Abstract
Background
Although cardiovascular (CV) disease is the leading cause of mortality and morbidity in dialysis patients, there is little evidence to guide the use of antiplatelet agents in dialysis patients.
Method
A nationwide database (Registry for Catastrophic Illnesses) for Taiwan, which has data from nearly all patients who received dialysis therapy from 1995 to 2008, was used. This is a population-based cohort study with time to event analyses to estimate the relation between antiplatelet agent use and outcomes. Hazard ratios were calculated to evaluate the effect of antiplatelet agent use on the risk of major CV events and mortality. Baseline characteristics were matched by propensity score (PS).
Results
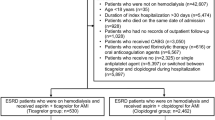
A total of 71,835 were included, and 10,595 (14.7%) patients received an anti-platelet agent. The median value of follow-up days was 61.6 months. After PS-based matching, 9598 patients who used an antiplatelet agent and 23,794 non-users were included in the analysis. After PS matching, there was no difference between patients using an antiplatelet agent or not in CV events (p = 0.672) and total mortality (p = 0.529). A subgroup analysis of different usage periods of antiplatelet agents indicated that CV events and total mortality were similar in those who used antiplatelet agents for short or long durations. In subgroup analysis, there was also no difference between patients with a different modality of dialysis (hemodialysis or peritoneal dialysis), different antiplatelet agents (aspirin, clopidogrel, and/or ticlopidine) or patients with/without previous cardiovascular disease in CV events and total mortality.
Conclusions
Antiplatelet agent usage does not reduce CV events and total mortality in dialysis patients.


Similar content being viewed by others
References
Sarnak MJ, Levey AS, Schoolwerth AC, Coresh J, Culleton B, Hamm LL, et al. Kidney disease as a risk factor for development of cardiovascular disease: a statement from the American Heart Association councils on kidney in cardiovascular disease, high blood pressure research, clinical cardiology, and epidemiology and prevention. Circulation. 2003;108(17):2154–69.
Herzog CA, Ma JZ, Collins AJ. Poor long-term survival after acute myocardial infarction among patients on long-term dialysis. N Engl J Med. 1998;339(12):799–805.
Antithrombotic Trialists C. Collaborative meta-analysis of randomised trials of antiplatelet therapy for prevention of death, myocardial infarction, and stroke in high risk patients. BMJ. 2002;324(7329):71–86.
Bell AD, Roussin A, Cartier R, Chan WS, Douketis JD, Gupta A, et al. The use of antiplatelet therapy in the outpatient setting: Canadian cardiovascular society guidelines. Can J Cardiol. 2011;27(Suppl A):S1–59.
Bell AD, Roussin A, Cartier R, Chan WS, Douketis JD, Gupta A, et al. The use of antiplatelet therapy in the outpatient setting: Canadian cardiovascular society guidelines executive summary. Can J Cardiol. 2011;27(2):208–21.
Workgroup KD. K/DOQI clinical practice guidelines for cardiovascular disease in dialysis patients. Am J Kidney Dis. 2005;45(4 Suppl 3):S1–153.
Trespalacios FC, Taylor AJ, Agodoa LY, Abbott KC. Incident acute coronary syndromes in chronic dialysis patients in the United States. Kidney Int. 2002;62(5):1799–805.
Ethier J, Bragg-Gresham JL, Piera L, Akizawa T, Asano Y, Mason N, et al. Aspirin prescription and outcomes in hemodialysis patients: the Dialysis Outcomes and Practice Patterns Study (DOPPS). Am J Kidney Dis. 2007;50(4):602–11.
Gent M, Beaumont D, Blanchard J, Bousser MG, Coffman J, Easton JD, et al. A randomised, blinded, trial of clopidogrel versus aspirin in patients at risk of ischaemic events (CAPRIE). Lancet. 1996;348(9038):1329–39.
Hankey GJ, Sudlow CL, Dunbabin DW. Thienopyridines or aspirin to prevent stroke and other serious vascular events in patients at high risk of vascular disease? A systematic review of the evidence from randomized trials. Stroke. 2000;31(7):1779–84.
Sood MM, Larkina M, Thumma JR, Tentori F, Gillespie BW, Fukuhara S, et al. Major bleeding events and risk stratification of antithrombotic agents in hemodialysis: results from the DOPPS. Kidney Int. 2013;84(3):600–8.
Chan KE, Lazarus JM, Thadhani R, Hakim RM. Anticoagulant and antiplatelet usage associates with mortality among hemodialysis patients. J Am Soc Nephrol. 2009;20(4):872–81.
Lu JFR, Hsiao WC. Does universal health insurance make health care unaffordable? Lessons from Taiwan. Health Aff. 2003;22(3):77–88.
Chiang TL. Taiwan's 1995 health care reform. Health Policy. 1997;39(3):225–39.
Tseng CH. Mortality and causes of death in a national sample of diabetic patients in Taiwan. Diabetes Care. 2004;27(7):1605–9.
Wu CK, Yang YH, Lin TT, Tsai CT, Hwang JJ, Lin JL et al. Statin use reduces the risk of dementia in elderly patients: a nationwide data survey and propensity analysis. J Intern Med. 2015;277(3):343–52.
Alexopoulos D, Xanthopoulou I, Panagiotou A, Komninakis D, Germanos N, Goudas P, et al. Prevalence of inadequate platelet inhibition by clopidogrel in patients receiving hemodialysis. Am J Kidney Dis. 2012;59(3):469–71.
Htun P, Kan T, Mueller E, Pohle C, Schindler R, Geisler T, et al. Haemodialysis impairs clopidogrel but not aspirin responsiveness in patients with end-stage renal disease. Results of a pilot study. Thromb Haemost. 2014;111(4):662–9.
Chen CY, Lee KT, Lee CT, Lai WT, Huang YB. Effectiveness and safety of antiplatelet in stroke patients with end-stage renal disease undergoing dialysis. Int J Stroke. 2014;9(5):580–90.
Funding
This study was financially supported by Taiwan’s Ministry of Science and Technology (MOST 103-2220-E-002 -011). The funders had no role in study design, data collection and analysis, decision to publish, or preparation of the manuscript. There are no relationships with industry. No conflict of interest exists in this study.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Ethical Approval
All procedures performed in the current study were conducted in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed Consent
The data of this study was obtained from the Taiwan National Health Insurance research database. Informed consent from individual patients was not required.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Chen, ZW., Wu, CK., Yang, YH. et al. Efficacy of Antiplatelet Agent Usage for Primary and Secondary Prevention in Dialysis Patients: a Nationwide Data Survey and Propensity Analysis. Cardiovasc Drugs Ther 33, 471–479 (2019). https://doi.org/10.1007/s10557-019-06882-0
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10557-019-06882-0