Abstract
Objective
This investigation aimed to characterize in a 6-month follow-up the microbial profile of implants restored with either titanium or zirconia abutments at the genus or higher taxonomic levels.
Methods
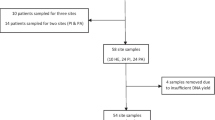
Twenty healthy individuals indicative for implant-retained single restorations were investigated. Half of participants were restored with titanium and half with zirconia abutments. Biofilm was collected from the implant-related sites after 1, 3, and 6 months of loading. The 16S rDNA genes were amplified and sequenced with Roche/454 platform.
Results
A total of 596 species were identified in 360 samples and grouped in 18 phyla and 104 genera. Titanium- or zirconia-related sites as well as teeth showed similar total numbers of operational taxonomic units (OTUs) colonizing surfaces over time. Firmicutes, Proteobacteria, Fusobacteria, Bacteroidetes, and Actinobacteria were the most prevalent phyla with significant differences between different surfaces and time point. Unclassified genera were found in lower levels (1.71% up to 9.57%) on titanium and zirconia samples when compared with teeth, with no significant differences.
Conclusion
Titanium- and zirconia-related surfaces are promptly colonized by a bacterial community similar to those found in the remaining adjacent teeth. Results suggest a selective adhesion of different bacterial genotypes for either titanium or zirconia surfaces. Data also indicate a significant interaction between the relative effects taxa, time point, and sampling site.
Clinical relevance
The present study disclosed a wider spectrum of microorganisms colonizing either titanium- or zirconia-related microbiomes in very early stage of implant colonization, revealing differences and suggesting a probably specific mechanism for selective bacterial adhesion.




Similar content being viewed by others
References
Stokman MA, van Winkelhoff AJ, Vissink A, Spijkervet FK, Raghoebar GM (2017) Bacterial colonization of the peri-implant sulcus in dentate patients: a prospective observational study. Clin Oral Investig 21(2):717–724. https://doi.org/10.1007/s00784-016-1941-x
Moraschini V, Poubel LA, Ferreira VF, Barboza ES (2015) Evaluation of survival and success rates of dental implants reported in longitudinal studies with a follow-up period of at least 10 years: a systematic review. Int J Oral Maxillofac Surg 44(3):377–388. https://doi.org/10.1016/j.ijom.2014.10.023
Chen MH, Shi JY. (2017) Clinical and radiological outcomes of implants in osteotome sinus floor elevation with and without grafting: a systematic review and a meta-analysis. J Prosthodont. https://doi.org/10.1111/jopr.12576
Jang HW, Kang JK, Lee K, Lee YS, Park PK (2011) A retrospective study on related factors affecting the survival rate of dental implants. J Adv Prosthodont 3(4):204–215. https://doi.org/10.4047/jap.2011.3.4.204
Sakka S, Baroudi K, Nassani MZ (2012) Factors associated with early and late failure of dental implants. J Investig Clin Dent 3:258–261
Gupta S, Gupta H, Tandan A (2015) Technical complications of implant-causes and management: a comprehensive review. Natl J Maxillofac Surg 6(1):3–8. https://doi.org/10.4103/0975-5950.168233
do Nascimento C, Miani PK, Pedrazzi V, Muller K, Albuquerque Junior RF (2012) Bacterial leakage along the implant-abutment interface: culture and DNA checkerboard hybridization analyses. Clin Oral Implants Res 23(10):1168–1172. https://doi.org/10.1111/j.1600-0501.2011.02280.x
Cançado Oliveira BF, Valerio CS, Jansen WC, Zenóbio EG, Manzi FR (2016) Accuracy of digital versus conventional periapical radiographs to detect misfit at the implant-abutment interface. Int J Oral Maxillofac Implants 31(5):1023–1029. https://doi.org/10.11607/jomi.4525
Scarano A, Valbonetti L, Degidi M, Pecci R, Piattelli A, de Oliveira PS, Perrotti V (2016) Implant-abutment contact surfaces and microgap measurements of different implant connections under 3-dimensional X-ray microtomography. Implant Dent 25:656–662
Passos SP, Gressler May L, Faria R, Özcan M, Bottino MA (2013) Implant-abutment gap versus microbial colonization: clinical significance based on a literature review. J Biomed Mater Res B Appl Biomater 101(7):1321–1328. https://doi.org/10.1002/jbm.b.32945
Canullo L, Penarrocha-Oltra D, Soldini C, Mazzocco F, Penarrocha M, Covani U (2015) Microbiological assessment of the implant-abutment interface in different connections: cross-sectional study after 5 years of functional loading. Clin Oral Implants Res 26(4):426–434. https://doi.org/10.1111/clr.12383
Penarrocha-Oltra D, Monreal-Bello A, Penarrocha-Diago M, Alonso-Perez-Barquero J, Botticelli D, Canullo L (2016) Microbial colonization of the peri-implant sulcus and implant connection of implants restored with cemented versus screw-retained superstructures: a cross-sectional study. J Periodontol 87(9):1002–1011. https://doi.org/10.1902/jop.2016.160017
Duarte AR, Rossetti PH, Rossetti LM, Torres SA, Bonachela WC (2006) In vitro sealing ability of two materials at five different implant-abutment surfaces. J Periodontol 77(11):1828–1832. https://doi.org/10.1902/jop.2006.060101
Barbosa RE, do Nascimento C, Issa JP, Watanabe E, Ito IY, de Albuquerque RF Jr (2009) Bacterial culture and DNA checkerboard for the detection of internal contamination in dental implants. J Prosthodont 18(5):376–381. https://doi.org/10.1111/j.1532-849X.2009.00454.x
Harder S, Dimaczek B, Açil Y, Terheyden H, Freitag-Wolf S, Kern M (2010) Molecular leakage at implant-abutment connection—in vitro investigation of tightness of internal conical implant-abutment connections against endotoxin penetration. Clin Oral Investig 14(4):427–432. https://doi.org/10.1007/s00784-009-0317-x
Harder S, Podschun R, Grancicova L, Mehl C, Kern M (2013) Analysis of the intraimplant microflora of two-piece dental implants. Clin Oral Investig 17(4):1135–1142. https://doi.org/10.1007/s00784-012-0805-2
Schmidlin PR, Muller P, Attin T, Wieland M, Hofer D, Guggenheim B (2013) Polyspecies biofilm formation on implant surfaces with different surface characteristics. J Appl Oral 21(1):48–55. https://doi.org/10.1590/1678-7757201302312
Zhao B, van der Mei HC, Subbiahdoss G, de Vries J, Rustema-Abbing M, Kuijer R, Busscher HJ, Ren Y (2014) Soft tissue integration versus early biofilm formation on different dental implant materials. Dent Mater 30(7):716–727. https://doi.org/10.1016/j.dental.2014.04.001
do Nascimento C, Pita MS, Santos Ede S, Monesi N, Pedrazzi V, Albuquerque Junior RF, Ribeiro RF (2016) Microbiome of titanium and zirconia dental implants abutments. Dent Mater 32:93–101
Volgenant CM, Zaura E, Brandt BW, Buijs MJ, Tellez M, Malik G, Ismail AI, Ten Cate JM, van der Veen MH (2017) Red fluorescence of dental plaque in children—a cross-sectional study. J Dent 58:40–47
Corinaldesi C, Danovaro R, Dell'Anno A (2005) Simultaneous recovery of extracellular and intracellular DNA suitable for molecular studies from marine sediments. Appl Environ Microbiol 71(1):46–50. https://doi.org/10.1128/AEM.71.1.46-50.2005
Meyer F, Paarmann D, D’Souza M, Olson R, Glass EM, Kubal M, Paczian T, Rodriguez A, Stevens R, Wilke A, Wilkening J, Edwards RA (2008) The metagenomics RAST server—a public resource for the automatic phylogenetic and functional analysis of metagenomes. BMC Bioinformatics 9(1):386. https://doi.org/10.1186/1471-2105-9-386
Noguchi K, Gel YR, Brunner E, Konietschke F (2012) nparLD: an R software package for the nonparametric analysis of longitudinal data in factorial experiments. J Stat Softw 50:1–23
Brunner E, Domhof S, Langer F (2012) Nonparametric analysis of longitudinal data in factorial experiments. Wiley, New York
de Melo F, do Nascimento C, Souza DO, de Albuquerque RF Jr (2017) Identification of oral bacteria on titanium implant surfaces by 16S rDNA sequencing. Clin Oral Implants Res 28(6):697–703. https://doi.org/10.1111/clr.12865
Palacios JAV, Garcia JJ, Caramês JMM, Quirynen M, da Silva Marques DN (2017) Short implants versus bone grafting and standard-length implants placement: a systematic review. Clin Oral Investig 22(1):69–80. https://doi.org/10.1007/s00784-017-2205-0
Sousa V, Nibali L, Spratt D, Dopico J, Mardas N, Petrie A, Donos N (2017) Peri-implant and periodontal microbiome diversity in aggressive periodontitis patients: a pilot study. Clin Oral Implants Res 28(5):558–570. https://doi.org/10.1111/clr.12834
Griffen AL, Beall CJ, Campbell JH, Firestone ND, Kumar PS, Yang ZK, Podar M, Leys EJ (2012) Distinct and complex bacterial profiles in human periodontitis and health revealed by 16s pyrosequencing. ISME J 6(6):1176–1185. https://doi.org/10.1038/ismej.2011.191
Drescher J, Schlafer S, Schaudinn C, Riep B, Neumann K, Friedmann A, Petrich A, Gobel UB, Moter A (2010) Molecular epidemiology and spatial distribution of Selenomonas spp. in subgingival biofilms. Eur J Oral Sci 118(5):466–474. https://doi.org/10.1111/j.1600-0722.2010.00765.x
Nagpal S, Prakash S, Bhat KG, Singh G (2016) Detection and comparison of Selenomonas sputigena in subgingival biofilms in chronic and aggressive periodontitis patients. J Indian Soc Periodontol 20(3):286–291. https://doi.org/10.4103/0972-124X.181247
Socransky SS, Haffajee AD, Cugini MA, Smith C, Kent RL Jr (1998) Microbial complexes in subgingival plaque. J Clin Periodontol 25(2):134–144. https://doi.org/10.1111/j.1600-051X.1998.tb02419.x
Kumar PS, Griffen AL, Barton JA, Paster BJ, Moeschberger ML, Leys EJ (2003) New bacterial species associated with chronic periodontitis. J Dent Res 82(5):338–344. https://doi.org/10.1177/154405910308200503
Dingsdag S, Nelson S, Coleman NV (2016) Bacterial communities associated with apical periodontitis and dental implant failure. Microb Ecol Health Dis. 27. https://doi.org/10.3402/mehd.v27.31307
Jhajharia K, Parolia A, Shetty KV, Mehta LK (2015) Biofilm in endodontics: a review. J Int Soc Prev Commun Dent 5(1):1–12. https://doi.org/10.4103/2231-0762.151956
Heuer W, Kettenring A, Stumpp SN, Eberhard J, Gellermann E, Winkel A, Stiesch M (2012) Metagenomic analysis of the peri-implant and periodontal microflora in patients with clinical signs of gingivitis or mucositis. Clin Oral Investig 16(3):843–850. https://doi.org/10.1007/s00784-011-0561-8
Pérez-Chaparro PJ, Duarte PM, Shibli JA, Montenegro S, Lacerda Heluy S, Figueiredo LC, Faveri M, Feres M (2016) The current weight of evidence of the microbiologic profile associated with peri-implantitis: a systematic review. J Periodontol 87(11):1295–1304. https://doi.org/10.1902/jop.2016.160184
Schaumann S, Staufenbiel I, Scherer R, Schilhabel M, Winkel A, Stumpp SN, Eberhard J, Stiesch M (2014) Pyrosequencing of supra- and subgingival biofilms from inflamed peri-implant and periodontal sites. BMC Oral Health 14(1):157. https://doi.org/10.1186/1472-6831-14-157
Yu XL, Chan Y, Zhuang LF, Lai HC, Lang NP, Lacap-Bugler DC, Leung WK, Watt RM (2016) Distributions of synergistetes in clinically-healthy and diseased periodontal and peri-implant niches. Microb Pathog 94:90–103
Sanz M, Beighton D, Curtis MA, Cury JA, Dige I, Dommisch H, Ellwood R, Giacaman R, Herrera D, Herzberg MC, Könönen E, Marsh PD, Meyle J, Mira A, Molina A, Mombelli A, Quirynen M, Reynolds EC, Shapira L, Zaura E (2017) Role of microbial biofilms in the maintenance of oral health and in the development of dental caries and periodontal diseases. Consensus report of group 1 of the Joint EFP/ORCA workshop on the boundaries between caries and periodontal disease. J Clin Periodontol 18:S5–S11
Subramani K, Jung RE, Molenberg A, Hammerle CH (2009) Biofilm on dental implants: a review of the literature. Int J Oral Maxillofac Implants 24(4):616–626
Al-Radha AS, Dymock D, Younes C, O'Sullivan D (2012) Surface properties of titanium and zirconia dental implant materials and their effect on bacterial adhesion. J Dent 40(2):146–153. https://doi.org/10.1016/j.jdent.2011.12.006
Jagathrakshakan SN, Sethumadhava RJ, Mehta DT, Ramanathan A (2015) 16S rRNA gene-based metagenomic analysis identifies a novel bacterial co-prevalence pattern in dental caries. Eur J Dent 9(1):127–132. https://doi.org/10.4103/1305-7456.149661
Hannig C, Hannig M (2009) The oral cavity—a key system to understand substratum-dependent bioadhesion on solid surfaces in man. 13(2):123–139. https://doi.org/10.1007/s00784-008-0243-3
Prasad KV, Sreenivasan PK, Patil S, Chhabra KG, Javali SB, DeVizio E (2011) Removal of dental plaque from different regions of the mouth after a 1-minute episode of mechanical oral hygiene. Am J Dent 24(1):60–64
do Nascimento C, Pita MS, Pedrazzi V, de Albuquerque Junior RF, Ribeiro RF (2013) In vivo evaluation of Candida spp adhesion on titanium or zirconia abutment surfaces. Arch Oral Biol 58(7):853–861. https://doi.org/10.1016/j.archoralbio.2013.01.014
do Nascimento C, da Rocha Aguiar C, Pita MS, Pedrazzi V, de Albuquerque Junior RF, Ribeiro RF (2013) Oral biofilm formation on the titanium and zirconia substrates. Microsc Res Tech 76(2):126–132. https://doi.org/10.1002/jemt.22143
do Nascimento C, Pita MS, Fernandes FH, Pedrazzi V, de Albuquerque Junior RF, Ribeiro RF (2014) Bacterial adhesion on the titanium and zirconia abutment surfaces. Clin Oral Implants Res 25(3):337–343. https://doi.org/10.1111/clr.12093
Funding
The work was supported by Fundação de Amparo à Pesquisa do Estado de São Paulo (FAPESP—Process 2010/12830-0 and 2014/22876-8) and Conselho Nacional de Desenvolvimento Científico e Tecnológico (CNPq—Process 457941/2014-6).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Approval for surgery and sampling was obtained from the local Research Ethics Committee (CAAE 0066.0.138.000-10).
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in this investigation involving human participants were in accordance with the ethical standards of the Faculty of Dentistry of Ribeirão Preto Ethical Committee (Brazil) and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
de Freitas, A.R., Silva, T.S.d., Ribeiro, R.F. et al. Oral bacterial colonization on dental implants restored with titanium or zirconia abutments: 6-month follow-up. Clin Oral Invest 22, 2335–2343 (2018). https://doi.org/10.1007/s00784-018-2334-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00784-018-2334-0