Abstract
Purpose
To evaluate the disinfectant properties of the three multipurpose contact lens disinfecting solutions available in Iran, against clinical isolates and the standard ISO ATCC strains of Pseudomonas aeruginosaand Staphylococcus aureus, based on the international organization for standardization (ISO) 14729 guidelines.
Methods
Three multipurpose solutions that were tested were ReNu Multiplus, Solo Care Aqua and All-Clean Soft. The test solutions were challenged with clinical isolates and the standard strains of P. aeruginosa(ATCC 9027) and S. aureus(ATCC 6538), based on the ISO Stand-alone procedure for disinfecting products. Solutions were sampled for surviving microorganisms at manufacturer's minimum recommended disinfection time. The number of viable organisms was determined and log reductions calculated.
Results
All of the three test solutions in this study provided a reduction greater than the required mean 3.0 logarithmic reduction against the recommended standard ATCC strains of P. aeruginosaand S. aureus. Antibacterial effectiveness of Solo Care Aqua and All-Clean Soft against clinical isolates of P. aeruginosaand S. aureuswere acceptable based on ISO 14729 Stand-alone test. ReNu MultiPlus showed a minimum acceptable efficacy against the clinical isolate of S. aureus, but did not reduce the clinical isolate by the same amount.
Conclusions
Although the contact lens disinfecting solutions meet/exceed the ISO 14729 Stand-alone primary acceptance criteria for standard strains of P. aeruginosaand S. aureus, their efficacy may be insufficient against clinical isolates of these organisms.
Similar content being viewed by others
Introduction
Worldwide, millions of people use contact lenses as an alternative to spectacles. It has been shown contact lenses wear, especially extended wear, is a major risk factor for microbial keratitis and corneal ulcers.1, 2, 3, 4, 5 Although the incidence rates of contact lens-related microbial keratitis is very low, this complication is an important health concern because a very large population is at risk and because of the potential for poor visual outcome and blindness.6, 7
Investigations have documented that contact lens-related microbial keratitis is most commonly caused by bacteria, such as Pseudomonas aeruginosa and Staphylococcus aureus.8, 9, 10, 11, 12, 13, 14, 15
P. aeruginosa is a Gram-negative bacterium that is commonly found in many environments, including water. It is an opportunistic pathogen and innately resistant to dilute solutions of disinfectants. Also P. aeruginosa keratitis associated with contact lens wear is difficult to treat because P. aeruginosa can display multiple resistance to antibiotics.16, 17, 18 Studies showed that extended wear of soft contact lenses increases the adherence of P. aeruginosa to the epithelial cells of its wearers.19, 20
S. aureus is an aerobic Gram-positive bacterium carried by 50–60% of normal population on the hands, face, nose, and skin as a commensal bacterium, and can readily find access to the eye. Generally, Staphylococcal ocular infection is most likely due to hand-to-eye transfer. One study showed that S. aureus is the most common bacterial cause of contact-lens-induced peripheral ulceration.13
The goal of this laboratory-based study is to evaluate and compare the antibacterial activity of the three multipurpose contact lens disinfecting solutions available in Iran when inoculated with the clinical isolates and standard ATCC strains of P. aeruginosa and S. aureus, based on the ISO 14729 Stand-alone procedure for disinfecting products.
The ISO 14729 guidelines are the used standard in industry to demonstrate the activities of contact lens disinfecting solutions against microorganisms. According to this guidelines for Stand-alone primary criteria, an active contact lens disinfecting solution must be able to reduce the viability of starting concentration of bacterial species (S. aureus, Serratia marcescens, P. aeruginosa) by 3 log (99.9%) and fungal species (Fusarium solani and Candida albicans) by 1 log (90%) at minimum disinfecting time as specified according to the manufacturer's label.21, 22
Materials and methods
Test solutions
Three multipurpose lens care solutions commercially available in the Iranian market, namely ReNu Multiplus (Bausch & Lomb, Rochester, NY, USA), Solo Care Aqua (CIBA Vision, Duluth, GA, USA), and All-Clean Soft (Avizor, Spain) were evaluated. 0.9% normal saline was used as control solution. The formulation and recommended disinfection times for test solutions are shown in Table 1. Three lots of each disinfectant and triplicate samples from each lot were tested. Products were within expiration dating and were tested according to manufacturer's labeled instructions for minimum disinfection time.
Test microorganisms
The test microorganisms included the ISO standards and clinical isolation of P. aeruginosa and S. aureus. The standard strains were obtained from Iranian Research Organization for Science & Technology provided from the American Type Culture Collection (ATCC) and included P. aeruginosa (ATCC 9027) and S. aureus (ATCC 6538). Clinical isolates of these organisms were obtained from asymptomatic contact lens wearers after handling. All of the bacterial strains were grown for 18–24 h on tryptone soya agar (TSA) at 30–35 °C and then collected, using a procedure based on the ISO 14729 standards. The inocula were centrifuged and suspended in normal saline and adjusted to have final concentration of 1.0 × 107–1.0 × 108 colony-forming units per milliliter (CFU/ml)
Test procedure
Test methods were based on the procedures described in ISO 14729 Stand-alone acceptance primary criteria. Growth conditions were as described previously. According to this test method, 0.1 ml of 1.0 × 107 CFU/ml test organisms suspension was added to 10 ml of each test solution. Then, the test solutions were mixed to disperse evenly the test organisms. Inoculated test solution was stored at room temperature and sampled for viable microorganisms at the labeled minimum recommended disinfection time. Then 0.1 ml aliquot was taken from each test tube, diluted with Dey–Engley neutralizing broth and permitted to stand at ambient temperature for at least 10–15 min to neutralize the preservative and then plated in TSA and incubated at 30–35 °C for 2 to 4 days for recovering the bacteria. After incubation, the number of surviving test microorganisms was determined and then the mean logarithmic reduction was calculated.21, 22
Results
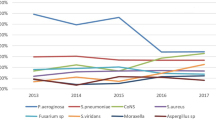
The mean log reduction at the manufacturer's minimum recommended disinfection time for each of the multipurpose solution against all test organisms is reported in Table 2.
Based on the data in Table 1, all test solutions exceeded the required 3.0 log reduction for the recommended standard ATCC strain of P. aeruginosa and S. aureus and, therefore, all solutions met the current ISO Stand-alone primary acceptance criteria for standard type of these organisms.
Similarly, all these solutions achieved the required 3.0 log reduction in bacterial count, when they were tested against the clinical isolate of S. aureus. But, Solo Care and All-Clean had maximum efficacy.
Although there were differences in their efficacy, Solo Care and All-Clean met and exceeded the required 3.0 log reduction for clinical isolate of P. aeruginosa, but ReNu Multi-Plus failed to meet the ISO Stand-alone primary acceptance criteria for this strain (Figure 1).
Discussion and conclusions
In the present study, the ISO Stand-alone test showed differences in susceptibility to three contact lens disinfectants among clinical isolates and laboratory strains of P. aeruginosa and S. aureus.
According to previous studies, one of the test hypotheses was that the clinically isolated would be more resistant than laboratory strains.23, 24, 25, 26, 27, 28 This hypothesis is confirmed by our study.
Therefore, it is clear that the ISO Stand-alone procedure does not ensure disinfectant efficacy during normal use, as demonstrated by the many reports of microbial contamination.29, 30, 31
Although it has been shown that the cleaning and rinsing steps of contact lens care regimen can remove more than 90% of the microbial contaminations from the lenses before the disinfection step,32 non-compliance is very high among contact lens wearers. According to the report of Turner et al,33 30% of contact lens users do not always clean their lenses before disinfection and 44% of them do not wash their hands before handling lenses; this indicates the importance of a good disinfection.
Similar to previous studies,23, 24, 25, 26, 27, 28 the present study showed that the efficacy of a contact lens disinfecting solution is dependent on the type of strains that are used as the challenge organism. Currently clinical strains of microorganisms do not get evaluated by standard test methods. There is a need for developing a new standard protocol for testing contact lens disinfecting solutions. Additionally, despite the use of contact lens disinfecting solution, it is still essential that contact lens wearers are recommended to comply with the manufacturer's labeled instructions for care regimen.

References
Jeng BH, Gritz DC, Kumar AB, Holsclaw DS, Porco TC, Smith SD et al. Epidemiology of ulcerative keratitis in Northern California. Arch Ophthalmol 2010; 128 (8): 1022–1028.
Green M, Apel A, Stapleton F . Risk factors and causative organisms in microbial keratitis. Cornea 2008; 27 (1): 22–27.
Preechawat P, Ratananikom U, Lerdvitayasakul R, Kunovisarut S . Contact lens-related microbial keratitis. J Med Assoc Thai 2007; 90 (4): 737–743.
Dart JKG, Stapleton F, Minassian D . Contact lenses and risk factors in microbial keratitis. Lancet 1991; 338: 650–653.
Dart JKG . Extended wear contact lenses, microbial keratitis, and public health. Lancet 1999; 354: 174–175.
Stapleton F, Keay L, Edwards K, Naduvilath T, Dart JK, Brian G et al. The incidence of contact lens-related microbial keratitis in Australia. Ophthalmology 2008; 115 (10): 1655–1662.
Holden BA, Sweeney DF, Sankaridurg PR, Carnt N, Edwards K, Stretton S et al. Microbial keratitis and vision loss with contact lenses. Eye Contact Lens 2003; 29 (1): S131–S134.
Norina TJ, Raihan S, Bakiah S, Ezanee M, Liza-Sharmini AT, Wan Hazzabah WH . Microbial keratitis: aetiological diagnosis and clinical features in patients admitted to Hospital Universiti Sains Malaysia. Singapore Med J 2008; 49 (1): 67–71.
Willcox MD . Pseudomonas aeruginosa infection and inflammation during contact lens wear: a review. Optom Vis Sci 2007; 84: 273–278.
Verhelst D, Koppen C, van Looveren J, Meheus A, Tassignon MS, the Belgian Keratitis Study Group. Clinical, epidemiological and cost aspects of contact lens related infectious keratitis in Belgium: results of a seven-year retrospective study. Bull Soc Belge Ophtalmol 2005; 7–15.
Schein OD, Ormerod LD, Barraquer E, Alfonso E, Egan KM, Paton BG et al. Microbiology of contact lens-related keratitis. Cornea 1989; 8: 281–285.
Cheng KH, Leung SL, Hoekman HW, Beekhuis WH, Mulder PG, Geerards AJ et al. Incidence of contact-lens-associated microbial keratitis and its related morbidity. Lancet 1999; 354: 181–185.
Jalbert I, Willcox MD, Sweeney DF . Isolation of Staphylococcus aureus from a contact lens at the time of a contact lens-induced peripheral ulcer: case report. Cornea 2000; 19: 116–120.
Wu PZ, Thakur A, Stapleton F, Willcox MD . Staphylococcus aureus causes acute inflammatory episodes in the cornea during contact lens wear. Clin Experiment Ophthalmol 2000; 28: 194–196.
Pachigolla G, Blomquist P, Cavanagh HD . Keratitis pathogens and antibiotic susceptibilities: a 5-year review of cases at an urban county hospital in north Texas. Eye Contact Lens 2007; 33: 45–49.
Chalita MR, Höfling-Lima AL, Paranhos A, Schor P, Belfort R . Shifting trends in in vitro antibiotic susceptibilities for common ocular isolates during a period of 15 years. Am J Ophthalmol 2004; 137: 43–51.
Yeh DL, Stinnett SS, Afshari NA . Analysis of bacterial cultures in infectious keratitis, 1997–2004. Am J Ophthalmol 2006; 142: 1066–1068.
Garg P, Sharma S, Rao GN . Ciprofloxacin-resistant Pseudomonas keratitis. Ophthalmol 1999; 106: 1319–1323.
Ren DH, Petroll WM, Jester JV, Ho-Fan J, Cavanagh HD . The relationship between contact lens oxygen permeability and binding of Pseudomonas aeruginosa to human corneal epithelial cells after overnight and extended wear. CLAO J 1999; 25 (2): 80–100.
Fleiszig S, Efron N, Pier G . Extended contact lens wear enhances Pseudomonas aeruginosa adherence to human corneal epithelium. Invest Ophthalmol Vis Sci 1992; 33 (10): 2908–2916.
International Standards Organization.. ISO 14729 Ophthalmic optics- Contact lens care products- Microbiological requirements and test methods for products and regimens for hygienic management of contact lenses. ISO: Geneva, Switzerland, 2001.
Rosenthal RA, Sutton SW, Schlech BA . Review of standard for evaluating the effectiveness of contact lens disinfectants. PDAJ Pharm Sci Technol 2002; 56 (1): 37–50.
Hume EBH, Flanagan J, Masoudi S, Zhu H, Cole N, Willcox Mark DP . Soft contact lens disinfection solution efficacy: clinical Fusarium isolates vs ATCC 36031. Optom Vis Sci 2009; 86: 415–419.
Hume EBH, Zhu H, Cole N et al. Efficacy of contact lens multipurpose solutions against Serratia marcescens. Optom Vis Sci 2007; 84: 316–320.
Groemminger SF, Norton S . Testing multi-purpose lens care solutions against staphylococcus aureus. Contact Lens Spectrum 2007. Available from [http://www.clspectrum.com/articleViewer.aspx?articleID=13228.].
Imamura Y, Chandra J, Mukherjee PK, Lattif AA, Szczotka-Flynn LB, Pearlman E et al. Fusarium and Candida albicans biofilms on soft contact lenses: model development, influence of lens type, and susceptibility to lens care solutions. Antimicrob Agents Chemother 2008; 52: 171–182.
Fux CA, Shirtliff M, Stoodley P, Costerton JW . Can laboratory reference strains mirror ‘‘real-world’’ pathogenesis? Trends Microbiol 2005; 13: 58–63.
Tsai T, Dannelly HK How Dangerous is Noncompliance with Multipurpose Solutions?http://www.clspectrum.com/articleViewer.aspx?articleID=11758.
Szczotka-Flynn LB, Pearlman E, Ghannoum M . Microbial contamination of contact lenses, lens care solutions, and their accessories: a literature review. Eye Contact Lens 2010; 2: 116–129.
Yung MS, Boost M, Cho P, Yap M . Microbial contamination of contact lenses and lens care accessories of soft contact lens wearers (university students) in Hong Kong. Ophthal Physiol Opt 2007; 27: 11–21.
Donzis PB, Mondino BJ, Weissman BA, Bruckner DA . Microbial contamination of contact lens care systems. Am J Ophthalmol 1987; 104 (4): 325–333.
Edward S, Bennett BAW . Clinical contact lens practice,, 1st edn Lippincott Wilkins and Williams: Philadelphia, 2005.
Turner FD, Gower LA, Stein JM, Sager DP, Amin D . Compliance and contact lens care: A new Assessment method. Optom Vis Sci 1993; 70: 998–1004.
Acknowledgements
We thank all persons in our laboratory for their technical support during the research.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Mohammadinia, M., Rahmani, S., Eslami, G. et al. Contact lens disinfecting solutions antibacterial efficacy: comparison between clinical isolates and the standard ISO ATCC strains of Pseudomonas aeruginosa and Staphylococcus aureus. Eye 26, 327–330 (2012). https://doi.org/10.1038/eye.2011.284
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/eye.2011.284
Keywords
This article is cited by
-
Synergistic antibacterial effects of exopolysaccharides/nickel-nanoparticles composites against multidrug-resistant bacteria
Scientific Reports (2023)
-
ANTIPSEUDOBASE: Database of Antimicrobial Peptides and Essential Oils Against Pseudomonas
International Journal of Peptide Research and Therapeutics (2023)
-
Biofilm inhibiting nanocomposite coatings—a promising alternative to combat surgical site infections
Journal of Coatings Technology and Research (2022)
-
In-vitroanalysis of the microbicidal activity of 6 contact lens care solutions
BMC Infectious Diseases (2012)