is important to evaluate longer-term treatment to clarify the effect of these combination therapies on central aortic pressure. Third, a potential weakness is that the calibration of central aortic pressures depends on the accuracy of the brachial pressure measurement.50, 51 Forth, we compared only two commonly used doses of each drug, and it is unclear whether no difference in central BPs would persist in other doses. Fifth, this was not a double-blind study. However, the open-label, randomized, prospective cross-over, blinded end-point design is often used, and if it is designed and conducted properly, the results are not thought to be biased.52 Moreover, all of the critical measurements were performed by an investigator who was blinded to treatment allocations. Sixth, pretreatment with angiotensin receptor blocker might create a bias in patient selection. Seventh, the development of hypokalemia, major side effect, was not compared. Eighth, our study population was limited to Asians and results may not be applicable to other populations.
Conclusion
Our study compared the antihypertensive efficacy of usual recommended doses of HCTZ (25 mg per day) and CTD (12.5 mg per day) on central aortic pressure. We found that CTD, at half the dose, is as potent as HCTZ (both combined with candesartan) in lowering central aortic pressure. In addition, CTD resulted in a significant reduction in PWV, whereas HCTZ showed a trend toward reduction of AIx.
References
Chobanian AV, Bakris GL, Black HR, Cushman WC, Green LA, Izzo JL, Jones DW, Materson BJ, Oparil S, Wright JT, Roccella EJ . The Seventh Report of the Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure: the JNC 7 report. JAMA 2003; 289: 2560–2572.
Krause T, Lovibond K, Caulfield M, McCormack T, Williams B . Management of hypertension: summary of NICE guidance. BMJ 2011; 343: d4891.
Dorsch MP, Gillespie BW, Erickson SR, Bleske BE, Weder AB . Chlorthalidone reduces cardiovascular events compared with hydrochlorothiazide: a retrospective cohort analysis. Hypertension 2011; 57: 689–694.
Sica DA . Chlorthalidone: has it always been the best thiazide-type diuretic? Hypertension 2006; 47: 321–322.
Ernst ME, Carter BL, Goerdt CJ, Steffensmeier JJ, Phillips BB, Zimmerman MB, Bergus GR . Comparative antihypertensive effects of hydrochlorothiazide and chlorthalidone on ambulatory and office blood pressure. Hypertension 2006; 47: 352–358.
Wing LM, Reid CM, Ryan P, Beilin LJ, Brown MA, Jennings GL, Johnston CI, McNeil JJ, Macdonald GJ, Marley JE, Morgan TO, West MJ . A comparison of outcomes with angiotensin-converting—enzyme inhibitors and diuretics for hypertension in the elderly. N Engl J Med 2003; 348: 583–592.
Jamerson K, Weber MA, Bakris GL, Dahlof B, Pitt B, Shi V, Hester A, Gupte J, Gatlin M, Velazquez EJ . Benazepril plus amlodipine or hydrochlorothiazide for hypertension in high-risk patients. N Engl J Med 2008; 359: 2417–2428.
O'Rourke M . Mechanical principles in arterial disease. Hypertension 1995; 26: 2–9.
Avolio AP, Chen SG, Wang RP, Zhang CL, Li MF, O'Rourke MF . Effects of aging on changing arterial compliance and left ventricular load in a northern Chinese urban community. Circulation 1983; 68: 50–58.
Pini R, Cavallini MC, Palmieri V, Marchionni N, Di Bari M, Devereux RB, Masotti G, Roman MJ . Central but not brachial blood pressure predicts cardiovascular events in an unselected geriatric population: the ICARe Dicomano Study. J Am Coll Cardiol 2008; 51: 2432–2439.
Roman MJ, Devereux RB, Kizer JR, Lee ET, Galloway JM, Ali T, Umans JG, Howard BV . Central pressure more strongly relates to vascular disease and outcome than does brachial pressure: the Strong Heart Study. Hypertension 2007; 50: 197–203.
Williams B, Lacy PS, Thom SM, Cruickshank K, Stanton A, Collier D, Hughes AD, Thurston H, O'Rourke M . Differential impact of blood pressure-lowering drugs on central aortic pressure and clinical outcomes: principal results of the Conduit Artery Function Evaluation (CAFE) study. Circulation 2006; 113: 1213–1225.
Carter BL, Ernst ME, Cohen JD . Hydrochlorothiazide versus chlorthalidone: evidence supporting their interchangeability. Hypertension 2004; 43: 4–9.
Hashimoto J, Watabe D, Hatanaka R, Hanasawa T, Metoki H, Asayama K, Ohkubo T, Totsune K, Imai Y . Enhanced radial late systolic pressure augmentation in hypertensive patients with left ventricular hypertrophy. Am J Hypertens 2006; 19: 27–32.
Kohara K, Tabara Y, Oshiumi A, Miyawaki Y, Kobayashi T, Miki T . Radial augmentation index: a useful and easily obtainable parameter for vascular aging. Am J Hypertens 2005; 18: 11S–14S.
Iketani T, Iketani Y, Takazawa K, Yamashina A . The influence of the peripheral reflection wave on left ventricular hypertrophy in patients with essential hypertension. Hypertens Res 2000; 23: 451–458.
Nichols WW . Clinical measurement of arterial stiffness obtained from noninvasive pressure waveforms. Am J Hypertens 2005; 18: 3S–10S.
Wilkinson IB, MacCallum H, Flint L, Cockcroft JR, Newby DE, Webb DJ . The influence of heart rate on augmentation index and central arterial pressure in humans. J Physiol 2000; 525: 263–270.
Lu TM, Hsu NW, Chen YH, Lee WS, Wu CC, Ding YA, Chang MS, Lin SJ . Pulsatility of ascending aorta and restenosis after coronary angioplasty in patients >60 years of age with stable angina pectoris. Am J Cardiol 2001; 88: 964–968.
Nakayama Y, Tsumura K, Yamashita N, Yoshimaru K, Hayashi T . Pulsatility of ascending aortic pressure waveform is a powerful predictor of restenosis after percutaneous transluminal coronary angioplasty. Circulation 2000; 101: 470–472.
Rooke GA, Feigl EO . Work as a correlate of canine left ventricular oxygen consumption, and the problem of catecholamine oxygen wasting. Circ Res 1982; 50: 273–286.
Yamashina A, Tomiyama H, Takeda K, Tsuda H, Arai T, Hirose K, Koji Y, Hori S, Yamamoto Y . Validity, reproducibility, and clinical significance of noninvasive brachial-ankle pulse wave velocity measurement. Hypertens Res 2002; 25: 359–364.
Levey AS, Bosch JP, Lewis JB, Greene T, Rogers N, Roth D . A more accurate method to estimate glomerular filtration rate from serum creatinine: a new prediction equation. Modification of Diet in Renal Disease Study Group. Ann Intern Med 1999; 130: 461–470.
Karamanoglu M, O'Rourke MF, Avolio AP, Kelly RP . An analysis of the relationship between central aortic and peripheral upper limb pressure waves in man. Eur Heart J 1993; 14: 160–167.
Hope SA, Meredith IT, Cameron JD . Effect of non-invasive calibration of radial waveforms on error in transfer-function-derived central aortic waveform characteristics. Clin Sci 2004; 107: 205–211.
Gallagher D, Adji A, O'Rourke MF . Validation of the transfer function technique for generating central from peripheral upper limb pressure waveform. Am J Hypertens 2004; 17: 1059–1067.
Pauca AL, O'Rourke MF, Kon ND . Prospective evaluation of a method for estimating ascending aortic pressure from the radial artery pressure waveform. Hypertension 2001; 38: 932–937.
Dhakam Z, Yasmin, McEniery CM, Burton T, Brown MJ, Wilkinson IB . A comparison of atenolol and nebivolol in isolated systolic hypertension. J Hypertens 2008; 26: 351–356.
Jiang XJ, O'Rourke MF, Zhang YQ, He XY, Liu LS . Superior effect of an angiotensin-converting enzyme inhibitor over a diuretic for reducing aortic systolic pressure. J Hypertens 2007; 25: 1095–1099.
Agabiti-Rosei E, Mancia G, O'Rourke MF, Roman MJ, Safar ME, Smulyan H, Wang JG, Wilkinson IB, Williams B, Vlachopoulos C . Central blood pressure measurements and antihypertensive therapy: a consensus document. Hypertension 2007; 50: 154–160.
Dhakam Z, McEniery CM, Yasmin, Cockcroft JR, Brown MJ, Wilkinson IB . Atenolol and eprosartan: differential effects on central blood pressure and aortic pulse wave velocity. Am J Hypertens 2006; 19: 214–219.
London GM, Asmar RG, O'Rourke MF, Safar ME . Mechanism(s) of selective systolic blood pressure reduction after a low-dose combination of perindopril/indapamide in hypertensive subjects: comparison with atenolol. J Am Coll Cardiol 2004; 43: 92–99.
Hirata K, Vlachopoulos C, Adji A, O'Rourke MF . Benefits from angiotensin-converting enzyme inhibitor 'beyond blood pressure lowering': beyond blood pressure or beyond the brachial artery? J Hypertens 2005; 23: 551–556.
Deary AJ, Schumann AL, Murfet H, Haydock S, Foo RS, Brown MJ . Influence of drugs and gender on the arterial pulse wave and natriuretic peptide secretion in untreated patients with essential hypertension. Clin Sci 2002; 103: 493–499.
Agabiti-Rosei E, Heagerty AM, Rizzoni D . Effects of antihypertensive treatment on small artery remodelling. J Hypertens 2009; 27: 1107–1114.
Mancia G, De Backer G, Dominiczak A, Cifkova R, Fagard R, Germano G, Grassi G, Heagerty AM, Kjeldsen SE, Laurent S, Narkiewicz K, Ruilope L, Rynkiewicz A, Schmieder RE, Boudier HA, Zanchetti A, Vahanian A, Camm J, De Caterina R, Dean V, Dickstein K, Filippatos G, Funck-Brentano C, Hellemans I, Kristensen SD, McGregor K, Sechtem U, Silber S, Tendera M, Widimsky P, Zamorano JL, Erdine S, Kiowski W, Agabiti-Rosei E, Ambrosioni E, Lindholm LH, Viigimaa M, Adamopoulos S, Bertomeu V, Clement D, Farsang C, Gaita D, Lip G, Mallion JM, Manolis AJ, Nilsson PM, O’Brien E, Ponikowski P, Redon J, Ruschitzka F, Tamargo J, van Zwieten P, Waeber B, Williams B . 2007 Guidelines for the management of arterial hypertension: the task force for the management of arterial hypertension of the European Society of Hypertension (ESH) and of the European Society of Cardiology (ESC). J Hypertens 2007; 25: 1105–1187.
Chobanian AV, Bakris GL, Black HR, Cushman WC, Green LA, Izzo JL, Jones DW, Materson BJ, Oparil S, Wright JT, Roccella EJ . Seventh report of the Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure. Hypertension 2003; 42: 1206–1252.
Dahlof B, Devereux RB, Kjeldsen SE, Julius S, Beevers G, de Faire U, Fyhrquist F, Ibsen H, Kristiansson K, Lederballe-Pedersen O, Lindholm LH, Nieminen MS, Omvik P, Oparil S, Wedel H . Cardiovascular morbidity and mortality in the Losartan Intervention For Endpoint reduction in hypertension study (LIFE): a randomised trial against atenolol. Lancet 2002; 359: 995–1003.
PROGRESS Collaborative Group. Randomised trial of a perindopril-based blood-pressure-lowering regimen among 6105 individuals with previous stroke or transient ischaemic attack. Lancet 2001; 358: 1033–1041.
Dart AM, Gatzka CD, Kingwell BA, Willson K, Cameron JD, Liang YL, Berry KL, Wing LM, Reid CM, Ryan P, Beilin LJ, Jennings GL, Johnston CI, McNeil JJ, Macdonald GJ, Morgan TO, West MJ . Brachial blood pressure but not carotid arterial waveforms predict cardiovascular events in elderly female hypertensives. Hypertension 2006; 47: 785–790.
McEniery CM, Yasmin, Hall IR, Qasem A, Wilkinson IB, Cockcroft JR . Normal vascular aging: differential effects on wave reflection and aortic pulse wave velocity: the Anglo-Cardiff Collaborative Trial (ACCT). J Am Coll Cardiol 2005; 46: 1753–1760.
Dao HH, Essalihi R, Bouvet C, Moreau P . Evolution and modulation of age-related medial elastocalcinosis: impact on large artery stiffness and isolated systolic hypertension. Cardiovasc Res 2005; 66: 307–317.
Essalihi R, Dao HH, Yamaguchi N, Moreau P . A new model of isolated systolic hypertension induced by chronic warfarin and vitamin K1 treatment. Am J Hypertens 2003; 16: 103–110.
Teitelbaum SL . Bone resorption by osteoclasts. Science 2000; 289: 1504–1508.
Woodman R, Brown C, Lockette W . Chlorthalidone decreases platelet aggregation and vascular permeability and promotes angiogenesis. Hypertension 2010; 56: 463–470.
Boutouyrie P, Bussy C, Lacolley P, Girerd X, Laloux B, Laurent S . Association between local pulse pressure, mean blood pressure, and large-artery remodeling. Circulation 1999; 100: 1387–1393.
Waddell TK, Dart AM, Medley TL, Cameron JD, Kingwell BA . Carotid pressure is a better predictor of coronary artery disease severity than brachial pressure. Hypertension 2001; 38: 927–931.
Nurnberger J, Keflioglu-Scheiber A, Opazo Saez AM, Wenzel RR, Philipp T, Schafers RF . Augmentation index is associated with cardiovascular risk. J Hypertens 2002; 20: 2407–2414.
Hayashi T, Nakayama Y, Tsumura K, Yoshimaru K, Ueda H . Reflection in the arterial system and the risk of coronary heart disease. Am J Hypertens 2002; 15: 405–409.
Davies JI, Band MM, Pringle S, Ogston S, Struthers AD . Peripheral blood pressure measurement is as good as applanation tonometry at predicting ascending aortic blood pressure. J Hypertens 2003; 21: 571–576.
Cloud GC, Rajkumar C, Kooner J, Cooke J, Bulpitt CJ . Estimation of central aortic pressure by SphygmoCor requires intra-arterial peripheral pressures. Clin Sci (Lond) 2003; 105: 219–225.
Kohro T, Yamazaki T . Cardiovascular clinical trials in Japan and controversies regarding prospective randomized open-label blinded end-point design. Hypertens Res 2009; 32: 109–114.
Acknowledgements
This research received no specific grant from any funding agency in the public, commercial or not-for-profit sectors. The statistical analyses were advised by the Department of Biostatistics, College of Medicine, The Catholic University of Korea.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kwon, BJ., Jang, SW., Choi, KY. et al. Comparison of the efficacy between hydrochlorothiazide and chlorthalidone on central aortic pressure when added on to candesartan in treatment-naïve patients of hypertension. Hypertens Res 36, 79–84 (2013). https://doi.org/10.1038/hr.2012.143
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/hr.2012.143
Keywords
This article is cited by
-
Combining angiotensin receptor blockers with chlorthalidone or hydrochlorothiazide – which is the better alternative? A meta-analysis
Systematic Reviews (2020)
-
Comparative efficacy and safety of chlorthalidone and hydrochlorothiazide—meta-analysis
Journal of Human Hypertension (2019)
-
Chlorthalidone, not hydrochlorothiazide, is the right diuretic for comparison
Clinical Hypertension (2018)
-
Comparisons of microvascular and macrovascular changes in aldosteronism-related hypertension and essential hypertension
Scientific Reports (2017)
-
Impact of the augmentation time ratio on direct measurement of central aortic pressure in the presence of coronary artery disease
Hypertension Research (2015)