Abstract
Objective
To clarify the usefulness of a personalized three-dimensional (3D) printed model of the kidney for preoperative education among patients who underwent robot-assisted partial nephrectomy (RAPN).
Methods
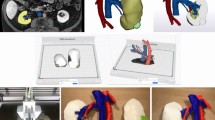
Twenty-nine cases of patients who planned to undergo RAPN and 19 of their families participated in this study. A three-dimensional model consisting of the kidney, tumors, ureter, inferior vena cava, and abdominal aorta in each case was generated using a Z Printer 450 based on the findings of preoperative enhanced CT. After preoperative education using enhanced CT and a 3D-printed model, two anatomy-related issues, three tumor-related issues, and two surgical procedure-related issues were evaluated using a visual analogue scale.
Results
The median age of all participants was 64 years old. The rate in male patients was significantly higher than that in families. In all three issues in patients and in two of three issues in families, scores in the 3D model were significantly higher than those in CT. In all issues in CT, scores of patients 64 years old or younger were higher than those of patients 65 years old or higher. On the other hand, no significant difference was found in the 3D model for scores on two of three issues regardless of the age of participants.
Conclusion
Our data indicate that the personalized 3D printed model of the kidney is useful for preoperative education among patients and their families who underwent RAPN, especially in elderly people.


Similar content being viewed by others
References
Van Poppel H, Da Pozzo L, Albrecht W et al (2011) A prospective, randomised EORTC intergroup phase 3 study comparing the oncologic outcome of elective nephron-sparing surgery and radical nephrectomy for low-stage renal cell carcinoma. Eur Urol 59(4):543–552. https://doi.org/10.1016/j.eururo.2010.12.013.
Zini L, Perrotte P, Capitanio U et al (2009) Radical versus partial nephrectomy: effect on overall and noncancer mortality. Cancer 115(7):1465–1471. https://doi.org/10.1002/cncr.24035
MacLennan S, Imamura M, Lapitan MC et al (2012) Systematic review of perioperative and quality-of-life outcomes following surgical management of localised renal cancer. Eur Urol 62(6):1097–1117. https://doi.org/10.1016/j.eururo.2012.07.028.
Choi JE, You JH, Kim DK et al (2015) Comparison of perioperative outcomes between robotic and laparoscopic partial nephrectomy: a systematic review and meta-analysis. Eur Urol 67(5):891–901. https://doi.org/10.1016/j.eururo.2014.12.028.
Levine JP, Patel A, Saadeh PB et al (2012) Computer-aided design and manufacturing in craniomaxillofacial surgery: the new state of the art. J Craniofac Surg 23(1):288–293. https://doi.org/10.1097/SCS.0b013e318241ba92
Bilhan H, Arat S, Mumcu E et al (2012) Precision of implant placement with stereolithographic templates: a pilot in vitro study. J Oral Implantol 38(5):569–574. https://doi.org/10.1563/AAID-JOI-D-10-00109
Rohner D, Guijarro-Martinez R, Bucher P et al (2013) Importance of patient-specific intraoperative guides in complex maxillofacial reconstruction. J Craniomaxillofac Surg 41(5):382–390. https://doi.org/10.1016/j.jcms.2012.10.021.
Silverstein JL, Maddex MM, Dorsey P et al (2014) Physical models of renal malignancies using standard cross-sectional imaging and 3-dimensional printers: a pilot study. Urology 84(2):268–272. https://doi.org/10.1016/j.urology.2014.03.042.
Zhang Y, Ge HW, Li NC et al (2016) Evaluation of three-dimensional printing for laparoscopic partial nephrectomy of renal tumors: a preliminary report. World J Urol 34(4):533–537. https://doi.org/10.1007/s00345-015-1530-7.
Bernhard JC, Isotani S, Matsugasumi T et al (2016) Personalized 3D printed model of kidney and tumor anatomy: a useful tool for patient education. World J Urol 34(4):337–345. https://doi.org/10.1007/s00345-015-1632-2.
Knoedler M, Feibus AH, Lange A et al (2015) Individualized physical 3-dimensional kidney tumor models constructed from 3-dimensional printers result in improved trainee anatomic understanding. Urology 85(6):1257–1261. https://doi.org/10.1016/j.urology.2015.02.053
Rundstedt FC, Scovell JM, Agrawal S et al (2017) Utility of patient-specific silicone renal models for planning and rehearsal of complex tumour resections prior to robot-assisted laparoscopic partial nephrectomy. BJU Int 119(4):598–604. https://doi.org/10.1111/bju.13712.
Thompson RH, Atwell T, Schmit G et al (2015) Comparison of partial nephrectomy and percutaneous ablation for cT1 renal masses. Eur Urol 67(2):252–259. https://doi.org/10.1016/j.eururo.2014.07.021.
Fink C, Diener MK, Bruckner T et al (2013) Impact of preoperative patient education on prevention of postoperative complications after major visceral surgery: study protocol for a randomized controlled trial (PEDUCAT trial). Trials 14:271. https://doi.org/10.1186/1745-6215-14-271
Keulers BJ, Scheltinga MR, Houterman S et al (2008) Surgeons underestimate their patients’ desire for preoperative information. World J Surg 32(6):964–970. https://doi.org/10.1007/s00268-008-9581-1
Watson RA (2014) A low-cost surgical application of additive fabrication. J Surg Educ 71(1):14–17. https://doi.org/10.1016/j.jsurg.2013.10.012
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflicts of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Teishima, J., Takayama, Y., Iwaguro, S. et al. Usefulness of personalized three-dimensional printed model on the satisfaction of preoperative education for patients undergoing robot-assisted partial nephrectomy and their families. Int Urol Nephrol 50, 1061–1066 (2018). https://doi.org/10.1007/s11255-018-1881-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11255-018-1881-2