Abstract
The failure of β-cells has a central role in the pathogenesis of type 2 diabetes, and the identification of novel approaches to improve functional β-cell mass is essential to prevent/revert the disease. Here we show a critical novel role for thrombospondin 1 (THBS1) in β-cell survival during lipotoxic stress in rat, mouse and human models. THBS1 acts from within the endoplasmic reticulum to activate PERK and NRF2 and induce a protective antioxidant defense response against palmitate. Prolonged palmitate exposure causes THBS1 degradation, oxidative stress, activation of JNK and upregulation of PUMA, culminating in β-cell death. These findings shed light on the mechanisms leading to β-cell failure during metabolic stress and point to THBS1 as an interesting therapeutic target to prevent oxidative stress in type 2 diabetes.
Similar content being viewed by others
Main
The prevalence of diabetes has reached 415 million people worldwide and is projected to affect 642 million by 2040.1 Western diets and sedentary lifestyle are major contributors to the increased prevalence of type 2 diabetes (T2D).2 In non-diabetic individuals, insulin resistance is compensated for by increased insulin secretion. Hyperglycemia develops in individuals who lack this compensatory response.3 Pancreatic β-cell dysfunction is thus central to the development and progression of T2D. In post-mortem studies, β-cell mass is decreased by 40% in T2D patients, probably secondary to increased β-cell apoptosis.4, 5 Why β-cells progressively fail in T2D is not well understood. Prospective studies indicate that increased circulating levels of even-chain saturated free fatty acids (FFAs), of which palmitate is the most common in man, are associated with T2D risk.6, 7 Palmitate affects functional β-cell mass and induces β-cell apoptosis.8
Accumulating evidence suggests that endoplasmic reticulum (ER) and oxidative stress are important mediators of β-cell failure in T2D.9, 10, 11, 12 ER stress develops when the protein load in the ER exceeds the capacity of the organelle to handle proper protein folding. In response, cells activate an adaptive response called the unfolded protein response (UPR) that is governed by the ER transmembrane proteins PKR-like ER kinase (PERK), inositol-requiring enzyme 1 (IRE1) and activating transcription factor 6 (ATF6). PERK attenuates protein translation and promotes expression of transcription factors such as ATF4. Palmitate depletes ER Ca2+ and induces pronounced PERK signaling, leading to the induction of the BH3-only BCL2 proteins PUMA and DP5 and consequently β-cell death.13, 14 Oxidative stress may also contribute to β-cell demise in T2D. Exposure of islets to palmitate increases the generation of reactive oxygen species (ROS) as a consequence of partial uncoupling of oxidative phosphorylation.9 Islets from T2D patients have elevated ROS levels.15
Thrombospondins (THBS) are multimeric Ca2+-binding glycoproteins produced by a large variety of cells. The THBS family consists of five members, of which THBS1 is the best studied. These secreted proteins have a large interactome, and thereby affect a variety of processes, including angiogenesis, platelet aggregation, cell adhesion and migration, wound healing, inflammation and cancer.16 The secreted form of THBS1 is a 450 kDa homotrimeric protein that binds to proteins in the extracellular matrix, such as fibronectin, proteoglycans and integrins.17 THBS1 also binds two membrane receptors, CD47 and CD36. The former has a role in the maintenance of immune tolerance,18 while the latter mediates the antiangiogenic effect of THBS1.19 The vascular density is increased in a range of tissues in THBS1 knockout mice.20 These animals have hypervascular and hyperplastic islets but they are glucose intolerant.21, 22 THBS1 deficiency decreases β-cell glucose-stimulated insulin release, proinsulin biosynthesis and glucose oxidation.21, 23 In these studies, it was suggested that islet endothelial cell-secreted THBS1 modulates β-cell function by activating transforming growth factor β-1 (TGFβ1).
Recently, an important role for intracellular THBS has been identified. In cardiomyocytes, THBS1 and THBS4 favor an adaptive UPR24 by binding to the luminal domain of the ER stress transducer ATF6α and promoting ATF6α nuclear shuttling. THBS thereby upregulates protective chaperones, such as binding immunoglobulin protein (BiP) and protein disulfide isomerase (PDI), and hence improves cardiac ER function and capacity.24
In our previous RNA-sequencing studies, we observed that human islets and autofluorescence-activated cell sorting (FACS)-purified primary rat β-cells abundantly express THBS1.25, 26 We hypothesized that intracellular THBS1 promotes an adaptive UPR and exerts direct β-cell protective effects. Surprisingly, we observed that THBS1 has a different and crucial role in β-cells. It acts as a master regulator of a PERK–NRF2-mediated antioxidant defense response that protects β-cells from lipotoxicity.
Results
ER-resident THBS1 protects β-cells against palmitate
We first examined the role of THBS1 in β-cell survival under lipotoxic conditions using loss- and gain-of-function approaches. THBS1 knockdown by siRNA potentiated palmitate-induced mitochondrial cytochrome c release (Supplementary Figure S1A), caspase-3 cleavage (Figure 1a) and apoptosis (Figure 1b). Similar findings were obtained in dispersed human islet cells, where THBS1 silencing also exacerbated lipotoxicity (Figure 1c and Supplementary Figure S1B). Consistent with these results, islets from THBS1 knockout mice21 were 2.2-fold more sensitive to palmitate compared with wild-type islets (Figure 1d). Conversely, overexpression of THBS1 decreased cytochrome c release, caspase-3 activation and protected INS-1E cells and human islet cells from palmitate (Figures 1e–g and Supplementary Figures S1C and D). THBS1 is synthesized in the ER where it can reside or be secreted, depending on the cell type and Ca2+ levels.27 Most of the intracellular THBS1 co-localized with the ER marker PDI (Supplementary Figure S2A). THBS1 was also detected in the Golgi apparatus but not in the mitochondria (Supplementary Figure S2A). To examine whether secreted THBS1 protects the cells via membrane receptor activation, we used conditioned medium from THBS1-overexpressing INS-1E cells, containing the 450 kDa homotrimeric secreted form of THBS1 (Supplementary Figure S1E). This medium, however, failed to prevent palmitate toxicity (Figure 1h). Exogenously added purified human THBS1 induced early phosphorylation of P38 mitogen-activated protein kinase (P38; Supplementary Figure S1F), as previously shown in other cell types.28 Similar to conditioned medium, however, exogenous THBS1 did not protect β-cells against lipotoxic death when added 24 h before and/or during palmitate exposure (Figure 1i).
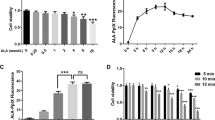
Intracellular THBS1 improves β-cell survival under lipotoxic conditions. (a) THBS1 and cleaved caspase-3 protein expression in INS-1E cells transfected with negative (N, control) or two different THBS1 (T1 and T2) siRNAs and exposed to 0.5 mM palmitate for 16 h (n=3–4). (b) Apoptosis in INS-1E cells transfected and treated as in a (n=3–5). (c) Apoptosis in dispersed human islet cells transfected with negative or THBS1 siRNA and exposed to 0.5 mM palmitate for 24 h (n=4). (d) Cell death in islets from wild-type (THBS1+/+) or THBS1 knockout (THBS1−/−) mice exposed to 0.5 mM palmitate for 48 h (n=4). (e) THBS1 and cleaved caspase-3 protein expression in INS-1E cells infected with luciferase (L, control) or THBS1 (T) adenovirus (ad) and exposed to palmitate for 16 h (n=3–4). (f) Apoptosis in INS-1E cells infected and treated as in e (n=3–5). (g) Apoptosis in dispersed human islet cells infected with luciferase or THBS1 adenovirus and exposed to palmitate for 24 h (n=3). (h) Apoptosis in INS-1E cells exposed for 16 h to palmitate in the presence of conditioned medium from INS-1E cells infected with luciferase or THBS1 adenovirus for 48 h (n=3). (i) Apoptosis in INS-1E cells pretreated or not for 24 h with 2 μg/ml THBS1 and exposed to palmitate plus THBS1 for 16 h (n=3). (j) THBS1 expression in INS-1E cells infected with luciferase, THBS1-FLAG (f) or THBS1-KDEL (k) adenovirus and exposed to palmitate for 16 h (n=3). (k) Apoptosis in INS-1E cells infected and treated as in j (n=3). *P<0.05 against untreated cells transfected with negative siRNA or infected with luciferase adenovirus. #P<0.05 against palmitate-treated cells transfected with negative siRNA or infected with luciferase adenovirus
The role of intracellular THBS1 was further examined using a THBS1 adenovirus containing the ER retention sequence KDEL. The THBS1-KDEL construct induced THBS1 overexpression in the ER as indicated by the co-localization with PDI or SERCA2 (Supplementary Figure S2B). THBS1-KDEL overexpressing cells were similarly protected against palmitate compared with cells overexpressing THBS1-FLAG (Figures 1j and k). These results demonstrate that ER-resident THBS1 is important for β-cell survival in lipotoxic conditions.
Palmitate induces THBS1 degradation
Because lipotoxicity is modulated by THBS1 expression levels, we evaluated whether FFA exposure modifies THBS1 expression. THBS1 mRNA levels were not altered in human islets exposed to palmitate, the monounsaturated FFA oleate or the combination of both FFAs (Supplementary Figure S1G). Palmitate reduced expression of endogenous and adenovirally induced THBS1 mRNA in dispersed human islet cells (Supplementary Figures S1B and D), while it increased THBS1 mRNA levels in INS-1E cells (Supplementary Figure S1H). At the protein level, THBS1 expression was decreased in INS-1E cells and human islets under lipotoxic conditions (Figures 2a and b and Supplementary Figure S2C). Palmitate induces ER stress and consequently attenuates protein translation via PERK-mediated eIF2α phosphorylation.14 To test whether the reduction of THBS1 protein by palmitate might be caused by attenuated protein translation, we measured THBS1 stability after shutdown of protein translation. An 8 h cycloheximide exposure decreased THBS1 expression by 36% (Figure 2c), compared with a reduction by 53% for palmitate (Figure 2a). Salubrinal, a selective inhibitor of eIF2α dephosphorylation that potently inhibits β-cell protein synthesis,29 did not alter THBS1 expression (Figure 2d). We therefore examined whether THBS1 is actively degraded during palmitate exposure. Pharmacological proteasome inhibition by MG132 fully prevented lipotoxic THBS1 downregulation (Figure 2e). Taken together, these results show that palmitate induces THBS1 degradation in the proteasome.
Palmitate decreases THBS1 protein expression in β-cells. (a) Time course analysis of THBS1 protein expression in INS-1E cells exposed to 0.5 mM palmitate (n=3). (b) THBS1 protein expression in human islets exposed to palmitate for 48 h (n=3). (c) THBS1 protein expression in INS-1E cells infected with THBS1 adenovirus and treated with 5 μg/ml cycloheximide for the indicated times (n=3). (d) THBS1 expression and eIF2α phosphorylation in INS-1E cells treated with 75 μM salubrinal for the indicated times (n=3). (e) THBS1 protein expression in INS-1E cells treated with palmitate and 2 μM of the proteasome inhibitor MG132 for the indicated times (n=3)
THBS1 modulates oxidative stress in β-cells
We next characterized the mechanisms of THBS1 cytoprotection. As THBS1 induces an adaptive UPR via activation of ATF6 in cardiomyocytes,24 we examined the ER stress response in β-cells. THBS1 knockdown decreased palmitate-induced expression of genes in the PERK pathway, namely CHOP, ATF4 and ATF3 (Figure 3a). Spliced X-box-binding protein 1 (XBP1s), but not IRE1 phosphorylation or expression, was also reduced by THBS1 silencing in palmitate-treated cells (Figure 3a and Supplementary Figure S3A).
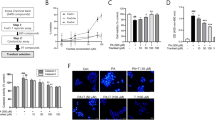
Modulation of ER stress signaling by THBS1. (a) Protein expression of ER stress markers in INS-1E cells transfected with negative (N, control) or two different THBS1 (T1 and T2) siRNAs and exposed or not (CTL) to 0.5 mM palmitate (PAL) for 8 h (n=3). (b) BiP and GRP94 mRNA expression and (c) UPR luciferase reporter activity in INS-1E cells transfected as in a and exposed to palmitate for 16 h (n=3). (d) BiP mRNA expression in pancreatic islets from wild-type (+/+) or THBS1 knockout (−/−) mice (n=5). (e) Protein expression of ER stress markers in INS-1E cells infected with luciferase (L, control) or THBS1 (T) adenovirus (ad) and exposed to palmitate for 16 h (n=3). (f) BiP and GRP94 mRNA expression in INS-1E cells infected and treated as in (e) (n=3). *P<0.05 against untreated cells transfected with negative siRNA or infected with luciferase-expressing adenovirus
ATF6 activation was assessed using an ATF6-GFP construct that upon palmitate exposure is cleaved to the active 77 kDa protein (corresponding to the 50 kDa native ATF6). ATF6 cleavage was decreased in THBS1-deficient cells under lipotoxic conditions (Supplementary Figure S3B). However, this change in ATF6 processing did not alter ATF6 reporter activity (Figure 3c) after palmitate exposure or affect expression of the ATF6 targets BiP or GRP94 (Figures 3a and b). Similarly, islets from THBS1 knockout mice21 have similar BiP expression compared with wild-type islets (Figure 3d).
To further investigate whether THBS1 induces a protective β-cell UPR, we performed the mirror experiment using the THBS1 adenovirus. THBS1 overexpression did not alter palmitate-induced PERK or IRE1 signaling and it did not affect ATF6 activation or downstream targets (Figures 3e and f and Supplementary Figures S3C and D). As THBS1-depleted cells showed reduced ATF6 cleavage in response to palmitate, we assessed whether THBS1-mediated protection is ATF6 dependent. Adenoviral THBS1-FLAG overexpression decreased palmitate toxicity similarly in ATF6-silenced or control β-cells (Supplementary Figures S3E and F). These data suggest that, different from cardiomyocytes, THBS1 does not protect β-cells via promotion of an adaptive UPR.
To determine whether THBS1 has general antiapoptotic properties, we examined other cell death stimuli. THBS1 overexpression protected cells from H2O2 but not from the BCL2/BCL-XL inhibitor ABT-737 or the general kinase inhibitor staurosporin (Figure 4a). These results suggest that THBS1 modulates oxidative stress, a pathway previously implicated in β-cell lipotoxicity.9
THBS1 improves β-cell survival via induction of antioxidant defense enzymes. (a) Apoptosis in INS-1E cells infected with luciferase (Luc, control) or THBS1 adenovirus (ad) and exposed or not (CTL) to 50 μM H2O2, 10 μM ABT-737 (ABT) or 0.2 μM staurosporin (STA) for 16 h (n=3). (b) Oxidative stress measured by DCF oxidation in INS-1E cells transfected with negative (Neg, control) or THBS1 siRNA or infected with luciferase or THBS1 adenovirus and exposed to 0.5 mM palmitate (PAL) for 3 h (n=3). (c) Oxidative stress measured by DCF oxidation in dispersed human islet cells transfected with negative or THBS1 siRNA or infected with luciferase or THBS1 adenovirus and exposed to palmitate for 6 h (n=5). (d) GSTM1, catalase and SOD2 mRNA expression in INS-1E cells transfected with negative (Neg) or THBS1 siRNAs or (e) infected with luciferase or THBS1 adenovirus and exposed to palmitate for 16 h (n=3). (f) GSTM1 and catalase mRNA expression in pancreatic islets isolated from wild-type (+/+) or THBS1 knockout (−/−) mice (n=5). (g) Apoptosis in dispersed rat islet cells transfected with negative or THBS1 siRNA and treated with palmitate and/or 25 μM of the SOD/catalase mimetic MnTMPyP (Mn) for 24 h (n=3). *P<0.05 against untreated cells transfected with negative siRNA or infected with luciferase-expressing adenovirus. #P<0.05 against palmitate-treated cells transfected with negative siRNA or infected with luciferase-expressing adenovirus. §P<0.05 as indicated
To test this hypothesis, we measured ROS using 2',7'-dichlorodihydrofluorescein diacetate, which is converted in the fluorescent form 2',7'-dichlorofluorescein (DCF) upon intracellular oxidation. Palmitate increased the DCF signal by 3-fold; this was augmented by THBS1 knockdown and inhibited by THBS1 overexpression (Figure 4b). Similar results were observed in dispersed human islets (Figure 4c). The cytoplasmic antioxidant enzymes glutathione s-transferase mu 1 (GSTM1) and catalase were upregulated by palmitate (Figure 4d), but this was abolished in THBS1-depleted cells (Figure 4d). Conversely, THBS1 overexpression further upregulated GSTM1 and catalase expression in palmitate-treated cells (Figure 4e). On the other hand, the mitochondrial antioxidant enzyme superoxide dismutase 2 (SOD2) was not modified by palmitate or THBS1 gain or loss of function (Figures 4d and e), suggesting a cell compartment-specific response. THBS1 also modulates oxidative stress in vivo, as GSTM1 was significantly decreased and catalase tended to be lower in THBS1−/− mouse islets (Figure 4f). To test whether oxidative stress mediates lipotoxic cell death in THBS1-deficient conditions, we used the O2− scavenger MnTMPyP. MnTMPyP partially protected rat islet cells from palmitate and abolished THBS1 silencing-mediated apoptosis (Figure 4g). Collectively, these results show that THBS1 protects β-cells from lipotoxicity by coordinating an antioxidative stress response.
THBS1 induces a PERK- and NRF2-dependent antioxidative stress defense
Induction of oxidative or ER stress in β-cells leads to the activation of the transcription factors nuclear factor erythroid-2-related factor-2 (NRF2; ref. 30) and ATF4,31 previously shown to regulate antioxidant enzymes.32, 33 Palmitate transiently increased NRF2 protein expression (Supplementary Figure S4A). NRF2 knockdown induced β-cell apoptosis in basal or palmitate condition (Supplementary Figures S4B and C), whereas ATF4 silencing was cytoprotective (data not shown). Given the proapoptotic role of ATF4, we focused subsequent experiments on NRF2. Neither THBS1 siRNA nor THBS1 overexpression altered NRF2 expression (Figure 5a). We next tested whether prosurvival signals from THBS1 are indeed NRF2-dependent. The cytoprotection from lipotoxicity conferred by THBS1 was lost in NRF2-depleted cells (Figures 5b and c). NRF2 controls the expression of cellular antioxidant and detoxifying enzymes by binding to antioxidant response elements (ARE) in their promoter regions.34 To assess the activation of NRF2 by THBS1, we used the pARE-TI-luciferase reporter.35 Palmitate increased ARE reporter activity by 2-fold. This was abolished by THBS1 knockdown and enhanced in THBS1-overexpressing cells (Figures 5d and e). Supporting the pivotal role of NRF2 in β-cell antioxidative stress defenses, silencing NRF2, but not ATF4, decreased palmitate-induced GSTM1 and catalase mRNA expression (Figures 5f and g). In keeping with this, the potentiation of GSTM1 and catalase expression by THBS1 overexpression was abolished in NRF2-deficient cells, whereas it was preserved in ATF4-deficient cells (Figures 5f and g).
NRF2 mediates the THBS1-induced antioxidative stress response. (a) NRF2 protein expression in INS-1E cells transfected with negative (N, control) or THBS1 (T2) siRNA (si) or infected with luciferase (L) or THBS1 (T) adenovirus (ad) and exposed to 0.5 mM palmitate for 16 h (n=3). (b) THBS1 and NRF2 protein expression in INS-1E cells transfected with negative (Neg) or NRF2 siRNA, infected with luciferase or THBS1 adenovirus and exposed to palmitate for 16 h (n=3). (c) Apoptosis in INS-1E cells transfected, infected and treated as in b (n=3). (d) ARE reporter activity in INS-1E cells transfected with negative or THBS1 siRNA or (e) infected with luciferase or THBS1 adenovirus and exposed to palmitate for 16 h (n=3). (f) THBS1, NRF2 and ATF4 protein expression in INS-1E cells transfected with negative, ATF4 or NRF2 siRNA, infected with luciferase or THBS1 adenovirus and exposed to palmitate for 16 h (n=3). (g) GSTM1 and catalase mRNA expression in INS-1E cells transfected, infected and treated as in (f) (n=3). *P<0.05 against untreated cells transfected with negative siRNA and/or infected with luciferase-expressing adenovirus. #P<0.05 against palmitate-treated cells transfected with negative siRNA and/or infected with luciferase-expressing adenovirus. §P<0.05 as indicated
NRF2 is kept inactive in the cytoplasm by interaction with Kelch ECH associating protein 1 (Keap1). During oxidative stress, Keap1 is modified by ROS and loses affinity for NRF2, allowing its nuclear translocation.36 The NRF2–Keap1 interaction can be also altered by phosphorylation of NRF2. During ER stress, PERK phosphorylates NRF2, leading to its nuclear translocation and target gene activation.37 Consistent with the decreased expression of downstream targets of PERK in THBS1-deficient cells (Figure 3a), palmitate-induced PERK phosphorylation was reduced at early time points (3 and 6 h) by THBS1 knockdown (Figure 6a). Conversely, THBS1 overexpression potentiated PERK phosphorylation after 3 or 6 h of palmitate exposure (Figure 6b). To directly assess the role of PERK in the THBS1–NRF2 pathway, we used the PERK inhibitor GSK2606414.38 PERK inhibition abolished ARE luciferase reporter activity in palmitate-treated THBS1-overexpressing cells (Figures 6c and d) suggesting that PERK activates NRF2 downstream of THBS1. In keeping with these findings, PERK inhibition decreased GSTM1 and catalase mRNA expression in THBS1-overexpressing cells (Figure 6e). These data suggest that THBS1 promotes PERK activation, stimulates NRF2 activity and transcriptionally induces a prosurvival antioxidative response in β-cells.
THBS1 regulates PERK-mediated NRF2 activation. (a) PERK phosphorylation and expression in INS-1E cells transfected with negative (N) or THBS1 (T) siRNA or (b) infected with luciferase (L) or THBS1 (T) adenovirus and exposed to 0.5 mM palmitate for the indicated times (n=3). (c) THBS1 protein expression and PERK phosphorylation in INS-1E cells infected with luciferase or THBS1 adenovirus and exposed to palmitate and/or 0.5 μM of the PERK inhibitor GSK2606414 for 6 h (n=3). (d) ARE reporter assay in INS-1E cells infected with luciferase (Luc) or THBS1 adenovirus and exposed to palmitate and/or 0.5 μM GSK2606414 for 16 h (n=4). (e) GSTM1 and catalase mRNA expression in INS-1E cells infected and treated as in (d) (n=3). *P<0.05 against untreated cells infected with luciferase-expressing adenovirus. #P<0.05 against palmitate-treated cells infected with luciferase adenovirus. §P<0.05 as indicated
Loss of THBS1 expression causes β-cell death via the JNK–PUMA pathway
Palmitate induces THBS1 degradation (Figure 2), which potentiates lipotoxicity through oxidative stress. We next investigated the downstream signals that culminate in β-cell apoptosis. c-Jun N-terminal kinase (JNK) and P38 are activated by oxidative stress in β-cells.39 Palmitate-induced JNK and P38 phosphorylation was enhanced in THBS1-deficient cells (Figure 7a and Supplementary Figure S5A), while THBS1 overexpression reduced both (Figure 7a and Supplementary Figure S5B). Using chemical inhibition, we observed that JNK, but not P38, mediates apoptosis in palmitate-treated THBS1-deficient cells (Figures 7b and c). Of the three known JNK isoforms, JNK1 has been shown to be proapoptotic in β-cells.40 JNK1 knockdown protected cells from apoptosis secondary to THBS1 silencing (Supplementary Figures S5C and D), confirming the results using chemical inhibition.
THBS1 silencing induces apoptosis via JNK-dependent PUMA upregulation. (a) JNK phosphorylation and protein expression in INS-1E cells transfected with negative (N) or two THBS1 (T1 and T2) siRNAs or infected with luciferase (L) or THBS1 (T) adenovirus (ad) and exposed to 0.5 mM palmitate for 3 h (n=3). (b) JNK phosphorylation in INS-1E cells transfected with negative or THBS1 siRNAs and exposed to palmitate and/or 10 μM of the JNK inhibitor SP600125 for 3 h (n=3). (c) Apoptosis in INS-1E cells transfected with negative (Neg) or THBS1 siRNAs and exposed to palmitate and/or 10 μM SP600125 or 10 μM of the P38 inhibitor SB203580 for 16 h (n=3). (d) PUMA mRNA expression in INS-1E cells transfected with negative or THBS1 siRNA and exposed to palmitate for the indicated times (n=4). (e) PUMA mRNA expression in INS-1E cells infected with luciferase or THBS1 adenovirus and exposed to palmitate for the indicated times (n=5). (f) JNK phosphorylation and expression in INS-1E cells transfected with negative or THBS1 siRNA and treated with palmitate or SP600125 for 4 h (n=3). (g) PUMA mRNA expression in INS-1E cells transfected and treated as in g (n=3). (h) Apoptosis in INS-1E cells transfected with negative, DP5, PUMA, BIM or BAD siRNA in combination with THBS1 siRNA and exposed to palmitate for 16 h. Control cells (CTL) were transfected with negative siRNA (n=3). *P<0.05 against untreated cells transfected with negative siRNA. #P<0.05 against palmitate-treated cells transfected with negative siRNA or infected with luciferase adenovirus. §P<0.05 as indicated
Induction of cytochrome c release and activation of caspase-3 (present data) indicate that THBS1 deficiency leads to cell death via the mitochondrial pathway of apoptosis. We next evaluated the involvement of BCL2 family members in the apoptotic process. The antiapoptotic proteins BCL2 or BCL-XL were not modified by THBS1 silencing (Supplementary Figure S6A), but the proapoptotic BH3-only BCL2 family members DP5 and PUMA were upregulated (Figure 7d and Supplementary Figure S6B). In the mirror experiment, THBS1 overexpression attenuated PUMA expression (Figure 7e), but it did not affect BCL2 or DP5 (Supplementary Figures S6C and D). The induction of PUMA by THBS1 depletion was mediated by JNK as it was abolished by chemical JNK inhibition (Figures 7f and g). We next double knocked down THBS1 and all proapoptotic BH3-only BCL2 family members known to contribute to lipotoxic β-cell death.13, 41, 42 PUMA silencing fully protected against THBS1 depletion (Figure 7h), whereas DP5, BIM or BAD knockdown were ineffective (Figure 7h). These results demonstrate that loss of THBS1 expression induces JNK–PUMA-mediated β-cell death.
Discussion
We presently identified a novel function of the ER-resident protein THBS1 as an upstream activator of PERK–NRF2-dependent antioxidative and prosurvival signaling (Figure 8). Our data identify PERK as a new member of the intracellular THBS1 interactome. THBS1 favors PERK phosphorylation and consequently NRF2 activation, thereby equipping β-cells with an effective antioxidative stress defense against lipotoxicity. Prolonged palmitate exposure, however, eventually results in proteasomal THBS1 degradation, loss of antioxidant enzyme expression and β-cell oxidative stress. This leads to JNK activation and PUMA-dependent triggering of the mitochondrial pathway of apoptosis.
THBS1 and THBS4 were previously shown to induce an adaptive UPR in the heart by interacting with ATF6, facilitating its ER-to-Golgi translocation and enhancing the ATF6 transcriptional program.24 Both THBS1 and THBS4 bind to ATF6 via the type 3 repeat domain.24 THBS1 is abundantly expressed in β-cells, but THBS4 is nearly absent (RPKM<0.05; evaluated by RNA sequencing).26 In contrast with the findings in cardiac as well as skeletal myocytes, THBS1 does not promote ATF6 signaling in β-cells. Another interesting difference between β-cells and heart is the subcellular site of action of THBS1. Lynch et al.24 showed that increased ATF6 activation in cardiomyocytes was dependent on THBS translocation to the Golgi, with ER-retained THBS being inactive. In β-cells, ER-resident THBS1 regulates PERK phosphorylation. This points to cell type-specific regulation of ER stress signaling. In keeping with this idea, palmitate induces ATF6 activation and BiP expression in cardiomyocytes,43 whereas it does not induce BiP protein in β-cells.44
Our present findings identify intracellular THBS as a regulator of PERK. Whether THBS1 directly interacts with PERK in the ER and perhaps promotes its oligomerization remains to be examined. Our results show that THBS1 enhances early PERK phosphorylation and prosurvival PERK–NRF2 signaling in β-cells. The data are in keeping with the cardiac gene expression signature of mild PERK activation in THBS4 overexpressing mice.24 PERK phosphorylates NRF2, leading to its nuclear import, maintenance of cellular redox homeostasis and prosurvival signaling.37 Our current data identify palmitate-induced targeting of THBS1 for proteasomal degradation as a mechanism that terminates the early prosurvival signals of PERK. Indeed, prolonged activation of the PERK pathway under lipotoxic conditions is essentially proapoptotic.13, 14, 29 By maintaining THBS1 levels in the ER using adenoviral overexpression, we improved β-cell survival under lipotoxic conditions. THBS1 promotes NRF2 activation and increases expression of the ROS scavenging enzymes GSTM1 and catalase. NRF2 is a master regulator of the oxidative stress response by modulating expression of ARE-containing genes, including enzymes involved in glutathione biosynthesis, H2O2 scavengers and chemical detoxification.45 At variance with the antioxidant response induced by intracellular THBS1, extracellular administration of THBS1 or agonist receptor peptides stimulate ROS production.46
Downstream of palmitate-induced THBS1 degradation and oxidative stress, we identified JNK1-dependent PUMA upregulation as the mediator of β-cell death. These results are in line with studies that demonstrated the pivotal role of PUMA as an apoptosis effector of oxidative stress.47 Islets from T2D patients have significantly higher PUMA mRNA levels.47 The THBS1-dependent inhibition of PUMA makes THBS1 induction an attractive strategy to improve β-cell fate in T2D.
THBS1 is an important therapeutic target in the cancer field due to its potential to restrain angiogenesis and inhibit tumor growth. These effects are essentially mediated extracellularly.48 Extracellular THBS1 has been suggested to have a deleterious role in obesity and insulin resistance, and a recent report identified circulating THBS1 as a biomarker of pre-diabetes.49 THBS1 is more abundantly expressed in visceral compared with subcutaneous fat, and it is increased by high fat feeding and obesity.50, 51 THBS1−/− mice are protected from high-fat-diet-induced obesity and insulin resistance through increased skeletal muscle insulin sensitivity and browning of subcutaneous fat.50 Because these mice have increased serum FFA and triglyceride levels, it was suggested that THBS1 in the adipose interstitial matrix facilitates CD36-mediated FFA uptake.52 Intracellular THBS1 induction rather than extracellular upregulation should therefore be envisaged as a novel therapeutic target in metabolic disease.
In conclusion, we demonstrate that ER-resident THBS1 is an important prosurvival factor in β-cells facing lipotoxic conditions. By promoting PERK-dependent NRF2 activation and consequently upregulating oxidative stress defense enzymes, THBS1 protects β-cells against the deleterious effects of palmitate. This study identifies THBS1 as a protective regulator of ER stress and antioxidant responses in β-cells. The discovery of new agents that induce intracellular THBS1 may be of relevance for the prevention/treatment of T2D.
Materials and Methods
INS-1E cells, FACS-purified primary rat β-cells, mouse islets and human islets
The rat insulin-producing INS-1E cell line (a kind gift from Professor C Wollheim, Centre Medical Universitaire, Geneva, Switzerland) was cultured in RPMI 1640 (with 2 mM GlutaMAX-I) containing 5% FBS53 and used at passages 60–72.
Male Wistar rats (Charles River Laboratories, Brussels, Belgium) were used according to the Belgian Regulations for Animal Care. All the experiments were approved by the local Ethical Committee. Islets were separated by collagenase digestion, handpicked, dispersed in single cells and β-cells purified by FACS (FACSAria, BD Biosciences, San Jose, CA, USA),40 with purity and viability >90%.
Islets from 10–13-week-old THBS1 knockout23 or wild-type mice were used for mRNA expression and cell death studies.
Human islets (from nine donors, age 62±5 years, BMI 25±3 kg/m2, six males and three females, cause of death cerebral hemorrhage (four), cardiovascular disease (three), trauma (one) or unknown (one)) were isolated by collagenase digestion and density gradient purification. The islets were cultured, dispersed and transfected as described.54 The percentage of β-cells, examined by insulin immunofluorescence,14 was 53±7%.
Treatments
For FFA exposure, the INS-1E cells were cultured in medium with 1% FBS and 0.75% FFA-free BSA.55 Palmitate and oleate (Sigma, Schnelldorf, Germany) were dissolved in 90% ethanol, and used at a final concentration of 0.5 mM. Primary rat islet cells were exposed in medium with 0.75% FFA-free BSA, and human islets in medium with 1% charcoal-absorbed BSA. Both the methods result in similar unbound FFA concentrations.55 Cycloheximide, MG132, ABT-737 and staurosporin were dissolved in DMSO and used at the indicated concentrations (Sigma). Salubrinal (ChemBridge, San Diego, CA, USA) was diluted in DMSO and used at 75 μM. H2O2 (Sigma) and MnTMPyP (Alexis Biochemicals, Lausen, Switzerland) were diluted in water. The PERK inhibitor GSK2606414 (a kind gift from William Zuercher, GlaxoSmithKline, Research Triangle Park, NC, USA), the P38 inhibitor SB203580 and the JNK inhibitor SP600125 (Sigma) were dissolved in DMSO. The compounds were added 2 h before palmitate exposure and maintained in the medium together with palmitate. Lyophilized THBS1 (purified from human platelets, Calbiochem, San Diego, CA, USA) was diluted in bidistilled water and used at 2 μg/ml.
RNAi
Proteins were knocked down using specific siRNAs. The siRNAs against DP5, PUMA, BIM, ATF4, BAD and JNK1 were previously validated.13, 41, 56, 57 THBS1 (rat THBS1-1 RSS362499, THBS1-2 RSS362500; human THBS1 RSS362501) and NRF2 siRNAs (NRF2-1 RSS343557, NRF2-2 RSS343558) were from Life Technologies (Carlsbad, CA, USA). ATF6 siRNA (s156439) was from Ambion (Foster City, CA, USA). The negative control of 21 nucleotide duplex RNA (Qiagen, Hilden, Germany) does not affect β-cell function, gene expression or viability.58 Lipid–RNA complexes were formed in 100 μl Optimem1 containing 1 μl Lipofectamine RNAiMAX (Life Technologies) and 150 nM siRNA and added to the cells at a final concentration of 30 nM siRNA.59 The transfected cells were cultured for 2 days before treatment.
Assessment of β-cell apoptosis
Apoptotic cells were counted by fluorescence microscopy after staining with the DNA-binding dyes propidium iodide (5 μg/ml) and Hoechst 33342 (10 μg/ml).29 Apoptosis was confirmed by western blot (see below) for caspase-3 cleavage and by cytochrome c release, as previously described.44
Real-time PCR
Poly(A)+-RNA was isolated and reverse transcribed. The real-time PCR amplification was done using IQ SYBR Green Supermix (Bio-Rad, Hercules, CA, USA) on an MyiQ2 instrument and the PCR product concentration calculated as copies/μl using a standard curve. Gene expression from rat samples was corrected for the reference gene glyceraldehyde-3-phosphate dehydrogenase (GAPDH). β-Actin was used as the reference gene for mouse or human samples. Primer sequences are described in Supplementary Table S1. Gene expression values are shown as fold change of control, except in the mouse islet experiments.
Western blot
Western blots were performed using 20 μg whole-cell extract protein.29 IRE1 phosphorylation was detected using Phos-tag-SDS gels.41 Briefly, the cell lysates were run on SDS-PAGE with 10 μM Phos-tag reagent (Wako, Richmond, VA, USA) and 100 μM MnCl2. The gels were then washed for 30 min in transfer buffer containing 1 mM EDTA and proteins transferred to a nitrocellulose membrane. For THBS1 detection in conditioned medium, INS-1E cells were transfected with adenovirus (see below). After 48 h, the medium was centrifuged at 20 000 × g for 20 min and 6 ml supernatant concentrated to 200 μl using Amicon Ultra Centrifugal Filters (Millipore, Tullagreen, Ireland). Laemmli load buffer (5 ×) was added and the samples were boiled for 5 min. The primary antibodies were anti-p-eIF2α (Ser51), eIF2α, β-actin, BCL2, ATF4, GRP94, COX4, BIM, p-P38 (Thr180/Tyr182), BCL-XL, p-JNK (Thr183, Tyr185), JNK, JNK1, PERK, p-PERK (Thr980), IRE1, BiP, GFP and cleaved caspase-3 from Cell Signaling (Beverly, MA, USA), XBP1, ATF3, CHOP and NRF2 from Santa Cruz Biotechnology (Santa Cruz, CA, USA), FLAG M2 and α-tubulin from Sigma, cytochrome c from BD Biosciences, GAPDH from Trevigen (Gaithersburg, MD, USA) and THBS1 from Thermo Scientific (Rockford, IL, USA). Horseradish peroxidase-labeled donkey anti-rabbit or donkey anti-mouse (1:10 000, Jackson Immuno Research, Baltimore Pike, PA, USA) antibodies were used as secondary antibodies. Protein signal was visualized using chemiluminescence Supersignal (Pierce, Rockford, IL, USA) and quantified using Scion Image (Scion Corporation, Frederick, MD, USA).
Infection with recombinant adenoviruses
The cells were infected either with adLUC (a luciferase-expressing control virus), adTHBS1 (expressing mouse THBS1 protein24), adTHBS1-FLAG (expressing mouse THBS1 protein fused to the FLAG peptide; Sirion Biotech, Planegg, Germany) or adTHBS1-KDEL (expressing mouse THBS1 protein fused to KDEL; Sirion) and used at a multiplicity of infection of 1. After 3 h of infection, the medium was changed and the cells were treated or collected 48 h after infection.
DCF assay
Oxidative stress was measured using the fluorescent probe 2’, 7’-dichlorofluorescein diacetate (DCF; Sigma) in INS-1E cells seeded in 96-well black plates. After treatment, the cells were loaded with 10 μM DCF for 30 min at 37 °C and washed. DCF fluorescence was quantified in Victor 2 reader (PerkinElmer, Walluf, Germany). The cells were then lysed and total protein measured. The data are expressed as DCF fluorescence corrected by total protein.
Plasmids and promoter reporter assay
The ATF6-GFP plasmid60 was from Addgene (32955) and the UPRE luciferase reporter construct was kindly provided by Professor Prywes (Columbia University, New York, NY, USA). The pARE-TI-luciferase reporter (kindly provided by Professor Fahl, University of Wisconsin-Madison, Madison, WI, USA) contains a single copy of the 41-base pair murine GST-Ya ARE and a minimal TATA-Inr promoter. The INS-1E cells were transfected using Lipofectamine 2000 with 250 ng reporter construct and the pRL-CMV plasmid (50 ng, with Renilla used as internal control for transfection efficiency), and 48 h later treated. Luciferase activities of cell lysates were expressed as relative luciferase/Renilla activity.
Immunofluorescence
The INS-1E cells were fixed with 4% formalin, permeabilized with 0.1% Triton, blocked in PBS with 3% goat serum and incubated overnight with antibodies against THBS1 (Thermo Scientific), PDI, HSP60, RCAS1 (Cell Signaling) or SERCA2 (Life Technologies). Following staining with Hoechst 33342 and secondary antibodies conjugated with Alexa fluor 568 or 488 (Life Technologies), the slides were analyzed by inverted fluorescence microscopy (Zeiss Axiovert 200, Oberkochen, Germany) at × 20 magnification and 20 °C. Confocal microscopy was performed in a LSM780 NLO system fitted on an Observer Z1 inverted microscope equipped with an alpha Plan-Apochromat × 63/1.46 oil objective (Zeiss). The 488 nm excitation wavelength of the Argon/2 laser, a main dichroic HFT 488/543 and a band-pass emission filter (BP 500–550 nm) were used for selective detection of the green fluorochrome (Alexa 488). The 543 nm excitation wavelength of the HeNe1 laser, a main dichroic HFT 488/543 and a long-pass emission filter (BP 590–650 nm) were used for selective detection of the red fluorochrome (Alexa 568). A 405 nm blue diode, a main dichroic HFT 405 and a band-pass emission filter (BP 415–465 nm) were used for selective detection of the DNA stain (Hoechst 33342). Images (512 by 512 pixels, zoom factor 4, line average 4; scaling: x-y: 0.066 micron, z: 0.327 micron) were acquired sequentially for each fluorochrome as a z-stack across the thickness of the cell and stored as eight-bits proprietary *.czi files. Single plane images were displayed and analyzed using Zen2012 (Black Edition) software (Zeiss) and exported as eight-bits uncompressed *.TIF images. The figures were prepared using Microsoft Office PowerPoint.
Statistical analysis
The data are presented as means±s.e.m. of the indicated number (n) of independent experiments. The comparisons were performed by analysis of variance followed by paired t-test with the Bonferroni correction for multiple comparisons. A P-value <0.05 was considered statistically significant.
Abbreviations
- ARE:
-
antioxidant response element
- ATF:
-
activating transcription factor
- BiP:
-
binding immunoglobulin protein
- DCF:
-
2’, 7’-dichlorofluorescein diacetate
- ER:
-
endoplasmic reticulum
- FACS:
-
autofluorescence-activated cell sorting
- FFA:
-
free fatty acid
- GAPDH:
-
glyceraldehyde-3-phosphate dehydrogenase
- GSTM1:
-
glutathione s-transferase mu 1
- IRE1:
-
inositol-requiring enzyme 1
- JNK:
-
c-Jun N-terminal kinase
- Keap1:
-
Kelch ECH associating protein 1
- NRF2:
-
nuclear factor erythroid-2-related factor-2
- P38:
-
P38 mitogen-activated protein kinase
- PDI:
-
protein disulfide isomerase
- PERK:
-
PKR-like ER kinase
- ROS:
-
reactive oxygen species
- SOD2:
-
superoxide dismutase 2
- T2D:
-
type 2 diabetes
- THBS:
-
thrombospondin
- UPR:
-
unfolded protein response
- XBP1s:
-
spliced X-box-binding protein 1
References
International Diabetes Federation. IDF_Diabetes_Atlas, 7th edn International Diabetes Federation: Brussels, Belgium, 2015.
Ley SH, Hamdy O, Mohan V, Hu FB . Prevention and management of type 2 diabetes: dietary components and nutritional strategies. Lancet 2014; 383: 1999–2007.
Kahn SE, Cooper ME, Del Prato S . Pathophysiology and treatment of type 2 diabetes: perspectives on the past, present, and future. Lancet 2014; 383: 1068–1083.
Butler AE, Janson J, Bonner-Weir S, Ritzel R, Rizza RA, Butler PC . β-cell deficit and increased β-cell apoptosis in humans with type 2 diabetes. Diabetes 2003; 52: 102–110.
Rahier J, Guiot Y, Goebbels RM, Sempoux C, Henquin JC . Pancreatic β-cell mass in European subjects with type 2 diabetes. Diabetes Obes Metab 2008; 10: 32–42.
Forouhi NG, Koulman A, Sharp SJ, Imamura F, Kroger J, Schulze MB et al. Differences in the prospective association between individual plasma phospholipid saturated fatty acids and incident type 2 diabetes: the EPIC-InterAct case-cohort study. Lancet Diabetes Endocrinol 2014; 2: 810–818.
Wang L, Folsom AR, Zheng ZJ, Pankow JS, Eckfeldt JH . Plasma fatty acid composition and incidence of diabetes in middle-aged adults: the Atherosclerosis Risk in Communities (ARIC) Study. Am J Clin Nutr 2003; 78: 91–98.
Cnop M, Igoillo-Esteve M, Cunha DA, Ladriere L, Eizirik DL . An update on lipotoxic endoplasmic reticulum stress in pancreatic β-cells. Biochem Soc Trans 2008; 36: 909–915.
Carlsson C, Borg LA, Welsh N . Sodium palmitate induces partial mitochondrial uncoupling and reactive oxygen species in rat pancreatic islets in vitro. Endocrinology 1999; 140: 3422–3428.
Sakuraba H, Mizukami H, Yagihashi N, Wada R, Hanyu C, Yagihashi S . Reduced beta-cell mass and expression of oxidative stress-related DNA damage in the islet of Japanese Type II diabetic patients. Diabetologia 2002; 45: 85–96.
Laybutt DR, Preston AM, Akerfeldt MC, Kench JG, Busch AK, Biankin AV et al. Endoplasmic reticulum stress contributes to beta cell apoptosis in type 2 diabetes. Diabetologia 2007; 50: 752–763.
Marchetti P, Bugliani M, Lupi R, Marselli L, Masini M, Boggi U et al. The endoplasmic reticulum in pancreatic beta cells of type 2 diabetes patients. Diabetologia 2007; 50: 2486–2494.
Cunha DA, Igoillo-Esteve M, Gurzov EN, Germano CM, Naamane N, Marhfour I et al. Death protein 5 and p53-upregulated modulator of apoptosis mediate the endoplasmic reticulum stress-mitochondrial dialog triggering lipotoxic rodent and human β-cell apoptosis. Diabetes 2012; 61: 2763–2775.
Cunha DA, Hekerman P, Ladriere L, Bazarra-Castro A, Ortis F, Wakeham MC et al. Initiation and execution of lipotoxic ER stress in pancreatic β-cells. J Cell Sci 2008; 121: 2308–2318.
Marchetti P, Del Guerra S, Marselli L, Lupi R, Masini M, Pollera M et al. Pancreatic islets from type 2 diabetic patients have functional defects and increased apoptosis that are ameliorated by metformin. J Clin Endocrinol Metab 2004; 89: 5535–5541.
Lawler J . Thrombospondin-1 as an endogenous inhibitor of angiogenesis and tumor growth. J Cell Mol Med 2002; 6: 1–12.
Tan K, Lawler J . The interaction of Thrombospondins with extracellular matrix proteins. J Cell Commun Signal 2009; 3: 177–187.
Grimbert P, Bouguermouh S, Baba N, Nakajima T, Allakhverdi Z, Braun D et al. Thrombospondin/CD47 interaction: a pathway to generate regulatory T cells from human CD4+ CD25- T cells in response to inflammation. J Immunol 2006; 177: 3534–3541.
Dawson DW, Pearce SF, Zhong R, Silverstein RL, Frazier WA, Bouck NP . CD36 mediates the in vitro inhibitory effects of thrombospondin-1 on endothelial cells. J Cell Biol 1997; 138: 707–717.
Crawford SE, Stellmach V, Murphy-Ullrich JE, Ribeiro SM, Lawler J, Hynes RO et al. Thrombospondin-1 is a major activator of TGF-beta1 in vivo. Cell 1998; 93: 1159–1170.
Olerud J, Mokhtari D, Johansson M, Christoffersson G, Lawler J, Welsh N et al. Thrombospondin-1: an islet endothelial cell signal of importance for beta-cell function. Diabetes 2011; 60: 1946–1954.
Olerud J, Johansson M, Lawler J, Welsh N, Carlsson PO . Improved vascular engraftment and graft function after inhibition of the angiostatic factor thrombospondin-1 in mouse pancreatic islets. Diabetes 2008; 57: 1870–1877.
Drott CJ, Olerud J, Emanuelsson H, Christoffersson G, Carlsson PO . Sustained beta-cell dysfunction but normalized islet mass in aged thrombospondin-1 deficient mice. PLoS One 2012; 7: e47451.
Lynch JM, Maillet M, Vanhoutte D, Schloemer A, Sargent MA, Blair NS et al. A thrombospondin-dependent pathway for a protective ER stress response. Cell 2012; 149: 1257–1268.
Cnop M, Abdulkarim B, Bottu G, Cunha DA, Igoillo-Esteve M, Masini M et al. RNA sequencing identifies dysregulation of the human pancreatic islet transcriptome by the saturated fatty acid palmitate. Diabetes 2014; 63: 1978–1993.
Villate O, Turatsinze JV, Mascali LG, Grieco FA, Nogueira TC, Cunha DA et al. Nova1 is a master regulator of alternative splicing in pancreatic beta cells. Nucleic Acids Res 2014; 42: 11818–11830.
Veliceasa D, Ivanovic M, Hoepfner FT, Thumbikat P, Volpert OV, Smith ND . Transient potential receptor channel 4 controls thrombospondin-1 secretion and angiogenesis in renal cell carcinoma. Febs J 2007; 274: 6365–6377.
Roberts W, Magwenzi S, Aburima A, Naseem KM . Thrombospondin-1 induces platelet activation through CD36-dependent inhibition of the cAMP/protein kinase A signaling cascade. Blood 2010; 116: 4297–4306.
Cnop M, Ladriere L, Hekerman P, Ortis F, Cardozo AK, Dogusan Z et al. Selective inhibition of eukaryotic translation initiation factor 2α dephosphorylation potentiates fatty acid-induced endoplasmic reticulum stress and causes pancreatic β-cell dysfunction and apoptosis. J Biol Chem 2007; 282: 3989–3997.
Yagishita Y, Fukutomi T, Sugawara A, Kawamura H, Takahashi T, Pi J et al. Nrf2 protects pancreatic beta-cells from oxidative and nitrosative stress in diabetic model mice. Diabetes 2014; 63: 605–618.
Kharroubi I, Ladriere L, Cardozo AK, Dogusan Z, Cnop M, Eizirik DL . Free fatty acids and cytokines induce pancreatic β-cell apoptosis by different mechanisms: role of nuclear factor-κB and endoplasmic reticulum stress. Endocrinology 2004; 145: 5087–5096.
Chanas SA, Jiang Q, McMahon M, McWalter GK, McLellan LI, Elcombe CR et al. Loss of the Nrf2 transcription factor causes a marked reduction in constitutive and inducible expression of the glutathione S-transferase Gsta1, Gsta2, Gstm1, Gstm2, Gstm3 and Gstm4 genes in the livers of male and female mice. Biochem J 2002; 365: 405–416.
Han J, Back SH, Hur J, Lin YH, Gildersleeve R, Shan J et al. ER-stress-induced transcriptional regulation increases protein synthesis leading to cell death. Nat Cell Biol 2013; 15: 481–490.
Venugopal R, Jaiswal AK . Nrf1 and Nrf2 positively and c-Fos and Fra1 negatively regulate the human antioxidant response element-mediated expression of NAD(P)H:quinone oxidoreductase1 gene. Proc Natl Acad Sci USA 1996; 93: 14960–14965.
Wasserman WW, Fahl WE . Functional antioxidant responsive elements. Proc Natl Acad Sci U S A 1997; 94: 5361–5366.
Kansanen E, Kivela AM, Levonen AL . Regulation of Nrf2-dependent gene expression by 15-deoxy-Delta12,14-prostaglandin J2. Free Radic Biol Med 2009; 47: 1310–1317.
Cullinan SB, Zhang D, Hannink M, Arvisais E, Kaufman RJ, Diehl JA . Nrf2 is a direct PERK substrate and effector of PERK-dependent cell survival. Mol Cell Biol 2003; 23: 7198–7209.
Atkins C, Liu Q, Minthorn E, Zhang SY, Figueroa DJ, Moss K et al. Characterization of a novel PERK kinase inhibitor with antitumor and antiangiogenic activity. Cancer Res 2013; 73: 1993–2002.
Kaneto H, Xu G, Fujii N, Kim S, Bonner-Weir S, Weir GC . Involvement of c-Jun N-terminal kinase in oxidative stress-mediated suppression of insulin gene expression. J Biol Chem 2002; 277: 30010–30018.
Marroqui L, Santin I, Dos Santos RS, Marselli L, Marchetti P, Eizirik DL . BACH2, a candidate risk gene for type 1 diabetes, regulates apoptosis in pancreatic beta-cells via JNK1 modulation and crosstalk with the candidate gene PTPN2. Diabetes 2014; 63: 2516–2527.
Cunha DA, Gurzov EN, Naamane N, Ortis F, Cardozo AK, Bugliani M et al. JunB protects beta-cells from lipotoxicity via the XBP1-AKT pathway. Cell Death Differ 2014; 21: 1313–1324.
Nogueira TC, Paula FM, Villate O, Colli ML, Moura RF, Cunha DA et al. GLIS3, a susceptibility gene for type 1 and type 2 diabetes, modulates pancreatic beta cell apoptosis via regulation of a splice variant of the BH3-only protein Bim. PLoS Genet 2013; 9: e1003532.
Zhao Y, Tan Y, Xi S, Li Y, Li C, Cui J et al. A novel mechanism by which SDF-1beta protects cardiac cells from palmitate-induced endoplasmic reticulum stress and apoptosis via CXCR7 and AMPK/p38 MAPK-mediated interleukin-6 generation. Diabetes 2013; 62: 2545–2558.
Cunha DA, Ladriere L, Ortis F, Igoillo-Esteve M, Gurzov EN, Lupi R et al. Glucagon-like peptide-1 agonists protect pancreatic β-cells from lipotoxic endoplasmic reticulum stress through upregulation of BiP and JunB. Diabetes 2009; 58: 2851–2862.
Uruno A, Yagishita Y, Yamamoto M . The Keap1-Nrf2 system and diabetes mellitus. Arch Biochem Biophys 2014; 566: 76–84.
Xing C, Lee S, Kim WJ, Jin G, Yang YG, Ji X et al. Role of oxidative stress and caspase 3 in CD47-mediated neuronal cell death. J Neurochem 2009; 108: 430–436.
Wali JA, Rondas D, McKenzie MD, Zhao Y, Elkerbout L, Fynch S et al. The proapoptotic BH3-only proteins Bim and Puma are downstream of endoplasmic reticulum and mitochondrial oxidative stress in pancreatic islets in response to glucotoxicity. Cell Death Dis 2014; 5: e1124.
Resovi A, Pinessi D, Chiorino G, Taraboletti G . Current understanding of the thrombospondin-1 interactome. Matrix Biol 2014; 37: 83–91.
von Toerne C, Huth C, de Las Heras Gala T, Kronenberg F, Herder C, Koenig W et al. MASP1, THBS1, GPLD1 and ApoA-IV are novel biomarkers associated with prediabetes: the KORA F4 study. Diabetologia 2016; 59: 1882–1892.
Inoue M, Jiang Y, Barnes RH 2nd, Tokunaga M, Martinez-Santibanez G, Geletka L et al. Thrombospondin 1 mediates high-fat diet-induced muscle fibrosis and insulin resistance in male mice. Endocrinology 2013; 154: 4548–4559.
Ramis JM, Franssen-van Hal NL, Kramer E, Llado I, Bouillaud F, Palou A et al. Carboxypeptidase E and thrombospondin-1 are differently expressed in subcutaneous and visceral fat of obese subjects. Cell Mol Life Sci 2002; 59: 1960–1971.
Kong P, Gonzalez-Quesada C, Li N, Cavalera M, Lee DW, Frangogiannis NG . Thrombospondin-1 regulates adiposity and metabolic dysfunction in diet-induced obesity enhancing adipose inflammation and stimulating adipocyte proliferation. Am J Physiol Endocrinol Metab 2014; 305: E439–E450.
Asfari M, Janjic D, Meda P, Li G, Halban PA, Wollheim CB . Establishment of 2-mercaptoethanol-dependent differentiated insulin-secreting cell lines. Endocrinology 1992; 130: 167–178.
Santin I, Moore F, Colli ML, Gurzov EN, Marselli L, Marchetti P et al. PTPN2, a candidate gene for type 1 diabetes, modulates pancreatic beta-cell apoptosis via regulation of the BH3-only protein Bim. Diabetes 2010; 60: 3279–3288.
Oliveira AF, Cunha DA, Ladriere L, Igoillo Esteve M, Bugliani M, Marchetti P et al. In vitro use of free fatty acids bound to albumin: a comparison of protocols. Biotechniques 2015; 58: 228–233.
Gurzov EN, Germano CM, Cunha DA, Ortis F, Vanderwinden JM, Marchetti P et al. p53 up-regulated modulator of apoptosis (PUMA) activation contributes to pancreatic β-cell apoptosis induced by proinflammatory cytokines and endoplasmic reticulum stress. J Biol Chem 2010; 285: 19910–19920.
Santin I, Moore F, Colli ML, Gurzov EN, Marselli L, Marchetti P et al. PTPN2, a candidate gene for type 1 diabetes, modulates pancreatic beta-cell apoptosis via regulation of the BH3-only protein Bim. Diabetes 2011; 60: 3279–3288.
Moore F, Naamane N, Colli ML, Bouckenooghe T, Ortis F, Gurzov EN et al. STAT1 is a master regulator of pancreatic β cell apoptosis and islet inflammation. J Biol Chem 2011; 286: 929–941.
Moore F, Cunha DA, Mulder H, Eizirik DL . Use of RNA interference to investigate cytokine signal transduction in pancreatic β-cells. Methods Mol Biol 2012; 820: 179–194.
Chen X, Shen J, Prywes R . The luminal domain of ATF6 senses endoplasmic reticulum (ER) stress and causes translocation of ATF6 from the ER to the Golgi. J Biol Chem 2002; 277: 13045–13052.
Acknowledgements
We thank Isabelle Millard, Anyishai Musuaya, Nathalie Pachera and Michael Pangerl for expert technical assistance and Laurence Ladriere for assistance with the human islet experiments. This project has received funding from the European Foundation for the Study of Diabetes (EFSD)/Lilly program grant, the European Union’s Horizon 2020 research and innovation program, project T2DSystems, under grant agreement no. 667191, the Fonds National de la Recherche Scientifique (FNRS), and Actions de Recherche Concertées de la Communauté Française (ARC), Belgium. DAC was supported by a FNRS post-doctoral fellowship. J-MV is Research Director at FRS-FNRS.
Author contributions
DAC, DLE and MiC contributed to the original idea and experimental design of the study. DAC, MoC and J-MV carried out the experiments and performed the data analysis. P-OC, JDM, MB and PM contributed materials and data interpretation. DAC and MiC wrote the manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
Edited by V Stambolic
Supplementary Information accompanies this paper on Cell Death and Differentiation website
Rights and permissions
About this article
Cite this article
Cunha, D., Cito, M., Carlsson, PO. et al. Thrombospondin 1 protects pancreatic β-cells from lipotoxicity via the PERK–NRF2 pathway. Cell Death Differ 23, 1995–2006 (2016). https://doi.org/10.1038/cdd.2016.89
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/cdd.2016.89
This article is cited by
-
Endoplasmic reticulum stress contributes to cisplatin-induced chronic kidney disease via the PERK–PKCδ pathway
Cellular and Molecular Life Sciences (2022)
-
Thrombospondin 1 Promotes Endoplasmic Reticulum Stress and Apoptosis in HK-2 Cells by Upregulating ATF6-CHOP
Current Medical Science (2022)
-
Network-based analysis of key regulatory genes implicated in Type 2 Diabetes Mellitus and Recurrent Miscarriages in Turner Syndrome
Scientific Reports (2021)
-
Thbs1 induces lethal cardiac atrophy through PERK-ATF4 regulated autophagy
Nature Communications (2021)
-
The parasite-derived peptide FhHDM-1 activates the PI3K/Akt pathway to prevent cytokine-induced apoptosis of β-cells
Journal of Molecular Medicine (2021)