Abstract
Background
Liver metastases are common in patients with neuroendocrine tumors (NETs), having a negative impact on disease prognosis. The options for selective therapy in patients with unresectable multiple liver metastases are limited to TACE (transarterial chemoembolization), TAE (transarterial embolization), or SIRT (selective internal radiation therapy).
Aim
To explore the clinical outcome, survival and safety of these therapies in NETs patients.
Methods
Retrospective case series of consecutive patients (mean age 56.6 years, 59% male) treated at two tertiary university medical centers from 2005 to 2015.
Results
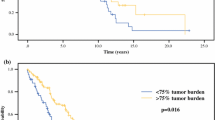
Fifty-seven patients with G1, G2, and low G3 NETs with liver metastases were investigated (pancreatic NET (pNET), 24; small bowel, 16; unknown origin (UKO), 9; rectal, 3; lung, 3; and gastric, 2). Fifty-three patients underwent TACE, three patients underwent TAE, and one patient underwent SIRT. Clinical improvement and tumor response were observed in 54/57 patients (95%), together with marked decreased in tumor markers. The median time to tumor progression following the first treatment was 14 ± 16 months. The median overall survival was 22 ± 18 months, more pronounced in the pNET, followed by small bowel and UKO subgroups. There was a trend for a better survival in patients with disease limited to the liver and in whom the primary tumor was resected.
Conclusion
Hepatic intra-arterial therapies are well tolerated in the majority of patients with NETs and liver metastases and associated with both clinical improvement and tumor stabilization for prolonged periods. These therapies should be always considered, irrespective of the presence of extrahepatic metastasis.


Similar content being viewed by others
References
S. Grozinsky-Glasberg, D.J. Gross, New drugs in the therapy of neuroendocrine tumors. J. Endocrinol. Invest. 35, 930–936 (2012)
I.M. Modlin, K.D. Lye, M. Kidd, A 5-decade analysis of 13,715 carcinoid tumors. Cancer 97, 934–959 (2003)
G. Rindi, The ENETS guidelines: the new TNM classification system. Tumori 96, 806–809 (2010)
M. Pavel, D. O’Toole, F. Costa et al. Vienna Consensus Conference ENETS Consensus Guidelines Update for the Management of Distant Metastatic Disease of Intestinal, Pancreatic, Bronchial Neuroendocrine Neoplasms (NEN) and NEN of Unknown Primary Site. Neuroendocrinology 103, 172–185 (2016)
T. de Baere, F. Deschamps, L. Tselikas et al. Interventional radiology: role in the treatment of liver metastases from GEP-NETs. Eur. J. Endocrinol. 172, R151–166 (2015)
B. Lawrence, B.I. Gustafsson, A. Chan et al. The epidemiology of gastroenteropancreatic neuroendocrine tumors. Endocrinol. Metab. Clin. North Am. 40, 1–18 (2011)
R.S. Chamberlain, D. Canes, K.T. Brown et al., Hepatic neuroendocrine metastases: does intervention alter outcomes? J. Am. Coll. Surg. 190, 432–445 (2000)
A.K. Clift, A. Frilling, Management of patients with hepatic metastases from neuroendocrine tumors. Ann. Saudi Med. 34, 279–290 (2014)
A. Frilling, A.K. Clift, Therapeutic strategies for neuroendocrine liver metastases. Cancer 121, 1172–1186 (2015)
A. Kennedy, L. Bester, R. Salem et al., Role of hepatic intra-arterial therapies in metastatic neuroendocrine tumours (NET): guidelines from the NET-Liver-Metastases Consensus Conference. HPB 17, 29–37 (2015)
S. Gupta, Intra-arterial liver-directed therapies for neuroendocrine hepatic metastases. Semin. Interv. Radiol. 30, 28–38 (2013)
F. Yinglu, L. Changquan, Z. Xiaofeng et al. A new way: alleviating postembolization syndrome following transcatheter arterial chemoembolization. J. Altern. Complement. Med. 15, 175–181 (2009)
E. Moon, M.D. Tam, R.N. Kikano et al. Prophylactic antibiotic guidelines in modern interventional radiology practice. Semin. Interv. Radiol. 27, 327–337 (2010)
G. Rindi, W.W. de Herder, D. O’Toole et al., Consensus guidelines for the management of patients with digestive neuroendocrine tumors: the second event and some final considerations. Neuroendocrinology 87, 5–7 (2008)
T.J. Vogl, N.N. Naguib, S. Zangos et al. Liver metastases of neuroendocrine carcinomas: interventional treatment via transarterial embolization, chemoembolization and thermal ablation. Eur. J. Radiol. 72, 517–528 (2009)
L.M. Wang, A.R. Jani, E.J. Hill et al. Anatomical basis and histopathological changes resulting from selective internal radiotherapy for liver metastases. J. Clin. Pathol. 66, 205–211 (2013)
S.C. Pitt, J. Knuth, J.M. Keily et al. Hepatic neuroendocrine metastases: chemo- or bland embolization? J. Gastrointest. Surg. 12, 1951–1960 (2008)
H. Martensson, A. Nobin, S. Bengmark et al. Embolization of the liver in the management of metastatic carcinoid tumors. J. Surg. Oncol. 27, 152–158 (1984)
M. Del Prete, F. Fiore, R. Modica et al., Multidisciplinary group for neuroendocrine tumors. hepatic arterial embolization in patients with neuroendocrine tumors. J. Exp. Clin. Cancer Res. 33, 33–43 (2014)
M. Pericleous, M.E. Caplin, E. Tsochatzis et al. Hepatic artery embolization in advanced neuroendocrine tumors: Efficacy and long-term outcomes. Asia Pac. J. Clin. Oncol. 12, 61–69 (2016)
C. Loewe, M. Schindl, M. Cejna et al. Permanent transarterial embolization of neuroendocrine metastases of the liver using cyanoacrylate and lipiodol: assessment of mid- and long-term results. Am. J. Roentgenol. 180, 1379–1384 (2003)
C.H. Carrasco, C. Charnsangavej, J. Ajani et al. The carcinoid syndrome: palliation by hepatic artery embolization. Am. J. Roentgenol. 147, 149–154 (1986)
C.H. Carrasco, S. Wallace, C. Charnsangavej et al. Treatment of hepatic metastases in ocular melanoma. Embolization of the hepatic artery with polyvinyl sponge and cisplatin. JAMA 255, 3152–3154 (1986)
J.R. Strosberg, J. Choi, A.B. Cantor et al. Selective hepatic artery embolization for treatment of patients with metastatic carcinoid and pancreatic endocrine tumors. Cancer Control. 13, 72–78 (2006)
B.K. Eriksson, E.G. Larsson, B.M. Skogseid et al. Liver embolizations of patients with malignant neuroendocrine gastrointestinal tumors. Cancer 83, 2293–2301 (1998)
F. Fiore, M. Del Prete, R. Franco et al. Transarterial embolization (TAE) is equally effective and slightly safer than transarterial chemoembolization (TACE) to manage liver metastases in neuroendocrine tumors. Endocrine 47, 177–182 (2014)
C. Sward, V. Johanson, E. Nieveen van Dijkum et al., Prolonged survival after hepatic artery embolization in patients with midgut carcinoid syndrome. Br. J. Surg. 96, 517–521 (2009)
S. Dominguez, A. Denys, I. Madeira et al. Hepatic arterial chemoembolization with streptozotocin in patients with metastatic digestive endocrine tumours. Eur. J. Gastroenterol. Hepatol. 12, 151–157 (2000)
P. Ruszniewski, P. Rougier, A. RocheA et al., Hepatic arterial chemoembolization in patients with liver metastases of endocrine tumors. A prospective phase II study in 24 patients. Cancer 71, 2624–2630 (1993)
J.D. Drougas, L.B. Anthony, T.K. Blair et al., Hepatic artery chemoembolization for management of patients with advanced metastatic carcinoid tumors. Am. J. Surg. 175, 408–412 (1998)
M. Bloomston, O. Al-Saif, D. Klemanski et al., Hepatic artery chemoembolization in 122 patients with metastatic carcinoid tumor: lessons learned. J. Gastrointest. Surg. 11, 264–271 (2007)
S. Gupta, M.M. Johnson, R. Murthy et al. Hepatic arterial embolization and chemoembolization for the treatment of patients with metastatic neuroendocrine tumors: variables affecting response rates and survival. Cancer 104, 1590–1602 (2005)
R. Caprotti, C. Angelini, C. Mussi et al. Gastrointestinal carcinoids. Prognosis and survival. Minerva Chir. 58, 523–532 (2003)
E.W. McDermott, B. Guduric, M.F. Brennan, Prognostic variables in patients with gastrointestinal carcinoid tumours. Br. J. Surg. 81, 1007–1009 (1994)
C.T. Sofocleous, E.N. Petre, M. Gonen et al., Factors affecting periprocedural morbidity and mortality and long-term patient survival after arterial embolization of hepatic neuroendocrine metastases. J. Vasc. Interv. Radiol. 25, 22–30 (2014)
J.A. Ajani, C.H. Carrasco, C. Charnsangavej et al. Islet cell tumors metastatic to the liver: effective palliation by sequential hepatic artery embolization. Ann. Intern. Med. 108, 340–344 (1988)
A. Nobin, B. Mansson, A. Lunderquist, Evaluation of temporary liver dearterialization and embolization in patients with metastatic carcinoid tumour. Acta Oncol. 28, 419–424 (1989)
E. Therasse, F. Breittmayer, A. Roche et al. Transcatheter chemoembolization of progressive carcinoid liver metastasis. Radiology 189, 541–547 (1993)
M.E. Clouse, L. Perry, K. Stuart et al. Hepatic arterial chemoembolization for metastatic neuroendocrine tumors. Digestion 55, 92–97 (1994)
L.J. Perry, K. Stuart, K.R. Stokes et al., Hepatic arterial chemoembolization for metastatic neuroendocrine tumors. Surgery 116, 1111–1116 (1994)
B. Wangberg, G. Westberg, U. Tylen et al. Survival of patients with disseminated midgut carcinoid tumors after aggressive tumor reduction. World J. Surg. 20, 892–899 (1996)
E. Diamandidou, J.A. Ajani, D.J. Yang et al., Two-phase study of hepatic artery vascular occlusion with microencapsulated cisplatin in patients with liver metastases from neuroendocrine tumors. Am. J. Roentgenol. 170, 339–344 (1998)
K.T. Brown, B.Y. Koh, L.A. Brody et al. Particle embolization of hepatic neuroendocrine metastases for control of pain and hormonal symptoms. J. Vasc. Interv. Radiol. 10, 397–403 (1999)
Y.H. Kim, J.A. Ajani, C.H. Carrasco et al. Selective hepatic arterial chemoembolization for liver metastases in patients with carcinoid tumor or islet cell carcinoma. Cancer Invest. 17, 474–478 (1999)
A. Roche, B.V. Girish, T. de Baere et al. Trans-catheter arterial chemoembolization as first-line treatment for hepatic metastases from endocrine tumors. Eur. Radiol. 13, 136–140 (2003)
S. Gupta, J.C. Yao, K. Ahrar et al., Hepatic artery embolization and chemoembolization for treatment of patients with metastatic carcinoid tumors: the M.D. Anderson experience. Cancer J. 9, 261–267 (2003)
O. Kress, H.J. Wagner, M. Wied et al. Transarterial chemoembolization of advanced liver metastases of neuroendocrine tumors--a retrospective single-center analysis. Digestion 68, 94–101 (2003)
A.T. Ruutiainen, M.C. Soulen, C.M. Tuite et al. Chemoembolization and bland embolization of neuroendocrine tumor metastases to the liver. J. Vasc. Interv. Radiol. 18, 847–855 (2007)
A.S. Ho, J. Picus, M.D. Darcy et al. Long-term outcome after chemoembolization and embolization of hepatic metastatic lesions from neuroendocrine tumors. Am. J. Roentgenol. 188, 1201–1207 (2007)
T. de Baere, F. Deschamps, C. Teriitheau et al., Transarterial chemoembolization of liver metastases from well differentiated gastroenteropancreatic endocrine tumors with doxorubicin-eluting beads: preliminary results. J. Vasc. Interv. Radiol. 19, 855–861 (2008)
A. Frilling, I.M. Modlin, M. Kidd, et al., Working Group on Neuroendocrine Liver Metastases, Recommendations for management of patients with neuroendocrine liver metastases. Lancet Oncol. 15, 8–21 (2014).
X.D. Dong, B.I. Carr, Hepatic artery chemoembolization for the treatment of liver metastases from neuroendocrine tumors: a long-term follow-up in 123 patients. Med. Oncol. 28, 286–290 (2011)
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Grozinsky-Glasberg, S., Kaltsas, G., Kaltsatou, M. et al. Hepatic intra-arterial therapies in metastatic neuroendocrine tumors: lessons from clinical practice. Endocrine 60, 499–509 (2018). https://doi.org/10.1007/s12020-018-1537-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12020-018-1537-0