Abstract
Objective
To conduct a meta-analysis examining the effects of bariatric surgery on nocturnal hypoxemia in obese patients with obstructive sleep apnea (OSA).
Methods
PubMed, EMBASE, Cochrane Library, and Web of Science were searched (the last search date was June 10, 2018) to identify relevant clinical studies. The mean arterial oxygen saturation (MeanSaO2), nadir oxygen saturation (NadirSaO2), apnea hypopnea index (AHI), and body mass index (BMI) data during the perioperative period were extracted and analyzed using a random effects model. Then, we performed subgroup and sensitivity analyses and calculated the publication bias to assess the between-study heterogeneity.
Results
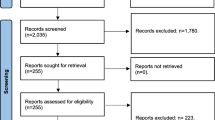
In total, 15 studies with 636 patients were included; 13 were prospective observational trials, 1 was a randomized controlled trial (RCT), and 1 was a retrospective trial. After surgery, the MeanSaO2 and NadirSaO2 increased by 1.36 [95% CI (0.72, 2.00)] and 1.08 [95% CI (0.68, 1.49)], respectively, and the AHI and BMI decreased by 1.11 [95% CI (0.82, 1.40)] and 1.97 [95% CI (1.67, 2.27)], respectively. However, the heterogeneity across all trials was high; we identified some of the sources of that heterogeneity through subsequent subgroup and sensitivity analyses.
Conclusions
Bariatric surgery is effective at improving nocturnal hypoxemia in obese patients with OSA; it also reduces body weight and the number of apnea events. More randomized controlled and comparative trials are necessary in the future to confirm our findings and to explore the potential underlying mechanisms.





Similar content being viewed by others
References
Collaborators GBDO, Afshin A, Forouzanfar MH, et al. Health effects of overweight and obesity in 195 countries over 25 years. N Engl J Med. 2017;377(1):13–27.
Young T, Peppard PE, Taheri S. Excess weight and sleep-disordered breathing. J Appl Physiol (1985). 2005;99(4):1592–9.
Tishler PV, Larkin EK, Schluchter MD, et al. Incidence of sleep-disordered breathing in an urban adult population: the relative importance of risk factors in the development of sleep-disordered breathing. JAMA. 2003;289(17):2230–7.
Young T, Peppard PE, Gottlieb DJ. Epidemiology of obstructive sleep apnea: a population health perspective. Am J Respir Crit Care Med. 2002;165(9):1217–39.
Capdevila OS, Kheirandish-Gozal L, Dayyat E, et al. Pediatric obstructive sleep apnea: complications, management, and long-term outcomes. Proc Am Thorac Soc. 2008;5(2):274–82.
Jakobsen GS, Smastuen MC, Sandbu R, et al. Association of bariatric surgery vs medical obesity treatment with long-term medical complications and obesity-related comorbidities. JAMA. 2018;319(3):291–301.
Ikramuddin S, Korner J, Lee WJ, et al. Lifestyle intervention and medical management with vs without roux-en-Y gastric bypass and control of hemoglobin A1c, LDL cholesterol, and systolic blood pressure at 5 years in the diabetes surgery study. JAMA. 2018;319(3):266–78.
Peromaa-Haavisto P, Tuomilehto H, Kossi J, et al. Obstructive sleep apnea: the effect of bariatric surgery after 12 months. A prospective multicenter trial. Sleep Med. 2017;35:85–90. English
Del Genio G, Limongelli P, Del Genio F, et al. Sleeve gastrectomy improves obstructive sleep apnea syndrome (OSAS): 5 year longitudinal study. Surg Obes Relat Dis. 2016;12(1):70–4.
Haines KL, Nelson LG, Gonzalez R, et al. Objective evidence that bariatric surgery improves obesity-related obstructive sleep apnea. Surgery. 2007;141(3):354–8.
Fritscher LG, Canani S, Mottin CC, et al. Bariatric surgery in the treatment of obstructive sleep apnea in morbidly obese patients. Respiration. 2007;74(6):647–52.
Lettieri CJ, Eliasson AH, Greenburg DL. Persistence of obstructive sleep apnea after surgical weight loss. J Clin Sleep Med. 2008;4(4):333–8. English
Krieger AC, Youn H, Modersitzki F, et al. Effects of laparoscopic adjustable gastric banding on sleep and metabolism: a 12-month follow-up study. Int J Gen Med. 2012;5:975–81.
Fredheim JM, Rollheim J, Sandbu R, et al. Obstructive sleep apnea after weight loss: a clinical trial comparing gastric bypass and intensive lifestyle intervention. J Clin Sleep Med. 2013;9(5):427–32. English
Bae EK, Lee YJ, Yun CH, et al. Effects of surgical weight loss for treating obstructive sleep apnea. Sleep Breath. 2014;18(4):901–5.
Ravesloot MJL, Hilgevoord AAJ, Van Wagensveld BA, et al. Assessment of the effect of bariatric surgery on obstructive sleep apnea at two postoperative intervals. Obes Surg. 2014;24(1):22–31. English
Zou J, Zhang P, Yu H, et al. Effect of laparoscopic Roux-en-Y gastric bypass surgery on obstructive sleep apnea in a Chinese population with obesity and T2DM. Obes Surg. 2015;25(8):1446–53.
Jiao X, Zou J, Zhang P, et al. Roux-en-Y gastric bypass surgery on obstructive sleep apnea-hypopnea syndrome: factors associated with postoperative efficacy. Obes Surg. 2016;26(12):2924–30.
Shaarawy H, Sarhan A. A ELH. Assessment of the effect of bariatric surgery on severe obstructive sleep apnea patients not tolerating CPAP therapy. Egyptian Journal of Chest Diseases and Tuberculosis. 2016;65(3):661–6. English
Suliman LAM, Abdalla DA. Does sleeve gastrectomy improve obstructive sleep apnea? Egyptian Journal of Chest Diseases and Tuberculosis. 2016;65(2):505–10. English
Amin R, Simakajornboon N, Szczesniak R, et al. Early improvement in obstructive sleep apnea and increase in orexin levels after bariatric surgery in adolescents and young adults. Surg Obes Relat Dis. 2017;13(1):95–100.
Aguiar I, Freitas W, Santos I, Apostolico N, Nacif S, Urbano J, et al. Obstructive sleep apnea and pulmonary function in patients with severe obesity before and after bariatric surgery: a randomized clinical trial. Multidiscip Respir Med. 2014;9(1) (no pagination).
Guardiano SA, Scott JA, Ware JC, et al. The long-term results of gastric bypass on indexes of sleep apnea. Chest. 2003;124(4):1615–9.
Fredheim JM, Rollheim J, Hofsø D, et al. The effect of intensive lifestyle intervention and bariatric surgery on moderate to severe obstructive sleep apnea in morbidly obese patients: A non-randomised clinical trial. Obes Facts. 2012;5:229. English
Peppard PE, Young T, Barnet JH, et al. Increased prevalence of sleep-disordered breathing in adults. Am J Epidemiol. 2013;177(9):1006–14.
McEvoy RD, Antic NA, Heeley E, et al. CPAP for prevention of cardiovascular events in obstructive sleep apnea. N Engl J Med. 2016;375(10):919–31.
Engleman H, Wild M. Improving CPAP use by patients with the sleep apnoea/hypopnoea syndrome (SAHS). Sleep Med Rev. 2003;7(1):81–99.
de Raaff CAL, Gorter-Stam MAW, de Vries N, et al. Perioperative management of obstructive sleep apnea in bariatric surgery: a consensus guideline. Surg Obes Relat Dis. 2017;13(7):1095–109.
Aurora RN, Crainiceanu C, Gottlieb DJ, et al. Obstructive sleep apnea during REM sleep and cardiovascular disease. Am J Respir Crit Care Med. 2018;197(5):653–60.
Simpson L, Mukherjee S, Cooper MN, et al. Sex differences in the association of regional fat distribution with the severity of obstructive sleep apnea. Sleep. 2010;33(4):467–74.
Acknowledgements
Many thanks to the patience and support from my tutor, professor Wang.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that there are no conflicts of interest.
Ethical Approval
For this type of study, formal consent is not required.
Financial Disclosure
None.
Electronic Supplementary Material
ESM 1
(DOCX 1170 kb)
Rights and permissions
About this article
Cite this article
Zhang, Y., Wang, W., Yang, C. et al. Improvement in Nocturnal Hypoxemia in Obese Patients with Obstructive Sleep Apnea after Bariatric Surgery: a Meta-Analysis. OBES SURG 29, 601–608 (2019). https://doi.org/10.1007/s11695-018-3573-5
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-018-3573-5