Abstract
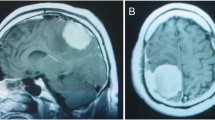
Intracranial aspergillosis (ICA) is very rare in the immunocompetent individuals, usually misdiagnosed as a tumor or an abscess. A high index of clinical suspicion is required in patients who present with focal neurological deficits, headache, or seizures. We report the case of a 25-year-old immunocompetent female, who presented with a 15-month history of headache, seizures, left-sided proptosis and ophthalmoplegia, and right hemiparesis. Recovery from the symptoms and decrease in the lesion size seen on the radiological assessment were achieved through two decompressive craniotomies followed by prolonged combined systemic antifungal therapies. Although the initial neuroimaging suggested a mitotic pathology, the surgical sample confirmed ICA. Now the patient is on single antifungal therapy (Tab. voriconazole, 200 mg twice daily) and doing her daily activities, but with a reduced intelligent quotient. We report a challenging case of ICA where multiple courses of combined antifungal therapies and repeat surgeries paved the way for a good prognosis.




Similar content being viewed by others
References
Dubey A, Patwardhan RV, Sampth S, Santosh V, Kolluri S, Nanda A. Intracranial fungal granuloma: analysis of 40 patients and review of the literature. Surg Neurol. 2005;63(3):254–60.
Hope WW, Walsh TJ, Denning DW. The invasive and saprophytic syndromes due to Aspergillus spp. Med Mycol. 2005;43(Suppl 1):S207–38.
Ruhnke M, Kofla G, Otto K, Schwartz S. CNS aspergillosis: recognition, diagnosis and management. CNS Drugs. 2007;21:659–76.
Panackal AA, Bennett JE, Williamson PR. Treatment options in invasive aspergillosis. Curr Treat Options Infect Dis. 2014;6(3):309–25. doi:10.1007/s40506-014-0016-2.
De Pauw B, Walsh TJ, Donnelly JP, et al. Revised definitions of invasive fungal disease from the European Organization for Research and Treatment of Cancer/Invasive Fungal Infections Cooperative Group and the National Institute of Allergy and Infectious Diseases Mycoses Study Group (EORTC/MSG) Consensus Group. Clin Infect Dis. 2008;46:1813–21.
Kourkoumpetis TK, Desalermos A, Muhammed M, Mylonakis E. Central nervous system aspergillosis: a series of 14 cases from a general hospital and review of 123 cases from the literature. Medicine (Baltimore). 2012;91(6):328–36. doi:10.1097/MD.0b013e318274cd77.
Al-Maskari N, Hussain I, Jumaa S, Al-Shail EA. Aspergillus flavus-induced brain abscess in an immunocompetent child: case report. Sultan Qaboos Univ Med J. 2016;16(2):e246–9. doi:10.18295/squmj.2016.16.02.019.
Beraldo D, Guerra R, Alvarenga V, Crepaldi L. Surgical treatment alone of cerebral aspergillosis in immunocompetent patient. J Neurol Surg A Cent Eur Neurosurg. 2016;77(5):452–6. doi:10.1055/s-0035-1558415.
Rasoolinejad M, Hajiabdolbaghi M, Manshadi SAD, Ardalan FA, Moradnejad P, Alijani N. Cerebral aspergillosis in an immunocompetent patient: a case report. Arch Neurosci. 2016;3(2):e31710. doi:10.5812/archneurosci.31710.
Mohammadi H, Sadeghi S, Zandi S. Central nervous system aspergilloma in an immunocompetent patient: a case report. Iran J Public Health. 2015;44(6):869–72.
Ellenbogen JR, Waqar M, Denning DW, et al. Posaconazole responsive cerebral aspergillosis in an immunocompetent adult. J Clin Neurosci. 2014;21(10):1825–7. doi:10.1016/j.jocn.2014.05.004.
Khandelwal A, Basheer N, Mahapatra AK. Multiple intracranial fungal abscesses in an immunocompetent infant treated surgically. J Pediatr Neurosci. 2014;9(2):159–61. doi:10.4103/1817-1745.139332.
Bao Z-S, You G, Li W-B, Jiang T. A single Aspergillus fumigatus intracranial abscess in an immunocompetent patient with parietal lobe tumorectomy. World J Surg Oncol. 2014;12:181. doi:10.1186/1477-7819-12-181.
Leyngold I, Olivi A, Ishii M, et al. Acute chiasmal abscess resulting from perineural extension of invasive sino-orbital aspergillosis in an immunocompetent patient. World Neurosurg. 2014;81(1):203.e1–6. doi:10.1016/j.wneu.2013.08.018.
Bokhari R, Baeesa S, Al-Maghrabi J, Madani T. Isolated cerebral aspergillosis in immunocompetent patients. World Neurosurg. 2014;82(1–2):e325–33. doi:10.1016/j.wneu.2013.09.037.
Xiao A, Jiang S, Liu Y, Deng K, You C. Invasive intracranial aspergillosis spread by the pterygopalatine fossa in an immunocompetent patient. Braz J Infect Dis. 2012;16(2):192–5.
Pelaez T, Gijón P, Bunsow E, et al. Resistance to voriconazole due to a G448S substitution in Aspergillus fumigatus in a patient with cerebral aspergillosis. J Clin Microbiol. 2012;50(7):2531–4. doi:10.1128/JCM.00329-12.
Li P, Cao EH, Zhao BL, et al. Invasive aspergillosis after near-drowning: case reports and review of the literature. Zhonghua Jie He He Hu Xi Za Zhi. 2011;34(9):657–62.
Ederies A, Chen J, Aviv RI, et al. Aspergillosis of the petrous apex and Meckel’s cave. Skull Base. 2010;20(3):189–92. doi:10.1055/s-0029-1246229.
Genzen JR, Kenney B. Central nervous system Aspergillus infection after epidural analgesia: diagnosis, therapeutic challenges, and literature review. Diagn Microbiol Infect Dis. 2009;65(3):312–8. doi:10.1016/j.diagmicrobio.2009.06.013.
Narayan SK, Kumar K, Swaminathan RP, Roopeshkumar VR, Bhavna B. Isolated cerebral aspergilloma in a young immunocompetent patient. Pract Neurol. 2009;9(3):166–8. doi:10.1136/jnnp.2009.176594.
Del Gaudio A, Catapano D, Pagano A, Zagaria G, Sorrentino E, D’Angelo V. Fatal subarachnoid hemorrhage from mycotic aneurysm ruptures in an immunocompetent patient with aspergillosis: a case report. Minerva Anestesiol. 2009;75(7–8):467–70.
Hiraga A, Uzawa A, Shibuya M, Numata T, Sunami S, Kamitsukasa I. Neuroaspergillosis in an immunocompetent patient successfully treated with voriconazole and a corticosteroid. Intern Med. 2009;48(14):1225–9.
Martins HS, da Silva TR, Scalabrini-Neto A, Velasco IT. Cerebral vasculitis caused by Aspergillus simulating ischemic stroke in an immunocompetent patient. J Emerg Med. 2010;38(5):597–600. doi:10.1016/j.jemermed.2007.09.062.
Ducolin C, Zuiani C, Sbuelz M, Bazzocchi M, Viale P. Invasive cerebral aspergillosis in an immunocompetent patient. A case report. Neuroradiol J. 2008;21(2):173–7.
Kulkarni V, Rajshekhar V, Mathews MS. An isolated non-dural-based cerebellar aspergilloma in an immunocompetent patient. Neurol India. 2007;55(3):310–1.
Challa S, Uppin SG, Purohit AK. Isolated cerebral Aspergillus granuloma with no obvious source of infection. Neurol India. 2007;55(3):289–91.
Taşdelen Fişgin N, Candir N, Sünbül M. Intracranial aspergillosis in an immunocompetent patient. Mikrobiyol Bul. 2007;41(2):303–7.
Sood S, Sharma R, Gupta S, Pathak D, Rishi S. Neuroaspergillosis in an immunocompetent patient. Indian J Med Microbiol. 2007;25(1):67–9.
Cho YS, Lee DK, Hong SD, Oh WS. Intracranial aspergillosis involving the internal auditory canal and inner ear in an immunocompetent patient. AJNR Am J Neuroradiol. 2007;28(1):138–40.
Aslam E, Imran M, Muhammad T, Faridi N. Rhinocerebral aspergillosis cripple: high oral doses of Itraconazole was the solution. J Pak Med Assoc. 2006;56:415–6.
Siddiqui AA, Shah AA, Bashir SH. Craniocerebral aspergillosis of sinonasal origin in immunocompetent patients: clinical spectrum and outcome in 25 cases. Neurosurgery. 2004;55(3):602–11.
Pongbhaesaj P, Dejthevaporn C, Tunlayadechanont S, et al. Aspergillosis of the central nervous system: a catastrophic opportunistic infection. Southeast Asian J Trop Med Public Health. 2004;35:119–25.
Srinivasan US. Intracranial aspergilloma in immunocompetent patients successfully treated with radical surgical intervention and antifungal therapy: case series. Ann Acad Med Singapore. 2008;37:783–7.
Ellenbogen JR, Waqar M, Cooke RP, Javadpour M. Management of granulomatous cerebral aspergillosis in immunocompetent adult patients: a review. Br J Neurosurg. 2016;30(3):280–5. doi:10.3109/02688697.2016.1139046.
Panackal AA, Li H, Kontoyiannis DP, et al. Geoclimatic influences on invasive aspergillosis after hematopoietic stem cell transplantation. Clin Infect Dis. 2010;50(12):1588–97. doi:10.1086/652761.
Shankar SK, Mahadevan A, Sundaram C, et al. Pathobiology of fungal infections of the central nervous system with special reference to the Indian scenario. Neurol India. 2007;55(3):198–215.
Nadkarni T, Goel A. Aspergilloma of the brain: an overview. J Postgrad Med. 2005;51(Suppl 1):S37–41.
Uppin MS, Anuradha S, Uppin SG, Paul TR, Prayaga AK, Sundaram C. Fungal infections as a contributing cause of death: an autopsy study. Indian J Pathol Microbiol. 2011;54:344–9.
Goel D, Bansal KK, Gupta C, et al. Why we missed an early diagnosis of cerebral aspergilloma: lesson from a case. Ann Indian Acad Neurol. 2007;10:263–5.
Hummel M, Spiess B, Kentouche K, et al. Detection of Aspergillus DNA in cerebrospinal fluid from patients with cerebral aspergillosis by a nested PCR assay. J Clin Microbiol. 2006;44:3989–93.
Guigue N, Lardeux S, Alanio A, Hamane S, Tabouret M, Bretagne S. Importance of operational factors in the reproducibility of Aspergillus galactomannan enzyme immune assay. PLoS ONE. 2015;10(4):e0124044. doi:10.1371/journal.pone.0124044.
Patterson TF, Thompson GR 3rd, Denning DW, et al. Practice guidelines for the diagnosis and management of aspergillosis: 2016 update by the infectious Diseases Society of America. Clin Infect Dis. 2016;63(4):e1–60. doi:10.1093/cid/ciw326.
Khandelwal N, Gupta V, Singh P. Central nervous system fungal infections in tropics. Neuroimaging Clin N Am. 2011;21(4):859–66. doi:10.1016/j.nic.2011.07.006.
McCarthy M, Rosengart A, Schuetz AN, Kontoyiannis DP, Walsh TJ. Mold infections of the central nervous system. N Engl J Med. 2014;371(2):150–60. doi:10.1056/NEJMra1216008.
Gaviani P, Schwartz RB, Hedley-Whyte ET, et al. Diffusion-weighted imaging of fungal cerebral infection. AJNR Am J Neuroradiol. 2005;26:1115–21.
Guarner J, Brandt ME. Histopathologic diagnosis of fungal infections in the 21st century. Clin Microbiol Rev. 2011;24(2):247–80. doi:10.1128/CMR.00053-10.
Sundaram C, Umabala P, Laxmi V, et al. Pathology of fungal infections of the central nervous system: 17 years’ experience from Southern India. Histopathology. 2006;49(4):396–405.
Schelenz S, Barnes RA, Barton RC, et al. British Society for Medical Mycology. British Society for Medical Mycologybest practice recommendations for the diagnosis of serious fungal diseases. Lancet Infect Dis. 2015;15(4):461–74. doi:10.1016/S1473-3099(15)70006-X.
Cordonnier C, Pautas C, Maury S, et al. Empirical versus preemptive antifungal therapy for high-risk, febrile, neutropenic patients: a randomized, controlled trial. Clin Infect Dis. 2009;48:1042–51.
Kethireddy S, Andes D. CNS pharmacokinetics of antifungal agents. Expert Opin Drug Metab Toxicol. 2007;3(4):573–81.
Marr KA, Schlamm HT, Herbrecht R, et al. Combination antifungal therapy for invasive aspergillosis: a randomized trial. Ann Intern Med. 2015;162:81–9.
Meletiadis J, Stergiopoulou T, O’Shaughnessy EM, Peter J, Walsh TJ. Concentration-dependent synergy and antagonism within a triple antifungal drug combination against Aspergillus species: analysis by a new response surface model. Antimicrob Agents Chemother. 2007;51(6):2053–64.
Panackal AA, Williamson KC, van de Beek D, Boulware DR, Williamson PR. Fighting the monster: applying the host damage framework to human central nervous system infections. MBio. 2016;7(1):e01906–15. doi:10.1128/mBio.01906-15.
Acknowledgements
Special thanks to the team of doctors from the Department of Neurosurgery for operating in the patient twice in succession as required.
Authors’ Contributions
PKP searched the literature, analyzed and drafted the study; SK collected data and drafted the study; NW provided the concept, analyzed, interpreted and revised the work; AG interpreted, including the literature search, especially the radiology data and critically revised the work; MCS and AN searched literature for the pathology part and drafted the work. PKP, SK, and NW were the physicians involved in patient management. All authors read and approved the final manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
We declare that we have no conflicts of interest.
Rights and permissions
About this article
Cite this article
Panda, P.K., Mavidi, S.K., Wig, N. et al. Intracranial Aspergillosis in an Immunocompetent Young Woman. Mycopathologia 182, 527–538 (2017). https://doi.org/10.1007/s11046-016-0106-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11046-016-0106-4