Abstract
Background
Henoch–Schönlein purpura (HSP) is the most common vasculitis in childhood. The long-term prognosis is variable and depends on renal involvement. The aims of this study were to investigate the clinical and laboratory characteristics of our HSP patients, to identify the risk factors for the development of Henoch–Schönlein purpura nephritis (HSPN) and to assess the efficacy of the Oxford Classification system for predicting renal outcomes.
Methods
We performed a retrospective review of HSP patients who admitted to our center between 2001 and 2016, and were < 18 years on admission.
Results
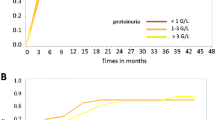
A total of 1120 children with HSP were analyzed. Their mean age was 7.4 ± 3.4 years. At onset, purpura was present in all cases, arthritis/arthralgia in 42.4%, abdominal involvement in 39% and renal involvement in 37%. Risk factors for the development of nephritis were age ≥ 8 years, atypical distribution of purpura, ESR > 20 mm/h and abdominal pain. Renal biopsy was performed on 75 patients before immunosuppressive treatment. The mesangial score was strongly associated with proteinuria. Segmental glomerulosclerosis, tubular atrophy/interstitial fibrosis, and crescent formation of ≥ 50% were associated with reduced eGFR at the time of biopsy. A Kaplan–Meier plot showed that segmental glomerulosclerosis and tubular atrophy/interstitial fibrosis significantly predict poor renal outcome.
Conclusion
The long-term morbidity of HSP is predominantly attributed to renal involvement. Patients with HSP, who have a high risk to develop nephritis, could be followed for longer periods of time. The Oxford classification is useful in predicting long-term outcomes of HSPN.

Similar content being viewed by others
References
Jennette JC. Overview of the 2012 revised International Chapel Hill Consensus Conference nomenclature of vasculitides. Clin Exp Nephrol. 2013;17(5):603–6.
Ozen S, Ruperto N, Dillon MJ, Bagga A, Barron K, Davin JC, Kawasaki T, Lindsley C, Petty RE, Prieur AM, Ravelli A, Woo P. EULAR/PReS endorsed consensus criteria for the classification of childhood vasculitides. Ann Rheum Dis. 2006;65(7):936–41.
Jauhola O, Ronkainen J, Koskimies O, et al. Outcome of Henoch–Schönlein purpura 8 years after treatment with a placebo or prednisone at disease onset. Pediatr Nephrol. 2012;27(6):933–9.
Ronkainen J, Nuutinen M, Koskimies O. The adult kidney 24 years after childhood Henoch–Schönlein purpura: a retrospective cohort study. Lancet. 2002;360(9334):666–70.
Trapani S, Micheli A, Grisolia F, Resti M, Chiappini E, Falcini F, De Martino M. Henoch–Schonlein purpura in childhood: epidemiological and clinical analysis of 150 cases over a 5-year period and review of literature. Semin Arthritis Rheum. 2005;35(3):143–53.
Chang WL, Yang YH, Wang LC, Lin YT, Chiang BL. Renal manifestations in Henoch–Schönlein purpura: a 10-year clinical study. Pediatr Nephrol. 2005;20(9):1269–72.
Koskimies O, Mir S, Rapola J, Vilska J. Henoch–Schonlein nephritis: long-term prognosis of unselected patients. Arch Dis Child. 1981;56(6):482–4.
Kobayashi O, Wada H, Okawa K, Takeyama I. Schonlein–Henoch’s syndrome in children. Contrib Nephrol. 1975;4:48–71.
Coppo R, Andrulli S, Amore A, et al. Predictors of outcome in Henoch–Schönlein nephritis in children and adults. Am J Kidney Dis. 2006;47(6):993–1003.
Cattran DC, Coppo R, Cook HT, et al. The Oxford Classification of IgA nephropathy: rationale, clinicopathological correlations, and classification. Kidney Int. 2009;76(5):534–45.
Coppo R, Troyanov S, Camilla R, et al. The Oxford IgA nephropathy clinicopathological classification is valid for children as well as adults. Kidney Int. 2010;77(10):921–7.
Alamartine E, Sauron C, Laurent B, et al. The use of the Oxford Classification of IgA nephropathy to predict renal survival. Clin J Am Soc Nephrol. 2011;6(10):2384–8.
Schwartz GJ, Brion LP, Spitzer A. The use of plasma creatinine concentration for estimating glomerular filtration rate in infants, children, and adolescents. Pediatr Clin N Am. 1987;34(3):571–90.
National High Blood Pressure Education Program Working Group on High Blood Pressure in Children and Adolescents. The fourth report on the diagnosis, evaluation, and treatment of high blood pressure in children and adolescents. Pediatrics. 2004;114(2 Suppl 4th Report):555–76.
Hass M. Henoch–Schönlein purpura nephritis. In: Jennete JC, Olsen JL, Schwartz MM, Silva FG, editors. Heptinstall’s pathology of the kidney. 6th ed. Philadelphia: Lippincott Williams & Wilkins; 2007. pp. 465–8.
Anil M, Aksu N, Kara OD, Bal A, Anil AB, Yavaşcan O, et al. Henoch–Schönlein purpura in children from western Turkey: a retrospective analysis of 430 cases. Turk J Pediatr. 2009;51(5):429–36.
Calviño MC, Llorca J, García-Porrúa C, Fernández-Iglesias JL, Rodriguez-Ledo P, González-Gay MA. Henoch–Schönlein purpura in children from northwestern Spain: a 20-year epidemiologic and clinical study. Medicine (Baltimore). 2001;80(5):279–90.
Kaku Y, Nohara K, Honda S. Renal involvement in Henoch–Schönlein purpura: a multivariate analysis of prognostic factors. Kidney Int. 1998;53(6):1755–9.
Kawasaki Y, Suzuki J, Sakai N, Nemoto K, Nozawa R, Suzuki S, Suzuki H. Clinical and pathological features of children with Henoch–Schoenlein purpura nephritis: risk factors associated with poor prognosis. Clin Nephrol. 2003;60(3):153–60.
Goldstein AR, White RH, Akuse R, Chantler C. Long-term follow-up of childhood Henoch–Schonlein nephritis. Lancet. 1992;339(8788):280–2.
Sano H, Izumida M, Shimizu H, Ogawa Y. Risk factors of renal involvement and significant proteinuria in Henoch–Schonlein purpura. Eur J Pediatr. 2002;161(4):196–201.
Rigante D, Candelli M, Federico G, Bartolozzi F, Porri MG, Stabile A. Predictive factors of renal involvement or relapsing disease in children with Henoch–Schonlein purpura. Rheumatol Int. 2005;25(1):45–8.
Bogdanovic R. Henoch–Schonlein purpura nephritis in children: risk factors, prevention and treatment. Acta Paediatr. 2009;98(12):1882–9.
Mollica F, Li Volti S, Garozzo R, et al. Effectiveness of early prednisone treatment in preventing the development of nephropathy in anaphylactoid purpura. Eur J Pediatr. 1992;151(2):140–4.
Ronkainen J, Koskimies O, Ala-Houhala M, Antikainen M, Merenmies J, Rajantie J, Ormälä T, Turtinen J, Nuutinen M. Early prednisone therapy in Henoch–Schönlein purpura: a randomized, double-blind, placebo-controlled trial. J Pediatr. 2006;149(2):241–7.
Jauhola O, Ronkainen J, Koskimies O, Ala-Houhala M, Arikoski P, Hölttä T, Jahnukainen T, Rajantie J, Ormälä T, Turtinen J, Nuutinen M. Renal manifestations of Henoch–Schonlein purpura in a 6-month prospective study of 223 children. Arch Dis Child. 2010;95(11):877–82.
Fretzayas A, Sionti I, Moustaki M, et al. Henoch–Schönlein purpura: a long-term prospective study in Greek children. J Clin Rheumatol. 2008;14(6):324–31.
Edstrom Halling S, Soderberg MP, Berg UB. Predictors of outcome in Henoch–Schonlein nephritis. Pediatr Nephrol. 2010;25(6):1101–8.
Narchi H. Risk of long term renal impairment and duration of follow up recommended for Henoch–Schönlein purpura with normal or minimal urinary findings: a systematic review. Arch Dis Child. 2005;90(9):916–20.
Pohl M. Henoch–Schönlein purpura nephritis. Pediatr Nephrol. 2015;30(2):245–52. https://doi.org/10.1007/s00467-014-2815-6 (Epub 2014 Apr 15, Review).
Davin JC, Coppo R. Henoch–Schönlein purpura nephritis in children. Nat Rev Nephrol. 2014;10(10):563–73. https://doi.org/10.1038/nrneph.2014.126 (Epub 2014 Jul 29).
Algoet C, Proesmans W. Renal biopsy 2–9 years after Henoch–Schonlein purpura. Pediatr Nephrol. 2003;18(5):471–3 (Epub 2003 Apr 3).
Kamei K, Ogura M, Sato M, Ito S, Ishikura K. Evolution of IgA nephropathy into anaphylactoid purpura in six cases-further evidence that IgA nephropathy and Henoch–Schonlein purpura nephritis share common pathogenesis. Pediatr Nephrol. 2016;31(5):779–85. https://doi.org/10.1007/s00467-015-3290-4.
Xu K, Zhang L, Ding J, Wang S, Su B, Xiao H, Wang F, Zhong X, Li Y. Value of the Oxford classification of IgA nephropathy in children with Henoch–Schönlein purpura nephritis. J Nephrol. 2018;31(2):279–86. https://doi.org/10.1007/s40620-017-0457-z.
Kim CH, Lim BJ, Bae YS, Kwon YE, Kim YL, Nam KH, et al. Using the Oxford classification of IgA nephropathy to predict long-term outcomes of Henoch–Schönlein purpura nephritis in adults. Mod Pathol. 2014;27(7):972–82. https://doi.org/10.1038/modpathol.2013.222.
Author information
Authors and Affiliations
Contributions
EKÇ designed, wrote the manuscript, and analyzed the data. GG, FY and FKE designed and wrote the manuscript. NA and DO evaluated biopsy specimens. FSÖA performed the statistical analyses. TG and MB participated in collection of data. All authors have read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
About this article
Cite this article
Çakıcı, E.K., Gür, G., Yazılıtaş, F. et al. A retrospective analysis of children with Henoch–Schonlein purpura and re-evaluation of renal pathologies using Oxford classification. Clin Exp Nephrol 23, 939–947 (2019). https://doi.org/10.1007/s10157-019-01726-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10157-019-01726-5