Abstract
Summary
This research is a cross-sectional study based on the participants aged 50 years and older from National Health and Nutrition Examination Survey (NHANES) database. Poor sleep patterns were associated with lower bone mineral density (BMD) and a higher risk of osteoporosis, especially among older individuals or females.
Introduction
Accumulated evidence demonstrates that sleep duration, which is one aspect of sleep pattern, is associated with the risk of osteoporosis. However, the related studies on the association between sleep patterns and the risk of osteoporosis were limited. Therefore, this research aims to investigate the association of sleep patterns with BMD and the risk of osteoporosis among individuals aged 50 years and older.
Methods
Participants aged ≥ 50 years from the NHANES database were included in the present study. The diagnosis of osteoporosis was based on the results of BMD testing. Moreover, all the participants were divided into different sleep pattern groups according to nocturnal sleep duration and bedtime. In addition, this study used multivariate linear regression models to evaluate the association between sleep patterns and BMD and exploited multiple logistic regression models to investigate the odds ratios (ORs) for osteoporosis.
Results
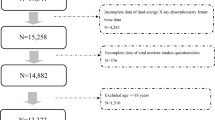
Finally, 1,865 individuals (non-osteoporosis: N = 1,713; osteoporosis: N = 152) aged over 50 years old with complete data were analyzed. The results of multivariate linear regression models showed that individuals with normal sleep duration/later bedtime or long sleep duration/later bedtime had lower femoral BMD than those with normal sleep duration/usual bedtime. Moreover, subjects with long sleep duration/later bedtime had a higher risk of osteoporosis compared with those with normal sleep duration/usual bedtime. In addition, subgroup analyses revealed the association of sleep patterns with BMD and the risk of osteoporosis appeared to be more pronounced among individuals aged ≥ 65 years or females.
Conclusion
This study demonstrated that sleep patterns are associated with BMD and the risk of osteoporosis. Poor sleep patterns contribute to decreased bone mass and the increased risk of osteoporosis. Therefore, a healthy sleep pattern is favorable for the prevention of osteoporosis.


Similar content being viewed by others
Data availability
All data were extracted from National Health and Nutrition Examination Survey (NHANES) 2017–2018 database. The detailed information was provided on the NHANES website.
Code availability
All analyses were performed with R software, V.4.0.3 [R: a language and statistical computing environment (program). Vienna, Austria: R Foundation for Statistical Computing, 2016] and EmpowerStats (http://www.empowerstats. com). The figures were generated using Adobe Photoshop (https://www.adobe.com/products/photoshop.html) or Origin 2021 (https://www.originlab.com/).
References
Ensrud KE, Crandall CJ (2017) Osteoporosis. Annals of internal medicine 167:Itc17-itc32
Wright NC, Looker AC, Saag KG, Curtis JR, Delzell ES, Randall S, Dawson-Hughes B (2014) The recent prevalence of osteoporosis and low bone mass in the United States based on bone mineral density at the femoral neck or lumbar spine. Journal of bone and mineral research: the official journal of the American Society for Bone and Mineral Research 29:2520–2526
Lu J, Ren Z, Liu X, Xu YJ, Liu Q (2019) Osteoporotic fracture guidelines and medical education related to the clinical practices: a nationwide survey in China. Orthop Surg 11:569–577
Hernlund E, Svedbom A, Ivergård M, Compston J, Cooper C, Stenmark J, McCloskey EV, Jönsson B, Kanis JA (2013) Osteoporosis in the European Union: medical management, epidemiology and economic burden. A report prepared in collaboration with the International Osteoporosis Foundation (IOF) and the European Federation of Pharmaceutical Industry Associations (EFPIA). Archives of osteoporosis 8:136
Si L, Winzenberg TM, Jiang Q, Chen M, Palmer AJ (2015) Projection of osteoporosis-related fractures and costs in China: 2010–2050. Osteoporosis international: a journal established as result of cooperation between the European Foundation for Osteoporosis and the National Osteoporosis Foundation of the USA 26:1929–1937
Johnston CB, Dagar M (2020) Osteoporosis in older adults. Med Clin North Am 104:873–884
Appelman-Dijkstra NM, Papapoulos SE (2015) Modulating bone resorption and bone formation in opposite directions in the treatment of postmenopausal osteoporosis. Drugs 75:1049–1058
Moradi S, Shab-Bidar S, Alizadeh S, Djafarian K (2017) Association between sleep duration and osteoporosis risk in middle-aged and elderly women: a systematic review and meta-analysis of observational studies. Metabolism: Clinical and experimental 69:199–206
Wang D, Ruan W, Peng Y, Li W (2018) Sleep duration and the risk of osteoporosis among middle-aged and elderly adults: a dose-response meta-analysis. Osteoporosis international: a journal established as result of cooperation between the European Foundation for Osteoporosis and the National Osteoporosis Foundation of the USA 29:1689–1695
Ochs-Balcom HM, Hovey KM, Andrews C et al (2020) Short sleep is associated with low bone mineral density and osteoporosis in the women’s health initiative. Journal of bone and mineral research: the official journal of the American Society for Bone and Mineral Research 35:261–268
Lucchesi C, Baldacci F, Cafalli M, Dini E, Giampietri L, Siciliano G, Gori S (2016) Fatigue, sleep-wake pattern, depressive and anxiety symptoms and body-mass index: analysis in a sample of episodic and chronic migraine patients. Neurological sciences: official journal of the Italian Neurological Society and of the Italian Society of Clinical Neurophysiology 37:987–989
Zhang S, Xie L, Yu H, Zhang W, Qian B (2019) Association between nighttime-daytime sleep patterns and chronic diseases in Chinese elderly population: a community-based cross-sectional study. BMC Geriatr 19:124
Tian Y, Shen L, Wu J et al (2015) Sleep duration and timing in relation to osteoporosis in an elderly Chinese population: a cross-sectional analysis in the Dongfeng-Tongji cohort study. Osteoporosis international: a journal established as result of cooperation between the European Foundation for Osteoporosis and the National Osteoporosis Foundation of the USA 26:2641–2648
CDC National Health and Nutrition Examination Survey 2017–2018. https://wwwn.cdc.gov/nchs/nhanes/continuousnhanes/default.aspx?BeginYear=2017 Accessed March 29 2021
CDC NHANES 2017–2018 Brochures and Consent Documents. https://wwwn.cdc.gov/nchs/nhanes/ContinuousNhanes/Documents.aspx?BeginYear=2017 Accessed Mar 29 2021
CDC NHANES Body Composition Procedures Manual. https://wwwn.cdc.gov/nchs/data/nhanes/2017-2018/manuals/Body_Composition_Procedures_Manual_2018.pdf Accessed Mar 29 2021
Looker AC, Orwoll ES, Johnston CC Jr, Lindsay RL, Wahner HW, Dunn WL, Calvo MS, Harris TB, Heyse SP (1997) Prevalence of low femoral bone density in older U.S. adults from NHANES III. Journal of bone and mineral research: the official journal of the American Society for Bone and Mineral Research 12:1761–1768
Hirshkowitz M, Whiton K, Albert SM et al (2015) National Sleep Foundation’s sleep time duration recommendations: methodology and results summary. Sleep Health 1:40–43
Compston JE, McClung MR, Leslie WD (2019) Osteoporosis. Lancet (London, England) 393:364–376
Weaver CM, Gordon CM, Janz KF, Kalkwarf HJ, Lappe JM, Lewis R, O’Karma M, Wallace TC, Zemel BS (2016) The National Osteoporosis Foundation’s position statement on peak bone mass development and lifestyle factors: a systematic review and implementation recommendations. Osteoporosis international: a journal established as result of cooperation between the European Foundation for Osteoporosis and the National Osteoporosis Foundation of the USA 27:1281–1386
Compston J, Cooper A, Cooper C et al (2017) UK clinical guideline for the prevention and treatment of osteoporosis. Arch Osteoporos 12:43
Zhu K, Prince RL (2015) Lifestyle and osteoporosis. Current Osteoporosis Reports 13:52–59
Briot K, Roux C, Thomas T et al (2018) 2018 update of French recommendations on the management of postmenopausal osteoporosis. Joint Bone Spine 85:519–530
Adler RA (2018) Update on osteoporosis in men. Best Pract Res Clin Endocrinol Metab 32:759–772
Santhi N, Lazar AS, McCabe PJ, Lo JC, Groeger JA, Dijk DJ (2016) Sex differences in the circadian regulation of sleep and waking cognition in humans. Proc Natl Acad Sci USA 113:E2730-2739
Khosla S, Monroe DG (2018) Regulation of bone metabolism by sex steroids. Cold Spring Harbor perspectives in medicine 8
Boyle WJ, Simonet WS, Lacey DL (2003) Osteoclast differentiation and activation. Nature 423:337–342
Hollander LE, Freeman EW, Sammel MD, Berlin JA, Grisso JA, Battistini M (2001) Sleep quality, estradiol levels, and behavioral factors in late reproductive age women. Obstet Gynecol 98:391–397
Sharan K, Lewis K, Furukawa T, Yadav VK (2017) Regulation of bone mass through pineal-derived melatonin-MT2 receptor pathway. Journal of pineal research 63
Maria S, Samsonraj RM, Munmun F, et al. (2018) Biological effects of melatonin on osteoblast/osteoclast cocultures, bone, and quality of life: implications of a role for MT2 melatonin receptors, MEK1/2, and MEK5 in melatonin-mediated osteoblastogenesis. Journal of pineal research 64
Greendale GA, Witt-Enderby P, Karlamangla AS, Munmun F, Crawford S, Huang M, Santoro N (2020) Melatonin patterns and levels during the human menstrual cycle and after menopause. Journal of the Endocrine Society 4:bvaa115
Wu AH, Wang R, Koh WP, Stanczyk FZ, Lee HP, Yu MC (2008) Sleep duration, melatonin and breast cancer among Chinese women in Singapore. Carcinogenesis 29:1244–1248
Reutrakul S, Hood MM, Crowley SJ, Morgan MK, Teodori M, Knutson KL, Van Cauter E (2013) Chronotype is independently associated with glycemic control in type 2 diabetes. Diabetes Care 36:2523–2529
López-Baena MT, Pérez-Roncero GR, Pérez-López FR, Mezones-Holguín E, Chedraui P (2020) Vitamin D, menopause, and aging: quo vadis? Climacteric: the journal of the International Menopause Society 23:123–129
Araujo AB, Wittert GA (2011) Endocrinology of the aging male. Best Pract Res Clin Endocrinol Metab 25:303–319
Yan M, Fu Z, Qin T, Wu N, Lv Y, Wei Q, Jiang H, Yin P (2018) Associations of sleep duration and prediabetes prevalence in a middle-aged and elderly Chinese population with regard to age and hypertension: The China Health and Retirement Longitudinal Study baseline survey. J Diabetes 10:847–856
Chan CMH, Siau CS, Wong JE, Wee LH, Jamil NA, Hoe VCW (2021) Prevalence of insufficient sleep and its associated factors among working adults in Malaysia. Nature and science of sleep 13:1109–1116
Ancoli-Israel S, Ayalon L, Salzman C (2008) Sleep in the elderly: normal variations and common sleep disorders. Harv Rev Psychiatry 16:279–286
Eastell R, O’Neill TW, Hofbauer LC, Langdahl B, Reid IR, Gold DT, Cummings SR (2016) Postmenopausal osteoporosis Nature reviews Disease primers 2:16069
Khosla S, Hofbauer LC (2017) Osteoporosis treatment: recent developments and ongoing challenges. Lancet Diabetes Endocrinol 5:898–907
Acknowledgements
We would like to express our gratitude to American Journal Experts (https://www.aje.com/) for the language editing services provided.
Funding
This study was supported by the National Natural Science Foundation of China (81874017, 81960403, and 82060405); Natural Science Foundation of Gansu Province of China (20JR5RA320); and Cuiying Scientific and Technological Innovation Program of Lanzhou University Second Hospital (CY2017-ZD02).
Author information
Authors and Affiliations
Contributions
YT and SW contributed equally to this work. YT and BG contributed the central idea, and YT and SW analyzed most of the data. YT wrote the initial draft of the paper. The remaining authors contributed to refining the ideas, carrying out additional analyses, and finalizing this paper.
Corresponding author
Ethics declarations
Ethics approval
The ethics review board of the National Center for Health Statistics approved the study. The detailed information was provided on the NHANES website.
Consent to participate
Informed consent was obtained from all study participants. The detailed information was provided on the NHANES website.
Consent for publication
Not applicable.
Conflict of interest
None.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Tang, Y., Wang, S., Yi, Q. et al. Sleep pattern and bone mineral density: a cross-sectional study of National Health and Nutrition Examination Survey (NHANES) 2017–2018. Arch Osteoporos 16, 157 (2021). https://doi.org/10.1007/s11657-021-01025-1
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s11657-021-01025-1