Abstract
Purpose
The ACOSOG Z0011 trial demonstrated that axillary lymph node dissection (ALND) is unnecessary in select patients with cT1-2N0 tumors undergoing breast-conserving therapy with 1–2 positive sentinel lymph nodes (SLNs). However, patients with preoperatively confirmed ALN metastasis were not included and may be subjected to unnecessary ALND. The aim of this study is to identify patients who can be considered for ALND omission when the preoperative ALN biopsy results are positive.
Methods
Breast cancer patients who underwent preoperative ALN biopsy and primary surgery were retrospectively reviewed. Among patients with positive ALN biopsy results, clinicopathological and imaging characteristics were compared according to LN disease burden (1–2 positive LNs vs. ≥ 3 positive LNs).
Results
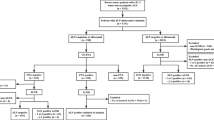
A total of 542 patients were included in the analysis. Among them, 225 (41.5%) patients had a preoperative positive ALN biopsy. More than 40% of the patients (n = 99, 44.0%) with a positive biopsy had only 1–2 positive ALNs. The association between nodal burden and imaging factors was strongest when ≥ 2 suspicious LNs were identified on PET/CT images (HR 8.795, 95% CI 4.756 to 13.262). More than one imaging modality showing ≥ 2 suspicious LNs was also strongly correlated with ≥ 3 positive ALNs (HR 5.148, 95% CI 2.881 to 9.200).
Conclusions
Nearly half of patients with a preoperative biopsy-proven ALN metastasis had only 1–2 positive LNs on ALND. Patients meeting ACOSOG Z0011 criteria with only one suspicious LN on PET/CT or those presenting with few abnormal ALNs on only one imaging modality appear appropriate for SLNB and consideration of ALND omission.

Similar content being viewed by others
References
Donker M, van Tienhoven G, Straver ME, Meijnen P, van de Velde CJ, Mansel RE, Cataliotti L, Westenberg AH, Klinkenbijl JH, Orzalesi L, Bouma WH, van der Mijle HC, Nieuwenhuijzen GA, Veltkamp SC, Slaets L, Duez NJ, de Graaf PW, van Dalen T, Marinelli A, Rijna H, Snoj M, Bundred NJ, Merkus JW, Belkacemi Y, Petignat P, Schinagl DA, Coens C, Messina CG, Bogaerts J, Rutgers EJ (2014) Radiotherapy or surgery of the axilla after a positive sentinel node in breast cancer (EORTC 10981–22023 AMAROS): a randomised, multicentre, open-label, phase 3 non-inferiority trial. Lancet Oncol 15(12):1303–1310. https://doi.org/10.1016/s1470-2045(14)70460-7
Giuliano AE, Hunt KK, Ballman KV, Beitsch PD, Whitworth PW, Blumencranz PW, Leitch AM, Saha S, McCall LM, Morrow M (2011) Axillary dissection vs no axillary dissection in women with invasive breast cancer and sentinel node metastasis: a randomized clinical trial. JAMA 305(6):569–575. https://doi.org/10.1001/jama.2011.90
Galimberti V, Cole BF, Zurrida S, Viale G, Luini A, Veronesi P, Baratella P, Chifu C, Sargenti M, Intra M, Gentilini O, Mastropasqua MG, Mazzarol G, Massarut S, Garbay JR, Zgajnar J, Galatius H, Recalcati A, Littlejohn D, Bamert M, Colleoni M, Price KN, Regan MM, Goldhirsch A, Coates AS, Gelber RD, Veronesi U (2013) Axillary dissection versus no axillary dissection in patients with sentinel-node micrometastases (IBCSG 23–01): a phase 3 randomised controlled trial. Lancet Oncol 14(4):297–305. https://doi.org/10.1016/s1470-2045(13)70035-4
Gentilini O, Veronesi U (2012) Abandoning sentinel lymph node biopsy in early breast cancer? A new trial in progress at the European Institute of Oncology of Milan (SOUND: Sentinel node vs Observation after axillary UltraSouND). Breast 21(5):678–681. https://doi.org/10.1016/j.breast.2012.06.013
Steyerburg E (2009) Clinical prediction models: a practical apporach to development, validation, and updating. Statistics for Biology and Health. Springer Science+Business Media, New York
Verheuvel NC, van den Hoven I, Ooms HW, Voogd AC, Roumen RM (2015) The role of ultrasound-guided lymph node biopsy in axillary staging of invasive breast cancer in the post-ACOSOG Z0011 trial era. Ann Surg Oncol 22(2):409–415. https://doi.org/10.1245/s10434-014-4071-1
Pilewskie M, Mautner SK, Stempel M, Eaton A, Morrow M (2016) Does a positive axillary lymph node needle biopsy result predict the need for an axillary lymph node dissection in clinically node-negative breast cancer patients in the ACOSOG Z0011 era? Ann Surg Oncol 23(4):1123–1128. https://doi.org/10.1245/s10434-015-4944-y
van Wely BJ, de Wilt JH, Francissen C, Teerenstra S, Strobbe LJ (2015) Meta-analysis of ultrasound-guided biopsy of suspicious axillary lymph nodes in the selection of patients with extensive axillary tumour burden in breast cancer. Br J Surg 102(3):159–168. https://doi.org/10.1002/bjs.9663
Harris CK, Tran HT, Lee K, Mylander C, Pack D, Rosman M, Tafra L, Umbricht CB, Andrade R, Liang W, Jackson RS (2017) Positive ultrasound-guided lymph node needle biopsy in breast cancer may not mandate axillary lymph node dissection. Ann Surg Oncol 24(10):3004–3010. https://doi.org/10.1245/s10434-017-5935-y
Boland MR, Prichard RS, Daskalova I, Lowery AJ, Evoy D, Geraghty J, Rothwell J, Quinn CM, O'Doherty A, McDermott EW (2015) Axillary nodal burden in primary breast cancer patients with positive pre-operative ultrasound guided fine needle aspiration cytology: management in the era of ACOSOG Z011. Eur J Surg Oncol 41(4):559–565. https://doi.org/10.1016/j.ejso.2015.01.011
Del Riego J, Diaz-Ruiz MJ, Teixido M, Ribe J, Vilagran M, Canales L, Sentis M (2018) The impact of axillary ultrasound with biopsy in overtreatment of early breast cancer. Eur J Radiol 98:158–164. https://doi.org/10.1016/j.ejrad.2017.11.018
Farrell TP, Adams NC, Stenson M, Carroll PA, Griffin M, Connolly EM, O'Keeffe SA (2015) The Z0011 Trial: Is this the end of axillary ultrasound in the pre-operative assessment of breast cancer patients? Eur Radiol 25(9):2682–2687. https://doi.org/10.1007/s00330-015-3683-6
Lloyd P, Theophilidou E, Newcombe RG, Pugh L, Goyal A (2017) Axillary tumour burden in women with a fine-needle aspiration/core biopsy-proven positive node on ultrasonography compared to women with a positive sentinel node. Br J Surg 104(13):1811–1815. https://doi.org/10.1002/bjs.10661
Valente SA, Levine GM, Silverstein MJ, Rayhanabad JA, Weng-Grumley JG, Ji L, Holmes DR, Sposto R, Sener SF (2012) Accuracy of predicting axillary lymph node positivity by physical examination, mammography, ultrasonography, and magnetic resonance imaging. Ann Surg Oncol 19(6):1825–1830. https://doi.org/10.1245/s10434-011-2200-7
Lanng C, Hoffmann J, Galatius H, Engel U (2007) Assessment of clinical palpation of the axilla as a criterion for performing the sentinel node procedure in breast cancer. Eur J Surg Oncol 33(3):281–284. https://doi.org/10.1016/j.ejso.2006.09.032
Specht MC, Fey JV, Borgen PI, Cody HS 3rd (2005) Is the clinically positive axilla in breast cancer really a contraindication to sentinel lymph node biopsy? J Am Coll Surg 200(1):10–14. https://doi.org/10.1016/j.jamcollsurg.2004.09.010
Feng Y, Huang R, He Y, Lu A, Fan Z, Fan T, Qi M, Wang X, Cao W, Wang X, Xie Y, Wang T, Li J, Ouyang T (2015) Efficacy of physical examination, ultrasound, and ultrasound combined with fine-needle aspiration for axilla staging of primary breast cancer. Breast Cancer Res Treat 149(3):761–765. https://doi.org/10.1007/s10549-015-3280-z
Kim EJ, Kim SH, Kang BJ, Choi BG, Song BJ, Choi JJ (2014) Diagnostic value of breast MRI for predicting metastatic axillary lymph nodes in breast cancer patients: diffusion-weighted MRI and conventional MRI. Magn Reson Imaging 32(10):1230–1236. https://doi.org/10.1016/j.mri.2014.07.001
Choi WH, Yoo IR, O JH, Kim SH, Chung SK (2011) The value of dual-time-point 18F-FDG PET/CT for identifying axillary lymph node metastasis in breast cancer patients. Br J Radiol 84(1003):593–599. https://doi.org/10.1259/bjr/56324742
Morrow M (2018) Management of the node-positive axilla in breast cancer in 2017: selecting the right option. JAMA Oncol 4(2):250–251. https://doi.org/10.1001/jamaoncol.2017.3625
Pilewskie M, Jochelson M, Gooch JC, Patil S, Stempel M, Morrow M (2016) Is Preoperative axillary imaging beneficial in identifying clinically node-negative patients requiring axillary lymph node dissection? J Am Coll Surg 222(2):138–145. https://doi.org/10.1016/j.jamcollsurg.2015.11.013
Lim GH, Upadhyaya VS, Acosta HA, Lim JMA, Allen JC Jr, Leong LCH (2018) Preoperative predictors of high and low axillary nodal burden in Z0011 eligible breast cancer patients with a positive lymph node needle biopsy result. Eur J Surg Oncol 44(7):945–950. https://doi.org/10.1016/j.ejso.2018.04.003
Song BI, Kim HW, Won KS (2017) Predictive value of (18)F-FDG PET/CT for axillary lymph node metastasis in invasive ductal breast cancer. Ann Surg Oncol 24(8):2174–2181. https://doi.org/10.1245/s10434-017-5860-0
Cooper KL, Meng Y, Harnan S, Ward SE, Fitzgerald P, Papaioannou D, Wyld L, Ingram C, Wilkinson ID, Lorenz E (2011) Positron emission tomography (PET) and magnetic resonance imaging (MRI) for the assessment of axillary lymph node metastases in early breast cancer: systematic review and economic evaluation. Health Technol Assess 15(4):1–134. https://doi.org/10.3310/hta15040
Cooper KL, Harnan S, Meng Y, Ward SE, Fitzgerald P, Papaioannou D, Wyld L, Ingram C, Wilkinson ID, Lorenz E (2011) Positron emission tomography (PET) for assessment of axillary lymph node status in early breast cancer: a systematic review and meta-analysis. Eur J Surg Oncol 37(3):187–198. https://doi.org/10.1016/j.ejso.2011.01.003
Funding
This work was supported by the Basic Science Research Program of the National Research Foundation funded by the Ministry of Education [2017R1D1A1B03033486 to B.J.C.].
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no competing interests.
Research involving human participants and/or animals
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
This study was approved by the institutional review board of Seoul St. Mary’s Hospital, College of Medicine, The Catholic University of Korea (IRB no. KC18RESI0614), and the need to obtain informed consent was waived.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Yoo, TK., Kang, B.J., Kim, S.H. et al. Axillary lymph node dissection is not obligatory in breast cancer patients with biopsy-proven axillary lymph node metastasis. Breast Cancer Res Treat 181, 403–409 (2020). https://doi.org/10.1007/s10549-020-05636-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10549-020-05636-z