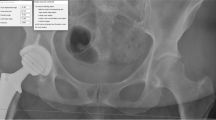
Abstract
Accurate and precise positioning of the acetabular cup remains a prevalent challenge in total hip arthroplasty (THA). Robotic assistance for THA has increased over the past decade due to the potential to improve the accuracy of implant placement. However, a common criticism of existing robotic systems is the requirement for preoperative computerized tomography (CT) scans. This additional imaging increases patient radiation exposure, as well as cost, and requires pin placement during surgery. The goal of this study was to analyze the radiation burden associated with a novel, CT-free robotic THA system compared to an unassisted manual THA approach (n = 100/arm). On average, the study cohort had a higher number of fluoroscopic images captured (7.5 vs. 4.3 images; p < 0.001), radiation dose (3.0 vs. 1.0 mGy; p < 0.001), and a longer duration of radiation exposure (18.8 vs. 6.3 s; p < 0.001), per procedure, than the control group. Additionally, no learning curve was detected by CUSUM analysis with respect to the number of fluoroscopic images taken during the adoption of the robotic THA system. While statistically significant, in comparison to published literature, the radiation exposure of the CT-free robotic THA system was comparable to that of unassisted manual THA approach and less than that of CT-based robotic approaches. Thus, the novel CT-free robotic system likely poses no clinically significant increase in radiation exposure to the patient compared to manual approaches.



Similar content being viewed by others
Data availability
Data is available in raw format for review as needed and upon request by authors.
Change history
15 April 2023
A Correction to this paper has been published: https://doi.org/10.1007/s11701-023-01584-0
References
Bhandari M, Matta JM, Dodgin D, Clark C, Kregor P, Bradley G et al (2009) Outcomes following the single-incision anterior approach to total hip arthroplasty: a multicenter observational study. Orthop Clin N Am. 40:329–42. https://doi.org/10.1016/J.OCL.2009.03.001.
Gazendam A, Bozzo A, Ekhtiari S, Kruse C, Hiasat N, Tushinski D et al (2022) Short-term outcomes vary by surgical approach in total hip arthroplasty: a network meta-analysis. Arch Orthop Trauma Surg. https://doi.org/10.1007/S00402-021-04131-4
Post ZD, Orozco F, Diaz-Ledezma C, Hozack WJ, Ong A (2014) Direct anterior approach for total hip arthroplasty: indications, technique, and results. J Am Acad Orthop Surg 22:595–603. https://doi.org/10.5435/JAAOS-22-09-595
Zimmerer A, Steinhaus M, Sickmüller E, Ulmar B, Hauschild M, Miehlke W et al (2022) Pain and rehabilitation after total hip arthroplasty are approach dependent: a multisurgeon, single-center, prospective cohort study. Arch Orthop Trauma Surg 142:3075–3082. https://doi.org/10.1007/S00402-021-03921-0
Connolly KP, Kamath AF (2016) Direct anterior total hip arthroplasty: comparative outcomes and contemporary results. World J Orthop 7:94–101. https://doi.org/10.5312/WJO.V7.I2.94
Lewinnek GE, Lewis JL, Tarr RI, Compere CL, Zimmerman JR (1978) Dislocations after total hip-replacement arthroplasties. J Bone Jt Surg Am 60:113–115. https://doi.org/10.1007/978-1-4471-5451-8_27
Kamath AF, Durbhakula SM, Pickering T, Cafferky NL, Murray TG, Wind MA et al (2021) Improved accuracy and fewer outliers with a novel CT-free robotic THA system in matched-pair analysis with manual THA. J Robot Surg. https://doi.org/10.1007/S11701-021-01315-3/FIGURES/5
James CR, Peterson BE, Crim JR, Cook JL, Crist BD (2018) The use of fluoroscopy during direct anterior hip arthroplasty: powerful or misleading? J Arthroplasty 33:1775–1779. https://doi.org/10.1016/J.ARTH.2018.01.040
Sugano N (2013) Computer-assisted orthopaedic surgery and robotic surgery in total hip arthroplasty. Clin Orthop Surg 5:1. https://doi.org/10.4055/CIOS.2013.5.1.1
Subramanian P, Wainwright TW, Bahadori S, Middleton RG (2019) A review of the evolution of robotic-assisted total hip arthroplasty. Hip Int 29:232–238. https://doi.org/10.1177/1120700019828286
Ponzio DY, Lonner JH (2015) Preoperative mapping in unicompartmental knee arthroplasty using computed tomography scans is associated with radiation exposure and carries high cost. J Arthroplasty 30:964–967. https://doi.org/10.1016/J.ARTH.2014.10.039
Pomeroy CL, Mason JB, Fehring TK, Masonis JL, Curtin BM (2016) Radiation exposure during fluoro-assisted direct anterior total hip arthroplasty. J Arthroplasty 31:1742–1745. https://doi.org/10.1016/J.ARTH.2016.01.031
McNabb DC, Jennings JM, Levy DL, Miner TM, Yang CC, Kim RH (2017) Direct anterior hip replacement does not pose undue radiation exposure risk to the patient or surgeon. J Bone Jt Surg Am 99:2020–2025. https://doi.org/10.2106/JBJS.17.00351
Curtin BM, Armstrong LC, Bucker BT, Odum SM, Jiranek WA (2016) Patient radiation exposure during fluoro-assisted direct anterior approach total hip arthroplasty. J Arthroplasty 31:1218–1221. https://doi.org/10.1016/j.arth.2015.12.012
Jinnai Y, Baba T, Zhuang X, Tanabe H, Banno S, Watari T et al (2020) Does a fluoro-assisted direct anterior approach for total hip arthroplasty pose an excessive risk of radiation exposure to the surgeon? SICOT-J. https://doi.org/10.1051/SICOTJ/2020004
Navarro SM, Frey C, Blackwell T, Voges SB, Schutte H Jr, Del. (2018) Clinical Results of direct anterior approach THA with minimal fluoroscopic exposure optimization techniques—pubMed. Surg Technol Int 11:277–280
Weeks CA, Preston S, Howard JL, Vasarhelyi EM, Matz J, Lanting BA (2016) Preoperative pelvic tilt analysis reduces fluoroscopy time in direct anterior total hip arthroplasty. Orthopedics 39:e962–e966. https://doi.org/10.3928/01477447-20160616-06
McArthur BA, Schueler BA, Howe BM, Trousdale RT, Taunton MJ (2015) Radiation exposure during fluoroscopic guided direct anterior approach for total hip arthroplasty. J Arthroplasty 30:1565–1568. https://doi.org/10.1016/J.ARTH.2015.03.029
Ong CB, Chiu YF, Premkumar A, Gonzalez Della Valle A (2022) Use of a novel imageless navigation system reduced fluoroscopy exposure and improved acetabular positioning in anterior approach total hip arthroplasty: a case-control study. Arch Orthop Trauma Surg. https://doi.org/10.1007/S00402-022-04520-3
Padmanabha A, Agarwal-Harding K, Villafuerte JA (2019) Improved perioperative outcomes with direct anterior approach total hip arthroplasty in a Veteran’s Affairs patient population. J Arthrosc Jt Surg 6:165–170. https://doi.org/10.1016/J.JAJS.2019.05.003
Biau DJ, Williams SM, Schlup MM, Nizard RS, Porcher R (2008) Quantitative and individualized assessment of the learning curve using LC-CUSUM. Br J Surg 95:925–929. https://doi.org/10.1002/BJS.6056
Kayani B, Konan S, Huq SS, Ibrahim MS, Ayuob A, Haddad FS (2021) The learning curve of robotic-arm assisted acetabular cup positioning during total hip arthroplasty. Hip Int 31:311–319. https://doi.org/10.1177/1120700019889334
Kayani B, Konan S, Huq SS, Tahmassebi J, Haddad FS (2019) Robotic-arm assisted total knee arthroplasty has a learning curve of seven cases for integration into the surgical workflow but no learning curve effect for accuracy of implant positioning. Knee Surg Sport Traumatol Arthrosc 27:1132. https://doi.org/10.1007/S00167-018-5138-5
Surgical Guide Mako TKA Surgical Guide n.d. https://www.strykermeded.com/media/2223/mako-tka-surgical-guide.pdf. Accessed 13 Dec 2022
Mako THA CT Scanning Protocol n.d. https://apps.ausrad.com/protocols/Protocols/ComputedTomography/01_Hospital_ERImaging/Seton AscensionCTProtocols/ImagingProtocol-CTMakoHip-ASMCCMorris.pdf. Accessed 13 Dec 2022
Chai W, Kong X, Yang M, Puah KL, Tang P, Chen J (2020) Robot-assisted total hip arthroplasty for arthrodesed hips. Ther Clin Risk Manag 16:357–368. https://doi.org/10.2147/TCRM.S246565
Huppertz A, Radmer S, Asbach P, Juran R, Schwenke C, Diederichs G et al (2011) Computed tomography for preoperative planning in minimal-invasive total hip arthroplasty: radiation exposure and cost analysis. Eur J Radiol 78:406–413. https://doi.org/10.1016/J.EJRAD.2009.11.024
Huppertz A, Lembcke A, Sariali EH, Durmus T, Schwenke C, Hamm B et al (2015) Low dose computed tomography for 3D planning of total hip arthroplasty: evaluation of radiation exposure and image quality. J Comput Assist Tomogr 39:649–656. https://doi.org/10.1097/RCT.0000000000000271
Sariali E, Mauprivez R, Khiami F, Pascal-Mousselard H, Catonné Y (2012) Accuracy of the preoperative planning for cementless total hip arthroplasty. A randomised comparison between three-dimensional computerised planning and conventional templating. Orthop Traumatol Surg Res 98:151–158. https://doi.org/10.1016/J.OTSR.2011.09.023
Geijer M, Rundgren G, Weber L, Flivik G (2017) Effective dose in low-dose CT compared with radiography for templating of total hip arthroplasty. Acta Radiol 58:1276–1282. https://doi.org/10.1177/0284185117693462
Tarwala R, Dorr LD (2011) Robotic assisted total hip arthroplasty using the MAKO platform. Curr Rev Musculoskelet Med 4:151–156. https://doi.org/10.1007/S12178-011-9086-7
Funding
The authors declare that no funds, grants, or other support was received during the preparation of this manuscript.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Material preparation, data collection, and analysis were performed by GB and CH. The first draft of the manuscript was written by GB and CO, and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
Graham Buchan, Christian Ong, Christian Hecht, and Akihiko Hasegawa declare they have no financial interests. Thomas Tanous and Blake Peterson serve on the Zimmer Biomet speaker’s bureau. Blake Peterson and Atul Kamath serve as consultants for Zimmer Biomet.
Ethics approval
This study was performed in line with the principles of the Declaration of Helsinki. Approval was granted by the Cleveland Clinic Foundation Institutional Review Board (June 3rd, 2022/ No. 22–528).
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Buchan, G., Ong, C., Hecht, C. et al. Equivalent radiation exposure with robotic total hip replacement using a novel, fluoroscopic-guided (CT-free) system: case–control study versus manual technique. J Robotic Surg 17, 1561–1567 (2023). https://doi.org/10.1007/s11701-023-01554-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11701-023-01554-6