Abstract
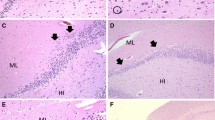
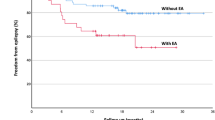
Sudden Unexpected Death in Childhood (SUDC) is the unexplained death of children aged between 1 and 18 years old. Hippocampal abnormalities have previously been described in Sudden Unexpected Death in Epilepsy (SUDEP) and it is possible that SUDC shares similar pathogenic mechanisms with SUDEP. Our aim was to determine the prevalence of hippocampal abnormalities, history of seizures and demographic features in our caseload of SUDC, SUDEP and SIDS cases. A review of post-mortem reports from 2003 to 2018 was carried out to identify cases of SUDC, SUDEP and SIDS. Histological evidence of hippocampal abnormalities, patient demographics (age, gender), sleeping position, and past medical history (history of seizures and illness 72 hours prior to death) were recorded. Statistical analysis was performed to compare the three groups. 48 SUDC, 18 SUDEP and 358 SIDS cases were identified. Hippocampal abnormalities associated with temporal lobe epilepsy were found in 44.4% of SUDC cases. 5/15 SUDC cases with a history of seizures demonstrated hippocampal abnormalities. SUDC cases were also more likely to be found prone compared to SIDS cases. In comparison with SIDS, both SUDC and SUDEP cases were more likely to demonstrate hippocampal abnormalities (SUDC: (OR = 9.4, 95% CI: 3.1–29.1, p < 0.001; SUDEP: OR = 35.4, 95% CI: 8.3–151.5, p < 0.001). We found a potential link between hippocampal abnormalities and epileptic seizures in SUDC. A concerted effort should be directed towards consistent sampling and standardized description of the hippocampus and clinical correlation with a history of seizures/epilepsy in postmortem reports.


Similar content being viewed by others
References
Kinney HC, Chadwick AE, Crandall LA, Grafe M, Armstrong DL, Kupsky WJ, et al. Sudden death, febrile seizures, and hippocampal and temporal lobe maldevelopment in toddlers: a new entity. Pediatr Dev Pathol. 2009;12:455–63.
Hesdorffer DC, Crandall LA, Friedman D, Devinsky O. Sudden unexplained death in childhood: a comparison of cases with and without a febrile seizure history. Epilepsia. 2015;56:1294–300.
Kinney HC, Armstrong DL, Chadwick AE, Crandall LA, Hilbert C, Belliveau RA, et al. Sudden death in toddlers associated with developmental abnormalities of the Hippocampus: a report of five cases. Pediatr Dev Pathol. 2007;10:208–23.
Crandall LG. Inexplicable child deaths: medicolegal death investigation resources from the SUDC Foundation and the SUDC registry and research collaborative. Acad Forensic Pathol. 2017;7:24–6.
Krous HF, Chadwick AE, Crandall L, Nadeau-Manning JM. Sudden unexpected death in childhood: a report of 50 cases. Pediatr Dev Pathol. 2005;8:307–19.
Goldstein RD, Kinney HC, Willinger M. Sudden unexpected death in Fetal life through early childhood. Pediatrics. 2016;137:e20154661.
Devinsky O, Hesdorffer DC, Thurman DJ, Lhatoo S, Richerson G. Sudden unexpected death in epilepsy: epidemiology, mechanisms, and prevention. Lancet Neurol. 2016;10:1075–88. https://doi.org/10.1016/S1474-4422(16)30158-2.
Donner EJ, Smith CR, Snead OC. Sudden unexplained death in children with epilepsy. Neurology. 2001;57:430–4.
Goldstein RD, Blair PS, Sens MA, Shapiro-Mendoza CK, Krous HF, Rognum TO, et al. Inconsistent classification of unexplained sudden deaths in infants and children hinders surveillance, prevention and research: recommendations from the 3rd international congress on Sudden infant and child death. Forensic Sci Med Pathol. 2019;15(4):622–28. https://doi.org/10.1007/s12024-019-00156-9.
Williamson L. Sudden Sudden unexpected death in infancy and childhood multi-agency guidelines for care and investigation [internet]. London. 2016. Available from: www.rcpath.org. Accessed 31 March 2020.
Maron BJ, Barbour DJ, Marraccini J V, Roberts WC. Sudden unexpected death 12 years after “near-miss” sudden infant death syndrome in infancy. Am J Cardiol. 1986;58(11):1104–5.
HM Government. Working together to safeguard children working together to safeguard children [internet]: Office; 2015. p. 393. Available from: http://informahealthcare.com/doi/abs/10.1080/13561820020003919.
Bright FM, Vink R, Byard RW. Neuropathological developments in sudden infant death syndrome. Pediatr Dev Pathol. 2018;21:515–21.
Paine SML, Jacques TS, Sebire NJ. Review: neuropathological features of unexplained sudden unexpected death in infancy: current evidence and controversies. Neuropathol Appl Neurobiol. 2014;40:364–84.
Liu Y, Liang Y, Tong F, Huang W, Tinzing L, Le Grange JM, et al. Sudden death from an epileptic seizure due to capillary telangiectasias in the hippocampus. Forensic Sci Med Pathol. 2019;15:243–8.
Kinney HC. Neuropathology provides new insight in the pathogenesis of the sudden infant death syndrome. Acta Neuropathol. 2009;117:247–55.
Gamss RP, Slasky SE, Bello JA, Miller TS, Shinnar S. Prevalence of hippocampal malrotation in a population without seizures: fig 1. Am J Neuroradiol [Internet]. 2009;30:1571–3. Available from: https://linkinghub.elsevier.com/retrieve/pii/S0022202X15370834.
Hefti MM, Cryan JB, Haas EA, Chadwick AE, Crandall LA, Trachtenberg FL, et al. Hippocampal malformation associated with sudden death in early childhood: a neuropathologic study. Forensic Sci Med Pathol. 2016;12:14–25.
Noebels J. Hippocampal abnormalities and sudden childhood death. Forensic Sci Med Pathol. 2016;12:198–9.
Dlouhy BJ, Ciliberto MA, Cifra CL, Kirby PA, Shrock DL, Nashelsky M, et al. Unexpected death of a child with complex febrile seizures-pathophysiology similar to sudden unexpected death in epilepsy? Front Neurol. 2017;8:21. https://doi.org/10.3389/fneur.2017.00021.
Thom M. Review: hippocampal sclerosis in epilepsy: a neuropathology review. Neuropathol Appl Neurobiol. 2014;40:520–43.
Thom M. Neuropathology of epilepsy: epilepsy-related deaths and SUDEP. Diagnostic Histopathol [Internet] Elsevier Ltd; 2019;25:23–33. Available from: https://doi.org/10.1016/j.mpdhp.2018.11.003.
Kinney HC, Poduri AH, Cryan JB, Haynes RL, Teot L, Sleeper LA, et al. Hippocampal formation maldevelopment and sudden unexpected death across the pediatric age spectrum. J Neuropathol Exp Neurol. 2016;75:981–97.
McGuone D, Leitner D, William C, Faustin A, Leelatian N, Reichard R, et al. Neuropathologic changes in sudden unexplained death in childhood. J Neuropathol Exp Neurol. 2020;79:336–46.
Kinney HC, Cryan JB, Haynes RL, Paterson DS, Haas EA, Mena OJ, et al. Dentate gyrus abnormalities in sudden unexplained death in infants: morphological marker of underlying brain vulnerability. Acta Neuropathol. 2015;129:65–80.
Blümcke I, Kistner I, Clusmann H, Schramm J, Becker AJ, Elger CE, et al. Towards a clinico-pathological classification of granule cell dispersion in human mesial temporal lobe epilepsies. Acta Neuropathol. 2009;117:535–44.
Houser CR. Granule cell dispersion in the dentate gyrus of humans with temporal lobe epilepsy. Brain Res. 1990;535:195–204.
Somani A, Zborovschi AB, Liu Y, Patodia S, Michalak Z, Sisodiya SM, et al. Hippocampal morphometry in sudden and unexpected death in epilepsy. Neurology. 2019;93:e804–14.
Parent JM, Yu TW, Leibowitz RT, Geschwind DH, Sloviter RS, Lowenstein DH. Dentate granule cell neurogenesis is increased by seizures and contributes to aberrant network reorganization in the adult rat hippocampus. J Neurosci. 1997;17:3727–38.
Wong LCH, Behr ER. Sudden unexplained death in infants and children: the role of undiagnosed inherited cardiac conditions. Europace. 2014;16:1706–13.
Gando I, Yang HQ, Coetzee WA. Functional significance of channelopathy gene variants in unexplained death. Forensic Sci med Pathol. 2019;15:437–44.
Da Silva BGC, Da Silveira MF, De Oliveira PD, Domingues MR, Neumann NA, Barros FC, et al. Prevalence and associated factors of supine sleep position in 3-month-old infants: findings from the 2015 Pelotas (Brazil) birth cohort. BMC Pediatr. 2019;19:1–8.
Cryan JB, Trachtenberg FL, Crandall LA, Hefti MM, Krous HF, Grafe M, et al. Sudden unexpected death in early childhood: general observations in a series of 151 cases. Forensic Sci Med Pathol. 2016;12:4–13.
Crandall LG, Lee JH, Stainman R, Friedman D, Devinsky O. Potential role of febrile seizures and other risk factors associated with sudden deaths in children. JAMA Netw Open. 2019;2:e192739.
Harden C, Tomson T, Gloss D, Buchhalter J, Cross JH, Donner E, et al. Practice guideline summary: Sudden unexpected death in epilepsy incidence rates and risk factors. Neurology. 2017;88:1674–80.
Abdel-Mannan O, Taylor H, Donner EJ, Sutcliffe AG. A systematic review of sudden unexpected death in epilepsy (SUDEP) in childhood. Epilepsy Behav [Internet] Elsevier Inc 2019;90:99–106. https://doi.org/10.1016/j.yebeh.2018.11.006.
Camfield P, Camfield C. Sudden unexpected death in people with epilepsy: a pediatric perspective. Semin Pediatr Neurol. 2005;12:10–4.
Goldman AM, Glasscock E, Yoo J, Chen TT, Klassen TL, Noebels JL. Arrhythmia in heart and brain: kcnq1 mutations link epilepsy and sudden unexplained death. Sci Transl Med [Internet]. 2009;1:2ra6–6. Available from: https://stm.sciencemag.org/lookup/doi/10.1126/scitranslmed.3000289.
Van Der Lende M, Surges R, Sander JW, Thijs RD. Cardiac arrhythmias during or after epileptic seizures. J Neurol Neurosurg Psychiatry. 2016;87:69–74.
Kasperavičiute D, Catarino CB, Matarin M, Leu C, Novy J, Tostevin A, et al. Epilepsy, hippocampal sclerosis and febrile seizures linked by common genetic variation around SCN1A. Brain. 2013;136:3140–50.
Thorn M. Neuropathologic findings in postmortem studies of sudden death in epilepsy. Epilepsia. 1997;38:S32–4.
Kinney HC, Thach BT. The sudden infant death syndrome. N Engl J Med [Internet]. 2009;361:795–805. Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3268262/pdf/nihms-342719.pdf.
Krous HF, Trachtenberg FL, Haas EA, Kinney HC, Stanley C. Risk factor changes for sudden infant death syndrome after initiation of back-to-sleep campaign. Pediatrics. 2012;129:630–8.
de Luca F, Hinde A. Effectiveness of the “Back-to-sleep” campaigns among healthcare professionals in the past 20 years: a systematic review. BMJ Open. 2016;6:e011435.
Blair PS, Platt MW, Smith IJ, Fleming PJ. Sudden infant death syndrome and sleeping position in pre-term and low birth weight infants: an opportunity for targeted intervention. Arch Dis Child. 2006;91:101–6.
Horne RSC, Hauck FR, Moon RY. Sudden infant death syndrome and advice for safe sleeping. BMJ [Internet]. 2015;350:1–7. https://doi.org/10.1136/bmj.h1989.
Fleming PJ, Blair PSP, Bacon C, Berry PJ. Sudden unexpected death in infancy. The CESDI SUDI studies 1993-1996. London: The Stationery Office. 2000.
Myers KA, McPherson RE, Clegg R, Buchhalter J. Sudden death after febrile seizure case report: cerebral suppression precedes severe bradycardia. Pediatrics. 2017;140(5):e20162051. https://doi.org/10.1542/peds.2016-2051.
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Kon, F.C., Vázquez, R.Z., Lang, A. et al. Hippocampal abnormalities and seizures: a 16-year single center review of sudden unexpected death in childhood, sudden unexpected death in epilepsy and SIDS. Forensic Sci Med Pathol 16, 423–434 (2020). https://doi.org/10.1007/s12024-020-00268-7
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12024-020-00268-7