Abstract
Background
Although anti-VEGF therapy of exudative AMD with bevacizumab and ranibizumab proved efficacious in the majority of patients, CNV activity does not respond to continued treatment after repeated injections in a considerable amount of patients. These are referred to as nonresponders. A change of the drug to bevacizumab or ranibizumab could possibly offer an alternative option for the treatment of nonresponding exudative AMD.
Methods and materials
A total of 138 nonresponders who switched therapy from bevacizumab to ranibizumab (n=114) or vice versa (n=24) were included in a retrospective study. Visual acuity (VA) and foveal thickness before and after the switch of therapy were compared. By means of linear regression analysis, we analyzed possible prognostic factors associated with a favorable outcome for visual acuity.
Results
Linear regression analysis revealed a statistically significant benefit for nonresponders when treatment was changed to a different anti-VEGF drug (bevacizumab or ranibizumab). VA at the time of the switch was positively correlated with a beneficial development of VA after changing the drug. There was no significant correlation with age, macular thickness, number of injections before the switch, or the development of VA under treatment before the switch. Both patients switching to Avastin and Lucentis benefitted without statistically significant differences.
Conclusions
An exchange of bevacizumab with ranibizumab or vice versa should be considered in nonresponders in the treatment of exudative AMD. Further prognostic factors may help to identify patients who might benefit from a switch. These factors should be investigated in further studies.
Similar content being viewed by others
Introduction
Intravitreal injections of anti-VEGF agents are now the standard in the treatment of exudative age-related macular degeneration (AMD).1 Pegaptanib, an aptamer targeting VEGF-A165, was first approved for the treatment of AMD.2 It has been succeeded by two drugs that have been more efficacious: the humanized IgG antibody bevacizumab (Avastin), and ranibizumab (Lucentis), containing only the antigen-binding part of the antibody. Although ranibizumab was presumed to have a better effect, on the basis of a higher affinity to the target VEGF,3 two large head-to-head-studies demonstrated a comparable efficacy of the two drugs in the treatment of exudative AMD.4, 5, 6 Recently, a third drug, aflibercept, has been approved for the treatment of exudative AMD and poses a new therapeutic option.
However, still up to one-fourth of all treated patients do not benefit from intravitreal injections and visual acuity (VA) deteriorates even under treatment. This group has been described as nonresponders. Definitions for nonresponders vary, ranging from morphologic definitions (eg, remaining intra- or subretinal fluid (IRF or SRF) under treatment) to functional outcomes (eg, deterioration of best corrected visual acuity (BCVA) or even a stable BCVA without improvement) or combinations of both. Up to now, there is no consensus, whether and how nonresponders should be treated. Combinations with other treatment forms have been discussed, for example, combination with photodynamic therapy (PDT) or brachytherapy. However, results have not been encouraging in patients with chronic AMD and there is currently no rationale to widely use these combinations in nonresponders.7, 8, 9, 10 Increasing the dose of ranibizumab was efficacious in some patients.11
After the FDA approval of ranibizumab, several groups reported about a switch from bevacizumab to ranibizumab12, 13 and found a comparable effect after the switch, though not only nonresponders were included. Two groups demonstrated a beneficial effect for patients with chronic AMD, switching from ranibizumab to bevacizumab14 and from ranibizumab to aflibercept.15
In our retrospective study, we investigated the outcomes of patients identified as nonresponders switching from ranibizumab to bevacizumab or vice versa. We analyzed if the patients benefitted from the switch and evaluated prognostic factors that were supposed to help in identifying patients who might benefit from a change of the drug.
Materials and methods
Study design
The retrospective study was approved by the local ethics committee of the University of Freiburg, Germany. We obtained written informed consent on the anonymous analysis of clinical data in all patients. The study adhered to the Declaration of Helsinki.
The purpose of the study was to evaluate if patients who did not improve under therapy (nonresponders) with an anti-VEGF (bevacizumab or ranibizumab) agent improved after switching to the other drug, and if factors could be identified, which help to identify patients who might benefit from a switch.
Screening
All patients treated with bevacizumab and ranibizumab at the University Eye Hospital, Freiburg, were identified by a database search for the terms ‘bevacizumab’ and ‘ranibizumab’. These subjects were entered into a database. Inclusion and exclusion criteria were checked for the identified subjects.
Inclusion criteria: patients who have been treated for exudative AMD with at least three consecutive monthly intravitreal injections with an anti-VEGF agent (bevacizumab or ranibizumab) and were unresponsive to treatment (no improvement or deterioration in visual acuity and morphology, ie, stable or increasing sub- or intraretinal fluid (SRF or IRF) as assessed by OCT). Patients switched to three monthly injections of the other agent with the first injection within 100 days after the last injection of the first agent. Exclusion criteria: indication other than AMD, other reasons for deterioration of BCVA (eg, change of lens status during the time of the study, uncontrolled glaucoma), any pre-treatment with intravitreal injections other than anti-VEGF, photodynamic therapy (PDT), or macular surgery, macular hemorrhage involving the fovea during the study, intraocular surgery during the course of the study (eg, cataract surgery). If both eyes fulfilled the inclusion criteria, only the eye that first received treatment was included.
Statistical analysis
We reviewed the medical records and collected data on BCVA and macular thickness from OCT measurements. We entered all intravitreal injections into the database. We assessed the date when bevacizumab was exchanged by ranibizumab or vice versa. The change of visual acuity in EDTRS lines that occurred before and after the switch of treatment was calculated. Central retinal thickness was determined over time. OCT measurements were performed with both the Stratus (Carl Zeiss Meditec, Oberkochen, Germany) and Spectralis (Heidelberg Engineering, Heidelberg, Germany) tomographers.
We compared BCVA in EDTRS lines before and after switch with the paired t-test for each group separately. Change in central retinal thickness was assessed accordingly.
We assessed by means of multiple linear regression analysis, whether age, current treatment (bevacizumab vs ranibizumab), logBCVA before treatment switch or central retinal thickness from the OCT are predictive for a gain in EDTRS lines after a treatment switch. The linear model was additionally adjusted for the OCT device (Stratus vs Spectralis).
Results
Search Results
In the screening, 435 patients were identified. Of those, 138 fulfilled the inclusion criteria, 114 in group 1 (switch from bevacizumab to ranibizumab) and 24 in group 2 (switch from ranibizumab to bevacizumab). Main reasons for exclusion were unsuitable therapy regimen (eg, more than 100 days between switch of anti-VEGF agent, or less than three monthly intravitreal treatments before or after switch), other additional underlying pathologies of the macula (eg, diabetic macular edema, macular pucker), ocular surgery during the time of switch (eg, cataract surgery), pre-treatment with PDT, triamcinolone, or Macugen, or macular hemorrhage in the fovea. VA and OCT data were available for 124 and 107 patients, respectively, in group 1 and all patients in group 2.
The characteristics for both groups are displayed in Table 1. The groups differed significantly in VA and macular thickness in OCT at the time of the switch of medication (P<0.05). However, all other investigated parameters were similar in both groups.
Visual Acuity and macular thickness
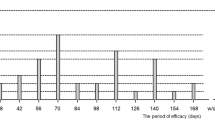
The gain/loss in ETDRS lines before and after the switch for both groups is shown in Figure 1. In group 1, while VA decreases slightly under treatment with bevacizumab, visual acuity improves significantly after the switch to ranibizumab (P<0.001). In group 2, VA decreases slightly under therapy with ranibizumab, and does not improve statistically significantly after switching from ranibizumab to bevacizumab (P=0.52).
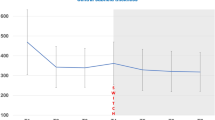
The change of macular thickness before and after the switch is displayed in Figure 2. In group 1, macular thickness decreases significantly after switching from bevacizumab to ranibizumab by a mean of 66 μm (P<0.001). In group 2, there is no statistical difference of macular thickness during the course of the therapy (mean change of 28 μm, P=0.67).
Figure 3 shows the results for visual acuity and macular thickness, when both groups are combined.
Linear Regression Analysis of prognostic factors
Results of the multiple linear regression analysis of prognostic factors are shown in Table 2. Of the included parameters, the VA at the time of switching the anti-VEGF therapy was statistically significantly positively correlated with the VA after the switch. A higher VA before switch was associated with a better outcome for the patient. Gain or loss of letters before the switch was not correlated with the outcome after the switch.
We did not observe a statistically significant association with the group (switch from bevacizumab to ranibizumab or vice versa) and the VA. Our model included the OCT manufacturer to control for a potential calibration bias. Macular thickness before the switch did not exert a statistically significant effect on VA.
Discussion
It is not known, yet, why some patients do not respond to anti-VEGF treatment or develop into nonresponders during the course of the treatment. Tachyphylaxis has been discussed to be important in the development of a resistance to intravitreal injections.16, 17 However, the mechanisms are not clear. In some cases, high doses of ranibizumab (2.0 mg opposed to the regularly used 0.5 mg) could yield a response in patients with persisting SRF or IRF under monthly injections of ranibizumab.11 Genetic variants of the VEGF gene18 seem to alter the response to anti-VEGF treatment. Although both bevacizumab and ranibizumab bind VEGF, minor differences in the binding properties might explain a differential response to different anti-VEGF agents, and might offer the possibility of a response even in patients who developed a tolerance to one drug.
In our study, nonresponders to either bevacizumab or ranibizumab benefitted from a switch to the other drug. Linear regression analysis revealed that VA at the time of the switch of medication was the only prognostic factor (of the ones analyzed) for the development of VA. Patients with a better VA had a better chance of gaining further after the switch. It did not matter if the patients had been treated with bevacizumab or ranibizumab before. This seems to contradict the results from the analysis of the two treatment groups, where a switch to bevacizumab appears to be less likely to end in a benefit for the patient (gain of 0.3 lines after switch to bevacizumab versus gain of 1.3 lines after switch to ranibizumab). However, this contradiction can be explained by the stage of disease at the time of the switch, as patients in group 2 (switch to bevacizumab) had a significantly lower VA and thus, regarding the linear regression analysis, a reduced chance of gaining VA. In addition to the lower VA, central foveal thickness was lower in group 2. Although morphologic data, such as scarring, or presence of SRF or IRF, have not been analyzed separately, this might be explained by a higher rate of patients with already (partially) scarred or fibrotic CNV, resulting in a poorer prognosis.
Visual acuity at the time of switch was identified as a prognostic factor, meaning that a better VA at the time of switch was correlated with a better response after the switch. However, there was no specific threshold in VA indicating a benefit after a switch of treatment. Thus, it is difficult to derive recommendations on the basis of VA in clinical practice. Morphologic parameters and spectral domain OCT have taken the main role for the controlling and management of therapy in responders, and a ‘zero tolerance for fluid’ was proclaimed as target of the therapy.4 However, persisting IRF or SRF under therapy is an attribute of nonresponders and does not help in the decision whether further treatment is advised.
As far as we are aware, this is the first study reporting a considerable (>100 patients) study size of patients estimated as nonresponders switching from bevacizumab to ranibizumab.
The study is limited by its retrospective design. As bevacizumab was available first, this results in a difference between the two study groups, with more patients in the group switching from bevacizumab to ranibizumab than vice versa. In addition, as discussed above, groups differed significantly in the parameters VA and foveal thickness at the time of switch.
Central foveal thickness (as measured by OCT) was the only morphologic parameter chosen for this study. For further studies, additional criteria, such as the presence of intra- or subretinal fluid, pigment epithelium detachment, or subretinal fibrosis, should be added to the analysis.
There are two retrospective studies which reported about the results of patients switching from bevacizumab to ranibizumab, when the latter became available.12, 13 Stepien et al13 observed a similar response after switching to ranibizumab in 84 patients. Karagiannis et al12 observed a transient decrease in VA and increase in macular thickness, interpreted as a transient ‘instability’ after switching to ranibizumab. Three of the included 34 patients developed a significant macular hemorrhage after switching to ranibizumab. However, both studies included patients not regarded as nonresponders, and response after switching to ranibizumab was to be expected.
Almony et al14 observed a beneficial effect of switching from ranibizumab to bevacizumab in 50 nonresponders. A failing response to ranibizumab was defined as no improvement in VA and no improvement in subretinal fluid in fluorescein angiography and OCT. After the switch, patients gained a mean of 0.3 lines, comparable with group 2 in our study, although results varied from a loss of two lines to a gain of four lines among the included patients.
Gasperini et al16 reported on 26 nonresponders, defined as no improvement in sub- or intraretinal fluid, or pigment epithelium detachment. Eight of ten patients responded (ie, total or partial resolution of fluid in OCT) after switching to ranibizumab. Thirteen of sixteen eyes responded after switching from ranibizumab to bevacizumab.
Kumar et al15 reported a significant improvement in visual and anatomical outcomes in 34 eyes with persistent subfoveal fluid formerly treated with ranibizumab after switching therapy to aflibercept.
None of the aforementioned studies evaluated prognostic factors for patients who might benefit from a switch of anti-VEGF drugs.
Clinical management of nonresponders to anti-VEGF therapy is challenging for the patient and the physician. Different options have been proposed in case of a failing response to treatment. However, there is still no common sense as to what would be the best option for the individual. In our study, a significant proportion of patients classified as nonresponders benefitted from a switch of the anti-VEGF drug (bevacizumab or ranibizumab). Thus, a switch of therapy to another anti-VEGF drug should be considered in nonresponders. Further morphologic criteria should be investigated in clinical trials to help to identify patients who might benefit from a switch of therapy.

References
Velez-Montoya R, Oliver SCN, Olson JL, Fine SL, Mandava N, Quiroz-Mercado H . Current knowledge and trends in age-related macular degeneration: today’s and future treatments. Retina 2012; 33 (8): 1487–1502.
Schmidt-Erfurth U, Pollreisz A, Mitsch C, Bolz M . Antivascular Endothelial Growth Factors in Age-Related Macular Degeneration. In: Bandello F, Battaglia Parodi M, Augustin AJ, Iacono P, Schlingemann RO, Schmidt-Erfurth U, (eds). Developments in Ophthalmology. KARGER: Basel, Switzerland, 2010 pp 21–38.
Klettner A, Roider J . Comparison of bevacizumab, ranibizumab, and pegaptanib in vitro: efficiency and possible additional pathways. Invest Ophthalmol Vis Sci 2008; 49 (10): 4523–4527.
CATT Research Group, Martin DF, Maguire MG, Ying GS, Grunwald JE, Fine SL et al. Ranibizumab and bevacizumab for neovascular age-related macular degeneration. N Engl J Med 2011; 364 (20): 1897–1908.
CATT Research Group, Martin DF, Maguire MG, Fine SL, Ying G-S, Jaffe GJ et al. Ranibizumab and bevacizumab for treatment of neovascular age-related macular degeneration: two-year results. Ophthalmology 2012; 119 (7): 1388–1398.
IVAN Study Investigators, Chakravarthy U, Harding SP, Rogers CA, Downes SM, Lotery AJ et al. Ranibizumab versus bevacizumab to treat neovascular age-related macular degeneration: one-year findings from the IVAN randomized trial. Ophthalmology 2012; 119 (7): 1399–1411.
Kaiser PK, Boyer DS, Cruess AF, Slakter JS, Pilz S, Weisberger A et al. Verteporfin plus ranibizumab for choroidal neovascularization in age-related macular degeneration: twelve-month results of the DENALI study. Ophthalmology 2012; 119 (5): 1001–1010.
Larsen M, Schmidt-Erfurth U, Lanzetta P, Wolf S, Simader C, Tokaji E et al. Verteporfin plus ranibizumab for choroidal neovascularization in age-related macular degeneration: twelve-month MONT BLANC study results. Ophthalmology 2012; 119 (5): 992–1000.
Dugel PU, Petrarca R, Bennett M, Barak A, Weinberger D, Nau J et al. Macular epiretinal brachytherapy in treated age-related macular degeneration: MERITAGE study: twelve-month safety and efficacy results. Ophthalmology 2012; 119 (7): 1425–1431.
Petrarca R, Dugel PU, Nau J, Slakter JS, Jaffe GJ, Jackson TL . Macular epiretinal brachytherapy in treated age-related macular degeneration (MERITAGE Study): 12 month optical coherence tomography and fluorescein angiography. Ophthalmology 2012; 120 (2): 328–333.
Brown DM, Chen E, Mariani A, Major JC . Super-dose anti-VEGF (SAVE) trial: 2.0 mg intravitreal ranibizumab for recalcitrant neovascular macular degeneration–primary end point. Ophthalmology 2012; 120 (2): 349–354.
Karagiannis DA, Ladas ID, Parikakis E, Georgalas I, Kotsolis A, Amariotakis G et al. Changing from bevacizumab to ranibizumab in age-related macular degeneration. Is it safe? Clin Interv Aging 2009; 4: 457–461.
Stepien KE, Rosenfeld PJ, Puliafito CA, Feuer W, Shi W, Al-Attar L et al. Comparison of intravitreal bevacizumab followed by ranibizumab for the treatment of neovascular age-related macular degeneration. Retina 2009; 29 (8): 1067–1073.
Almony A, Mansouri A, Shah GK, Blinder KJ . Efficacy of intravitreal bevacizumab after unresponsive treatment with intravitreal ranibizumab. Can J Ophthalmol 2011; 46 (2): 182–185.
Kumar N, Marsiglia M, Mrejen S, AT-C Fung, Slakter J, Sorenson J et al. Visual and anatomical outcomes of intravitreal aflibercept in eyes with persistent subfoveal fluid despite previous treatments with ranibizumab in patients with neovascular age-related macular degeneration. Retina 2013; 33 (8): 1605–1612.
Gasperini JL, Fawzi AA, Khondkaryan A, Lam L, Chong LP, Eliott D et al. Bevacizumab and ranibizumab tachyphylaxis in the treatment of choroidal neovascularisation. Br J Ophthalmol 2012; 96 (1): 14–20.
Binder S . Loss of reactivity in intravitreal anti-VEGF therapy: tachyphylaxis or tolerance? Br J Ophthalmol 2012; 96 (1): 1–2.
Abedi F, Wickremasinghe S, Richardson AJ, Makalic E, Schmidt DF, Sandhu SS et al. Variants in the VEGFA gene and treatment outcome after anti-VEGF treatment for neovascular age-related macular degeneration. Ophthalmology 2013; 120 (1): 115–121.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Ehlken, C., Jungmann, S., Böhringer, D. et al. Switch of anti-VEGF agents is an option for nonresponders in the treatment of AMD. Eye 28, 538–545 (2014). https://doi.org/10.1038/eye.2014.64
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/eye.2014.64
This article is cited by
-
Granzyme B degrades extracellular matrix and promotes inflammation and choroidal neovascularization
Angiogenesis (2024)
-
JP1, a polypeptide specifically targeting integrin αVβ3, ameliorates choroidal neovascularization and diabetic retinopathy in mice
Acta Pharmacologica Sinica (2023)
-
Real-world experience with brolucizumab in neovascular age-related macular degeneration over 2 years: the REBA extension study
Graefe's Archive for Clinical and Experimental Ophthalmology (2023)
-
Biophysical differences in IgG1 Fc-based therapeutics relate to their cellular handling, interaction with FcRn and plasma half-life
Communications Biology (2022)
-
Cost containment by peer prior authorization program for second line treatment in patients with retinal disease
Israel Journal of Health Policy Research (2021)