Abstract
Background
Gastroenterologists have ignored or emphasized the importance of the rectosigmoid junction in continence or constipation on and off for 200 years. Here, we revisit its significance using high-resolution colonic manometry.
Methods
Manometry, using an 84-channel water-perfused catheter, was performed in 18 healthy volunteers.
Results
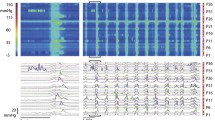
The rectosigmoid junction registers as an intermittent pressure band of 26.2 ± 7.2 mmHg, or intermittent phasic transient pressure increases at a dominant frequency of 3 cpm and an amplitude of 28.6 ± 8.6 mmHg; or a combination of tone and transient pressures, at a single sensor, 10–17 cm above the anal verge. Features are its relaxation or contraction in concert with relaxation or contraction of the anal sphincters when a motor pattern such as a high-amplitude propagating pressure wave or a simultaneous pressure wave comes down, indicating that such pressure increases or decreases at the rectosigmoid junction are part of neurally driven programs. We show that the junction is a site where motor patterns end, or where they start; e.g. retrogradely propagating cyclic motor patterns emerge from the junction.
Conclusions
The rectosigmoid junction is a functional sphincter that should be referred to as the sphincter of O’Beirne; it is part of the “braking mechanism,” contributing to continence by keeping content away from the rectum. In an accompanying case report, we show that its excessive presence in a patient with severe constipation can be a primary pathophysiology.








Similar content being viewed by others
Abbreviations
- HRCM:
-
High-resolution colonic manometry
- HAPW:
-
High amplitude propagating pressure wave
- HAPW-SPW:
-
High amplitude propagating pressure wave, followed by a simultaneous pressure wave
- SPW:
-
Simultaneous pressure wave
References
O’Beirne J. New Views of the Process of Defecation, and Their Application to the Pathology and Treatment of Diseases of the Stomach, Bowels, and Other Organs. Dublin: Hodges and Smith; 1833.
O’Beirne J. Organic structure of the rectum. Lancet. 1834;21:712–719.
Ballantyne GH. Rectosigmoid sphincter of O’Beirne. Dis Colon Rectum. 1986;29:525–531.
Balli R. Le rontgendiagnostic surtout au point de vue des organes de l’abdomen. Acta Radiol. 1928;89–106.
Balli R. The sphincters of the colon. Radiology. 1939;33:372–376.
Baker WNW, Mann CV. The rectosigmoid junction zone, another sphincter? In: Thomas PA, Mann CV, eds. Alimentary Sphincter and Their Disorders. London: Palgrave Macmillan; 1981:201–211.
Buntzen S, Nordgren S, Hultén L, Delbro D. The role of nitric oxide in the acetylcholine-induced relaxation of the feline internal anal sphincter, in vitro. Scand J Gastroenterol. 1996;31:1189–1194.
Cook TA, Brading AF, Mortensen NJ. The pharmacology of the internal anal sphincter and new treatments of ano-rectal disorders. Aliment Pharmacol Ther. 2001;15:887–898.
Hill JR, Kelley ML, Schlegel JF, Code CF. Pressure profile of the rectum and anus of healthy persons. Dis Colon Rectum. 1960;3:203–209.
Chen J-H, Collins SM, Milkova N, Pervez M, Nirmalathasan S, Wei T, Hanman A, Huizinga JD. The sphincter of O’Beirne – Part 2: report of a case of chronic constipation with autonomous dyssynergia. Dig Dis Sci. (Epub ahead of print). https://doi.org/10.1007/s10620-020-06723-3.
Chen J-H, Parsons SP, Shokrollahi M, et al. Characterization of simultaneous pressure waves as biomarkers for colonic motility assessed by high-resolution colonic manometry. Front Physiol Gastrointest Sci. 2018;9:1248. https://doi.org/10.3389/fphys.2018.01248.
Milkova N, Parsons SP, Ratcliffe E, Huizinga JD, Chen JH. On the nature of high-amplitude propagating pressure waves in the human colon. Am J Physiol Gastrointest Liver Physiol. 2020;318:G646–G660.
Wadhwa RP, Mistry FP, Bhatia SJ, Abraham P. Existence of a high pressure zone at the rectosigmoid junction in normal Indian men. Dis Colon Rectum. 1996;39:1122–1125.
Ritchie JA, Tuckey MS. Intraluminal pressure studies at different distances from the anus in normal subjects and in patients with the irritable colon syndrome. Am J Dig Dis. 1969;14:96–106.
Chowdhury AR, Dinoso VP, Lorber SH. Characterization of a hyperactive segment at the rectosigmoid junction. Gastroenterology. 1976;71:584–588.
Shafik A, Mostafa RM, Shafik AA. Electrophysiological study of the rectosigmoid canal: evidence of a rectosigmoid sphincter. J Anat. 2002;200:517–521.
Fisher R, Cohen S. Physiological characteristics of the human pyloric sphincter. Gastroenterology. 1973;64:67–75.
Code CF, Fyke FE, Schlegel JF. The gastroesophageal sphincter in healthy human beings. Gastroenterologia. 1956;86:135–150.
Shafik A. The hypertonic rectosigmoid junction: description of a new clinicopathologic entity causing constipation. Surg Laparosc Endosc. 1997;7:116–120.
Culligan K, Coffey JC, Kiran RP, Kalady M, Lavery IC, Remzi FH. The mesocolon: a prospective observational study. Colorectal Dis. 2012;14:421–428. (discussion 428).
Irving MH, Catchpole B. ABC of colorectal diseases. Anatomy and physiology of the colon, rectum, and anus. BMJ. 1992;304:1106–1108.
McNeil NI, Rampton DS. Is the rectum usually empty?—A quantitative study in subjects with and without diarrhea. Dis Colon Rectum. 1981;24:596–599.
Shafik A, Ali YA, Afifi R. Is the rectum a conduit or storage organ. Int Surg. 1997;82:194–197.
Malcolm A, Camilleri M. Coloanal motor coordination in association with high-amplitude colonic contractions after pharmacological stimulation. Am J Gastroenterol. 2000;95:715–719.
Lin AY, Dinning PG, Milne T, Bissett IP, O’Grady G. The “rectosigmoid brake”: review of an emerging neuromodulation target for colorectal functional disorders. Clin Exp Pharmacol Physiol. 2017;44:719–728.
Shafik A. Sigmoido-rectal junction reflex: role in the defecation mechanism. Clin Anat. 1996;9:391–394.
Lierse W, Frohmuller H, Stelzner F, Stegner H-E. In: Lang J, Wachsmuth W, eds. Applied Anatomy of the Pelvis. Berlin: Springer; 1984.
Moszkowicz D, Peschaud F, Bessede T, Benoit G, Alsaid B. Internal anal sphincter parasympathetic-nitrergic and sympathetic-adrenergic innervation: a 3-dimensional morphological and functional analysis. Dis Colon Rectum. 2012;55:473–481.
Mills K, Hausman N, Chess-Williams R. Characterization of the alpha1-adrenoceptor subtype mediating contractions of the pig internal anal sphincter. Br J Pharmacol. 2008;155:110–117.
Mills K, Chess-Williams R. Pharmacology of the internal anal sphincter and its relevance to faecal incontinence. Auton Autacoid Pharmacol. 2009;29:85–95.
Shafik A. Recto-colic reflex: role in the defecation mechanism. Int Surg. 1996;81:292–294.
Rao SS, Welcher K. Periodic rectal motor activity: the intrinsic colonic gatekeeper. Am J Gastroenterol. 1996;91:890–897.
Lin AY, Du P, Dinning PG, et al. High-resolution anatomic correlation of cyclic motor patterns in the human colon: evidence of a rectosigmoid brake. Am J Physiol Gastrointest Liver Physiol. 2017;312:G508–G515.
Pervez M, Ratcliffe E, Parsons SP, Chen J-H, Huizinga JD. The cyclic motor patterns in the human colon. Neurogastroenterol Motil. 2020;e13807:1–17. https://doi.org/10.1111/nmo.13807.
Chen J-H, Yang Z, Yu Y, Huizinga JD. Haustral boundary contractions in the proximal 3-taeniated colon of the rabbit. Am J Physiol. 2016;310:G181–G192.
Yoneda S, Fukui H, Takaki M. Pacemaker activity from submucosal interstitial cells of Cajal drives high-frequency and low-amplitude circular muscle contractions in the mouse proximal colon. Neurogastroenterol Motil. 2004;16:621–627.
Chen J-H, Yu Y, Yang Z, et al. Intraluminal pressure patterns in the human colon assessed by high-resolution manometry. Sci Rep. 2017;7:41436. https://doi.org/10.1038/srep41436.
Broens PM, Penninckx FM, Ochoa JB. Fecal continence revisited: the anal external sphincter continence reflex. Dis Colon Rectum. 2013;56:1273–1281.
Broens PMA, Jonker JE, Trzpis M. The puborectal continence reflex: a new regulatory mechanism controlling fecal continence. Int J Colorectal Dis. 2018;33:627–633.
Acknowledgments
JDH received a Canadian Foundation for Innovation John Evans Leadership Grant for the equipment used in this study. The hardware was designed in collaboration with Medical Measurement Systems. The catheters were designed in collaboration with Howard Mui and staff at Mui Scientific. Sharjana Nirmalathasan was supported in part by a scholarship from NSERC. This study was supported by an operating grant to JDH from the Canadian Institutes of Health Research PJT-152942. The authors acknowledge the continuing support from Elyanne Ratcliffe, David Armstrong, Stephen M. Collins, and staff at the Endoscopy Unit.
Author information
Authors and Affiliations
Contributions
All HRCM studies were carried out by JHC. Analysis was carried out by SN, MP and NM and the interpretation of data was done by JHC, SN, NM, MP and JDH. All authors contributed to manuscript writing and all approved the final version.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no competing interests.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Chen, JH., Nirmalathasan, S., Pervez, M. et al. The Sphincter of O’Beirne – Part 1: Study of 18 Normal Subjects. Dig Dis Sci 66, 3516–3528 (2021). https://doi.org/10.1007/s10620-020-06657-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10620-020-06657-w