Abstract
Purpose
Prior reports have examined the relationship between obstructive sleep apnea (OSA) and the mortality rate of lung cancer. However, the findings remain controversial. The present meta-analysis was performed to assess the relationship between OSA and increased risk of mortality in patients with lung cancer.
Methods
PubMed, Web of Science, and Embase were systematically searched for the correlative studies. Data were analyzed and pooled to evaluate odds ratios (ORs) of lung cancer mortality related to OSA.
Results
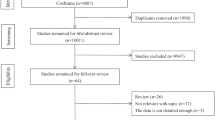
From 249 identified studies, 3 met inclusion criteria and were analyzed, including 67 patients with lung cancer and comorbid OSA and 45 patients with lung cancer and no OSA. The meta-analysis indicated that OSA was not significantly correlated with mortality rate in lung cancer (OR = 2.005, 95% CI = 0.703 to 5.715, z = 1.30, p = 0.193). There was no significant publication bias according to Begg’s tests (p = 0.296) and Egger’s tests (p = 0.097).
Conclusion
This meta-analysis suggests that OSA is not significantly correlated with the mortality rate in lung cancer.




Similar content being viewed by others
Data availability
All data generated or analyzed during this study are included in this published article.
References
Young T, Palta M, Dempsey J, Skatrud J, Weber S, Badr S (1993) The occurrence of sleep-disordered breathing among middle-aged adults. N Engl J Med 328(17):1230–1235
Lindberg E, Gislason T (2000) Epidemiology of sleep-related obstructive breathing. Sleep Med Rev 4(5):411–433
Floras JS (2018) Sleep apnea and cardiovascular disease: an enigmatic risk factor. Circ Res 122(12):1741–1764
Peppard PE, Young T, Palta M, Skatrud J (2000) Prospective study of the association between sleep-disordered breathing and hypertension. N Engl J Med 342(19):1378–1384
Reutrakul S, Mokhlesi B (2017) Obstructive sleep apnea and diabetes: a state of the art review. Chest 152(5):1070–1086
Leng Y, McEvoy CT, Allen IE, Yaffe K (2017) Association of sleep-disordered breathing with cognitive function and risk of cognitive impairment: a systematic review and meta-analysis. JAMA Neurol 74(10):1237–1245
Moyer CA, Sonnad SS, Garetz SL, Helman JI, Chervin RD (2001) Quality of life in obstructive sleep apnea: a systematic review of the literature. Sleep Med 2(6):477–491
Nieto FJ, Peppard PE, Young T, Finn L, Hla KM, Farre R (2012) Sleep-disordered breathing and cancer mortality: results from the Wisconsin Sleep Cohort Study. Am J Respir Crit Care Med 186(2):190–194
Marshall NS, Wong KK, Cullen SR, Knuiman MW, Grunstein RR (2014) Sleep apnea and 20-year follow-up for all-cause mortality, stroke, and cancer incidence and mortality in the Busselton Health Study cohort. J Clin Sleep Med 10(4):355–362
Almendros I, Wang Y, Becker L, Lennon FE, Zheng J, Coats BR, Schoenfelt KS, Carreras A, Hakim F, Zhang SX, Farre R, Gozal D (2014) Intermittent hypoxia-induced changes in tumor-associated macrophages and tumor malignancy in a mouse model of sleep apnea. Am J Respir Crit Care Med 189(5):593–601
Almendros I, Khalyfa A, Trzepizur W, Gileles-Hillel A, Huang L, Akbarpour M, Andrade J, Farre R, Gozal D (2016) Tumor cell malignant properties are enhanced by circulating exosomes in sleep apnea. Chest 150(5):1030–1041
Almendros I, Montserrat JM, Torres M, Bonsignore MR, Chimenti L, Navajas D, Farre R (2012) Obesity and intermittent hypoxia increase tumor growth in a mouse model of sleep apnea. Sleep Med 13(10):1254–1260
Bray F, Ferlay J, Soerjomataram I, Siegel RL, Torre LA, Jemal A (2018) Global cancer statistics 2018: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin 68(6):394–424
Liu Y, Lao M, Chen J, Lu M, Luo S, Ou Q, Luo Z, Yuan P, Chen J, Ye G, Gao X (2020) Short-term prognostic effects of circulating regulatory T-cell suppressive function and vascular endothelial growth factor level in patients with non-small cell lung cancer and obstructive sleep apnea. Sleep Med 70:88–96
Liu W, Luo M, Fang YY, Wei S, Zhou L, Liu K (2019) Relationship between occurrence and progression of lung cancer and nocturnal intermittent hypoxia, apnea and daytime sleepiness. Curr Med Sci 39(4):568–575
Huang HY, Lin SW, Chuang LP, Wang CL, Sun MH, Li HY, Chang CJ, Chang SC, Yang CT, Chen NH (2020) Severe OSA associated with higher risk of mortality in stage III and IV lung cancer. J Clin Sleep Med 16(7):1091–1098
Seijo LM, Perez-Warnisher MT, Giraldo-Cadavid LF, Oliveros H, Cabezas E, Troncoso MF, Gomez T, Melchor R, Pinillos EJ, El Hachem A, Gotera C, Rodriguez P, Gonzalez-Mangado N, Peces-Barba G (2019) Obstructive sleep apnea and nocturnal hypoxemia are associated with an increased risk of lung cancer. Sleep Med 63:41–45
Moher D, Liberati A, Tetzlaff J, Altman DG (2009) Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. BMJ 339:332–336
Stroup DF, Berlin JA, Morton SC, Olkin I, Williamson GD, Rennie D, Moher D, Becker BJ, Sipe TA, Thacker SB (2000) Meta-analysis of observational studies in epidemiology: a proposal for reporting. Meta-analysis Of Observational Studies in Epidemiology (MOOSE) group. Jama 283(15):2008–2012
Li L, Lu J, Xue W, Wang L, Zhai Y, Fan Z, Wu G, Fan F, Li J, Zhang C, Zhang Y, Zhao J (2017) Target of obstructive sleep apnea syndrome merge lung cancer: based on big data platform. Oncotarget 8(13):21567–21578
Campos-Rodriguez F, Martinez-Garcia MA, Martinez M, Duran-Cantolla J, Pena Mde L, Masdeu MJ, Gonzalez M, Campo F, Gallego I, Marin JM, Barbe F, Montserrat JM, Farre R (2013) Association between obstructive sleep apnea and cancer incidence in a large multicenter Spanish cohort. Am J Respir Crit Care Med 187(1):99–105
Chang WP, Liu ME, Chang WC, Yang AC, Ku YC, Pai JT, Lin YW, Tsai SJ (2014) Sleep apnea and the subsequent risk of breast cancer in women: a nationwide population-based cohort study. Sleep Med 15(9):1016–1020
Justeau G, Gerves-Pinquie C, Le Vaillant M, Trzepizur W, Meslier N, Goupil F, Pigeanne T, Launois S, Leclair-Visonneau L, Masson P, Bizieux-Thaminy A, Humeau MP, Gosselin C, Blanchard M, Urban T, Gagnadoux F, Group ES (2020) Association between nocturnal hypoxemia and cancer incidence in patients investigated for OSA: data from a large multicenter french cohort. Chest
Kendzerska T, Leung RS, Hawker G, Tomlinson G, Gershon AS (2014) Obstructive sleep apnea and the prevalence and incidence of cancer. Can Med Assoc J 186(13):985–992
Martinez-Garcia MA, Campos-Rodriguez F, Duran-Cantolla J, de la Pena M, Masdeu MJ, Gonzalez M, Del Campo F, Serra PC, Valero-Sanchez I, Ferrer MJ, Marin JM, Barbe F, Martinez M, Farre R, Montserrat JM, Spanish Sleep N (2014) Obstructive sleep apnea is associated with cancer mortality in younger patients. Sleep Med 15(7):742–748
Martinez-Garcia MA, Campos-Rodriguez F, Catalan-Serra P, Soler-Cataluna JJ, Almeida-Gonzalez C, De la Cruz MI, Duran-Cantolla J, Montserrat JM (2012) Cardiovascular mortality in obstructive sleep apnea in the elderly: role of long-term continuous positive airway pressure treatment: a prospective observational study. Am J Respir Crit Care Med 186(9):909–916
Zhang XB, Peng LH, Lyu Z, Jiang XT, Du YP (2017) Obstructive sleep apnoea and the incidence and mortality of cancer: a meta-analysis. Eur J Cancer Care 26(2). https://doi.org/10.1111/ecc.12427
Akbarpour M, Khalyfa A, Qiao Z, Gileles-Hillel A, Almendros I, Farre R, Gozal D (2017) Altered CD8+ T-cell lymphocyte function and TC1 cell stemness contribute to enhanced malignant tumor properties in murine models of sleep apnea. Sleep 40(2). https://doi.org/10.1093/sleep/zsw040
Li L, Ren F, Qi C, Xu L, Fang Y, Liang M, Feng J, Chen B, Ning W, Cao J (2018) Intermittent hypoxia promotes melanoma lung metastasis via oxidative stress and inflammation responses in a mouse model of obstructive sleep apnea. Respir Res 19(1):28
Funding
This work was supported by grant from Science and Technology Major Project of Fujian Province (2017YZ0001-2) and National Natural Science Foundation of China (81900088, 81870074). The funding bodies played no role in the design of the study and collection, analysis, and interpretation of data and in writing the manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethics approval and consent to participate
All analyses were based on previous published studies; thus, no ethical approval and patient consent are required.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Chen, MX., Chen, LD., Zeng, AM. et al. Obstructive sleep apnea and the risk of mortality in patients with lung cancer: a meta-analysis. Sleep Breath 26, 559–566 (2022). https://doi.org/10.1007/s11325-021-02416-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11325-021-02416-x