Abstract
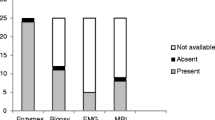
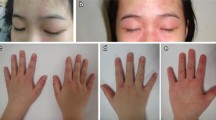
Juvenile dermatomyositis (JDM) is a rare chronic inflammatory disease of unknown etiology and primarily involves muscle and skin. It is the most common idiopathic inflammatory myopathy of childhood. This study aimed to evaluate demographic and clinical features, laboratory data, treatment modalities, and outcome of patients with JDM at a referral pediatric rheumatology center in Turkey. We retrospectively reviewed medical records of patients diagnosed with JDM between the years 2003–2016 at the Pediatric Rheumatology Department Cerrahpasa Medical Faculty. A total of 50 patients (35 females), median age at the onset 6.1 ± 4.1 years, were identified. Mean follow-up period was 74.5 ± 49.7 months. Presenting clinical symptoms included heliotrope rash (100%), Gottron papule (96%), muscle weakness (90%), erythroderma (88%), and calcinosis (38%). All patients had elevated muscle enzymes at the disease onset. Sixty-eight percent of the patients had anti-nuclear antibody positivity. Electromyography on 27 patients and muscle biopsy on 14 patients were performed, and all of them showed signs of juvenile dermatomyositis. Early aggressive treatment with corticosteroids mostly in combination with methotrexate was used. Cyclosporine was added to 48% of the patients’ treatment regimen in case of severe or refractory disease. All patients except two cases, who were referred to our clinic after long disease duration with widespread calcinosis, achieved remission. Early diagnosis and early initiation of intensive therapy are important in reducing JDM complications. International collaboration is needed in order to better understanding and management of the disease.
Similar content being viewed by others
References
Huber A, Feldman BM (2013) An update on inflammatory myositis in children. Curr Opin Rheumatol 25:630–635
Rider LG, Lindsley CB, Miller FW (2016) Juvenile Dermatomyositis. In: Petty RE, Laxer RM, Lindsley CB, Wedderburn L (eds) Textbook of pediatric rheumatology, 7th edn. Elsevier, Philadelphia, pp 351–383
Rider LG, Katz JD, Jones OY (2013) Developments in the classification and treatment of the juvenile idiopathic inflammatory myopathies. Rheum Dis Clin N Am 39:877–904
Symmons DP, Sills JA, Davis SM (1995) The incidence of juvenile dermatomyositis: results from a nation-wide study. Br J Rheumatol 34:732–736
Mendez EP, Lipton R, Ramsey-Goldman R, Roettcher P, Bowyer S, Dyer A, Pachman LM (2003) US incidence of juvenile dermatomyositis, 1995–1998: results from the National Institute of Arthritis and Musculoskeletal and Skin Diseases registry. Arthritis Rheum 49:300–305
Batthish M, Feldman BM (2011) Juvenile Dermatomyositis. Curr Rheumatol Rep 13:216–224
Shah M, Mamyrova G, Targoff IN, Huber AM, Malley JD, Rice MM, Miller FW, Rider LG (2013) The clinical phenotypes of the juvenile idiopathic inflammatory myopathies. Medicine (Baltimore) 92:25–41
Ramanan AV, Feldman BM (2002) Clinical features and outcomes of juvenile dermatomyositis and other childhood onset myositis syndromes. Rheum Dis Clin N Am 28:833–857
Morris P, Dare J (2010) Juvenile dermatomyositis as a paraneoplastic phenomenon: an update. J Pediatr Hematol Oncol 32:189–191
Bohan A, Peter JB (1975) Polymyositis and dermatomyositis (first of two parts). N Engl J Med 292:344–347
Bohan A, Peter JB (1975) Polymyositis and dermatomyositis (second of two parts). N Engl J Med 292:403–407
Robinson AB, Hoeltzel MF, Wahezi DM, Becker ML, Kessler EA, Schmeling H et al (2013) Clinical characteristics of children with juvenile dermatomyositis: the childhood arthritis and rheumatology research alliance (CARRA) registry. Arthritis Care Res 66:404–410
Brown VE, Pilkington CA, Feldman BM, Davidson JE (2006) An international consensus survey of the diagnostic criteria for juvenile dermatomyositis (JDM). Rheumatology (Oxford) 45:990–993
Gowdie PJ, Allen RC, Kornberg AJ, Akikusa JD (2013) Clinical features and disease course of patients with juvenile dermatomyositis. Int J Rheum Dis 16:561–567
Martin N, Li CK, Wedderburn LR (2012) Juvenile dermatomyositis: new insights and new treatment strategies. The Adv Musculoskelet Dis 4:41–50
Ernste FC, Reed AM (2013) Idiopathic inflammatory myopathies: current trends in pathogenesis, clinical features, and up-to-date treatment recommendations. Mayo Clin Proc 88:83–105
Carstens PO, Schmidt J (2014) Diagnosis, pathogenesis and treatment of myositis: recent advances. Clin Exp Immunol 175:349–358
Hashkes PJ, Wright BM, Lauer MS, Worley SE, Tang AS, Roettcher PA, Bowyer SL (2010) Mortality outcomes in pediatric rheumatology in the US. Arthritis Rheum 62:599–608
Lazarevic D, Pistorio A, Palmisani E, Miettunen P, Ravelli A, Pilkington C et al (2013) The PRINTO criteria for clinically inactive disease in juvenile dermatomyositis. Ann Rheum Dis 72:686–693
Malek A, Raeeskarami SR, Ziaee V, Aghighi Y, Moradinejad MH (2014) Clinical course and outcomes of Iranian children with juvenile dermatomyositis and polymyositis. Clin Rheumatol 33:1113–1118
Ruperto N, Pistorio A, Oliveira S, Zulian F, Cuttica R, Ravelli A et al (2016) Prednisone versus prednisone plus cyclosporine versus prednisone plus methotrexate in new-onset juvenile dermatomyositis: a randomised trial. Lancet 387:671–678
Faller G, Mistry BJ, Tikly M (2014) Juvenile dermatomyositis in South African child is characterized by frequent dystrophic calcification: a cross sectional study. Pediatr Rheumatol Online J 12:2
McCann LJ, Juggins AD, Maillard SM, Wedderburn LR, Davidson JE, Murray KJ, Pilkington CA (2006) The Juvenile Dermatomyositis National Registry and Repository (UK and Ireland)—clinical characteristics of children recruited within 5 yr. Rheumatology (Oxford) 45:1255–1260
Ravelli A, Trail L, Ferrari C, Ruperto N, Pistorio A, Pilkington C et al (2010) Long term outcome and prognostic factors of juvenile dermatomyositis: a multinational, multicenter study of 490 patients. Arthritis Care Res (Hoboken) 62:63–72
Prasad S, Misra R, Agarwal V (2013) Juvenile dermatomyositis at a tertiary care hospital: is there any change in the last decade? Int J Rheum Dis 16:556–560
Saini I, Kalaivani M, Kabra SK (2016) Calcinosis in juvenile dermatomyositis: frequency, risk factors and outcome. Rheumatol Int 36:961–965
Kishi T, Miyamae T, Hara R, Nakajima S, Imagawa T, Mori M, Yokota S (2013) Clinical analyses of 50 children with juvenile dermatomyositis. Mod Rheumatol 23:311–317
Kim S, El-Hallak M, Dedeoglu F, Zurakowski D, Fuhlbrigge RC, Sundel RP (2009) Complete and sustained remission of juvenile dermatomyositis resulting from aggressive treatment. Arthritis Rheum 60:1825–1830
Estruch R, Grau JM, Fernandez-Sola J, Casademont J, Monforte R, Urbano-Marquez A (1992) Microvascular changes in skeletal muscle in idiopathic inflammatory myopathy. Hum Pathol 23:888–895
Dorph C, Englund P, Nennesmo I, Lundberg IE (2006) Signs of inflammation in both symptomatic and asymptomatic muscles from patients with polymyositis and dermatomyositis. Ann Rheum Dis 65:1565–1571
Gitiaux C, De Antonio M, Aouizerate J, Gherardi RK, Guilbert T, Barnerias C et al (2016) Vaculopathy-related clinical and pathological features are associated with severe juvenile dermatomyositis. Rheumatology (Oxford) 55:470–479
Kolasinski SL, Chi AS, Lopez-Garib AJ (2016) Current perspectives on imaging for systemic lupus erythematosus, systemic sclerosis, and dermatomyositis/polymyositis. Rheum Dis Clin N Am 42:711–732
Elessawy SS, Abdelsalam EM, Abdel Razek E, Tharwat S (2016) Whole-body MRI for full assessment and characterization of diffuse inflammatory myopathy. Acta Radiol Open 5:2058460116668216 eCollection 2016
Enders FB, Bader-Meunier B, Baildam E, Constantin T, Dolezalova P, Feldman BM et al (2016) Consensus-based recommendations for the management of juvenile dermatomyositis. Ann Rheum Dis. doi:10.1136/annrheumdis-2016-209247 [Epub ahead of print]
Aggarwal R, Loganathan P, Koontz D, Qi Z, Reed AM, Oddis CV (2016) Cutaneous improvement in refractory adult and juvenile dermatomyositis after treatment with rituximab. Rheumatology (Oxford). Nov 11. pii: kew396. [Epub ahead of print]
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
None.
Electronic supplementary material
Supplementary file 1
The treatment algorithm of our clinic for Juvenile dermatomyositis (DOCX 38 kb)
Rights and permissions
About this article
Cite this article
Barut, K., Aydin, P.O.A., Adrovic, A. et al. Juvenile dermatomyositis: a tertiary center experience. Clin Rheumatol 36, 361–366 (2017). https://doi.org/10.1007/s10067-016-3530-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10067-016-3530-4