Abstract
Purpose
Although the burden of illness due to Streptococcus pyogenes is widely recognized, other β-hemolytic streptococci are also important causes of invasive infections. The objective of this study was to compare the population-based epidemiology of groups A, B, and C/G β-hemolytic streptococcal bloodstream infection (BSI).
Methods
Population-based surveillance was conducted in the western interior of British Columbia, Canada, 2011–2018.
Results
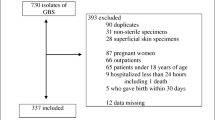
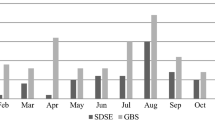
A total of 210 episodes were identified for an incidence of 14.4 per 100,000; the incidences of groups A, B and C/G streptococcal BSI were 4.2, 4.7, and 5.5 per 100,000, respectively. There was an increasing annual incidence of β-hemolytic streptococcal BSI from 2011 through to a peak incidence in 2016 that decreased thereafter. Fifty-two percent (110) of BSIs were community associated, 43% (91) were healthcare associated, and 4% (9) were hospital onset. Patients with group A were younger, more likely to be female, and have fewer co-morbidities than patients with groups B and C/G streptococcal BSI. The most common focus of infection was soft tissue (109/52%), followed by primary (33; 16%), and bone and joint (20; 10%) and these varied by streptococcal species (p < 0.001). The 30-day all-cause case fatality rate was 11% (24/210) and did not significantly vary by group (p = 0.7).
Conclusion
Although the determinants vary, the overall burden of disease related to BSI is similar amongst groups A, B and C/G β-hemolytic streptococci.


Similar content being viewed by others
References
Davies HD, McGeer A, Schwartz B, Green K, Cann D, Simor AE, et al. Invasive group A streptococcal infections in Ontario, Canada. Ontario group A streptococcal study group. N Engl J Med. 1996;335:547–54. https://doi.org/10.1056/nejm199608223350803.
Farley MM, Harvey RC, Stull T, Smith JD, Schuchat A, Wenger JD, et al. A population-based assessment of invasive disease due to group B Streptococcus in nonpregnant adults. N Engl J Med. 1993;328:1807–11. https://doi.org/10.1056/NEJM199306243282503.
Kristensen B, Schonheyder HC. A 13-year survey of bacteraemia due to beta-haemolytic streptococci in a Danish county. J Med Microbiol. 1995;43:63–7. https://doi.org/10.1099/00222615-43-1-63.
Nelson GE, Pondo T, Toews KA, Farley MM, Lindegren ML, Lynfield R, et al. Epidemiology of invasive group A streptococcal infections in the United States, 2005–2012. Clin Infect Dis. 2016;63:478–86. https://doi.org/10.1093/cid/ciw248.
Ballard MS, Schonheyder HC, Knudsen JD, Lyytikainen O, Dryden M, Kennedy KJ, et al. The changing epidemiology of group B streptococcus bloodstream infection: a multi-national population-based assessment. Infect Dis (Lond). 2016;48:386–91. https://doi.org/10.3109/23744235.2015.1131330.
Laupland KB, Ross T, Church DL, Gregson DB. Population-based surveillance of invasive pyogenic streptococcal infection in a large Canadian region. Clin Microbiol Infect. 2006;12:224–30. https://doi.org/10.1111/j.1469-0691.2005.01345.x.
Rantala S, Vahakuopus S, Vuopio-Varkila J, Vuento R, Syrjanen J. Streptococcus dysgalactiae subsp. equisimilis Bacteremia, Finland, 1995–2004. Emerg Infect Dis. 2010;16:843–6. https://doi.org/10.3201/eid1605.080803.
Siljander T, Lyytikainen O, Vahakuopus S, Snellman M, Jalava J, Vuopio J. Epidemiology, outcome and emm types of invasive group A streptococcal infections in Finland. Eur J Clin Microbiol Infect Dis. 2010;29:1229–35. https://doi.org/10.1007/s10096-010-0989-9.
Kaul R, McGeer A, Low DE, Green K, Schwartz B. Population-based surveillance for group A streptococcal necrotizing fasciitis: clinical features, prognostic indicators, and microbiologic analysis of seventy-seven cases. Ontario group A streptococcal study. Am J Med. 1997;103:18–24.
Simonsen KA, Anderson-Berry AL, Delair SF, Davies HD. Early-onset neonatal sepsis. Clin Microbiol Rev. 2014;27:21–47. https://doi.org/10.1128/CMR.00031-13.
Kittang BR, Bruun T, Langeland N, Mylvaganam H, Glambek M, Skrede S. Invasive group A, C and G streptococcal disease in western Norway: virulence gene profiles, clinical features and outcomes. Clin Microbiol Infect. 2011;17:358–64. https://doi.org/10.1111/j.1469-0691.2010.03253.x.
Ekelund K, Skinhoj P, Madsen J, Konradsen HB. Invasive group A, B, C and G streptococcal infections in Denmark 1999–2002: epidemiological and clinical aspects. Clin Microbiol Infect. 2005;11:569–76. https://doi.org/10.1111/j.1469-0691.2005.01169.x.
Rantala S, Vuopio-Varkila J, Vuento R, Huhtala H, Syrjanen J. Predictors of mortality in beta-hemolytic streptococcal bacteremia: a population-based study. J Infect. 2009;58:266–72. https://doi.org/10.1016/j.jinf.2009.01.015.
Laupland KB, Pasquill K, Parfitt EC, Dagasso G, Gupta K, Steele L. Inhospital death is a biased measure of fatal outcome from bloodstream infection. Clin Epidemiol. 2019;11:47–52. https://doi.org/10.2147/CLEP.S187381.
Laupland KB, Pasquill K, Parfitt EC, Dagasso G, Steele L. Streptococcus anginosus group bloodstream infections in the western interior of British Columbia, Canada. Infect Dis (Lond). 2018;50:423–8. https://doi.org/10.1080/23744235.2017.1416163.
Friedman ND, Kaye KS, Stout JE, McGarry SA, Trivette SL, Briggs JP, et al. Health care-associated bloodstream infections in adults: a reason to change the accepted definition of community-acquired infections. Ann Intern Med. 2002;137:791–7.
Charlson ME, Pompei P, Ales KL, MacKenzie CR. A new method of classifying prognostic comorbidity in longitudinal studies: development and validation. J Chronic Dis. 1987;40:373–83.
Population Estimates, BCstats. Available at: http://www.bcstats.gov.bc.ca/StatisticsBySubject/Demography/PopulationEstimates.aspx. Accessed 27 Mar 2019.
Phares CR, Lynfield R, Farley MM, Mohle-Boetani J, Harrison LH, Petit S, et al. Epidemiology of invasive group B streptococcal disease in the United States, 1999–2005. JAMA. 2008;299:2056–65. https://doi.org/10.1001/jama.299.17.2056.
Williamson DA, Morgan J, Hope V, Fraser JD, Moreland NJ, Proft T, et al. Increasing incidence of invasive group A streptococcus disease in New Zealand, 2002–2012: a national population-based study. J Infect. 2015;70:127–34. https://doi.org/10.1016/j.jinf.2014.09.001.
Harris P, Siew DA, Proud M, Buettner P, Norton R. Bacteraemia caused by beta-haemolytic streptococci in North Queensland: changing trends over a 14-year period. Clin Microbiol Infect. 2011;17:1216–22. https://doi.org/10.1111/j.1469-0691.2010.03427.x.
Laupland KB, Niven DJ, Pasquill K, Parfitt EC, Steele L. Culturing rate and the surveillance of bloodstream infections: a population-based assessment. Clin Microbiol Infect. 2018;24:910 e1- e4. https://doi.org/10.1016/j.cmi.2017.12.021.
Mehl A, Asvold BO, Lydersen S, Paulsen J, Solligard E, Damas JK, et al. Burden of bloodstream infection in an area of Mid-Norway 2002–2013: a prospective population-based observational study. BMC Infect Dis. 2017;17:205. https://doi.org/10.1186/s12879-017-2291-2.
Tyrrell GJ, Lovgren M, St Jean T, Hoang L, Patrick DM, Horsman G, et al. Epidemic of group A streptococcus M/emm59 causing invasive disease in Canada. Clin Infect Dis. 2010;51:1290–7. https://doi.org/10.1086/657068.
Dickson C, Pham MT, Nguyen V, Brubacher C, Silverman MS, Khaled K, et al. Community outbreak of invasive group A streptococcus infection in Ontario, Canada. Can Commun Dis Rep. 2018;44:182–8.
Laupland KB. Defining the epidemiology of bloodstream infections: the ‘gold standard’ of population-based assessment. Epidemiol Infect. 2013;141:2149–57. https://doi.org/10.1017/S0950268812002725.
Steer AC, Jenney AJ, Oppedisano F, Batzloff MR, Hartas J, Passmore J, et al. High burden of invasive beta-haemolytic streptococcal infections in Fiji. Epidemiol Infect. 2008;136:621–7. https://doi.org/10.1017/S095026880700917X.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
On behalf of all authors, the corresponding author states that there is no conflict of interest.
Rights and permissions
About this article
Cite this article
Laupland, K.B., Pasquill, K., Parfitt, E.C. et al. Bloodstream infection due to β-hemolytic streptococci: a population-based comparative analysis. Infection 47, 1021–1025 (2019). https://doi.org/10.1007/s15010-019-01356-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s15010-019-01356-9