Abstract
Purpose
To fill the gap in knowledge about associations of health-related quality of life (HRQoL) with comorbid diabetes mellitus (DM), hypertension (HTN), and/or mild cognitive impairment (MCI) in the elderly, we explored associations of comorbid DM, HTN, and/or MCI with HRQoL.
Methods
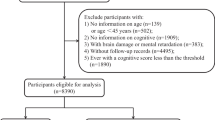
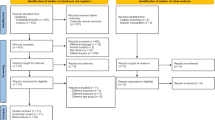
Data for this study were from a population-based cross-sectional survey of elderly Taiwanese (≥ 65 years old). Participants (N = 4,634; 47.9% male) were categorized into eight chronic-illness groups: DM only (n = 224); HTN only (n = 1226); DM and HTN (n = 365); MCI only (n = 497); DM and MCI (n = 58); HTN and MCI (n = 303); DM, HTN, and MCI (n = 101); and none (healthy; n = 1860). Associations were examined between the eight chronic-illness groups and HRQoL (measured by EQ-5D scores) using binary logistic regression analyses and generalized linear models adjusted for covariates. Index scores were calculated from EQ-5D scores using Taiwan’s general population-preference weights.
Results
Compared to the healthy group, after adjusting covariates, MCI alone or with other comorbidities was significantly, negatively associated with HRQoL. Among all chronic-illness groups, comorbid DM, HTN, and MCI exhibited the lowest HRQoL. After adjusting covariates, between-group odds ratios for index scores were significant when comparing comorbid DM and MCI to DM only, comparing comorbid HTN and MCI to HTN only and comorbid DM, comparing HTN and MCI to comorbid DM and HTN, suggesting that MCI additively affects HRQoL.
Conclusions
HRQoL of older Taiwanese adults was negatively associated with having MCI. Thus, clinicians managing older persons with chronic illnesses should assess their cognitive function to identify high-risk groups needing HRQoL assistance.
Similar content being viewed by others
References
Department of Statistics, Ministry of Interior, Taiwan. (2018). Monthly bulletin of interior statistics: 1.5 Population by age of 0–14, 15–64, 65+ and by 6-year age group [Data file]. Retrieved from https://www.moi.gov.tw/files/site_stuff/321/1/month/m1-05.xls.
National Development Council, Taiwan. (2016). Population projections for R.O.C. (Taiwan): 2016–2060. Retrieved from https://www.ndc.gov.tw/en/cp.aspx?n=2E5DCB04C64512CC.
Eshkoor, S. A., Hamid, T. A., Mun, C. Y., & Ng, C. K. (2015). Mild cognitive impairment and its management in older people. Clinical Interventions in Aging, 10, 687–693. https://doi.org/10.2147/CIA.S73922.
Sun, Y., Lee, H. J., Yang, S. C., Chen, T. F., Lin, K. N., Lin, C. C., et al. (2014). A nationwide survey of mild cognitive impairment and dementia, including very mild dementia, in Taiwan. PLoS ONE, 9(6), e100303. https://doi.org/10.1371/journal.pone.0100303.
Lonie, J. A., Parra-Rodriguez, M. A., Tierney, K. M., Herrmann, L. L., Donaghey, C., O’Carroll, R. E., et al. (2010). Predicting outcome in mild cognitive impairment: 4-year follow-up study. The British Journal of Psychiatry, 197(2), 135–140. https://doi.org/10.1192/bjp.bp.110.077958.
Ryuno, H., Kamide, K., Gondo, Y., Kabayama, M., Oguro, R., Nakama, C., et al. (2017). Longitudinal association of hypertension and diabetes mellitus with cognitive functioning in a general 70-year-old population: The SONIC study. Hypertension Research, 40(7), 665–670. https://doi.org/10.1038/hr.2017.15.
Hassing, L. B., Hofer, S. M., Nilsson, S. E., Berg, S., Pedersen, N. L., McClearn, G., et al. (2004). Comorbid type 2 diabetes mellitus and hypertension exacerbates cognitive decline: Evidence from a longitudinal study. Age and Ageing, 33(4), 355–361.
Hazari, M. A. H., Reddy, B. R., Uzma, N., & Kumar, B. S. (2015). Cognitive impairment in type 2 diabetes mellitus. International Journal of Diabetes Mellitus, 3(1), 19–24. https://doi.org/10.1016/j.ijdm.2011.01.001.
Li, J. Q., Tan, L., Wang, H. F., Tan, M. S., Tan, L., Xu, W., et al. (2015). Risk factors for predicting progression from mild cognitive impairment to Alzheimer’s disease: A systematic review and meta-analysis of cohort studies. Journal of Neurology, Neurosurgery, and Psychiatry, 87(5), 476–484. https://doi.org/10.1136/jnnp-2014-310095.
Chi, M. J., Lee, C. Y., & Wu, S. C. (2011). The prevalence of chronic conditions and medical expenditures of the elderly by chronic condition indicator (CCI). Archives of Gerontology and Geriatrics, 52(3), 284–289. https://doi.org/10.1016/j.archger.2010.04.017.
Musekamp, G., Bengel, J., Schuler, M., & Faller, H. (2016). Improved self-management skills predict improvements in quality of life and depression in patients with chronic disorders. Patient Education and Counseling, 99(8), 1355–1361. https://doi.org/10.1016/j.pec.2016.03.022.
Kirkman, M. S., Briscoe, V. J., Clark, N., Florez, H., Haas, L. B., Halter, J. B., et al. (2012). Diabetes in older adults. Diabetes Care, 35(12), 2650–2664. https://doi.org/10.2337/dc12-1801.
Poljičanin, T., Ajduković, D., Šekerija, M., Pibernik-Okanović, M., Metelko, Ž, & Mavrinac, G. V. (2010). Diabetes mellitus and hypertension have comparable adverse effects on health-related quality of life. BMC Public Health, 10(1), 12. https://doi.org/10.1186/1471-2458-10-12.
Trevisol, D. J., Moreira, L. B., Kerkhoff, A., Fuchs, S. C., & Fuchs, F. D. (2011). Health-related quality of life and hypertension: A systematic review and meta-analysis of observational studies. Journal of Hypertension, 29(2), 179–188. https://doi.org/10.1097/HJH.0b013e328340d76f.
Solli, O., Stavem, K., & Kristiansen, I. S. (2010). Health-related quality of life in diabetes: The associations of complications with EQ-5D scores. Health and Quality of Life Outcomes, 8(1), 18. https://doi.org/10.1186/1477-7525-8-18.
Green, A. J., Bazata, D. D., Fox, K. M., & Grandy, S. (2012). Quality of life, depression, and healthcare resource utilization among adults with type 2 diabetes mellitus and concomitant hypertension and obesity: A prospective survey. Cardiology Research and Practice. 2012. https://doi.org/10.1155/2012/404107.
Wee, H. L., Cheung, Y. B., Li, S. C., Fong, K. Y., & Thumboo, J. (2005). The impact of diabetes mellitus and other chronic medical conditions on health-related Quality of Life: Is the whole greater than the sum of its parts? Health and Quality of Life Outcomes, 3(1), 2.
Bárrios, H., Narciso, S., Guerreiro, M., Maroco, J., Logsdon, R., & De Mendonça, A. (2013). Quality of life in patients with mild cognitive impairment. Aging & Mental Health, 17(3), 287–292. https://doi.org/10.1080/13607863.2012.747083.
Apostolova, L. G., & Cummings, J. L. (2008). Neuropsychiatric manifestations in mild cognitive impairment: A systematic review of the literature. Dementia and Geriatric Cognitive Disorders, 25(2), 115–126. https://doi.org/10.1159/000112509.
Jekel, K., Damian, M., Wattmo, C., Hausner, L., Bullock, R., Connelly, P. J., et al. (2015). Mild cognitive impairment and deficits in instrumental activities of daily living: A systematic review. Alzheimer’s Research & Therapy, 7(1), 17. https://doi.org/10.1186/s13195-015-0099-0.
Teng, E., Tassniyom, K., & Lu, P. H. (2012). Reduced quality-of-life ratings in mild cognitive impairment: Analyses of subject and informant responses. The American Journal of Geriatric Psychiatry, 20(12), 1016–1025. https://doi.org/10.1097/JGP.0b013e31826ce640.
McKhann, G. M., Knopman, D. S., Chertkow, H., Hyman, B. T., Jack, C. R., Kawas, C. H., et al. (2011). The diagnosis of dementia due to Alzheimer’s disease: Recommendations from the National Institute on Aging-Alzheimer’s Association workgroups on diagnostic guidelines for Alzheimer’s disease. Alzheimer’s & Dementia, 7(3), 263–269. https://doi.org/10.1016/j.jalz.2011.03.005.
Lee, H. Y., Hung, M. C., Hu, F. C., Chang, Y. Y., Hsieh, C. L., & Wang, J. D. (2013). Estimating quality weights for EQ-5D (EuroQol-5 dimensions) health states with the time trade-off method in Taiwan. Journal of the Formosan Medical Association, 112(11), 699–706. https://doi.org/10.1016/j.jfma.2012.12.015.
Johansson, M. M., Marcusson, J., & Wressle, E. (2012). Cognition, daily living, and health-related quality of life in 85-year-olds in Sweden. Aging, Neuropsychology, and Cognition, 19(3), 421–432. https://doi.org/10.1080/13825585.2011.629290.
Chen, H. M., & Chen, C. M. (2017). Factors associated with quality of life among older adults with chronic disease in Taiwan. International Journal of Gerontology, 11(1), 12–15. doi: 0.1016/j.ijge.2016.07.002.
Yang, K.-F., Hsu, C.-H., Tang, Y.-J., & Kung, C.-C. (2012). Correlation among activities of daily living, quality of life, and sense of well-being in elderly community dwellers. Taiwan Geriatrics & Gerontology, 7(4), 217–232.
Lawson, R. A., Yarnall, A. J., Duncan, G. W., Khoo, T. K., Breen, D. P., Barker, R. A., et al. (2014). Severity of mild cognitive impairment in early Parkinson’s disease contributes to poorer quality of life. Parkinsonism & Related Disorders, 20(10), 1071–1075. https://doi.org/10.1016/j.parkreldis.2014.07.004.
Beerens, H. C., Zwakhalen, S. M., Verbeek, H., Ruwaard, D., & Hamers, J. P. (2013). Factors associated with quality of life of people with dementia in long-term care facilities: A systematic review. International Journal of Nursing Studies, 50(9), 1259–1270. https://doi.org/10.1016/j.ijnurstu.2013.02.005.
Bourassa, K. J., Memel, M., Woolverton, C., & Sbarra, D. A. (2017). Social participation predicts cognitive functioning in aging adults over time: comparisons with physical health, depression, and physical activity. Aging & Mental Health, 21(2), 133–146. https://doi.org/10.1080/13607863.2015.1081152.
Lindbergh, C. A., Dishman, R. K., & Miller, L. S. (2016). Functional disability in mild cognitive impairment: A systematic review and meta-analysis. Neuropsychology Review, 26(2), 129–159. https://doi.org/10.1007/s11065-016-9321-5.
Reppermund, S., Sachdev, P. S., Crawford, J., Kochan, N. A., Slavin, M. J., Kang, K., et al. (2011). The relationship of neuropsychological function to instrumental activities of daily living in mild cognitive impairment. International Journal of Geriatric Psychiatry, 26(8), 843–852. https://doi.org/10.1002/gps.2612.
Agborsangaya, C. B., Lau, D., Lahtinen, M., Cooke, T., & Johnson, J. A. (2013). Health-related quality of life and healthcare utilization in multimorbidity: Results of a cross-sectional survey. Quality of Life Research, 22(4), 791–799. https://doi.org/10.1007/s11136-012-0214-7.
Parker, L., Moran, G. M., Roberts, L. M., Calvert, M., & McCahon, D. (2014). The burden of common chronic disease on health-related quality of life in an elderly community-dwelling population in the UK. Family Practice, 31(5), 557–563. https://doi.org/10.1093/fampra/cmu035.
Mangen, M. J. J., Bolkenbaas, M., Huijts, S. M., van Werkhoven, C. H., Bonten, M. J., & de Wit, G. A. (2017). Quality of life in community-dwelling Dutch elderly measured by EQ-5D-3L. Health and Quality of Life Outcomes, 15(1), 3. https://doi.org/10.1186/s12955-016-0577-5.
Xu, R. H., Cheung, A. W. L., & Wong, E. L. Y. (2017). Examining the health-related quality of life using EQ-5D-5L in patients with four kinds of chronic diseases from specialist outpatient clinics in Hong Kong SAR, China. Patient Preference and Adherence, 11, 1565–1572. https://doi.org/10.2147/PPA.S143944.
Lastra, G., Syed, S., Kurukulasuriya, L. R., Manrique, C., & Sowers, J. R. (2014). Type 2 diabetes mellitus and hypertension: An update. Endocrinology and Metabolism Clinics, 43(1), 103–122. https://doi.org/10.1016/j.ecl.2013.09.005.
Xu, T., Clemson, L., O’Loughlin, K., Lannin, N. A., Dean, C., & Koh, G. (2018). Risk factors for falls in community stroke survivors: A systematic review and meta-analysis. Archives of Physical Medicine and Rehabilitation, 99(3), 563–573.e5. https://doi.org/10.1016/j.apmr.2017.06.032.
Holt, E. W., Muntner, P., Joyce, C. J., Webber, L., & Krousel-Wood, M. A. (2010). Health-related quality of life and antihypertensive medication adherence among older adults. Age and Ageing, 39(4), 481–487. https://doi.org/10.1093/ageing/afq040.
Acknowledgements
The authors would like to express their gratitude to the Taiwan Alzheimer’s Disease Association for generously allowing us to use an invaluable database that they partly developed and supporting us under the commission of the Ministry of Health and Welfare of Taiwan (DOH100-TD-M113-100001). The views expressed throughout this study are exclusively those of the authors and do not represent the views or opinions of the Ministry of Health and Welfare, Taiwan.
Funding
This work was supported by the Chang Gung Medical Foundation [grant numbers BMRP297, CMRPD1E0162] and Healthy Aging Research Center, Chang Gung University, Taiwan [grant number EMRPD1H0361, EMRPD1H0551].
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
The data were approved by the National Taiwan University Hospital’s Institutional Review Board. Informed consent was obtained from the participants or their proxy.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Liu, HY., Tsai, WC., Chiu, MJ. et al. Mild cognitive impairment in combination with comorbid diabetes mellitus and hypertension is negatively associated with health-related quality of life among older persons in Taiwan. Qual Life Res 28, 1281–1291 (2019). https://doi.org/10.1007/s11136-019-02101-3
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11136-019-02101-3