Abstract
Objectives
Rheumatoid arthritis (RA) is a heterogeneous autoimmune disease, characterized by chronic inflammation, hyperplasia (swelling), tenderness, erosion of cartilage and bones in synovial joints. Transforming growth factor-β1 (TGF-β1) is an important regulator of inflammation, and its polymorphism is implicated in several diseases. Therefore, the study was done to determine whether TGF-β1 C/T gene polymorphism was associated with RA in North Indian population.
Methods
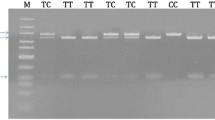
Eighty-seven (male/female: 29/58) healthy controls and 76 (male/female: 17/59) RA patients were recruited for association study between TGF-β1 +869C/T polymorphism. TGF-β1 +869C/T polymorphism was genotyped by allele specific amplification refractory mutation system polymerase chain reaction (ARMS-PCR) to test susceptibility to clinical presentation of RA patients in North Indian population by comparing RA genotypes with control groups.
Results
The genotypic association studies and dominant, recessive, and allelic models revealed that TGF-β1 +869C/T gene polymorphism is involved in the onset of RA. TGF-β1 +869 T (either TT or CT) allele and TT v/s CC (OR = 36.18, 95% CI = 11.98–109.31, P = 0.001); TT + CT v/s CC (OR = 0.16, 95% CI = 0.08–0.33, P = 0.001); TT v/s CC + CT (OR = 0.04, 95% CI = 0.1–0.09, P = 0.001); and T v/s C (OR = 0.12, 95% CI = 0.07–0.2, P = 0.001) show significant association with RA as compared with CC genotype or C alleles (P = 0.001). The patient carrying T alleles showed significant associations with increased ESR, uric acid, CRP, DAS28-ESR, and number of tender joints as compared to other genotypes. In the presence of RF, DAS-28-ESR was high in CT genotype. ESR, CRP, and swollen joint count were highest in TT genotype of RF negative patients.
Conclusions
TGF-β1 polymorphism is associated with disease activity of RA. Disease activity is strongly modulated in the presence of serum RF and TGF-β1 polymorphism.
Key Points •TGF-β1 +869C/T polymorphism was found to be associated with RA in the patients. •The polymorphism showed significant association with all inflammatory parameters as ESR, CRP, and DAS-28 in RA subjects. •RF negative patients showed high ESR, CRP, and swollen joint count with TT genotype. •TGF-β1 polymorphism and serum RF are modulating disease activity in RA. |
Similar content being viewed by others
References
Mcinnes IB, Schett G (2011) The pathogenesis of rheumatoid arthritis. N Engl J Med 365:2205–2219. https://doi.org/10.1056/NEJMra1004965
Moreland L (2005) Unmet needs in rheumatoid arthritis. Arthritis Res Ther 7:S2–S7. https://doi.org/10.1186/ar1736
Turesson C, Matteson EL (2004) Management of extra-articular disease manifestations in rheumatoid arthritis. Curr Opin Rheumatol 16:206–211. https://doi.org/10.1097/00002281-200405000-00007
Gibofsky A (2014) Epidemiology, pathophysiology, and diagnosis of rheumatoid arthritis: a synopsis. Am J Manag Care 20:S128–S135
Cojocaru M, Cojocaru IM, Silosi I, Vrabie CD, Tanasescu R (2010) Extra-articular manifestations in rheumatoid arthritis. Maedica. 5:286
Chang WW, Su H, He L, Zhao KF, Wu JL, Xu ZW (2010) Association between transforming growth factor-β1 T869C polymorphism and rheumatoid arthritis: a meta-analysis. Rheumatology (Oxford) 49:652–656. https://doi.org/10.1093/rheumatology/kep417
Bowes J, Barton A (2008) Recent advances in the genetics of RA susceptibility. Rheumatology (Oxford) 47:399–302. https://doi.org/10.1093/rheumatology/ken005
Imboden JB (2009) The immunopathogenesis of rheumatoid arthritis. Annu Rev Pathol-Mech 4:417–434. https://doi.org/10.1146/annurev.pathol.4.110807.092254
Macgregor AJ, Snieder H, Rigby AS, Koskenvuo M, Kaprio J, Aho K et al (2000) Characterizing the quantitative genetic contribution to rheumatoid arthritis using data from twins. Arthritis Rheum 43:30–37. https://doi.org/10.1002/1529-0131(200001)43:1<30:AID-ANR5>3.0.CO;2-B
John S, Myerscough A, Marlow A, Hajeer A, Silman A, Ollier W, Worthington J (1998) Linkage of cytokine genes to rheumatoid arthritis. Evidence of genetic heterogeneity. Ann Rheum Dis 57:361–365. https://doi.org/10.1136/ard.57.6.361
Cheon H, Yu SJ, Yoo DH, Chae IJ, Song GG, Sohn J (2002) Increased expression of pro-inflammatory cytokines and metalloproteinase-1 by TGF-β1 in synovial fibroblasts from rheumatoid arthritis and normal individuals. Clin Exp Immunol 127:547–552. https://doi.org/10.1046/j.1365-2249.2002.01785.x
Chu CQ, Field M, Abney E, Zheng RQH, Allard S, Feldmann M, Maini RN (1991) Transforming growth factor-β1 in rheumatoid synovial membrane and cartilage pannus junction. Clin Exp Immunol 86:380–386. https://doi.org/10.1111/j.1365-2249.1991.tb02941.x
Fujii D, Brissenden JE, Derynck R, Francke U (1986) Transforming growth factor β gene maps to human chromosome 19 long arm and to mouse chromosome 7. Somat Cell Mol Genet 12:281–288. https://doi.org/10.1007/bf01570787
Blobe GC, Schiemann WP, Lodish HF (2000) Role of transforming growth factor β in human disease. N Engl J Med 342:1350–1358. https://doi.org/10.1056/NEJM200005043421807
Li B, Khanna A, Sharma V, Singh T, Suthanthiran M, August P (1999) TGF-β1 DNA polymorphisms, protein levels, and blood pressure. Hypertension 33:271–275. https://doi.org/10.1161/01.HYP.33.1.271
He B, Xu C, Yang B, Landtblom AM, Fredrikson S, Hillert J (1998) Linkage and association analysis of genes encoding cytokines and myelin proteins in multiple sclerosis. J Neuroimmunol 86:13–19. https://doi.org/10.1016/s0165-5728(98)00003-4
Yamada Y, Miyauchi A, Goto J, Takagi Y, Okuizumi H, Kanematsu M, Hase M, Takai H, Harada A, Ikeda K (1998) Association of a polymorphism of the transforming growth factor-β1 gene with genetic susceptibility to osteoporosis in postmenopausal Japanese women. J Bone Miner Res 13:1569–1576. https://doi.org/10.1359/jbmr.1998.13.10.1569
Zhu Y, Liu F, Zhang F, Yao DF, Chen XD (2006) Correlation of transforming growth factor beta1 gene T869C polymorphism and rheumatoid arthritis in Chinese population. Chin Med J 32:1112
Wang YP, Xiao LS, Zhou Y, Fei Y, Li JP (2007) Gene polymorphisms of transforming growth factor-beta 1 with rheumatoid arthritis. Asia Pac J Public Health 23:1405
Alayli G, Kara N, Tander B, Canturk F, Gunes S, Bagci H (2009) Association of transforming growth factor β1 gene polymorphism with rheumatoid arthritis in a Turkish population. Joint Bone Spine 76:20–23. https://doi.org/10.1016/j.jbspin.2008.02.012
Panoulas VF, Douglas KMJ, Smith JP, Stavropoulos-Kalinoglou A, Metsios GS, Nightingale P et al (2008) Transforming growth factor-β1 869T/C, but not interleukin-6-174G/C, polymorphism associates with hypertension in rheumatoid arthritis. Rheumatology(Oxford) 48:113–118. https://doi.org/10.1093/rheumatology/ken443
Kim SY, Han SW, Kim GW, Lee JM, Kang YM (2004) TGF-ß1 polymorphism determines the progression of joint damage in rheumatoid arthritis. Scand J Rheumatol 33:389–394. https://doi.org/10.1080/03009740410010344
Pokorny V, Chau J, Wu L, Yeoman S, Black P, Mcqueen F et al (2003) Transforming growth factor β1 gene (HSTGFB1) nucleotide T869C (codon 10) polymorphism is not associated with prevalence or severity of rheumatoid arthritis in a Caucasian population. Ann Rheum Dis 62:907–908. https://doi.org/10.1136/ard.62.9.907
Patel SL, Kumar V, Mishra R, Chandra V, Prakash J, Gupta V et al (2015) Effectiveness of methotrexate therapy with occasional corticosteroid in rheumatoid arthritis. Curr Orthop Pract 26:148–154. https://doi.org/10.1097/BCO.0000000000000213
Arnett FC, Edworthy SM, Bloch DA, Mcshane DJ, Fries JF, Cooper NS et al (1988) The American Rheumatism Association 1987 revised criteria for the classification of rheumatoid arthritis. Arthritis Rheum 31:315–324. https://doi.org/10.1002/art.178010302
Miller SA, Dykes DD, Polesky HFRN (1988) A simple salting out procedure for extracting DNA from human nucleated cells. Nucleic Acids Res 16:1215. https://doi.org/10.1093/nar/16.3.1215
Perrey C, Turner SJ, Pravica V, Howell WM, Hutchinson IV (1999) ARMS-PCR methodologies to determine IL-10, TNF-α, TNF-β and TGF-β1 gene polymorphisms. Transpl Immunol 2:127–128. https://doi.org/10.1016/s0966-3274(99)80030-6
Aldener-cannavá A, Olerup O (1994) HLA-DQB1 ‘LOW-RESOLUTION’TYPING BY PCR AMPLIFICATION WITH SEQUENCE-SPECIFIC PRIMERS (PCR-SSP). Int J Immunogenet 21:447–455. https://doi.org/10.1111/j.1744-313x.1994.tb00217.x
Gauderman WJ, Morrison JM (2006) "QUANTO 1.1: a computer program for power and sample size calculations for genetic-epidemiology studies.; http://hydra. usc. edu/gxe
Sugiura Y, Niimi T, Sato S, Yoshinouchi T, Banno S, Naniwa T, Maeda H, Shimizu S, Ueda R (2002) Transforming growth factor β1 gene polymorphism in rheumatoid arthritis. Ann Rheum Dis 61:826–828. https://doi.org/10.1136/ard.61.9.826
Hussein YM, Mohamed RH, EE EL-S, Alzahrani SS (2014) Interaction between TGF-β1 (869C/T) polymorphism and biochemical risk factor for prediction of disease progression in rheumatoid arthritis. Gene 536:393–397. https://doi.org/10.1016/j.gene.2013.11.042
Evans CH, Ghivizzani SC, Robbins PD (2006) Gene therapy for arthritis: what next? Arthritis Rheum 54:1714–1729. https://doi.org/10.1002/art.21886
Yokota M, Ichihara S, Lin TL, Nakashima N, Yamada Y (2000) Association of a T29→C polymorphism of the transforming growth factor-β1 gene with genetic susceptibility to myocardial infarction in Japanese. Circulation 101:2783–2787. https://doi.org/10.1161/01.cir.101.24.2783
Zhou TB, Zhao HL, Fang SL, Drummen GP (2014) Association of transforming growth factor-β1 T869C, G915C, and C509T gene polymorphisms with rheumatoid arthritis risk. J Recept Sig Transduct 34:469–475. https://doi.org/10.3109/10799893.2014.919594
Zhang L (2013) Yan jw, Wang YX, Wan YN, Li JP, Liu P et al. Association of TGF-β1+ 869C/T promoter polymorphism with susceptibility to autoimmune diseases: a meta-analysis. Mol Biol Rep 40:4811–4817. https://doi.org/10.1007/s11033-013-2577-4
Ceccarelli F, Perricone C, Fabris M, Alessandri C, Iagnocco A, Fabro C et al (2011) Transforming growth factor β 869C/T and interleukin 6-174G/C polymorphisms relate to the severity and progression of bone-erosive damage detected by ultrasound in rheumatoid arthritis. Arthritis Res Ther 13:R111. https://doi.org/10.1186/ar3396
Mattey DL, Nixon N, Dawes PT, Kerr J (2005) Association of polymorphism in the transforming growth factor β1 gene with disease outcome and mortality in rheumatoid arthritis. Ann Rheum Dis 64:1190–1194. https://doi.org/10.1136/ard.2004.031674
Crilly A, Hamilton J, Clark CJ, Jardine A, Madhok R (2002) Analysis of transforming growth factor β1 gene polymorphisms in patients with systemic sclerosis. Ann Rheum Dis 61:678–681. https://doi.org/10.1136/ard.61.8.678
Dunning AM, Ellis PD, Mcbride S, Kirschenlohr HL, Healey CS, Kemp PR et al (2003) A transforming growth factorβ1 signal peptide variant increases secretion in vitro and is associated with increased incidence of invasive breast cancer. Cancer Res 63:2610–2615
Wu L, Chau J, Young RP, Pokorny V, Mills GD, Hopkins R et al (2004) Transforming growth factor-β1 genotype and susceptibility to chronic obstructive pulmonary disease. J Med Genet 41:285–285. https://doi.org/10.1136/thorax.2003.005769
Hinke V, Seck T, Clanget C, Scheidt-Nave C, Ziegler R, Pfeilschifter J (2001) Association of transforming growth factor-b1 (TGFβ1) T29? C gene polymorphism with bone mineral density (BMD), changes in BMD, and serum concentrations of TGF-b1 in a population-based sample of postmenopausal German women. Calcif Tissue Int 69:315–320. https://doi.org/10.1007/s002230020024
Arkwright PD, Laurie S, Super M, Pravica V, Schwarz MJ, Webb AK, Hutchinson IV (2000) TGF-β1 genotype and accelerated decline in lung function of patients with cystic fibrosis. Thorax 55:459–462. https://doi.org/10.1136/thorax.55.6.459
Garcia-Gonzalez MA, Strunk M, Piazuelo E, Benito R, Santolaria S, Jiménez P, Sopeña F, Pascual C, Simón MA, Sainz R, Lanas A (2006) TGFB1 gene polymorphisms: their relevance in the susceptibility to Helicobacter pylori-related diseases. Genes Immun 7:640–646
Ning L, Jianwei L, Chenhe Z, FuHua Z (2017) Association between transforming growth factor-beta 1 gene single nucleotide polymorphisms and knee osteoarthritis susceptibility in a Chinese Han population. J Int Med Res 45(5):1495–1504
Zentilin P, Seriolo B, Dulbecco P, Caratto E, Iiritano E, Fasciolo D, Bilardi C, Mansi C (2002) Testa E &Savarino V Eradication of Helicobacter pylori may reduce disease severity in rheumatoid arthritis. Aliment Pharmacol Ther 16(7):1291–1299
Lee YH, Bae SC (2017) Association between circulating transforming growth factor-β1 level and polymorphisms in systemic lupus erythematosus and rheumatoid arthritis: a meta-analysis. Cell Mol Biol (Noisy-le-grand) 63(1):53–59. https://doi.org/10.14715/cmb/2017.63.1.11
Yamada Y, Okuizumi H, Miyauchi A, Takagi Y, Ikeda K, Harada A (2000) Association of transforming growth factor β1 genotype with spinal osteophytosis in Japanese women. Arthritis Rheum 43:452–460
Hsu CY, Iribarren C, McCulloch CE, Darbinian J, Go AS (2009) Risk factors for end-stage renal disease: 25-year follow-up. Arch Intern Med 169:342–350. https://doi.org/10.1001/archinternmed.2008.605
Kitas GD, Erb N (2003) Tackling ischaemic heart disease in rheumatoid arthritis. Rheumatology (Oxford) 42:607–613. https://doi.org/10.1093/rheumatology/keg175
Dessein PH, Joffe BI, Stanwix AE (2003) Inflammation, insulin resistance, and aberrant lipid metabolism as cardiovascular risk factors in rheumatoid arthritis. J Rheumatol 30:1403–1405
Panoulas VF, Milionis HJ, Douglas KM, Nightingale P, Kita MD, Klocke R, Elisaf MS, Kitas GD (2007) Association of serum uric acid with cardiovascular disease in rheumatoid arthritis. Rheumatology (Oxford) 46:1466–1470. https://doi.org/10.1093/rheumatology/kem159
Tsouli SG, Liberopoulos EN, Mikhailidis DP, Athyros VG, Elisaf MS (2006) Elevated serum uric acid levels in metabolic syndrome: an active component or an innocent bystander? Metabolism. 55:1293–1301. https://doi.org/10.1016/j.metabol.2006.05.013
Peres RS, Donate PB, Talbot J, Cecilio NT, Lobo PR, Machado CC, Lima KWA, Oliveira RD, Carregaro V, Nakaya HI, Cunha TM, Alves-Filho JC, Liew FY, Louzada-Junior P, Cunha FQ (2018) TGF-β signalling defect is linked to low CD39 expression on regulatory T cells and methotrexate resistance in rheumatoid arthritis. J Autoimmun 90:49–58. https://doi.org/10.1016/j.jaut.2018.01.004
Acknowledgments
The manuscript has not been previously published nor has it been submitted simultaneously for publication elsewhere. The Indian Council of Medical Research (ICMR), New Delhi (India), is highly acknowledged for the Grant support to academic research work.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
None.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Patel, S.L., Prakash, J. & Gupta, V. TGF-β1 +869C/T polymorphism increases susceptibility to rheumatoid arthritis in North Indian population. Clin Rheumatol 39, 2881–2888 (2020). https://doi.org/10.1007/s10067-020-05064-w
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10067-020-05064-w