Abstract
Introduction
Sleeve gastrectomy (SG) is a common bariatric procedure with high rates of weight regain (WR). Clinicians and patients have identified a lack of follow-up support and maladaptive lifestyle behaviours as potential causes for WR. While text message support has been shown to be effective for weight loss in non-surgical patients, it has not been investigated for reducing WR in bariatric patients.
Purpose
To determine the effectiveness of text message support in reducing weight regain following sleeve gastrectomy.
Methods
A text message intervention was designed. The effectiveness of the intervention was investigated by a randomised trial powered to detect a 15% difference in the primary outcome of percent excess weight loss (84 participants required). Secondary outcomes were the Bariatric Analysis and Reporting System (BAROS) score and patient satisfaction. Outcomes were assessed at 6 and 12 months.
Results
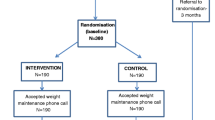
Ninety-five participants were randomised to either standard care or text message support (daily text message for 1 year). While there was no significant difference in the primary outcome at 6 or 12 months, patients who received the intervention tended to have less WR and a significantly better BAROS score at 12 months. Participants who received text message support found it beneficial, would have liked the messages to continue, and felt WR was reduced by having the text message support.
Conclusion
Text message support following SG is feasible, may reduce weight regain, improves the BAROS score and is valued by patients.
Trial Registration


Similar content being viewed by others
References
Angrisani L, Santonicola A, Iovino P, et al. Bariatric surgery worldwide 2013. Obes Surg. 2015 Oct;25(10):1822–32.
Colquitt JL, Pickett K, Loveman E, et al. Surgery for weight loss in adults. Cochrane Database Syst Rev. 2014;8
Jammu GS, Sharma R. A 7-year clinical audit of 1107 cases comparing sleeve gastrectomy, Roux-en-Y gastric bypass, and mini-gastric bypass, to determine an effective and safe bariatric and metabolic procedure. Obes Surg. 2016 May;26(5):926–32.
Sjostrom L. Review of the key results from the Swedish Obese Subjects (SOS) trial—a prospective controlled intervention study of bariatric surgery. J Intern Med. 2013;273(3):219–34.
Lauti M, Kularatna M, Hill AG, et al. Weight regain following sleeve gastrectomy—a systematic review. Obes Surg. 2016;26(6):1326–34.
Jimenez A, Casamitjana R, Flores L, et al. Long-term effects of sleeve gastrectomy and Roux-en-Y gastric bypass surgery on type 2 diabetes mellitus in morbidly obese subjects. Ann Surg. 2012;256(6):1023–9.
Brethauer SA, Aminian A, Romero-Talamas H, et al. Can diabetes be surgically cured? Long-term metabolic effects of bariatric surgery in obese patients with type 2 diabetes mellitus. Ann Surg. 2013;258(4):628–37.
Karlsson J, Taft C, Ryden A, et al. Ten-year trends in health-related quality of life after surgical and conventional treatment for severe obesity: the SOS intervention study. Int J Obesity. 2007;31(8):1248–61.
Sheppard CE, Lester EL, Chuck AW, et al. The economic impact of weight regain. Gastroenterol Res Pract. 2013;379564
Spivak H, Rubin M, Sadot E, et al. Laparoscopic sleeve gastrectomy using 42-French versus 32-French bougie: the first-year outcome. Obes Surg. 2014;24(7):1090–3.
Beumer JD, Shenfine J. Laparoscopic sleeve gastrectomy using 42-French versus 32-French bougie. Obes Surg. 2014;24(7):1094.
Cal P, Deluca L, Jakob T, et al. Laparoscopic sleeve gastrectomy with 27 versus 39 Fr bougie calibration: a randomized controlled trial. Surg Endosc. 2016;30(5):1812–5.
Hawasli A, Jacquish B, Almahmeed T, et al. Early effects of bougie size on sleeve gastrectomy outcome. Am J Surg. 2015;209(3):473–7.
Rosenthal RJ, International Sleeve Gastrectomy Expert P, Diaz AA, Arvidsson D, Baker RS, Basso N, et al. International Sleeve Gastrectomy Expert Panel Consensus Statement: best practice guidelines based on experience of >12,000 cases. Surg Obes Relat Dis 2012 Jan-Feb;8(1):8–19.
Gagner M, Hutchinson C, Rosenthal R. Fifth International Consensus Conference: current status of sleeve gastrectomy. Surg Obes Relat Dis. 2016 May;12(4):750–6.
Weiner RA, Theodoridou S, Weiner S. Failure of laparoscopic sleeve gastrectomy - further procedure? Obes Facts. 2011;4(Suppl 1):42–6.
Obeidat F, Shanti H, Mismar A, et al. The magnitude of antral resection in laparoscopic sleeve gastrectomy and its relationship to excess weight loss. Obes Surg. 2015;25(10):1928–32.
Abdallah E, El Nakeeb A, Yousef T, et al. Impact of extent of antral resection on surgical outcomes of sleeve gastrectomy for morbid obesity (a prospective randomized study). Obes Surg. 2014;24(10):1587–94.
Braghetto I, Cortes C, Herquinigo D, et al. Evaluation of the radiological gastric capacity and evolution of the BMI 2–3 years after sleeve gastrectomy. Obes Surg. 2009;19(9):1262–9. Epub 2009/06/18
Braghetto I, Csendes A, Lanzarini E, et al. Is laparoscopic sleeve gastrectomy an acceptable primary bariatric procedure in obese patients? Early and 5-year postoperative results. Surg Laparosc Endosc Percutan Tech. 2012 Dec;22(6):479–86.
Felsenreich DM, Langer FB, Kefurt R, Panhofer P, Schermann M, Beckerhinn P, et al. Weight loss, weight regain, and conversions to Roux-en-Y gastric bypass: 10-year results of laparoscopic sleeve gastrectomy. Surg Obes Relat Dis 2016 Feb 26.
Bohdjalian A, Langer FB, Shakeri-Leiden Muhler S, et al. Sleeve gastrectomy as sole and definitive bariatric procedure: 5-year results for weight loss and ghrelin. Obes Surg. 2010;20(5):535–40.
Himpens J, Dobbeleir J, Peeters G. Long-term results of laparoscopic sleeve gastrectomy for obesity. Ann Surg. 2010;252(2):319–24.
Sarela AI, Dexter SP, O'Kane M, et al. Long-term follow-up after laparoscopic sleeve gastrectomy: 8–9-year results. Surg Obes Relat Dis. 2012;8(6):679–84.
Lombardo M, Bellia A, Mattiuzzo F, et al. Frequent follow-up visits reduce weight regain in long-term management after bariatric surgery. Bariatr Surg Pract Patient Care. 2015;10(3):119–25.
Kehagias I, Spyropoulos C, Karamanakos S, et al. Efficacy of sleeve gastrectomy as sole procedure in patients with clinically severe obesity (BMI </=50 kg/m(2)). Surg Obes Relat Dis. 2013;9(3):363–9. Epub 2012/02/22
Keren D, Matter I, Lavy A. Lifestyle modification parallels to sleeve success. Obes Surg. 2014;24(5):735–40.
Lauti M, Stevenson S, Hill AG, et al. Patient perspectives about follow-up care and weight regain following sleeve gastrectomy. Obes Surg. 2016;26(11):2724–31.
Cole-Lewis H, Kershaw T. Text messaging as a tool for behavior change in disease prevention and management. Epidemiol Rev. 2010;32:56–69.
Lyzwinski LN. A systematic review and meta-analysis of mobile devices and weight loss with an intervention content analysis. J Pers Med. 2014;4(3):311–85.
Ni Mhurchu C, Whittaker R, McRobbie H, et al. Feasibility, acceptability and potential effectiveness of a mobile health (mHealth) weight management programme for New Zealand adults. BMC Obes. 2014;1:10.
Schulz KF, Altman DG, Moher D, et al. CONSORT 2010 Statement: updated guidelines for reporting parallel group randomised trials. J Clin Epidemiol. 2010 Aug;63(8):834–40.
Lemanu DP, Singh PP, Rahman H, et al. Five-year results after laparoscopic sleeve gastrectomy: a prospective study. Surg Obes Relat Dis. 2015;11(3):518–24.
Michie S, Atkins L, West R. The Behaviour Change Wheel: a guide to designing interventions. Great Britain: Silverback Publishing; 2014 2014.
Michie S, Richardson M, Johnston M, et al. The behavior change technique taxonomy (v1) of 93 hierarchically clustered techniques: building an international consensus for the reporting of behavior change interventions. Ann Behav Med. 2013 Aug;46(1):81–95.
Shaw RJ, Bosworth HB, Silva SS, et al. Mobile health messages help sustain recent weight loss. Am J Med. 2013;126(11):1002–9.
Brethauer SA, Kim J, El Chaar M, et al. Standardized outcomes reporting in metabolic and bariatric surgery. Surg Obes Relat Dis. 2015;25(4):587–606.
Oria HE, Moorehead MK. Bariatric analysis and reporting outcome system (BAROS). Obes Surg. 1998;8(5):487–99.
Oria HE, Moorehead MK. Updated Bariatric Analysis and Reporting Outcome System (BAROS). Surg Obes Relat Dis. 2009;5(1):60–6.
Montero PN, Stefanidis D, Norton HJ, et al. Reported excess weight loss after bariatric surgery could vary significantly depending on calculation method: a plea for standardization. Surg Obes Relat Dis. 2011;7(4):531–4.
van de Laar AW. The %EBMIL/%EWL double booby-trap. A comment on studies that compare the effect of bariatric surgery between heavier and lighter patients. Obes Surg. 2016;26(3):612–3.
van de Laar AW, Acherman YI. Weight loss percentile charts of large representative series: a benchmark defining sufficient weight loss challenging current criteria for success of bariatric surgery. Obes Surg. 2014;24(5):727–34.
Carter MC, Burley VJ, Cade JE. Handheld electronic technology for weight loss in overweight/obese adults. Curr Obes Rep. 2014;3(3):307–15.
Fischer HH, Fischer IP, Pereira RI, et al. Text message support for weight loss in patients with prediabetes: a randomized clinical trial. Diabetes Care. 2016;39(8):1364–70.
Fjeldsoe BS, Goode AD, Phongsavan P, et al. Evaluating the maintenance of lifestyle changes in a randomized controlled trial of the ‘Get Healthy, Stay Healthy’ program. JMIR Mhealth Uhealth. 2016;4(2):e42.
Liu F, Kong X, Cao J, et al. Mobile phone intervention and weight loss among overweight and obese adults: a meta-analysis of randomized controlled trials. Am J Epidemiol. 2015 Mar 1;181(5):337–48.
Aguilar-Martinez A, Sole-Sedeno JM, Mancebo-Moreno G, et al. Use of mobile phones as a tool for weight loss: a systematic review. J Telemed Telecare. 2014 Sep;20(6):339–49.
Jerome GJ, Dalcin A, Coughlin JW, et al. Longitudinal accuracy of web-based self-reported weights: results from the Hopkins POWER trial. J Med Internet Res. 2014;16(7):e173. Epub 2014/07/22
Funding
This study was funded by the Health Research Council of New Zealand by way of a Clinical Research Training Fellowship (15/008) awarded to the first author.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
It was approved by the Northern B Health and Disability Ethics Committee in December 2014 (reference 14/NTB/206).
Conflict of Interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Lauti, M., Kularatna, M., Pillai, A. et al. A Randomised Trial of Text Message Support for Reducing Weight Regain Following Sleeve Gastrectomy. OBES SURG 28, 2178–2186 (2018). https://doi.org/10.1007/s11695-018-3176-1
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-018-3176-1